Vitiligo
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 13 Nov 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Vitiligo causes white patches on the skin which vary in size and number. There are usually no other symptoms, but it can have a significant effect on mood and self-esteem. Affected areas of skin can be covered by skin camouflage creams. Treatment has improved in recent years and in some cases the pigment can be restored.
At a glance
Vitiligo is a skin condition where patches of skin lose their natural colour.
It happens because cells that make skin pigment are damaged or destroyed.
Vitiligo is not usually sore or itchy, but affected skin can burn easily in the sun.
It can start at any age, and about 1 in 100 people develop it.
Treatments can include creams, light therapy, or skin camouflage.
People with vitiligo may be more prone to certain other autoimmune conditions.
In this article:
Video picks for Other skin problems
Continue reading below
What is vitiligo?
Vitiligo is due to a lack of colour (pigment) in the affected areas of the skin. Vitiligo does not cause any other symptoms. However, the appearance of vitiligo can be distressing. This is particularly so for darker-skinned people where white patches are more noticeable.
What causes vitiligo?
Back to contentsAreas of skin with patches of vitiligo have no or very few melanocytes. The melanocytes are either damaged or destroyed in the body. Therefore, melanin cannot be made and the colour of the skin is lost. It is not known why the melanocytes go from affected areas of the skin.
They may be destroyed by the immune system or self-destruct for reasons not yet known. It is thought to be an autoimmune condition. This means that the immune system (which normally protects the body from infections) causes damage. In the case of vitiligo, it destroys the cells in the skin that make melanin.
Continue reading below
Understanding the layers of the skin
Back to contentsTo understand the cause of vitiligo, it is useful to have a basic understanding of the skin. The skin has two layers - the epidermis and the dermis. Beneath the dermis is a layer of fat and then the deeper structures such as muscles and tendons.
Skin diagram cross-section view
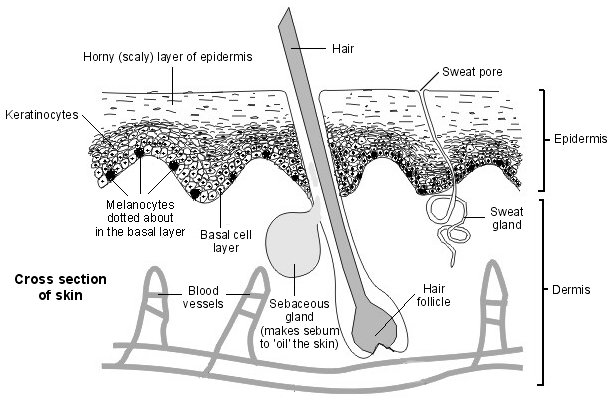
There are cells called melanocytes in the bottom of the epidermis which make a pigment called melanin. The melanin is passed to the nearby skin cells, which colours the skin and protects them from the sun's rays.
Melanin causes the skin to tan in fair-skinned people. Dark-skinned people have more active melanocytes. The melanocytes are stimulated to make more melanin when exposed to sunlight.
How common is vitiligo?
Back to contentsAbout 1 in 100 people develop vitiligo. Men and women are equally affected. It can develop at any age. However, it begins before the age of 20 years in about half of cases. There is some genetic factor involved and vitiligo may run in the family.
Nearly 1 in 3 affected people have some other family member who is also affected. Vitiligo is not infectious. It is not more common in any racial or ethnic groups. It is more obvious in people with darker skin.
Continue reading below
Where does vitiligo usually appear?
Back to contentsVitiligo on left hand
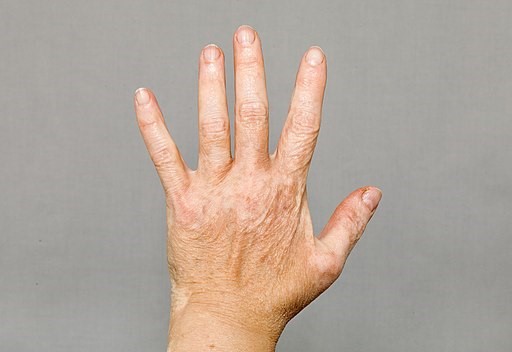
© Simone Trovato Monastra, CC BY-SA 4.0, via Wikimedia Commons
The most common areas of skin affected by vitiligo are:
Face.
Neck.
Hands.
Wrists.
Scalp.
However, any area of the skin can be affected. Other common sites include the nipples and genitals. Vitiligo can also affect areas where there are body folds, such as the armpits or groins. It may occur in places where the skin has been injured in the past (cuts, burns or other skin conditions).
It may be symmetrical in that patches may appear in similar places on each arm or leg. In the areas of the scalp that are affected, the hair too is affected, causing it to become grey or white. Hair of the body or eyes can also lose colour.
