Basal cell carcinoma
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 26 Nov 2021
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Non-melanoma skin cancer article more useful, or one of our other health articles.
In this article:
Continue reading below
What are basal cell carcinomas?
Basal cell carcinomas (BCCs) are slow-growing, locally invasive, malignant epidermal skin tumours. They are the most common skin cancer in humans and typically arise on sun-exposed skin. The tumour infiltrates local tissues through the slow irregular growth of subclinical finger-like outgrowths, and morbidity results from local tissue invasion and destruction, especially on areas of chronic sun exposure, such as the face, head and neck .
Metastasis is extremely rare with a metastasis rate of 0.0028% to 0.5%.1
Basal cell carcinomas were once known as rodent ulcers but this term is no longer frequently used.
Basal cell carcinoma symptoms
Back to contentsThe sun-exposed areas of the head and neck are the most commonly involved sites . Approximately 80% occur on the head and neck, with the rest mainly on the trunk and lower limbs.
Early lesions are often small, translucent or pearly and have raised areas with telangiectasia.
The classic basal cell carcinoma has an indurated edge and ulcerated centre. It is slow-growing but can spread deeply to cause considerable destruction.
Basal cell carcinoma - nodular type
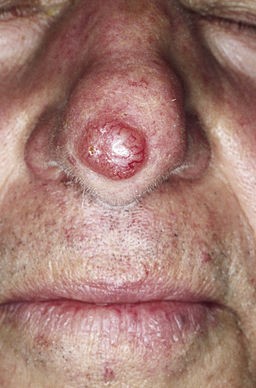
© M. Sand, D. Sand, C. Thrandorf, V. Paech, P. Altmeyer, F. G. Bechara, CC BY 2.0, via Wikimedia Commons
Continue reading below
How common are basal cell carcinomas? (Epidemiology)
Back to contentsBasal cell carcinoma predominantly affects white people and is less common in people with other skin types. The lifetime risk of BCC development in white men is 33-39% and in white women is 23-28%. 2
BCC is the most common malignancy worldwide and is showing a global increase in incidence. 1
There is a doubling in diagnoses every 25 years, some of which is due to better detection, but there is an increase in incidence due to increased life expectancy and more sun exposure.2
Risk factors for basal cell carcinomas1
Age. The risk increases with age. The median age at diagnosis is 68.
Gender. Men are more at risk than women, possibly due to an increased sun exposure.
Skin type. Skin type 1, found in people with red hair and freckles, is the highest risk for developing basal cell carcinomas.1
UV exposure. Exposure to the sun is the most significant risk factor for basal cell carcinomas. This is due to UV-mediated genetic mutations and inflammatory processes which promote cancer growth.2
Previous skin cancer. A previous diagnosis of basal cell or squamous cell carcinoma increases the risk of further basal cell carcinomas.
The chance of developing a second BCC within three years of the first presentation is between 33 and 70%. 3
Gorlin syndrome is a rare condition, occurring in approximately 1 in 50,000 people and is associated with multiple basal cell carcinomas as well as other anomalies.4
Other conditions associated with an increased risk of BCC include xeroderma pigmentosa and albinism.
Basal cell carcinoma subtypes5
Back to contentsNodular
Solitary, shiny, red nodule with large telangiectatic vessels.
Commonly on the face.
Cystic, pearly, telangiectasia.
May be ulcerated.
Micronodular and microcystic types may infiltrate deeply.
Superficial
Most common type in younger adults.
Erythematous well-demarcated scaly plaques, often larger than 20 mm at presentation. Central clearing and a thread-like border. A rolled edge can be seen if stretched. The lesion may bleed or weep.
Slow growth over months or years; usually not aggressive, rarely become invasive and extremely rarely metastasise. Less likely to erode and ulcerate than nodular basal cell carcinomas.
May be confused with Bowen's disease or inflammatory dermatoses.
Particularly responsive to medical rather than surgical treatment.
Morphoeic
Also known as sclerosing or infiltrative basal cell carcinoma.
Usually found in mid-facial sites.
More aggressive and have poorly defined borders.
Characterised by thickened yellowish plaques.
May have wide and deep subclinical extension.
Prone to recurrence after treatment.
Basosquamous
Mixed basal cell carcinoma and squamous cell carcinoma (SCC).
