Genital warts
Anogenital warts
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 29 Mar 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
In this series:Sexually transmitted infectionsGenital herpesGonorrhoeaUrethritis in menTrichomoniasisMycoplasma genitalium
Anogenital warts are sometimes just called genital warts. Genital warts are a common sexually transmitted infection. They are small lumps that develop around the genital area. They may not cause any symptoms but sometimes they can be uncomfortable or itch or bleed. They are usually passed on by sexual contact.
In this article:
Video picks for Sexually transmitted infections
Continue reading below
What are genital warts?
Anogenital warts are small lumps that develop on the genitals and/or around the back passage (anus). They are caused by a virus called the human papillomavirus (HPV). There are over 100 types of this virus. Most anogenital warts are caused by types 6 or 11. Common warts that many people have on their hands and feet are caused by a different type of HPV.
How do you get genital warts?
Back to contentsHow do you get genital warts?
The virus is passed on by sexual contact. You need close skin-to-skin contact to pass on the virus. This means that you do not necessarily need to have vaginal, anal or oral sex to pass on infection. Sharing sex toys may also pass on infection. Very rarely, anogenital warts may be passed on from hand warts. They may also rarely be passed on to a baby when a woman gives birth.
It can take weeks or months to develop warts after being infected with HPV. Also, most people infected with HPV do not develop warts. You can be a carrier of the virus without realising it and you may pass on the virus to others who then develop warts. It is also possible to pass on the virus after warts have been treated or gone.
Because it can take some time to develop warts after being infected with HPV, if you have just developed noticeable anogenital warts, it does not necessarily mean that either partner has been recently unfaithful. You may have had HPV for a long time without developing warts.
Also, note that you may get anal warts even if you have not had anal sex.
Continue reading below
How common are genital warts?
Back to contentsThey are common and are one of the most commonly diagnosed sexually transmitted infections (STIs) in the UK. Many more people are infected with the virus but do not develop visible warts (they are carriers).
An individual has quite a high chance of having HPV infection in their lifetime. However, most people do not know that they have been infected because they have no symptoms. Therefore it is difficult to know exactly how common it is. Only a few people with HPV infection develop anogenital warts. Around 1 in 10 sexually active people develop genital warts at some point in their lives.
Where do genital warts appear?
Back to contentsIn men, the warts usually develop on the outer skin of the penis. In women, the warts usually develop on the vulva, just outside the vagina. Warts may also develop on the skin around the back passage (anus), both in men and in women.
Sometimes warts develop inside the vagina, on the neck of the womb (cervix), on the scrotum, or inside the anus. They also sometimes occur inside the tube that drains urine from the bladder to the outside (the urethra). Rarely, they occur in the mouth or nose.
Continue reading below
What do genital warts look like?
Back to contentsAnogenital warts may have several different appearances. There may be one or more. Sometimes individual warts join together to form one large warty area. They may look like small, skin-coloured lumps on the skin (similar to the common warts that many people have on their hands). Others may be red or pink, grey or white. Warts that develop on skin that is warm, moist and non-hairy (such as the vulva) tend to be soft. Warts that develop on skin that is dry and hairy (such as around the bottom) tend to be firm.
The number of warts that develop varies from person to person. Some people have just a few that are barely noticeable. Some people have many around their genitals and anus.
Female anogenital warts
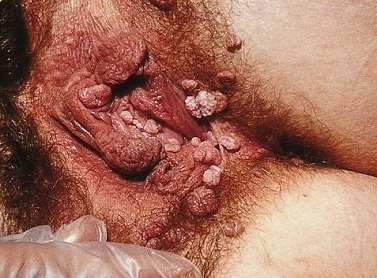
© SOA-AIDS Amsterdam, via Wikimedia Commons
Genital wart symptoms
Back to contentsOften there are no symptoms of genital warts, other than a lump on the skin being noticed. In most cases, the warts cause no physical discomfort. They sometimes cause irritation and soreness, especially if they occur around the back passage (anus). Sometimes the warts can bleed or cause pain on intercourse. If you have warts inside your anus, this can sometimes cause bleeding when you go to the toilet. If you have warts inside the tube from which your urine is passed (urethra), the stream of urine may be different, or there may be bleeding.
