Folliculitis
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 15 Sept 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Folliculitis means inflammation of the hair follicles of the skin. Most of the skin is covered with tiny hairs which grow out of hair follicles. In folliculitis, many hair follicles in one area of the skin are affected.
At a glance
Folliculitis is inflammation of the hair follicles, which causes red bumps on the skin.
Symptoms can include pus-filled spots, yellow crusts, pain, heat, and itching.
It can occur anywhere on the body where hair grows, such as the face, scalp, or legs.
Common causes include bacterial infection, shaving irritation, and blocked hair follicles.
Most mild cases clear up on their own within 7 to 10 days without specific treatment.
Seek medical help if the infection spreads deeper or to the surrounding skin.
In this article:
Video picks for Hair and scalp problems
Continue reading below
What is folliculitis?
Folliculitis means inflammation of the hair follicles. Folliculitis can be a mild, short-lived condition or a severe long-term problem. Folliculitis can occur anywhere on hair-bearing skin. There are a number of causes of inflammation which can result in folliculitis.
Rash of folliculitis
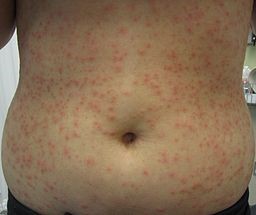
© James Heilman, MD, CC BY-SA 3.0, via Wikimedia Commons
Folliculitis symptoms
Back to contentsWhen hair follicles become infected or inflamed they swell causing a red bump on the skin.
Sometimes the affected follicles fill with pus, covering the affected skin with small, rounded, yellow-red spots (pustules).
Affected skin may develop a crust, which can be yellow or golden coloured due to infection.
The affected skin can feel painful, hot and may be itchy.
Continue reading below
Folliculitis locations
Back to contentsFolliculitis can be found everywhere where hair grows but the following areas are particularly common:
Buttocks.
Legs.
Back.
Chest.
Face.
Scalp.
Types of folliculitis
Back to contentsBacterial folliculitis
This is the commonest type of folliculitis and usually arises from the typical bacteria which normally live on the skin causing an infection in the hair follicles. It is very common and easily treated with antibiotics if it is significant enough to need treatment. Often it will settle on its own without treatment.
There are a few specific types of folliculitis:
Sycosis barbae
This is the medical name for a long-term (chronic) folliculitis in the beard area of the face. The skin is painful and crusted, with burning and itching on shaving. Numerous pustules develop in the hair follicles. It can be difficult to treat and some men grow a beard to solve the problem.
Hot tub folliculitis
As the name suggests, this tends to affect people after using a hot tub. The hot water encourages a bacteria called Pseudomonas aeruginosa to grow (particularly if there is not enough chlorine in the water to keep it clean). This type of folliculitis is generally harmless and is prevented by proper maintenance of hot tubs. Showering after using the hot tub does not seem to reduce the chance of folliculitis. Antibiotics are not needed for hot tub folliculitis; it usually settles within 2 weeks.
Gram-negative folliculitis
This is a type of folliculitis that may occur after acne has been treated with long-term antibiotics. Gram-negative refers to a type of stain that is used in a laboratory to identify different types of bacteria.
Pseudo-folliculitis
Also known as "razor bumps", this is caused by inflammation from shaving and ingrowing hairs. Pseudo-folliculitis is more common in people with curly or Afro-Caribbean hair, as these hairs are more likely to curl back and grow into the skin. Ingrowing hairs can also be caused by dead skin cells blocking the hair follicle so the hair cannot exit the follicle.
Malassezia folliculitis
Also known as pityrosporum folliculitis, this is caused by yeasts which normally live on the skin but occasionally cause inflammation. Malassezia folliculitis is more common in adolescent boys and young men and is also more common in hot humid climates. Other things that make malassezia folliculitis more common are frequent use of sunscreen, excessive sweating, antibiotic use and the immune system being impaired.