Potentially more aggressive than other forms of BCC.
Continue reading below
Differential diagnosis
Back to contentsNodular basal cell carcinoma:
Sebaceous hyperplasia.
Fibrous papule.
Superficial basal cell carcinoma:
Pigmented basal cell carcinoma (see the separate article Pigmented Skin Lesions):
Morphoeic basal cell carcinoma:
Scar tissue.
Referral
Back to contentsThe National Institute for Health and Care Excellence (NICE) recommends:6
Routine referral for people if they have a skin lesion that raises the suspicion of a BCC.
Only consider a suspected cancer pathway referral (for an appointment within two weeks) for people with a skin lesion that raises the suspicion of a BCC if there is particular concern that a delay may have a significant impact, because of factors such as lesion site or size.
Diagnosing basal cell carcinomas (investigations)1
Back to contentsDiagnosis is primarily by visual inspection.
Dermoscopy is very useful for diagnosing basal cell carcinomas.
A biopsy may be advised for further diagnosis where necessary.
All excised specimens should be sent for histopathological examination.
CT or MRI scan is indicated in cases where the tumour may have invaded major nerves, the orbit or the parotid gland or in those rare incidences where metastasis may have occurred.
Basal cell carcinoma treatment and management
Back to contentsA Cochrane review found that:7
Surgical interventions have the lowest recurrence rates.
There may be slightly fewer recurrences with Mohs' micrographic surgery over surgical excision for high-risk facial primary BCC.
Non-surgical treatments, when used for low-risk BCC, are less effective than surgical treatments, but recurrence rates are acceptable and cosmetic outcomes are probably superior.
Of the non-surgical treatments, imiquimod has the best evidence to support its efficacy.
Recurrent basal cell carcinoma is more difficult to cure than primary lesions .
Surgical treatment
Mohs' micrographic surgery is considered the gold standard treatment for basal cell carcinomas:1
Excision of the BCC is carried out in stages and each stage checked histologically.
It is advocated for use in cases where it is critical to obtain a clear margin while preserving the maximum amount of normal surrounding tissue, especially for recurrent and high-risk aggressive growth pattern BCCs such as morphoeic BCCs.
High-risk and recurrent tumours are best treated by Mohs' micrographic surgery where this is available.8The main problems are the length of the procedure, the need for special equipment and training and the relatively high cost.
There is a 5 year recurrence of 2.9% with Moh's surgery. 9
Tumours which have been incompletely excised, especially high-risk BCC and lesions incompletely excised at the deep margin are at high risk of recurrence and should be re-excised.
Curettage and cautery/electrodesiccation.
This is often suggested for low risk primary basal cell carcinomas but there is no clear consensus on its use.
It is performed using a curette to remove soft material from the tumour and the base of the tumour is then destroyed, using either hyfrecation or cautery.
The reported 5-year recurrence rate is between 3 and 20%.9
Cryotherapy/cryosurgery
Cryotherapy is sometimes used for treating small low-risk lesions, including superficial BCCs.
The 5-year recurrence rate has been reported as between 6 and 39%. 9
Non-surgical treatment
Topical treatment is useful for patients with multiple superficial basal cell carcinomas or those who are poor surgical candidates.
Imiquimod 5% cream and fluorouracil 5% cream are both licensed for this indication.
There is a high rate of localised skin reactions including erythema, pruritus, pain, swelling, hypopigmentation, hyperpigmentation, crusting, bleeding, and erosions.
The only head-to head study suggested that 5-FU is inferior to imiquimod at 5-year follow up. 10
Treatment success at one year is between 80 and 83.5%. 9
Imiquimod has been limited for use by some UK ICBs who advise 5-FU as the first-line treatment and imiquimod either restricted for those patients for whom 5-FU has not been beneficial or not to be used at all. 1112
Photodynamic therapy (PDT) 13
PDT is less effective than surgery but the cosmetic results are better.
It involves the use of light therapy in combination with a topical photosensitising agent to destroy cancer cells.
It can be used as an alternative to surgery for the treatment of superficial basal cell carcinomas and thin nodular basal cell carcinomas where surgery is less suitable for a particular patient or lesion, including poorly healing skin sites, multiple lesions, when cosmesis is important, and with patient preference.
It should not be used when surgery is clearly indicated.