Very rarely, vitiligo can affect the whole body. This is called universal, or complete, vitiligo.
How quickly does vitiligo progress?
Back to contentsSmall areas of milky-white skin usually develop first. The contrast between vitiligo skin and normal skin varies. In fair-skinned people, it may only be noticeable in summer when normal skin tans. The contrast is more noticeable in darker-skinned people.
The course and severity of vitiligo vary from person to person. Sometimes a few small patches develop slowly and progress no further. Sometimes a number of patches develop quite quickly and then remain static for months or years without changing.
However, it is quite common for the white patches gradually to become bigger and for more patches to appear on other parts of the body. Large areas of the skin may eventually be affected.
There is no way of predicting how much of the skin will eventually be affected when the first patch develops. The white patches are usually permanent. Rarely, some patches of vitiligo may regain their colour (re-pigment) and return to normal.
Vitiligo symptoms
Back to contentsPeople with vitiligo are usually well. Vitiligo is not sore or itchy. However, the appearance of the skin can be distressing, particularly if the face or the hands are affected. There is no natural protection from the sun in affected areas of the skin. This means that skin affected by vitiligo burns much more easily than normal skin if exposed to sunlight.
Vitiligo treatment
Back to contentsAlthough there is no cure for vitiligo, there are treatments available which can help. Some people may not be concerned about the white patches of skin if they are in areas not noticeable to others.
Some treatments have been shown to slow down the progression of vitiligo; some treatments cause affected skin to return to normal in some cases.
No single treatment for vitiligo works well in all cases. The response to the various treatments is variable and can depend on the type of vitiligo. There are a number of treatments, and specialist advice may be needed to advise on the best one.
Skin camouflage
Skin camouflage uses special coloured cover creams that are put on the white patches of vitiligo. Skin camouflage does not alter the disease but improves the skin's appearance. The aim is to find a colour to match the colour of the skin.
Some special cover creams can be prescribed on the NHS. The creams can disguise vitiligo very well, which may greatly increase self-confidence. A GP may refer a person with vitiligo to the Changing Faces skin camouflage advice service (see below) to help find the right cream.
There are also self-tanning lotions available from pharmacies. These may also hide the vitiligo and can last several days before needing to be reapplied. However, they often do not provide an exact match for each skin colour.
They may be most useful for large areas of vitiligo where matching the colour exactly to nearby skin is not needed so much. Fake tans can also be useful for areas where camouflage is less effective (for example, the back of the hands).
Steroid cream
A steroid cream, used when a small patch of vitiligo first develops, may prevent a smaller patch from becoming bigger. Occasionally, skin colour may return over a treated area. Steroids work partly by suppressing the immune system (which probably attacks the melanocytes).
Treatments that may be considered by a skin specialist
Tacrolimus or pimecrolimus cream
Tacrolimus or pimecrolimus creams can be used as an alternative to steroid cream. They have been shown to restore skin colour to some people with vitiligo.
They also work by suppressing cells of the immune system in the skin. It seems to be most effective for vitiligo on the face. It can also be used on the skin of children.
PUVA treatment
PUVA stands for psoralen and ultraviolet A (UVA) light. It involves taking a special medicine (a psoralen) which makes the skin very sensitive to light.
This medicine can be in the form of a tablet or a cream. The skin is then treated with UVA light from a special machine in hospital. This treatment is very time-consuming.
Treatment is needed twice a week for up to two years. PUVA may cause side-effects such as sunburn-type reactions or skin freckling. If colour does return to the white patches there is still a chance that it may go white again at a later stage.
Narrowband UVB phototherapy
This is another light treatment which is now used more commonly than PUVA. It uses ultraviolet B (UVB) light. As with PUVA, treatment is twice a week but it is not necessary to take a medicine to sensitise the skin and the treatment sessions are much shorter.
It is less damaging to the skin than PUVA. It is useful when large areas are affected. Sometimes it is used in combination with tacrolimus or pimecrolimus cream.
Laser treatments
Laser treatment for vitiligo is currently not available under the NHS as there is no definite proof yet that it is effective.
Skin grafting
Grafting of normal skin to small patches of vitiligo has been tried. It is time-consuming and not always successful or available.
Other treatments
Complementary treatments
There is currently insufficient evidence to recommend any complementary treatments for vitiligo.
Treatment to remove colour from (de-pigment) the skin completely
In some people with extensive vitiligo, a treatment may be considered to make the remaining normal areas of skin go white.
This makes all the skin an even white colour so it all looks the same. This is done only after a full discussion with a specialist. The removal of all the skin pigment is permanent and it takes up to a year to complete.