Folliculitis
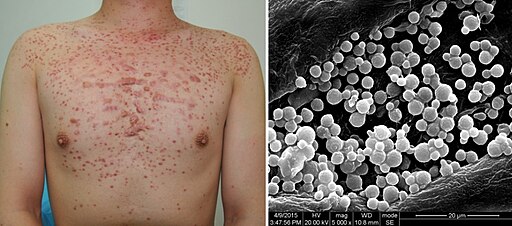
© Ran Yuping et al., CC BY-SA 3.0, via Wikimedia Commons
Eosinophilic folliculitis
This rare form of folliculitis is also known as eosinophilic pustular folliculitis or Ofuji disease. It causes itchy pustules and is more common in men than women. The pustules are usually seen on the head, neck and trunk and can persist for weeks or months. It may look like acne. It is associated with HIV but also occurs in people without HIV. Simple anti-inflammatory drugs have been reported to help in up to 7 out of 10 people with eosinophilic folliculitis. Antibiotics may also help.
Carbuncles
A carbuncle is a group of inflamed follicles close together which then join together into one hot red lump with pus coming out of several points. This can be very painful and antibiotics are often needed. Warm compresses may help avoid the need for antibiotics.
Furuncles (boils)
This is an infection deeper in the hair follicle which causes a small abscess just under the skin. It is hot and red. Antibiotics may be needed but warm compresses can often help.
Continue reading below
Causes of folliculitis
Back to contentsFolliculitis occurs at sites where hair follicles are inflamed. There are a number of causes:
Infection. Most folliculitis infections are caused by a bacteria called Staphylococcus aureus (S. aureus), which usually lives harmlessly on the skin. Occasionally other bacteria, fungi (Pityrosporum or Candida albicans) or parasites are the cause.
Physical irritation caused by shaving or friction.
Chemical irritation caused by chemicals applied to the skin.
Blockage of the hair follicle eg, by dead skin cells or thick creams.
Excessive sweating (hyperhidrosis) due to overactivity of the sweat glands.
Steroid creams.
Inflammatory skin conditions are an uncommon cause.
Complications of folliculitis
Back to contentsMost cases of folliculitis get better without any complications. Occasionally the following can occur:
Scarring of the skin.
Darkening of the affected skin (hyperpigmentation).
Hair loss at the affected site due to scarring of the skin.
Deep folliculitis. This occurs if the infection spreads deeper into the follicles causing a boil.
Cellulitis. This is when infection spreads into the surrounding skin, making it hot and red.
Medical advice should be sought if there is an infection which is spreading deeper or onto surrounding skin.
Diagnosing folliculitis
Back to contentsThere are no specific tests for folliculitis. Normally the diagnosis is obvious from the type of rash.
Occasionally a swab might help if there is discharge from the pustules.
Folliculitis treatment
Back to contentsIdentifying the cause of the folliculitis will help decide what will help. General measures include:
Avoiding things that aggravate the condition.
Taking a break from hair removal until the folliculitis has settled down.
Avoiding wearing tight clothes over the affected area, particularly if it causing sweating.
Keeping cool and keeping folliculitis exposed to the fresh air.
Not sharing towels, flannels or razors.
Applying an antibacterial moisturiser (emollient) and soap substitute. See below for more information.
Mild cases
Most cases of folliculitis are mild and do not need any treatment. It often clears without any treatment within 7-10 days.
It may be helpful to use:
A moisturiser (emollient) which contains an antibacterial agent - for example, Dermol® cream.
Lotion or Emulsiderm®.
These may help the folliculitis to clear more quickly and reduce the risk of it becoming worse. You can use one of these emollients as a soap substitute until the folliculitis has cleared (and long-term if needed). These can also be added to the bath or shower - specific bath or shower products are not needed.
If simple measures over a few days do not result in improvement of the folliculitis, medical advice should be sought for further advice and treatment.
Localised folliculitis
For localised areas of folliculitis, an antibiotic cream may be useful. Fusidic acid is a suitable antibiotic cream that can be applied 3-4 times per day to affected areas. If the folliculitis is thought to be fungal, a different treatment may be used.
