Mpox virus
Monkeypox
Peer reviewed by Dr Rosalyn Adleman, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 8 Apr 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Mpox, previously known as monkeypox, is a viral infection caused by the mpox (monkeypox) virus. It is very similar to the smallpox virus but causes fewer deaths. It was previously thought not to be very infectious but it seems to be spreading more easily in recent years. There is an effective vaccine that works against smallpox which also works against mpox.
At a glance
Mpox is an infection caused by the mpox virus, previously known as monkeypox.
It can spread through close contact with an infected person, their rash, body fluids, or contaminated items.
Symptoms often include fever, headache, muscle aches, swollen lymph nodes, tiredness, and a rash.
The rash typically starts in the mouth, then spreads, developing into fluid-filled blisters that later crust and scab.
Most people recover on their own within three to four weeks.
If you suspect you have been exposed and develop symptoms, contact NHS 111 or a sexual health clinic.
In this article:
Video picks for Skin infections
Continue reading below
What is mpox?
Mpox
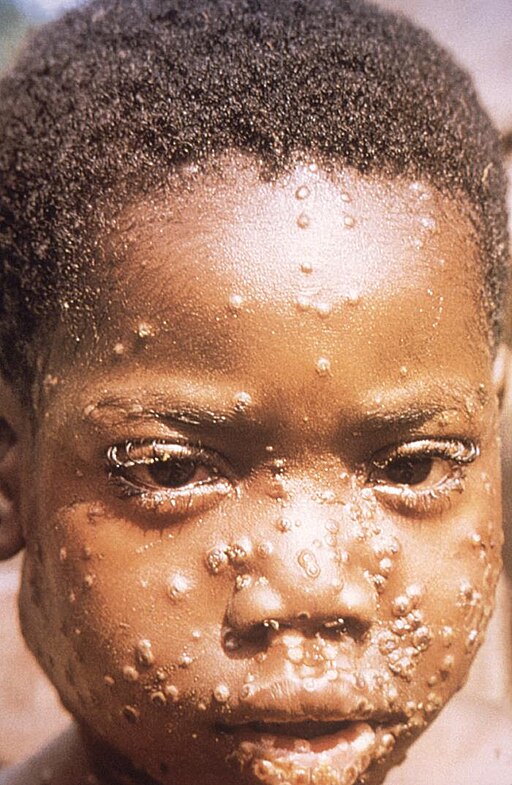
© CDC/ Brian W.J. Mahy, BSc, MA, PhD, ScD, DSc, Public domain, via Wikimedia Commons
Mpox, previously known as monkeypox, is an infection caused by the mpox virus. The virus belongs to the Orthopox virus family - this family also includes smallpox and other viruses. This virus is also known as zoonotic because it can be spread from animals to humans and from humans to animals.
Chickenpox is a different illness and the chickenpox virus belongs to a different family of viruses.
How do you get mpox?
Back to contentsPreviously it seemed that mpox was not very infectious and did not spread easily between people. However, more recently it is spreading more easily between people.
It can enter the body through broken skin (even if you cannot see it) or through the nose, eyes or mouth.
From person to person, you can get it from being in contact with:
An infected person who coughs or sneezes on to you.
The monkeypox (mpox) rash.
Fluids from the body of an infected person. This can happen during sexual or close skin-to-skin contact. Men who have sex with men appear to be particularly at risk.
Clothes, towels and bed linen that people with the illness have used.
Continue reading below
Mpox symptoms
Back to contentsIf you catch mpox, you will usually have an incubation period, which is the time between catching the virus and developing symptoms. In mpox this is usually between 7 to 14 days but it can be up to 21 days.
After this, mild symptoms can occur. Mpox symptoms include:
Muscle aches and pains.
Swollen lymph nodes (the lumps you sometimes feel in your neck when you have a sore throat). The main lymph nodes you may feel are in your neck, armpits and groin. Mpox can look like smallpox but people with smallpox do not get the swollen lymph nodes.
Tiredness.
About 1-2 days after the fever, the rash will start. It usually starts in your mouth and then spreads to your face and other parts of your body, including the soles of your feet and the palms of your hands. Some people only have a few skin lesions; other people may have several thousand.
You will be infectious until the scabs have dropped off and the skin underneath looks intact. This can be up to 4 weeks after the symptoms started.
