Bladder cancer
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Rachel Hudson, MRCGPLast updated 30 Jun 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
The common early symptom of bladder cancer is blood in the urine. In most cases, the cancer is confined to the inside lining of the bladder. Treatment of these superficial bladder cancers is relatively easy and often curative.
If the cancer has spread into or through the muscle layer of the bladder wall then curative treatment is more difficult, but possible. If the cancer is not curative, treatment often slows the progress of the cancer, and alleviates symptoms
At a glance
Bladder cancer usually develops from cells lining the inside of the bladder.
The first symptom is typically painless blood in the urine, which needs medical checking.
Bladder cancer is common in the UK, with about 10,000 cases yearly.
Smoking is a key risk factor, linked to around half of all bladder cancers.
Diagnosis often involves a cystoscopy, where a doctor looks inside the bladder.
Treatment varies depending on whether the cancer is superficial or has invaded muscle.
In this article:
Video picks for Other cancer types
Continue reading below
What is bladder cancer?
In most cases in the UK, the bladder cancer develops from the transitional cells which line the inside of the bladder. This type of cancer is called transitional cell bladder cancer.
The rest of this leaflet only deals with the common type of bladder cancer - transitional cell bladder cancer.
Transitional cell bladder cancer is divided into two groups:
Superficial tumours. These occur in about 4 in 5 cases. These tumours are confined to the inner lining, or just below the inside lining, of the bladder. Sometimes the cells which form this type of cancer multiply to form little growths which stick out like warts from the inside lining of the bladder.
Muscle-invasive tumours. These occur in about 1 in 5 cases. These tumours have spread to the muscle layer of the bladder or right through the wall of the bladder.
The treatment and outlook for each of these two groups are very different. Superficial tumours rarely spread and can usually be cured. However, if left untreated, in some cases they can develop into muscle-invasive tumours.
Muscle-invasive tumours have a high chance of spreading to other parts of the body (they metastasise) and treatment has less chance of being curative.
See the separate leaflet called Cancer for more information about cancer.
Bladder cancer symptoms
Back to contentsBlood in urine
In most cases, the first symptom is to pass blood in your urine (haematuria). Haematuria caused by an early bladder tumour is usually painless. You should always see your doctor if you pass blood in your urine. The blood in your urine may come and go as the tumour bleeds from time to time. Blood in the urine does not mean you definitely have bladder cancer as there are other causes, such as a urine infection, but it is important to see your doctor to have it checked out.
Other symptoms
Some tumours may cause irritation of the bladder and cause symptoms similar to a urine infection. For example, passing urine frequently or pain on passing urine. If the cancer is a muscle-invasive type, and grows through the wall of the bladder, other symptoms may develop over time. For example, pain in the lower tummy (abdomen).
If the cancer spreads to other parts of the body, various other symptoms can develop.
Continue reading below
How common is bladder cancer?
Back to contentsBladder cancer is a common cancer; it is the seventh most common cancer in the UK. About 10,000 people develop bladder cancer in the UK each year. The most common type of bladder cancer in the UK is transitional cell bladder cancer, other types of bladder cancer are rare in the UK.
What causes bladder cancer?
Back to contentsA cancerous tumour starts from one abnormal cell. The exact reason why a cell becomes cancerous is unclear. It is thought that something damages or alters certain genes in the cell. This makes the cell abnormal and multiply out of control. See the separate leaflet called Causes of Cancer for more details.
In many cases, the reason why a bladder cancer develops is not known. However, there are factors which are known to alter the risk of bladder cancer developing. These include:
Increasing age. Most bladder cancers occur in people over the age of 50. It is rare in people aged younger than 40.
Smoking. Bladder cancer is 2-6 times more common in smokers than in non-smokers. Some of the chemicals from tobacco get into the body and are passed out in urine. These chemicals in the urine are damaging (carcinogenic) to the bladder cells. It is estimated that about half of bladder cancers are related to smoking.