Warts look unsightly and some people become distressed by this. They may cause embarrassment, or interfere with sexual activity.
Are genital warts itchy?
Genital warts can be itchy, but not always. They can also be sore and uncomfortable.
How to test for genital warts
Back to contentsAnogenital warts can usually be diagnosed by their typical appearance when you are examined by a doctor or nurse. Your doctor or nurse will examine your external genitalia to look for warts. They may also suggest that they do an internal examination of your vagina or back passage to look for warts here.
So, tests are not usually needed to confirm the diagnosis. However, around 1 in 5 people with anogenital warts also have another STI. Tests such as swabs are commonly advised to check for other infections - even if you do not have any symptoms.
If you have anogenital warts, in the UK your doctor or nurse will usually refer you to a sexual health specialist in a genitourinary medicine (GUM) clinic for tests and treatment. If you are worried that you may have anogenital warts or another STI, the best option is to visit a GUM clinic from the outset. You do not need a referral from your GP to attend a GUM clinic. You can ring your GP surgery, local hospital or health authority and ask where the nearest clinic is. Local and national information is also available on the internet - for example, see Further Reading below for 'Find a sexual health clinic service".
The GUM clinic doctor or nurse will be able to diagnose your warts, and advise on treatment. They will also test you (and your partner if possible) for other infections. They will not normally write to your GP with your results unless you wish them to. All information about your visit to a GUM clinic is confidential and would only be shared with your GP with your permission. If the diagnosis is unclear, or if your warts are not getting better with treatment, you may occasionally need further tests. This usually involves taking a sample of the wart tissue to be looked at through a microscope (a biopsy).
Genital warts treatment
Back to contentsThere are a number of different treatments that can be used and they are described below. Whatever the treatment for genital warts, it usually takes several weeks of treatment to clear the warts. Sometimes it can take up to six months of treatment.
Treatment may be a little uncomfortable and cause some irritation of the skin around the area that is being treated. Also, smokers tend to respond less well to treatment, so stopping smoking may be beneficial to your treatment. Sometimes, one treatment may not be successful. If this is the case, another treatment may be advised. There is also a chance that anogenital warts can return after treatment. This is because the treatments do not clear the HPV virus itself but just treat the warty lumps.
Wart treatments that are sold over the counter in pharmacies should not be used to treat anogenital warts.
Chemical treatments
A number of chemicals, when put on to warts, will burn or destroy the wart tissue.The main alternatives used are:
Other chemicals may be advised if there is little success with the above. These are applied by the doctor or nurse in the clinic, rather than you applying them yourself at home. Another treatment called sinecatechins ointment is used for people whose immune systems are not working fully.
Physical treatments
Various techniques can destroy the wart tissue. They include:
Freezing warts with liquid nitrogen. This is a common treatment which is called cryotherapy. Liquid nitrogen is sprayed on or applied to the wart. Liquid nitrogen is very cold. The freezing and thawing destroys the wart tissue. To clear the warts fully you may need several treatments, a week or so apart. This treatment may be used if you have a small number of warts. This is often a good option if you are pregnant.
Having the warts cut off (surgical removal) under local anaesthetic. This may be an option if you have just a few warts that can be easily removed in this way.
Electrocautery. This is a technique where the warts are destroyed by burning.
A laser. This is another technique sometimes used to destroy the warts by burning.
Which is the best treatment?
Back to contentsEach treatment has pros and cons. The treatment decided upon depends on factors such as:
How many warts are present. For example, cryotherapy is usually only used for small-to-moderate numbers of warts.
Where the warts are. For example, some chemical treatments should not be used internally - such as on the neck of the womb (cervix), vagina or inside the back passage (anus).
Your preference. For example, whether a home-based or clinic-based treatment is preferred.
Whether you are pregnant. Some chemical treatments should not be used if you are pregnant.
The surgical treatments (cutting, freezing, burning treatments) are generally the most successful. However, they are not always appropriate. Warts may come back whichever treatment is used.
Do genital warts go away on their own?
Back to contentsOne option is not to have any treatment. Anogenital warts are not serious but can be unsightly. Some people prefer just to leave them alone. There is a good chance that they will go without any treatment. In fact, about one third of visible warts disappear by themselves over six months.
