Benign skin tumours
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 30 Nov 2022
Meets Patient’s editorial guidelines
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
The vast majority of skin tumours are benign. There are a few very common benign skin tumours. It is very common for doctors to be asked about such lesions and very often advice is sought when consulting about something else (or quite often outside formal consultation).
Continue reading below
Diagnosis
Assess the history of the lesion's appearance and growth.
Carefully examine the lesion. Allow the appropriate time, light and perhaps magnification, to identify such tumours correctly.
Have sufficient knowledge to differentiate these from skin cancers and particularly malignant skin tumours.
Be aware of the limits of one's knowledge in this field.
Consider the amount of sun exposure the patient is generally subjected to (eg, people who work mainly outside) and the site of the lesion (cancers are more likely on sun-exposed areas, such as the face).
Refer for diagnosis or biopsy lesions where there is any uncertainty of their nature. See the National Institute for Health and Care Excellence (NICE) guidance - under 'Referral', below.
Experience in Australia, the country with the world's highest incidence of skin cancer, shows that adequately trained primary care practitioners in open-access skin cancer clinics can diagnose a wide range of skin lesions, with high specificity and moderate-to-high sensitivity.
It can be useful to divide skin lesions into the following categories:
Macular or slightly raised (papular) lesions.
Frankly papular lesions.
Lesions beneath the epidermis (not related to bony or deeper structures).
It must be borne in mind that such a schema works only for common benign skin lesions and that there are many rarer lesions that will present differently. If the diagnosis is unclear, or the lesion has an atypical appearance, dermatological referral and/or biopsy of the lesion should be considered.
The tumours listed do not include the full range of benign dermatoses which produce skin lesions but not necessarily skin tumours (for example, psoriasis, acne vulgaris, discoid lupus erythematosus, neurofibromatosis, pyoderma gangrenosum, necrobiosis lipoidica diabeticorum and many others).
Macular or slightly raised papular lesions
Naevi
These can be defined as circumscribed, well-defined congenital lesions, also known as moles.
They appear and evolve from the age of 2 years up to 60 years. They are more common on the head, neck and trunk.
Only very rarely do they undergo malignant change.
There is a great deal of variability in size, shape and amount of hair present. Naevomelanocytic naevi are the most common and are categorised into three different subtypes, each of these have a linked, separate article:
The junctional naevi are characterised by melanocytic proliferation limited to the basal epidermis with minimal elevation.
The compound naevus is believed to represent an intermediate step in the evolution of the melanocytic naevus. Components of both dermal and junctional naevi are found simultaneously.
Intradermal naevi are the most common type of adult naevus. These may be papillary, pedunculated, or flat and are often hairy. They are often multiple. The melanocytes in this subtype are entirely within the dermis and have irregular margins. While the junctional naevus can have a reputation for degeneration into malignant melanoma, the intradermal naevus does not.
Special subtypes include the blue naevus:
These are discrete lesions located in the head and neck (occasionally on the arms). One variety (cellular blue naevus) occurs on the buttock and sacrococcygeal areas.
The blue naevus has abundant melanin pigment. It is located entirely within the dermis and no epidermal or junctional component is present.
They can be misdiagnosed as benign fibrous histiocytomas.
A malignant variant of the blue naevus does exist.
Campbell de Morgan spots (or cherry angiomas)
Campbell de Morgan spots are common in adults.
They are asymptomatic acquired vascular lesions of unknown aetiology.
Treatment is for cosmetic purposes only and may be by shave excision, laser ablation, electrodesiccation or cryotherapy.
Dermatofibroma
Dermatofibroma are considered to be a benign tumour, or may represent a fibrous reaction to minor trauma and insect bites.
They are firm raised papules or nodules. They vary in colour from brown to purple and red.
They occur anywhere but are seen most commonly on the lower limb. Fitzpatrick's sign may be used to aid diagnosis (dimpling of the lesion beneath the skin when subject to bilateral compression, ie gently pinching the lesion on either side).
The lesions may resemble melanomas, so biopsy may be necessary to confirm the diagnosis.
Occasionally the lesion may be removed for cosmetic reasons.