Other chemicals. Certain workplace and environmental chemicals have been linked to bladder cancer - for example, substances used in the rubber and dye industries. Many of these chemicals are now banned in the UK. However, bladder cancer may develop as late as 10-25 years after exposure to certain chemicals. This means that some cases are still being diagnosed in people who worked with these chemicals years ago.
Gender. Bladder cancer is about three times more common in men than in women.
Ethnic background. Bladder cancer is more common in white people than in black people.
Previous radiotherapy or chemotherapy slightly increases the risk.
Schistosomiasis. This bladder infection, which is caused by a parasite in certain hot countries, increases the risk.
Repeated bouts of other types of bladder infection may also slightly increase the risk in some people.
Continue reading below
How is bladder cancer diagnosed?
Back to contentsUrine Microscopy
If you see blood in your urine, or it is picked up on a urine dipstick test, a sample is sent to the laboratory to confirm if red blood cells are visible under a microscope.
Cystoscopy
Cystoscopy is the main test done to confirm a bladder tumour. Having a cystoscopy entails a doctor or nurse looking into your bladder with a special thin telescope called a cystoscope. The cystoscope is passed into your bladder via your water pipe (urethra).
A cystoscopy which is done just to look into your bladder is normally carried out under local anaesthetic. If a procedure is done, such as removing a tumour via a cystoscope, a general anaesthetic is usually used.
During cystoscopy a doctor or nurse can:
See any areas on the lining of your bladder which look abnormal.
Take small samples (biopsies) of suspicious areas. A small sample of tissue is removed from a part of the body and then examined under the microscope to look for abnormal cells.
Remove a superficial tumour with instruments which can be passed down a side channel of the cystoscope.
See the separate leaflet called Cystoscopy for more details.
Special urine tests
Urine tests have been developed which can detect bladder cancer. For example, urine tests such as the UroVysion test, ImmunoCyt test and NMP-22 test. These tests detect chemicals, proteins and chromosomal changes in urine that are made by bladder cancer cells. However these tests are not routinely done, although their use is increasing in some hospitals. They can be used in some circumstances, to detect transitional cell carcinoma higher up the urinary system than the bladder, ie in the ureter (the tube that connects the kidney to the bladder on each side)
Ultrasound scan
This is a safe and painless test which uses sound waves to create images of organs and structures inside your body. An ultrasound scan may be used to diagnose a bladder cancer.
CT scan (computerised tomography)
Another test called CT urogram is a special type of CT scan that obtains pictures of your urinary tract. This is sometimes done to look for a bladder tumour.
Editor’s note
Dr Krishna Vakharia, 16th October 2023
The National Institute for Health and Care Excellence (NICE) has recommended that a person should receive a diagnosis or ruling out of cancer within 28 days of being referred urgently by their GP for suspected cancer.
Assessing the extent and spread of bladder cancer
Back to contentsIf initial tests confirm that the cancer is a superficial tumour then no further tests may be necessary. Superficial bladder tumours have a low risk of spread to other parts of the body.
However, if you have a muscle-invasive tumour, further tests may be advised to assess if the cancer has spread. For example, a CT scan, a magnetic resonance imaging (MRI) scan or other tests. This assessment is called staging of the cancer.
The aim of staging is to find out:
How much the tumour in the bladder has grown, and whether it has grown to the edge or through the outer part of the bladder wall.
Whether the cancer has spread to local lymph nodes.
Whether the cancer has spread to other areas of the body (metastasised).
Cancer stages
By finding out the stage of the cancer, it helps doctors to advise on the best treatment options. It also gives a reasonable indication of outlook (prognosis). See the separate leaflet called Stages of Cancer for more details.
How fast does bladder cancer spread?
Transitional cell cancer usually doesn't spread quickly. If it is superficial when diagnosed, treatment can prevent spread effectively.
Superficial/non-invasive bladder tumours are staged, depending on how big/thick they are, and classified as low, medium or high risk, depending on how likely they are to spread. This staging will help to decide which treatment(s) are required.