Child with monkeypox (mpox) virus
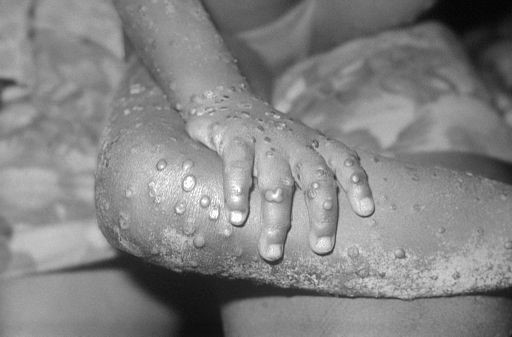
© Public domain, via Wikimedia Commons
Mpox rash
Back to contentsMpox can sometimes be confused with chickenpox. The rash looks quite similar to chickenpox, especially in the early stages. However, blisters filled with clear fluid later become filled with cloudy yellow-white liquid.
The rash starts as flat spots that become raised.
These then fill with liquid to become blisters.
The clear fluid turns cloudy, like pus.
They crust over.
They then form scabs which later fall off.
Monkeypox (mpox) in British patients 2022
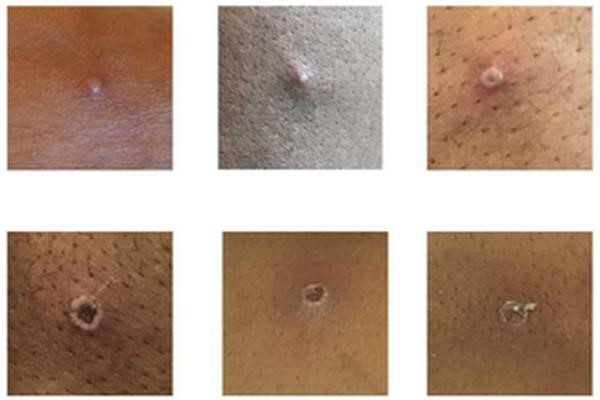
© UK government, OGL 3, via Wikimedia Commons
Do people recover from mpox?
Most people usually get better on their own after about three to four weeks.
Continue reading below
How is mpox diagnosed?
Back to contentsAs the rash and symptoms seen in monkeypox (mpox) are similar to those found in smallpox or chickenpox, it can initially be difficult to diagnose.
In smallpox or chickenpox, you do not get the swollen lymph glands you develop in monkeypox (mpox). However, other viral illnesses could still cause this symptom.
To be certain, a sample from the blister of the rash should be sent to a laboratory to be analysed. Here, the monkeypox (mpox) virus is grown and you can get a firm diagnosis. Blood samples are not helpful as it is difficult to separate the viruses or antibodies from other viruses in the family. Antibodies are proteins made by our immune system during infection. These help fight the virus. Antibodies also stay in the body for some time to help fight the infection more quickly if it comes back again.
Mpox treatment
Back to contentsAt the moment, there are no treatments specifically designed to treat monkeypox (mpox) in humans. As most people have mild symptoms, they do not need treatment apart from to help the symptoms of fever or pain.
If you have mpox it is advised to wear a mask and keep the skin lesions covered as much as possible, in order to protect people around you.
If unwell, there are some options such as:
Antiviral medicine
Cidofovir, tecovirimat and brinicidofovir are sometimes tried when people with mpox are very sick. They have not yet been shown to be effective. In animals, they have successfully helped fight the infection. Brinicidofovir has been shown to be safer than cidofovir. Cidofovir can cause problems in the kidneys.
Immunoglobulins
Immunoglobulins are antibodies. These are proteins that are made by the body's immune system to fight infection. We can also make treatments for some diseases by getting these antibodies from a number of people and creating a medicine.
Vaccinia immune globulin (VIG) is an immunoglobulin made from antibodies from people who have had the smallpox vaccine. It has, so far, not been shown to help people who have had complications from smallpox infection. It has not been used in people with mpox. Since smallpox and mpox are similar, it may be an option to be used one day.
Mpox vaccine
Back to contentsThe smallpox vaccine has been shown to work well to protect people against mpox. In 2019, a newer smallpox vaccine (a "third generation" vaccine) was developed and approved, and this works even better than the previous vaccines.
The newer vaccine is known as the Jynneos vaccine and can prevent mpox from developing. It also reduces the symptoms if someone who is vaccinated gets infected with monkeypox.
Mpox prevention
Back to contentsAvoid contact with animals that could have the virus (including animals that are sick or that have been found dead in areas where monkeypox (mpox) occurs).
Avoid contact with any materials, such as bedding, that have been in contact with a sick animal or person.
Avoid physical contact with anyone who has a rash which includes blisters or pus-filled spots.
Isolate infected people from others who could be at risk for infection.
Wash your hands with soap and water or use an alcohol hand gel.
If you suspect you may have been exposed to monkeypox (mpox) and develop symptoms (especially swollen glands and a rash), contact NHS 111 (or your local sexual health clinic) by phone as soon as possible.