Multiple dermatofibromas may be seen in association with autoimmune disorders such as systemic lupus erythematosus, or in patients who are immunocompromised.
Actinic keratosis
Actinic keratosis is known as solar keratosis and senile keratosis.
They are rough, scaly, erythematous papules or plaques found on sun-exposed areas.
A variety of treatments is available. Excision is generally unnecessary.
Sebaceous (senile) hyperplasia1
Sebaceous hyperplasia is common in middle-aged and older patients.
It presents as soft, yellow, dome-shaped papules, some of which are centrally umbilicated.
They commonly occur on the face but sometimes affect the vulva.
They are of no clinical significance, although they can appear similar to early basal cell carcinomas.
Treatment with electrodesiccation or laser ablation is successful; oral isotretinoin has been used in patients with multiple lesions.
Biopsy may be required if the diagnosis is uncertain.
Continue reading below
Frankly papular lesions
Seborrhoeic keratosis
Seborrhoeic keratoses are brown or black lesions which appear to be 'stuck on' to the surface of the skin.
They occur most commonly on the trunk and scalp but may be found anywhere.
The incidence of the lesions increases with age.
They may be mistaken for melanomas, although melanomas have a greater range of colour.
They are usually asymptomatic but may itch or become inflamed after friction from clothing.
Biopsy should be undertaken if the diagnosis is in any doubt.
They may be treated for cosmetic reasons with cryotherapy.
A sudden onset or increase in the number of lesions may signal an underlying malignancy, usually of the stomach, colon or breast - this is known as the Leser-Trélat sign, a paraneoplastic dermatosis.2 Occasionally, the sign is seen in people who have no detectable malignancy.
Typical appearance of seborrhoeic keratosesSeborrhoeic keratosis
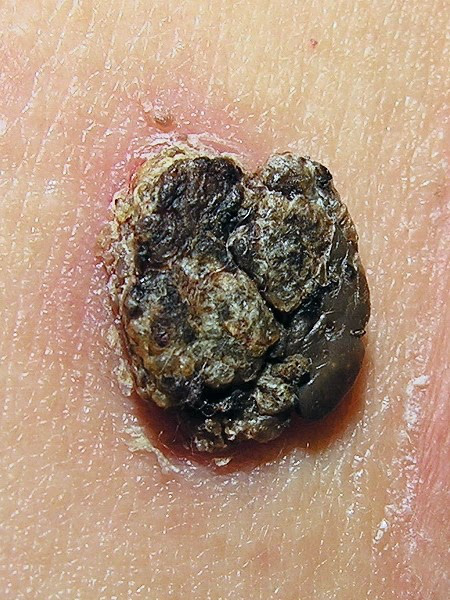
By Lmbuga, Public domain, via Wikimedia Commons
Inverted follicular keratosis3
Probably an inflammatory variant of seborrhoeic keratosis.
It is commonly found on the face (typically the upper eyelid) and other sun-exposed areas in elderly patients.
They are acquired lesions and tend to be solitary. They present as a papule or nodule.
Treatment with simple excision is adequate.
Keratoacanthomas
Keratoacanthomas are rapidly growing papular lesions, often with a central umbilicated keratinous core which may be expelled after several weeks, leaving a hypopigmented scar.
They are usually single and occur in sun-exposed areas, mainly in older patients.
Total excision is the treatment of choice, as they are histologically similar to squamous cell carcinoma and tend to leave a prominent scar after they have undergone spontaneous involution. Smaller lesions can be treated with electrodesiccation and curettage or blunt dissection.
Radiotherapy is an option for patients with recurrence or large lesions.