Treating superficial bladder tumours
Back to contentsRemoval of the tumour
Most superficial bladder tumours are removed by a specialist with the aid of a cystoscope (described earlier). This is called transurethral resection (TUR), as the tumour is removed (resected) via a cystoscope which is passed up the water pipe (urethra). It does not involve an operation to cut into the bladder. Thin instruments can be passed down a side channel of the cystoscope to remove the tumour.
Immediate chemotherapy
Following a TUR, it is usual to have one dose of chemotherapy in the bladder (intravesical chemotherapy). This is usually done within 24 hours of having a TUR. It involves inserting a liquid into the bladder via a tube (catheter) which then remains for a few hours.
The liquid contains a chemotherapy medicine. Chemotherapy medicines kill cancer cells or stop them from multiplying. The aim is to kill any cancer cells that have been left behind following the TUR.
Studies have shown that one dose of intravesical chemotherapy reduces the chance of the tumour returning in the future. See the separate leaflet called Chemotherapy for more details.
Further chemotherapy/immunotherapy
The tumour that is removed during a TUR is examined under the microscope. This enables the exact stage and type of the tumour to be determined. Depending on the stage and type of the cancer, further intravesical chemotherapy may be advised.
This is done by using a catheter (as described above) and may be done every 1-4 weeks for several months. The aim is to be as certain as possible that all cancer cells are killed, which reduces the chance of the cancer returning.
The most commonly used medicine for further chemotherapy is called BCG. This is actually a vaccine which is used to prevent tuberculosis (TB). It is not clear how it works for bladder cancer.
It may stimulate the immune system in some way to clear any abnormal cells in the bladder lining. So, strictly speaking, treatment with BCG is immunotherapy. Other chemotherapy medicines are occasionally used instead of BCG.
Repeat checks
After a superficial tumour is removed, you will need a cystoscopy every so often. A return of a tumour occurs in some cases, and routine check cystoscopies will detect these at an early stage. If one returns, it can be treated again.
The time interval between check cystoscopies is every three months at first. It then becomes longer if your bladder remains free of tumour at each check. You may need a check cystoscopy every now and then for several years to make sure the tumour has not returned.
As mentioned above, urine tests have been developed to diagnose bladder cancer. If trials are successful, a urine test may become the way to check if a tumour has returned, rather than having a cystoscopy.
Treating muscle-invasive tumours
Back to contentsTreatment options that may be considered include surgery, chemotherapy and radiotherapy. The treatment advised for each case depends on various factors such as the stage of the cancer (how large the cancer is and whether it has spread), and your general health.
You should have a full discussion with a specialist who knows your case. They will be able to give the pros and cons, the likely success rate, the possible side-effects and other details about the possible treatment options for your type of cancer.
You should also discuss with your specialist the aims of treatment. For example:
Treatment may aim to cure the cancer. Some bladder muscle-invasive cancers can be cured, particularly if they are treated in the early stages of the disease. (Doctors tend to use the word remission rather than the word cured. Remission means there is no sign of the cancer following treatment. If you are in remission, you may be cured. However, in some cases a cancer returns months or years later. This is why doctors are sometimes reluctant to use the word cured.)
Treatment may aim to control the cancer. If a cure is not realistic, with treatment it is often possible to limit the growth or spread of the cancer so that it progresses less rapidly. This may keep you free of symptoms for some time.
Treatment may aim to ease symptoms. If a cure is not possible, treatments may be used to reduce the size of a cancer, which may ease symptoms such as pain. If a cancer is advanced then you may require treatments such as painkillers or other treatments to help keep you free of pain or other symptoms.
Cystectomy
A surgical operation to remove your bladder (a cystectomy) is the most common treatment. This is a major operation. Before surgery you need a full discussion with a surgeon to understand the implications of the operation planned. For example, you will need an alternative way of passing urine if you have your bladder removed.
One way for this is by a urostomy. This involves a surgeon using a technique to arrange a system for urine to drain into a bag which you wear on the outside of your tummy (abdomen). An alternative operation may be possible where the surgeon creates an artificial type of bladder from a part of the gut.
