Cystoscopy
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 10 Aug 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
A cystoscopy is a procedure which looks into the bladder with a special telescope called a cystoscope.
Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor or local hospital.
At a glance
A cystoscopy uses a thin telescope to look inside the bladder via the urethra.
It can diagnose frequent urine infections, blood in urine, or persistent pain when urinating.
A cystoscopy can also treat conditions like bladder stones or small bladder tumours.
The procedure usually takes 5-10 minutes and is often done while you are awake.
You might feel a mild burning or frequent need to urinate for a day after.
Seek medical help if pain or bleeding is severe or lasts over two days, or if you get a fever.
In this article:
Video picks for Urine and bladder tests
Continue reading below
Why is a cystoscopy done?
To help with diagnosis
A cystoscopy may be done to help to find the cause of symptoms such as:
Unusual cells found in a urine sample.
Persistent pain when passing urine.
Difficulty in passing urine - which may be due to prostate enlargement or a narrowing (stricture) of the urethra.
Cystoscopy may also be done to monitor progress of conditions. For example, some people have a routine cystoscopy every now and then after treatment for a bladder tumour. This helps to detect any early recurrence which can be treated before it spreads further.
To treat certain conditions, or to do certain procedures
By using various instruments which are passed down the side channels a doctor can:
Remove bladder stones. If a stone is lodged higher - in a ureter - the doctor may extend the cystoscope up into a ureter. The ureters are the tubes that drain urine from the kidneys to the bladder.
Remove small lumps (polyps) or tumours from the lining of the bladder.
Insert a small tube (stent) into a narrowed ureter. This helps the flow of urine if there is a narrowing.
Perform a special X-ray of the ureters and kidneys. A doctor can inject a dye into the ureters up towards the kidney. This shows up on X-ray pictures and helps to show problems of the kidney or ureter.
Remove the prostate gland (by using a special type of cystoscope which 'chips' away at the prostate gland bit by bit).
What is a cystoscope?
Back to contentsA cystoscope is a thin telescope which is passed into the bladder via the urethra, the tube that takes urine from the bladder to the outside of the body. There are two types. The cystoscope can be looked down but it also transmits pictures to a computer screen so they can be seen by other members of the team. Both types of cystoscope have side channels where various thin instruments can be passed down. For example a small sample (biopsy) may be taken from the bladder wall using an instrument which can pinch tissue and carry it back down the side channel.
Continue reading below
Types of cystoscopy
Back to contentsA flexible cystoscope is the most commonly used. It is a thin, flexible, fibre-optic telescope which is about as thick as a pencil. As it is flexible, it passes easily along the curves of the urethra. The flexible tip can also be moved easily so that the whole of the bladder lining can be seen.
Flexible cystoscope
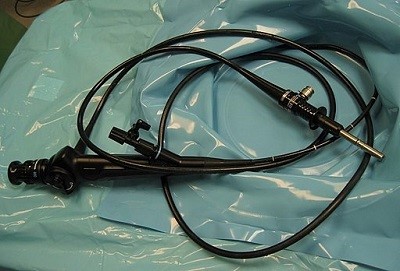
© By Michael Reeve, via Wikimedia Commons
A rigid cystoscope is a thin, solid, straight telescope. It allows a greater variety of devices to pass down the side channels so can be used for a wider variety of procedures.
Diagram of a rigid cystoscope and how a cystoscopy is performed
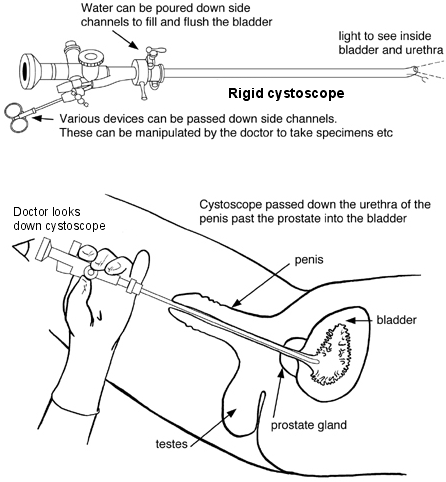
Cystoscopy procedure
Back to contentsCystoscopy is usually done as an outpatient procedure. This means people go home the same day and aren't required to stay overnight. It is usually done whilst awake. Some people are given a sedative to help them to relax.
The opening to the urethra (at the end of the penis, or the outside of the vagina) and the nearby skin will be cleaned. Some 'jelly' is then squirted into the opening of the urethra. The jelly usually contains a local anaesthetic to numb the lining of the urethra. This helps the cystoscope to pass into the urethra with as little discomfort as possible.
Male and female cystoscopy
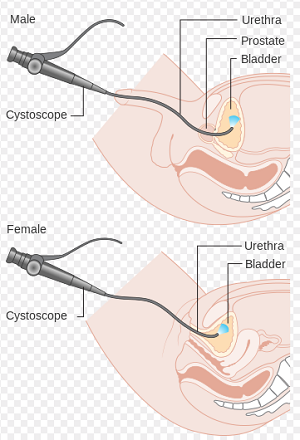
The cystoscope is then gently pushed up into the bladder and the lining of the urethra and bladder is carefully examined. Sterile water is passed down a side channel in the cystoscope to fill the bladder slowly. This makes it easier to see the lining of the bladder and the bladder wall. As the bladder fills it causes the feeling of a need to pass urine which may be uncomfortable.