Intralesional chemotherapy is a treatment option where there is a large lesion in an area on which it would be difficult to achieve excision with a good cosmetic result - eg, the eyelids or nasolabial fold.4
Typical appearance of keratoacanthomaKeratoacanthoma
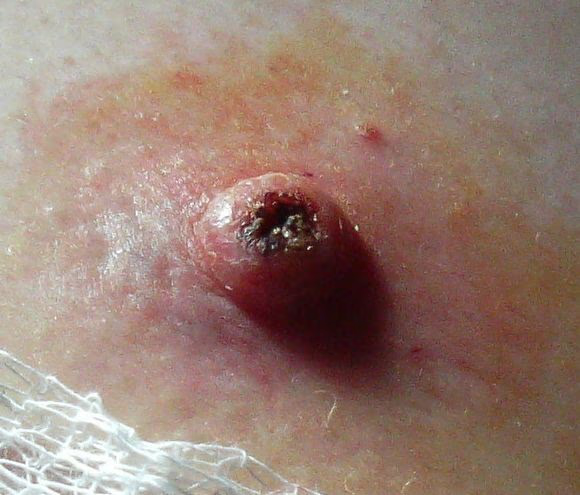
By Jmarchn, CC BY-SA 3.0, via Wikimedia Commons
Skin tags (acrochordons)5 6
These are found in approximately 25% of people, the numbers increasing with age and obesity.
They are an area of hyperplastic epidermis and are frequently found in areas where friction occurs - eg, the neck, axillae and inguinal region.
They may be treated for cosmetic reasons or because of irritation.
They are of no pathological significance in adults but in children may herald the development of naevoid basal cell carcinoma syndrome.7
Pyogenic granuloma
Pyogenic granuloma are also known as granuloma telangiectaticum and an association with trauma is frequent.
They are rapidly proliferating solitary lesions with a tendency to bleed. They are usually less than 1 cm in diameter.
Excision biopsy is usually recommended.
Cutaneous horn8
This is also known as cornu cutaneum.
It is a feature of hyperkeratotic lesions including actinic keratosis, seborrhoeic keratosis, verrucae and epidermoid carcinoma.
Benign skin lesions beneath the epidermis
Lipomas
Lipomas are the most commonly seen subcutaneous tumours.
They may occur anywhere on the body, are made up of adipocytes and have a firm rubbery consistency.
They are usually asymptomatic, although may cause symptoms due to mechanical pressure on underlying structures such as nerves.
Removal is not generally required for other than cosmetic reasons.
Lipomas which occur on the thigh and are greater than 5 cm in diameter should be referred for specialist opinion to rule out liposarcoma.
Sebaceous cyst (epidermoid, epidermal, inclusion or keratinoid cysts)
Sebaceous cysts are round cysts filled with keratin and which communicate with the skin through a small round keratin-filled plug. The term sebaceous is a misnomer, as the sebaceous glands do not form any part of the lesion.
They range in size from a few millimetres to several centimetres and commonly occur on the face, back and chest.
Rupture of the cyst wall commonly occurs resulting in an inflammatory reaction.
They may be removed either because of recurrent infection, or because of their appearance. They may either be removed intact, or by expressing the contents of the cyst through a small incision and then removing the cyst wall.
Dermoid cyst is a variant of the sebaceous cyst. Excision is the treatment of choice.
Continue reading below
Uncommon benign skin tumours
Trichilemmoma9
Trichilemmoma are a more rare form of benign skin tumour.
There is an associated condition called Cowden's disease (when found with tumours of mouth, breast, thyroid and gut).
A rare carcinoma variant of trichilemmoma is known as trichilemmal carcinoma.
Naevus sebaceous of Jadassohn10
These are epithelial naevi and are congenital hamartomas with a yellowish orange colour. They are raised slightly with a waxy appearance.
They have various elements within them (including sebaceous, apocrine).
They are usually present on the scalp and face and slowly enlarge.
They have a risk of becoming malignant. Therefore, complete surgical excision is the treatment of choice.
Trichoepithelioma11
These are uncommon pink or flesh-coloured benign lesions on the face and scalp (occasionally the trunk and neck).
They appear during adolescence and may be familial.
They should be treated with complete surgical excision.
Pilomatrixoma12
This is an uncommon variation of the epidermal cyst occurring on the neck, head and arms of children and young adults.
It typically presents as a solitary subcutaneous nodule with attachment to the skin. There is a history of episodes of inflammation and pain.
Treatment is by excision. The capsule is very friable.
A rare malignant form exists (the malignant pilomatrixoma or pilomatrix carcinoma).