General advice for people with vitiligo
Back to contentsWhite patches cannot tan; they can only burn. Therefore, skin sun protection is very important and sun should be avoided in the hottest times of the day. White patches should be covered with with clothes or a hat where possible, or with high-factor sunblock. For people with vitiligo, some brands of sunblock can be prescribed on the NHS by a doctor.
In fair-skinned people, avoiding tanning of normal skin can make patches of vitiligo much less noticeable.
It is important to avoid any injury to the skin when possible, as new white patches may develop in areas of injury.
Note: the use of sunbeds is not recommended. The ultraviolet radiation from sunbeds can damage the skin and people who use tanning devices are much more likely than average to be at risk of developing skin cancer (melanoma). Therefore, sunbeds should be avoided.
Complications of vitiligo
Back to contentsVitiligo itself does not develop into any other condition. However, other diseases caused by the immune system (autoimmune disorders) are slightly more common in people with vitiligo. Such disorders include:
A condition where the thyroid gland is overactive is particularly associated with vitiligo.
Low self-esteem
Most people with vitiligo do not have these but a doctor may suggest a blood test to rule them out,
Some people with vitiligo are embarrassed about their condition. This can lead to low self-esteem and even to depression. Some people find that counselling can be beneficial.
Joining a local support group can be a useful way to help understand more about this condition. The Vitiligo Society (see below) has more information on support options.
Your doctor may also recommend you have a blood test every year to check this has not developed.
Patient picks for Other skin problems

Skin, nail and hair health
Erythema nodosum
Erythema nodosum is a condition that causes red rounded lumps (nodules) to form just below the skin surface, most commonly on the shins. In most people, no specific cause or trigger can be found. But in some people a trigger (commonly a streptococcal infection or sarcoidosis) can be identified. Usually, the nodules heal within six to eight weeks with no treatment needed. However, it is important to look for a possible underlying trigger, as this may need treatment.
by Dr Hayley Willacy, FRCGP

Skin, nail and hair health
Port-wine stain
A port-wine stain is a differently coloured patch of skin that a baby is born with. It is usually over their face, neck or scalp, and looks pink or pale purple. It is often called a port-wine birthmark now.
by Dr Hayley Willacy, FRCGP
Frequently asked questions
Can vitiligo be completely cured?
There is currently no cure for vitiligo. However, several treatments are available that can help restore skin colour or slow down its progression for some people. The effectiveness of these treatments varies depending on the individual and the type of vitiligo.
If I have vitiligo, will my children also have it?
Vitiligo can have a genetic factor, and it sometimes runs in families. Nearly 1 in 3 affected people have another family member with the condition. However, it's not guaranteed that your children will develop it.
How can I protect my white patches of skin from the sun?
It's very important to protect the white patches of skin from the sun because they cannot tan and will burn easily. You should cover these areas with clothes or a hat where possible, or use a high-factor sunblock. Your doctor may be able to prescribe some brands of sunblock on the NHS.
Are there any natural or complementary treatments for vitiligo that work?
Currently, there isn't enough evidence to recommend any specific complementary treatments for vitiligo. It's best to discuss any treatment options with a skin specialist.
Does vitiligo cause any pain or itching?
No, vitiligo does not typically cause any physical symptoms like soreness or itching. The main impact is on the appearance of the skin, which can be distressing for some.
Is it possible for the white patches to regain colour naturally without treatment?
Yes, very rarely, some patches of vitiligo may regain their colour or re-pigment on their own and return to normal, but this is not common.
What should I do if vitiligo is affecting my self-esteem?
It is common for vitiligo to impact self-esteem and can even lead to depression. If you are struggling, counselling can be beneficial. Joining a support group, such as those recommended by The Vitiligo Society, can also be a useful way to connect with others and learn more about the condition.
Further reading and references
- Vitiligo Society UK
- Vitiligo; DermNet NZ
- Changing Faces
- Whitton ME, Pinart M, Batchelor J, et al; Interventions for vitiligo. Cochrane Database Syst Rev. 2015 Feb 24;(2):CD003263. doi: 10.1002/14651858.CD003263.pub5.
- Vitiligo; Primary Care Dermatology Society (PCDS)
- Vitiligo; NICE CKS, January 2022 (UK access only)
- Eleftheriadou V, Atkar R, Batchelor J, et al; British Association of Dermatologists guidelines for the management of people with vitiligo 2021. Br J Dermatol. 2022 Jan;186(1):18-29. doi: 10.1111/bjd.20596. Epub 2021 Sep 7.
- Fraczek A, Kasprowicz-Furmanczyk M, Placek W, et al; Surgical Treatment of Vitiligo. Int J Environ Res Public Health. 2022 Apr 15;19(8). pii: ijerph19084812. doi: 10.3390/ijerph19084812.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 11 Nov 2028
13 Nov 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.