The cystoscope is then gently pulled out. If a biopsy was taken, the sample would be sent away to be tested and looked at under a microscope. It can take several weeks for the report of the biopsy to come back to the doctor.
In some cases a general anaesthetic is given when a cystoscopy is done, particularly if a rigid cystoscope is used. In some cases a spinal anaesthetic is given which numbs all the lower half of the body.
Continue reading below
How long does a cystoscopy take?
Back to contentsA cystoscopy takes about 5-10 minutes if it is just to look inside the bladder. It may last longer if a procedure is being performed - for example, taking a sample (biopsy) from the lining of the bladder.
Is a cystoscopy painful?
Back to contentsCystoscopies are not usually painful, particularly as local anaesthetic is used to insert the cystoscope. They can be uncomfortable, especially when the bladder has been filled with water.
Complications of a cystoscopy
Back to contentsMost cystoscopies are done without any problem.
For the following 24 hours there may be a mild burning sensation when passing urine and a feeling of a need to pass urine more often than usual. The urine may also look pink due to mild bleeding, particularly if a biopsy was taken.
Occasionally, a urine infection develops shortly after a cystoscopy. This can cause a high temperature (fever) and pain on passing urine.
Rarely, the cystoscope may damage or perforate the bladder. After having a cystoscopy, medical advice should be sought if:
Pain or bleeding is severe.
Pain or bleeding lasts longer than two days.
Symptoms of infection develop, such as a fever.
Preparing for a cystoscopy
Back to contentsThere are not usually any particular preparations needed before a flexible cystoscopy. Usually it is possible to eat and drink as normal beforehand. There is no need to empty the bladder. A rigid cystoscopy normally requires a general anaesthetic so guidance will be given about when to stop eating and drinking and what to do.
After a cystoscopy
Back to contentsAfter a flexible cystoscopy, it is usual to need to empty the bladder urgently and then to go home without any need for additional support. After a rigid cystoscopy, a catheter may be used to empty the bladder and the normal advice would be given about having a general anaesthetic (to wait in the hospital for a few hours to recover, to be unable to drive home, to need support at home for 24 hours).
Patient picks for Urine and bladder tests

Tests and investigations
Intravenous urography
Intravenous urography is a test that uses X-rays and a special dye to help assess your kidneys, ureters, bladder and urethra. Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor or local hospital.
by Dr Doug McKechnie, MRCGP
Tests and investigations
Midstream specimen of urine
A midstream specimen of urine (MSU or MSSU) is usually tested to look for infection, although in some cases, illness other than infection might be diagnosed based partly on what is seen in an MSU.
by Dr Rachel Hudson, MRCGP
Frequently asked questions
What is the urethra?
The urethra is the tube that carries urine from the bladder to the outside of the body. A cystoscope is passed into the bladder through this tube during the procedure.
How is a biopsy taken during a cystoscopy, and how long until I get the results?
During a cystoscopy, a small sample (biopsy) can be taken from the bladder wall using an instrument passed down a side channel of the cystoscope. This instrument can pinch tissue and carry it back. After the sample is taken, it's sent for testing and examined under a microscope. It can take several weeks for the report of the biopsy to be sent back to your doctor.
Will I be given anything to help with pain during the cystoscopy?
Yes, a local anaesthetic jelly is usually squirted into the opening of the urethra before the cystoscope is inserted. This numbs the lining of the urethra to help the cystoscope pass with as little discomfort as possible. Some people may also be given a sedative to help them relax during the procedure.
What should I do if my symptoms like burning or bleeding continue for more than two days after the procedure?
You should seek medical advice if pain or bleeding is severe or lasts longer than two days after a cystoscopy. It's also important to contact a doctor if you develop symptoms of an infection, such as a fever.
How do I prepare for a flexible cystoscopy compared to a rigid one?
For a flexible cystoscopy, you typically don't need any special preparations and can eat and drink as normal beforehand, with no need to empty your bladder. However, a rigid cystoscopy usually requires a general anaesthetic, so you would receive specific instructions on when to stop eating and drinking and what else you need to do to prepare.
What happens immediately after a flexible cystoscopy?
After a flexible cystoscopy, it's common to feel an urgent need to empty your bladder. You can usually go home without needing additional support. For rigid cystoscopies, different advice applies due to the general anaesthetic.
Further reading and references
- Zhang ZS, Wang XL, Xu CL, et al; Music reduces panic: an initial study of listening to preferred music improves male patient discomfort and anxiety during flexible cystoscopy. J Endourol. 2014 Jun;28(6):739-44. doi: 10.1089/end.2013.0705. Epub 2014 Mar 31.
- Gee JR, Waterman BJ, Jarrard DF, et al; Flexible and rigid cystoscopy in women. JSLS. 2009 Apr-Jun;13(2):135-8.
- Engelsgjerd JS, Deibert CM; Cystoscopy
- DeGeorge KC, Holt HR, Hodges SC; Bladder Cancer: Diagnosis and Treatment. Am Fam Physician. 2017 Oct 15;96(8):507-514.
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 8 Aug 2028
10 Aug 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.