Pseudoepitheliomatous hyperplasia13
It can be difficult to distinguish from squamous carcinoma.
Another term for this lesion is pseudocarcinomatous hyperplasia.
An important feature is a history of trauma and irritation.
A conservative approach is warranted but, if there is any doubt, treat it as for squamous carcinoma with appropriate margins of excision.
Referral for skin tumours
It is worth considering NICE guidance on referral if cancer is suspected:14
Refer a patient presenting with skin lesions suggestive of skin cancer or in whom a biopsy has confirmed skin cancer to a team specialising in skin cancer.
Skin lesion (pigmented and suspicious) with a weighted 7-point checklist score of 3 or more: refer people using a suspected cancer pathway referral (for an appointment within two weeks).
Skin lesion (pigmented or non-pigmented) that suggests nodular melanoma: consider a suspected cancer pathway referral (for an appointment within two weeks).
Skin lesion that raises the suspicion of a squamous cell carcinoma: consider a suspected cancer pathway referral (for an appointment within two weeks).
Skin lesion that raises the suspicion of a basal cell carcinoma: consider routine referral.
Only consider a suspected cancer pathway referral (for an appointment within two weeks) if there is particular concern that a delay may have a significant impact, because of factors such as lesion site or size.
Further reading and references
- DermNet NZ
- Skin cancers - recognition and referral; NICE CKS, Febrary 2021 (UK access only)
- British Association of Dermatologists guidelines for the management of adults with basal cell carcinoma 2021*; BAD (May 2021)
- Skin cancer; National Institute for Health and Care excellence (NICE) Quality Standard, September 2016 - last updated January 2024
- Farci F, Rapini RP; Sebaceous Hyperplasia
- Wollina U; Recent advances in managing and understanding seborrheic keratosis. F1000Res. 2019 Aug 28;8. doi: 10.12688/f1000research.18983.1. eCollection 2019.
- Pe'er J; Pathology of eyelid tumors. Indian J Ophthalmol. 2016 Mar;64(3):177-90. doi: 10.4103/0301-4738.181752.
- Zito PM, Scharf R; Keratoacanthoma. StatPearls, Aug 2022.
- Pandey A, Sonthalia S; Skin Tags
- Belgam Syed SY, Lipoff JB, Chatterjee K; Acrochordon
- Bresler SC, Padwa BL, Granter SR; Nevoid Basal Cell Carcinoma Syndrome (Gorlin Syndrome). Head Neck Pathol. 2016 Jun;10(2):119-24. doi: 10.1007/s12105-016-0706-9. Epub 2016 Mar 14.
- Thiers BH, Strat N, Snyder AN, et al; Cutaneous Horn
- Lozano-Masdemont B, Lara Simon IM, Lopez LG; Dermoscopic Features of Facial Trichilemmoma. Actas Dermosifiliogr. 2017 Nov;108(9):863-864. doi: 10.1016/j.ad.2017.03.009. Epub 2017 May 11.
- Neto MPDS, Assis BR, Andrade GR; Sebaceous nevus of Jadassohn: review and clinical-surgical approach. An Bras Dermatol. 2022 Sep-Oct;97(5):628-636. doi: 10.1016/j.abd.2021.11.001. Epub 2022 Jul 19.
- Skorin L, Bauer SA; Trichoepithelioma. J Am Osteopath Assoc. 2020 Aug 6. pii: 2765213. doi: 10.7556/jaoa.2020.103.
- Zhao A, Kedarisetty S, Arriola AGP, et al; Pilomatrixoma and its Imitators. Ear Nose Throat J. 2021 Sep 22:1455613211044778. doi: 10.1177/01455613211044778.
- Alslaim F, Al Farajat F, Alslaim HS, et al; Etiology and Management of Peristomal Pseudoepitheliomatous Hyperplasia. Cureus. 2021 Dec 6;13(12):e20196. doi: 10.7759/cureus.20196. eCollection 2021 Dec.
- Suspected cancer: recognition and referral; NICE guideline (2015 - last updated October 2023)
Article History
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 29 Nov 2027
30 Nov 2022 | Latest version

Feeling unwell?
Assess your symptoms online for free