A cystectomy can be undertaken by an open operation where you will have a scar on your abdominal wall or by keyhole surgery. Your surgeon will be able to discuss with you in detail which type of operation is most suitable for you.
Even if the cancer is advanced and a cure is not possible, some surgical techniques may still have a place to ease symptoms. For example, if the passage of urine is blocked by a tumour then placing a tube (catheter) or other techniques may be appropriate.
Radiotherapy
Radiotherapy is often used instead of surgery as a curative treatment. It can also be used for some people who have symptoms of pain or bleeding that are not improving. Radiotherapy is a treatment which uses high-energy beams of radiation which are focused on cancerous tissue. This kills cancer cells or stops cancer cells from multiplying. See the separate leaflet called Radiotherapy for more details.
Chemotherapy
Chemotherapy is a treatment of cancer by using anti-cancer medicines which kill cancer cells or stop them from multiplying. Prior to surgery or radiotherapy, a course of chemotherapy may be advised. This is called neoadjuvant chemotherapy.
Chemotherapy used before surgery may improve the outlook (prognosis). In some cases a course of chemotherapy is given following surgery. See the separate leaflet called Chemotherapy for more details.
Immunotherapy
These are medicines given into the blood stream by an infusion. They prompt the immune system to recognise cancer cells and destroy them.
Nivolumab - given to people with muscle-invasive bladder cancer after bladder removal surgery (cystectomy), to reduce the risk of the cancer returning (called adjuvant treatment).
Avelumab - given as a maintenance treatment after chemotherapy to patients with metastatic cancer (cancer which has spread to other areas of the body) to extend their life.
Atezolizumab - given to patients with metastatic cancer if their cancer has progressed following chemotherapy.
What is the outlook for bladder cancer?
Back to contentsSuperficial bladder tumours
There is a good chance of a cure with treatment. Also, routine checks every few months following treatment will often detect returning tumours early and treatment can be repeated as necessary.
Muscle-invasive bladder tumours
A cure is less likely than with a superficial tumour. As a rule, the earlier the stage of the tumour, the better the chance of a cure with the treatments listed above. However, even if it is not cured, treatment can often slow down the progression of the cancer.
Can you prevent bladder cancer?
Back to contentsAccording to Cancer Research UK, 49% of cases of bladder cancer in the UK are preventable. The vast majority of these are caused by smoking, so if you are a smoker, stopping smoking is the most effective way to prevent bladder cancer.
Other ways to prevent bladder cancer are avoiding exposure to chemicals in the workplace, and avoiding exposure to large amounts of ionising radiation.
What is the bladder?
Back to contentsThe urinary tract
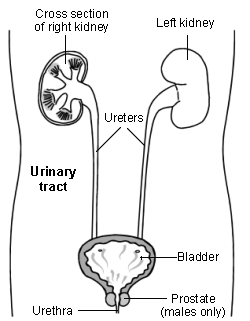
The bladder is part of the urinary tract. It is at the bottom of the abdomen. It fills with urine and we pass urine out through a tube called the urethra. The urethra passes through the prostate gland and penis in men. The urethra is shorter in women and opens just above the vagina.
Cells that line the inside of the bladder are called transitional cells or urothelial cells. The outer part of the bladder wall contains a thick layer of muscle tissue which contracts from time to time to push out the urine.
Patient picks for Other cancer types

Cancer
Kidney cancer
Most cases of kidney cancer develop in people between the ages of 60 and 70 although it can affect any age group. The most common early symptom is blood in the urine. If kidney cancer is diagnosed at an early stage, there is a good chance of a cure. A description of what kidneys are and how they work is at the bottom of this article.
by Dr Philippa Vincent, MRCGP

Cancer
Primary bone cancer
Primary bone cancer occurs where a cancer originates in a bone. It is a rare type of cancer. There are several different types. Treatments which may be considered include surgery, chemotherapy and radiotherapy. The type of treatment used and the outlook depend on various factors including the type, site and stage of the cancer.
by Dr Rosalyn Adleman, MRCGP
Frequently asked questions
What is the likelihood of my bladder cancer returning after treatment?
