Perforated eardrum
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Surangi Mendis, MRCGPLast updated 5 Aug 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
A burst (perforated) eardrum is usually not serious and often heals in a few weeks on its own. Complications sometimes occur, such as hearing loss and infection in the middle ear. A small procedure to repair the eardrum may be an option if it does not heal by itself, especially if the perforation causes hearing loss.
At a glance
A perforated eardrum is a tear or hole in the eardrum.
It can cause changes in hearing, earache, noises in the ear, or fluid leakage.
Common causes include middle ear infections, direct injury, or sudden loud noises.
Most perforated eardrums heal on their own within 6-8 weeks.
See your GP if you have symptoms of a perforated eardrum.
In this article:
Video picks for Hearing problems
Continue reading below
What is a perforated eardrum?
What is a perforated eardrum?
A perforated eardrum is a tear or hole in the eardrum. It can affect hearing. The extent of hearing loss can vary greatly. For example, small holes may only cause minimal loss of hearing. Larger holes may affect hearing more severely. Also, if the tiny bones (ossicles) behind the eardrum are damaged in addition to the perforation, then the hearing loss would be greater than, for example, one caused by a small perforation away from the ossicles.
With a perforation, there is greater risk of developing an ear infection. This is because the eardrum normally acts as a barrier to prevent bacteria and other germs entering the middle ear.
Perforated eardrum symptoms
Back to contentsThere may be no symptoms, or there may be symptoms associated with the cause of the perforation. The most common cause of perforation is infection.
Possible symptoms and signs of a perforated eardrum include:
Changes in how you hear, that may range from slightly muffled hearing to significant loss.
Noises in your ear - ringing or buzzing (tinnitus).
Aching or pain in your ear.
Itching in your ear.
Fluid leaking from your ear.
Dizziness.
The feeling of air coming out of the ear when the nose is blown - blowing the nose usually causes the eardrum to balloon outwards a little but if there is a hole, air will be pushed out of the ear instead.
If your perforated eardrum is caused by a middle ear infection, you may have earache which suddenly gets worse when the drum perforates but then quickly improves or even completely resolves. This is because the perforation usually allows pus to be released from behind the eardrum, relieving pressure.
The symptoms will usually pass once your eardrum has healed and any infection has been treated.
Continue reading below
When to see a doctor about a perforated eardrum
Back to contentsSee your GP if you have symptoms of a perforated eardrum. They can usually confirm whether a perforation is present. If you have symptoms of infection, such as fluid leaking from the ear or a high temperature, antibiotic medications may be required. If you have hearing loss that does not improve over time, a hearing test or referral to an ear specialist may be requested.
How is a perforated eardrum diagnosed?
A doctor can usually diagnose a torn (perforated) eardrum simply by looking into the ear with a special torch called an otoscope. However, sometimes it is difficult to see the eardrum if there is a lot of inflammation, wax, or infection present in the ear.
If a hearing test is performed for any reason, for example, if there is also suspected hearing loss, a test of the middle ear known as tympanometry is also usually performed. This can confirm whether a perforation is present.
Perforated eardrum causes
Back to contentsCauses include:
Middle ear infections, which can damage the eardrum. In this situation there is often discharge as pus runs out from the middle ear.
Direct injury to the ear - for example, a punch to the ear.
A sudden loud noise - for example, from a nearby explosion. The shock waves and sudden sound waves can tear (perforate) the eardrum. This is often the most severe type of perforation and it can lead to significant hearing loss and ringing in the ear (tinnitus).
Barotrauma. This occurs when there is a sudden change in air pressure, creating a sharp difference between the air pressure outside the ear and in the middle ear, for example, when descending in an aircraft or whilst scuba diving. Pain in the ear due to a tense eardrum is common during height (altitude) changes when flying. However, a perforated eardrum only happens rarely in extreme cases.
See the separate leaflet called Barotrauma to the ear for more detailsPoking foreign objects, such as a cotton bud, into the ear. This can sometimes damage the eardrum.
Grommets. These are tiny tubes that are placed through the eardrum. They allow air to pass in and out of the middle ear to stop production of the fluid that causes glue ear. When a grommet falls out, there is a tiny hole left in the eardrum. This heals quickly in most cases.
Continue reading below
What is the eardrum and how do we hear?
Back to contentsCross-section of the ear
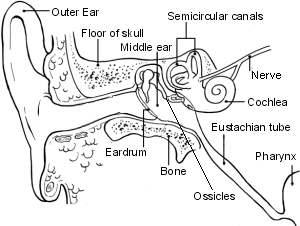
The eardrum (also called the tympanic membrane) is a thin skin-like structure in the ear. It lies between the outer (external) ear and the middle ear.
The ear is divided into three parts - the outer, middle, and inner ear. Sound waves enter the outer ear and hit the eardrum, causing the eardrum to vibrate.
Behind the eardrum are three tiny bones (ossicles). The vibrations pass from the eardrum to the bones of the middle ear. The bones then transmit the vibrations to the cochlea in the inner ear. The cochlea converts the vibrations to sound signals which are sent down a nerve to the brain, which we 'hear'.
The middle ear behind the eardrum is normally filled with air. The middle ear is connected to the back of the nose by the Eustachian tube. This allows air to move in and out of the middle ear.
Perforated eardrum treatment
Back to contentsTreatment is usually only required if the eardrum does not heal after a few weeks or if complications arise, such as hearing loss or ear infections.
No treatment is needed in most cases
A torn (perforated) eardrum will usually heal by itself within 6-8 weeks. It is a skin-like structure and, like skin that is cut, it will usually heal. In some cases, a doctor may prescribe antibiotic medicines, usually drops, if there is an infection or risk of infection developing in the middle ear whilst the eardrum is healing.
What happens if water passes through a perforated eardrum?
It is best to avoid water getting into the ear whilst it is healing. For example, you may be advised to put a large ball of cotton wool covered with petroleum jelly (eg, Vaseline™) into your outer ear whilst showering or washing your hair. It is best not to swim until the eardrum has healed.
Medical treatment
Occasionally, a perforated eardrum gets infected and needs antibiotics. It is thought that some antibiotic ear drops can occasionally damage the nerve supply to the ear. Your doctor will select a type that does not have this risk.
Surgical treatment
A small operation may be required to treat a perforated drum that does not heal by itself. Various techniques can be used to repair the eardrum, depending on how severe the damage is. This operation may be called a myringoplasty (repair of the perforated eardrum only) or a tympanoplasty (repair of perforated eardrum and inspection of the middle ear bones, the ossicles). These operations are usually successful in fixing the perforation and improving hearing.
However, not all people with an unhealed perforation need medical treatment or surgery. Some people have a small permanent perforation with no symptoms and no significant hearing loss. Treatment is mainly considered if there is hearing loss, as this may improve if the perforation is fixed. Also, swimmers may prefer to have a perforation repaired, as getting water in the middle ear can increase the risk ear infections.
If you have a perforation that has not healed by itself, a doctor who is an ear specialist can discuss options to help decide whether treatment is necessary.
Patient picks for Hearing problems