More severe cases
If the folliculitis is more severe or widespread then a course of oral antibiotic tablets may be needed.
Recurrent or long-term (chronic) folliculitis
Recurrent folliculitis occurs when the infection keeps coming back, although it disappears with treatment. The gaps between episodes may get shorter and, eventually, chronic folliculitis is the result.
In these cases, a clinician may take a sample (swab) from the skin where the folliculitis is. This swab can show if an infection is responsible and identify which type of infection it is. The correct medication can then be used to try and eradicate the bacteria from the skin.
Preventing folliculitis
Back to contentsTo try and prevent folliculitis, the following actions may help:
Keeping skin clean, dry and free from abrasions or irritations.
Keeping skin well-moisturised.
Using clean, sharp razors and shaving in the direction of hair growth, or using an electric razor.
Using a shaving soap, gel or foam to lubricate the blades across the skin to help prevent nicks and cuts.
Using hair removal methods other than shaving.
Avoiding chemicals or items which irritate the skin.
Exfoliating regularly to remove dead skin cells.
Using antiseptic washes routinely is not generally recommended as they can make the skin sore and dry.
Is folliculitis contagious?
Back to contentsFolliculitis itself is not contagious. In hot-tub folliculitis, other people who have been exposed to the same hot tub are likely to develop folliculitis as well.
Patient picks for Hair and scalp problems

Skin, nail and hair health
Seborrhoeic dermatitis
Seborrhoeic dermatitis causes bad dandruff and sometimes a rash, commonly on the face and upper body. An anti-yeast (antifungal) shampoo and/or an antifungal cream will usually clear the dandruff and rash. The condition tends to come back (recur). If it recurs frequently, regular use of an antifungal shampoo and/or cream can help to keep it away.
by Dr Toni Hazell, MRCGP

Skin, nail and hair health
Telogen effluvium
Telogen effluvium (hair loss) is a condition where more than normal amounts of hair fall out. There is a general 'thinning' of the hair. Unlike some other hair and scalp conditions, it is temporary and the hair growth usually recovers.
by Dr Hayley Willacy, FRCGP
Frequently asked questions
Can certain clothes make folliculitis worse?
Yes, wearing tight clothes over the affected area, especially if it causes sweating, can aggravate folliculitis. It's recommended to avoid such clothing.
Are there any specific moisturisers or soap substitutes that can help with folliculitis?
Yes, an antibacterial moisturiser (emollient) such as Dermol® cream, lotion or Emulsiderm® can be helpful. These can also be used as a soap substitute or added to bath or shower water to help clear folliculitis and reduce the risk of it worsening.
How long does it usually take for mild folliculitis to clear up?
Most mild cases of folliculitis clear up on their own without any specific treatment within 7-10 days. However, if simple measures don't show improvement within a few days, it's advisable to seek medical advice.
What should I do if my folliculitis keeps coming back?
If your folliculitis is recurrent, meaning it keeps returning even after treatment, a clinician may take a sample (swab) from the affected skin. This can help identify the specific infection and allow for the correct medication to be used to try and eradicate the bacteria.
Is it better to shave or use other hair removal methods if I have folliculitis?
To help prevent folliculitis, it's recommended to use clean, sharp razors and shave in the direction of hair growth, or use an electric razor. Using shaving soap, gel, or foam can also help lubricate the skin. Alternatively, using hair removal methods other than shaving can also be considered.
Can I use antiseptic washes to prevent folliculitis?
Routine use of antiseptic washes is generally not recommended as they can make the skin sore and dry, which might not be beneficial for preventing folliculitis.
Further reading and references
- Folliculitis; DermNet NZ
- Folliculitis and boils (furuncles/carbuncles), Primary Care Dermatology Society (PCDS), 2016
- Winters RD, Mitchell M; Folliculitis. StatPearls, September 2019.
- Eosinophilic Pustular Folliculitis; DermNet
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Sept 2027
15 Sept 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.