If you have a superficial bladder tumour, routine checks every few months after treatment are put in place because there is a chance the tumour can return. These checks help to detect any new tumours early so they can be treated again if necessary.
Are there different kinds of bladder cancer?
Yes, there are different kinds. In the UK, most cases develop from transitional cells lining the bladder, called transitional cell bladder cancer. This type is further divided into superficial tumours, which are confined to the inner lining, and muscle-invasive tumours, which have spread to the bladder's muscle layer or through its wall. Other types of bladder cancer are rare in the UK.
What happens if a superficial tumour develops into a muscle-invasive tumour?
If a superficial tumour, which is usually curable, is left untreated, it can sometimes develop into a muscle-invasive tumour. Muscle-invasive tumours have a higher chance of spreading to other parts of the body, and the treatment for them is less likely to be curative compared to superficial tumours.
Why would my doctor use a tuberculosis vaccine to treat bladder cancer?
The medicine BCG, which is a vaccine for tuberculosis, is commonly used for further chemotherapy in the bladder (intravesical chemotherapy). It's not fully understood how it works for bladder cancer, but it's thought to stimulate the immune system to clear abnormal cells in the bladder lining. This type of treatment is often referred to as immunotherapy.
Can bladder cancer be cured?
For superficial bladder tumours, there is a good chance of a cure with treatment. For muscle-invasive tumours, a cure is less likely than with superficial tumours, but the earlier the stage of the tumour, the better the chance of a cure. Even if a cure isn't possible, treatment can often slow down the progression of the cancer and help manage symptoms.
What is the typical age range for people who get bladder cancer?
Most bladder cancers occur in people over the age of 50. It is rare in people younger than 40.
Can I prevent bladder cancer?
According to Cancer Research UK, about 49% of bladder cancer cases in the UK are preventable. The most effective way to prevent it, especially if you smoke, is to stop smoking. Other preventative measures include avoiding exposure to certain chemicals in the workplace and limiting exposure to large amounts of ionising radiation.
Further reading and references
- Urinary incontinence in neurological disease: assessment and management; NICE Clinical Guideline (August 2012 - last updated October 2023)
- Bladder cancer: diagnosis and management of bladder cancer; NICE Guideline (February 2015)
- Bellmunt J, Orsola A, Leow JJ, et al; Bladder cancer: ESMO Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2014 Sep;25 Suppl 3:iii40-8. doi: 10.1093/annonc/mdu223. Epub 2014 Aug 5.
- Non-muscle-invasive Bladder Cancer; European Association of Urology Guidelines (2016)
- Muscle-invasive and Metastatic Bladder Cancer; European Association of Urology Guidelines (2016)
- Bladder cancer statistics; Cancer Research UK.
- Avelumab for maintenance treatment of locally advanced or metastatic urothelial cancer after platinum-based chemotherapy; NICE Technology appraisal guidance, May 2022
- Nivolumab for adjuvant treatment of invasive urothelial cancer at high risk of recurrence; NICE Technology appraisal guidance, August 2022
- van der Heijden MS, Loriot Y, Duran I, et al; Atezolizumab Versus Chemotherapy in Patients with Platinum-treated Locally Advanced or Metastatic Urothelial Carcinoma: A Long-term Overall Survival and Safety Update from the Phase 3 IMvigor211 Clinical Trial. Eur Urol. 2021 Jul;80(1):7-11. doi: 10.1016/j.eururo.2021.03.024. Epub 2021 Apr 23.
Continue reading below
About the authorView full bio

Dr Rachel Hudson, MRCGP
General Practitioner and Medical Author
MBChB, MRCGP (2008), BSc (Medical Science), DFSRH, DRCOG, DCH
Dr Rachel Hudson, is an NHS GP working in the North West of England.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
30 Jun 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.