Recurrence rates were higher than with surgical or topical management (over 37%).9
Radiotherapy 1
Radiotherapy is indicated where surgery is contra-indicated or as an adjuvant treatment in cases where further surgery could risk damage to major nerves or other vital structures, or when perineural invasion is present.
The downsides of radiotherapy include long courses of treatment, high costs of treatment, worse cosmetic outcomes and an increased risk of secondary skin cancers.
Recurrence rates are similar to those of Moh's surgery.
Hedgehog inhibitors
Vismodegib and sonidegib are approved in the UK for management of basal cell carcinomas associated with Gorlin syndrome or in people without Gorlin syndrome who have multiple basal cell carcinomas. 14
Side effects include muscle spasms, taste alterations, hair loss, fatigue, and weight loss which are apparent in most patients and lead to treatment discontinuation in approximately 30% of patients. 9
Conservative management
Sometimes, especially in the very elderly and debilitated, it may be appropriate to provide no treatment (given the slow growth and low risk of many superficial BCCs) or palliative (debulking or radiotherapy) treatment if the tumour is symptomatic.
Basal cell carcinoma prognosis
Back to contentsMortality is low because basal cell carcinomas rarely metastasise.
Following development of a BCC, patients are at significantly increased risk of developing subsequent BCCs at other sites .
Patients with BCC also have an increased risk of developing SCC and malignant melanoma.
There may also be a small increased risk of other malignancies, such as cancer of the lung, thyroid, mouth, breast and cervix and also non-Hodgkin's lymphoma. 15
If long-term follow-up is recommended then this should be done by dermatologists and not transferred to general practice.
Basal cell carcinoma prevention
Back to contentsEducation on sun avoidance:
Avoid UV exposure in susceptible individuals, particularly children and adolescents.
Stay out of the sun between 10 am and 4 pm.
Use high-factor sunscreens.
Wear wide-brimmed hats, long-sleeved shirts and trousers.
Further reading and references
- Basal Cell Carcinoma; DermIS (Dermatology Information System)
- Superficial Basal Cell Carcinoma; DermIS (Dermatology Information System)
- Puckett Y, Steele RB; Basal Cell Carcinoma.
- Advanced basal cell carcinoma: What dermatologists need to know about diagnosis; A C Krakowski et al; Journal of the American Association of Dermatology
- Risk of Developing a Subsequent Nonmelanoma Skin Cancer in Patients With a History of Nonmelanoma Skin Cancer; I Marcil and R Stern; JAMA Dermatology
- Spiker AM, Troxell T, Ramsey ML; Gorlin Syndrome.
- Basal Cell Carcinoma; A Oakley; DermNet
- Skin cancers - recognition and referral; NICE CKS, April 2025 (UK access only)
- Thomson J, Hogan S, Leonardi-Bee J, et al; Interventions for basal cell carcinoma of the skin. Cochrane Database Syst Rev. 2020 Nov 17;11:CD003412. doi: 10.1002/14651858.CD003412.pub3.
- Basal Cell Carcinoma of the Skin; National Cancer Institute (USA)
- European consensus-based interdisciplinary guideline for diagnosis and treatment of basal cell carcinoma—update 2023; K Perris et al; European Journal of Cancer
- Five-Year Results of a Randomized Controlled Trial Comparing Effectiveness of Photodynamic Therapy, Topical Imiquimod, and Topical 5-Fluorouracil in Patients with Superficial Basal Cell Carcinoma; M Hansen et al; Journal of Investigative Dermatology
- NCL Joint Formulary
- Coventry and Warwickshire Joint Formulary
- Collier NJ, Rhodes LE; Photodynamic Therapy for Basal Cell Carcinoma: The Clinical Context for Future Research Priorities. Molecules. 2020 Nov 18;25(22):5398. doi: 10.3390/molecules25225398.
- Clinical Commissioning Policy: Vismodegib for adults with either Gorlin syndrome or non-Gorlin syndrome related multiple basal cell carcinomas. (Adults); July 2021
- Kuru H, Jokelainen J, Tasanen K, et al; Risk of Non-cutaneous Cancers in Individuals with Basal Cell Carcinoma: A Population-based Cohort Study. Acta Derm Venereol. 2022 Nov 30;102:adv00826. doi: 10.2340/actadv.v102.4451.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 25 Nov 2026
26 Nov 2021 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free