Ear, nose and throat
Earwax
A build-up of earwax can cause reduced hearing and sometimes other symptoms. Earwax can usually be easily removed.
by Dr Philippa Vincent, MRCGP

Ear, nose and throat
Eustachian tube dysfunction
Eustachian tube dysfunction (ETD) can cause dulled hearing and a feeling of pressure or fullness in the affected ear. It is usually just lasts for a few weeks during and after a cold. There are various other causes and sometimes it lasts longer. Often no treatment is needed but decongestants, antihistamines or a steroid nasal spray sometimes help.
by Dr Surangi Mendis, MRCGP
Frequently asked questions
If I have a perforated eardrum, will I always experience symptoms?
Not necessarily. It's possible to have a perforated eardrum with no symptoms at all. However, you might experience changes in hearing, noises in your ear like ringing, earache or pain, itching, fluid leaking from the ear, dizziness, or feel air coming out of your ear when you blow your nose.
How long does it take for a perforated eardrum to heal on its own?
In most cases, a torn eardrum will heal by itself within 6-8 weeks. It acts like skin that has been cut and typically repairs itself.
Can I prevent a perforated eardrum?
Some causes, like middle ear infections, can lead to a perforated eardrum, so managing ear infections promptly may help. Other causes, such as direct injury or poking objects into the ear, can be avoided by being careful around your ears and not inserting foreign objects like cotton buds.
What should I do if my earache gets worse, then suddenly better when I have a middle ear infection?
If you have a middle ear infection, an earache that suddenly gets worse but then quickly improves or resolves might mean your eardrum has perforated. This happens because the perforation can allow pus to be released, relieving pressure. You should still see your GP if you suspect a perforated eardrum.
Are there any specific activities I should avoid while my eardrum is healing?
While your eardrum is healing, it's best to prevent water from entering your ear. For example, you might be advised to place a large ball of cotton wool covered with petroleum jelly into your outer ear when showering or washing your hair. It's also recommended to avoid swimming until the eardrum has fully healed.
If my perforated eardrum doesn't heal, will I definitely need surgery?
Not all unhealed perforations require surgery. Some people with a small, permanent perforation have no symptoms and no significant hearing loss. Surgery is generally considered if there is notable hearing loss that could improve with repair, or if someone, like a swimmer, wants to reduce the risk of ear infections from water entering the middle ear.
Further reading and references
- British National Formulary (BNF); NICE Evidence Services (UK access only)
- Leis JA, Rutka JA, Gold WL; Aminoglycoside-induced ototoxicity. CMAJ. 2015 Jan 6;187(1):E52. doi: 10.1503/cmaj.140339. Epub 2014 Sep 15.
- Illes K, Gergo D, Keresztely Z, et al; Factors influencing successful reconstruction of tympanic membrane perforations: a systematic review and meta-analysis. Eur Arch Otorhinolaryngol. 2023 Jun;280(6):2639-2652. doi: 10.1007/s00405-023-07831-2. Epub 2023 Feb 22.
- Nicholas Jungbauer W Jr, Jeong S, Nguyen SA, et al; Comparing Myringoplasty to Type I Tympanoplasty in Tympanic Membrane Repair: A Systematic Review and Meta-analysis. Otolaryngol Head Neck Surg. 2023 May;168(5):922-934. doi: 10.1002/ohn.191. Epub 2023 Feb 8.
- Ear, Treatment summary; BNF/NICE
Continue reading below
About the authorView full bio

Dr Surangi Mendis, MRCGP
Consultant and Medical Author
MBBS, BSc (1st), MRCGP (2014), DFSRH, PGcert otology and audiology
Surangi Mendis is a consultant in Audiovestibular Medicine and Neuro-otology at The Royal National ENT and Eastman Dental Hospitals, UCLH.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 4 Aug 2027
5 Aug 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.