Can I give genital warts to my partner?
Back to contentsYour current sexual partner(s) may wish to be checked to see if they have warts or other STIs. It is a good idea to advise your current sexual partner, and any partners from the previous six months, to be checked.
Can genital warts cause cancer?
Back to contentsThe types of HPV that most commonly cause anogenital warts (types 6 and 11) do not increase your risk of cancer. HPV types 6 and 11 cause over 9 in 10 cases of anogenital warts. However, some other types of HPV do increase your risk of developing cancer. You may have more than one type of HPV infection at the same time (one type that causes anogenital warts and one type that may increase your risk of cancer).
It is known that most cases of cancer of the neck of the womb (cervix) are caused by HPV infection. So, it is particularly important that women with anogenital warts have cervical screening tests at the usual recommended times and do not put it off. You do not need to have cervical screening tests more regularly if you have anogenital warts. See the separate leaflet called Cervical Screening (Cervical Smear Test) for further details.
It also appears that the risk of other cancers is slightly higher if you have HPV infection. This includes other cancers in the genital area and some cancers of the mouth, throat and neck.
How to prevent genital warts
Back to contentsCondoms
Condoms (male or female) may prevent genital warts from being passed on to new sexual partners who are not infected. However, using a condom every time does not completely protect you from getting HPV infection as the skin that is not covered by a condom can become infected. But condoms do help to protect against other STIs such as chlamydia and HIV. You should also use condoms whilst having oral sex and you should not share sex toys.
When you are being treated for warts, it is commonly advised that you should use condoms when you have sex, until the warts have completely gone.
HPV vaccine
In the UK, the Department of Health originally chose a type of vaccine (Cervarix®) that did not protect against the common strains of HPV that cause anogenital warts (types 6 and 11) in its national immunisation campaign. However, from September 2012 the vaccine used was changed to a type that covers HPV-6/11/16/18 (Gardasil®). Between 2021 and 2022 Gardasil was developed to protect against nine strains of HPV. This vaccine also protects against cervical cancer, vulval/vaginal cancer, anal cancer and cancer of the penis. See the separate leaflet called HPV Vaccine (Human Papillomavirus Immunisation) for further details.
It is hoped that by vaccinating teenage girls before they catch the HPV infection, the numbers of anogenital warts overall in years to come will be much reduced. This has already been shown to happen in countries such as Australia, which started vaccinating earlier.
What is the outlook?
Back to contentsMany anogenital warts clear up on their own without any treatment being needed. Up to a third of warts clear up within 3-6 months without treatment. If not, they can usually be cleared with treatment. However, in at least 1 in 4 cases, new warts develop at some time after successful treatment. This is usually because the same infection has re-activated, not because you have a newly acquired infection. If warts do come back, they can be treated in the same way.
HPV infection clears up in most people within two years of catching it, without any treatment.
Patient picks for Sexually transmitted infections

Sexual health
Trichomoniasis
Trichomoniasis is a sexually transmitted infection (STI) caused by a tiny germ called trichomonas vaginalis. It can lead to pain and discharge from the vagina or penis, but it often does not cause any symptoms. This means you can pass it on without knowing you have it.
by Dr Rachel Hudson, MRCGP

Sexual health
Mycoplasma genitalium
Mycoplasma genitalium (also called Mgen and sometimes seen as M. genitalium) is a sexually transmitted infection caused by a germ (bacterium). Mycoplasma genitalium transmission can occur when having sex with a person who already has the infection. Mgen is more common in young people and in people who do not use condoms during sex. It is often asymptomatic but it can cause serious health problems if left untreated. There are concerns that Mgen has the potential to become a 'superbug', which means a bacterium which is resistant to available antibiotic treatments.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Management of anogenital warts; British Association for Sexual Health and HIV (2015 -updated 2024)
- Genital warts - Images; DermNet NZ
- Leslie SW, Sajjad H, Kumar S; Genital Warts
- Find a sexual health clinic near you; NHS services
- Warts - anogenital; NICE CKS, May 2024 (UK access only)
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 27 Mar 2028
29 Mar 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.