Mpox and pregnancy
Back to contentsThere have not been many studies looking at what happens to women who become infected with mpox whilst pregnant. There have been 7 studies but only looking at 32 women. The results of the pregnancies were only described in 12 of these cases; in half of these, the baby died.
From previous studies looking at smallpox in pregnancy, there were high rates of miscarriage and stillbirths; pregnant women often developed more severe disease than non-pregnant women. It is thought likely that mpox will behave similarly to smallpox in pregnant women.
Frequently asked questions
Back to contentsHow and where did mpox start?
Mpox (monkeypox) was first found in an outbreak in monkeys used for research that were being shipped from Singapore to Denmark in 1958. This is why it was initially called monkeypox.
The first confirmed case of a human contracting monkeypox was in a child in the Democratic Republic of Congo (DRC) in 1970. It was first thought that this child had smallpox as the symptoms were so similar. Since then, there have been a few outbreaks of the virus but mainly in African countries. Most outbreaks have been in DRC and Nigeria. It is thought monkeypox (mpox) normally lives in rats, mice and squirrels in Africa.
It is rare to have outbreaks outside Africa. However, in 2003, there were a few cases in the USA, with humans and prairie dogs infected. All made a full recovery. Between 2018 and 2021, there had only been seven cases in the UK.
In 2022, there was a significant outbreak of mpox which involved outbreaks in multiple countries on different continents. Most cases occurred in men who had sex with men, although cases were seen in other people as well. There were 3732 cases in the UK in 2022. There were 429 cases of mpox in the UK in 2023 and 2024.
Why are there more cases of mpox now?
Mpox (monkeypox) is related to the smallpox virus. Over 50 years ago, there was a huge drive to get rid of smallpox. Everyone was offered the smallpox vaccine. This vaccine also helped in reducing the infections of mpox (monkeypox) as both viruses are similar. By 1980, there were no further people getting smallpox.
Over time, people have stopped being vaccinated against smallpox as the virus no longer exists. This has meant people, mainly children and those under the age of 40 or 50, have not had the smallpox vaccine. These people are now at higher risk of catching mpox if they come into close contact with an animal or person who has it.
Also, viruses develop over time. Viruses develop to become more infectious but less deadly. This is because viruses spread more easily, the more infectious that they are but, if they cause too many deaths, there is a risk that they will die out. New strains of viruses that are descended from the same ancestors are called "clades" and it is thought that the 2022 outbreak of mpox (monkeypox) was a new clade.
Is monkeypox deadly?
The death rate of mpox (monkeypox) can change depending on the strain of the mpox virus you have. The West African strain can cause 1 death for every 100 people who have the illness. The Congo Basin (central African) strain causes about 1 death in every 10 people who have been infected.
There can be complications that can make people more ill. People with weakened immune systems such as those on chemotherapy can have complications from the illness. They may need treatment in a hospital. Complications include:
Chest infections such as pneumonia.
Sepsis(infection into the bloodstream and throughout the body).
Encephalitis (infection in the brain).
Infection of the eye which can cause loss of vision.
Patient picks for Skin infections

Infections
Chickenpox in adults and teenagers
Chickenpox causes spots (a rash) and can make you feel unwell. Symptoms tend to be worse in adults than in children. Treatments can ease the symptoms until the illness goes. An antiviral medicine may limit the severity of the illness if the medicine is started within 24 hours of the rash first starting. Full recovery is usual. Serious complications are rare, but are more common in adults than in children. They are more likely to occur in pregnant women and in people with a weakened immune system, such as those on chemotherapy. If you are pregnant and have not had chickenpox (or been immunised) and come into contact with a person with chickenpox - see your doctor urgently, as treatment may prevent chickenpox from developing.
by Dr Colin Tidy, MRCGP

Infections
Cat scratch disease
Cat scratch disease is a bacterial infection caused by cat scratches or bites. It causes swollen lymph nodes and other symptoms such as a fever. It usually goes away without treatment, but antibiotics are often used to help clear the infection quicker.
by Dr Doug McKechnie, MRCGP
Further reading and references
- Monkeypox; GOV.UK (May 2022)
- Marlyn Moore, Farah Zahra; Monkeypox, National Library of Medicine, February 2022.
- Monkeypox; Centers for Disease Control and Prevention
- Monkeypox; Dermnet NZ
- Monkeypox - United Kingdom of Great Britain and Northern Ireland; World Health Organization, May 2022
- Mpox in Pregnancy — Risks, Vertical Transmission, Prevention, and Treatment; J Nachega et al; The New England Journal of Medicine
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Rosalyn Adleman, MRCGP
MRCGP
Dr Rosalyn Adleman, is an NHS GP working in north London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 7 Apr 2028
8 Apr 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.