Idiopathic intracranial hypertension
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 19 Sept 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In idiopathic intracranial hypertension there is raised pressure within the skull (raised intracranial pressure), which puts pressure on the brain. Idiopathic means that the cause of this raised pressure is unknown. The main symptoms are headache and loss of sight (visual loss). It mostly affects women of childbearing age who are overweight or obese. Treatment is aimed at preventing permanent visual loss and includes treatment with medicines. Brain surgery (neurosurgery) may also be used. For many people, a combination of medical and surgical treatment can help to control their symptoms well.
At a glance
Idiopathic intracranial hypertension (IIH) means raised pressure around the brain with no clear cause.
It can cause headaches, pulsatile tinnitus, and changes in vision.
If untreated, IIH can damage the optic nerve, potentially leading to blindness.
IIH is rare and mostly affects overweight women of childbearing age.
Diagnosis involves检查 (examination) of symptoms, eye tests, and scans to exclude other causes.
Treatment aims to relieve headaches and prevent vision loss, including weight loss and medicines.
Surgical options include shunts to drain fluid or a procedure around the optic nerve.
In this article:
Video picks for Headache
Continue reading below
What is idiopathic intracranial hypertension?
Intracranial hypertension means raised pressure inside the skull and around the brain. Idiopathic intracranial hypertension (IIH) is a condition where raised pressure inside the skull occurs without an identifiable cause. Idiopathic means that the cause of this raised pressure is unknown.
There are many other causes of raised intracranial pressure. When there is a clear cause, such as a brain tumour, it's sometimes called secondary intracranial hypertension. However, in IIH, there is no clear cause.
The brain is surrounded by a fluid called cerebrospinal fluid (CSF). It's thought that, in IIH, there is a problem where too much CSF is produced, not enough CSF is re-absorbed, or both. We don't know exactly why this happens in IIH, although there are several theories.
Having too much CSF around the brain causes high pressure inside the skull. This raised pressure leads to the symptoms of idiopathic intracranial hypertension. It can cause headaches and also swelling of the first part of the optic nerve - the optic disc - at the back of the eye. this Swelling of the optic nerve is called papilloedema. If papilloedema is not recognised and treated, it can cause damage to the optic nerve. This can lead to vision problems, including blindness.
Idiopathic intracranial hypertension used to be called benign intracranial hypertension. However, this name is not being used as much now. This is because IIH isn't harmless (benign). It can cause some quite disabling symptoms and can lead to loss of vision if it is not treated. Another old name is 'pseudotumour cerebri', as it can lead to some signs and symptoms of a brain tumour, without a brain tumour actually being present.
How common is idiopathic intracranial hypertension?
Back to contentsIdiopathic intracranial hypertension is rare. It affects 1 or 2 people in every 100,000. It mostly affects women of childbearing age who are overweight or obese. However, men and children can sometimes be affected as well as people who are not overweight.
Idiopathic intracranial hypertension occurs more frequently in some groups of people. Possible risk factors include:
Gender. Amongst adults, more than 9 out of 10 people with idiopathic intracranial hypertension are women. It's thought that female hormones may play a role in the condition.
Overweight and obesity. This is very common amongst people with idiopathic intracranial hypertension. Hormonal changes from obesity might be linked to the condition.
Rarely, certain medications: stopping steroids can trigger idiopathic intracranial hypertension, and other medications such as tetracycline antibiotics, lithium, and vitamin A have all be linked with it.
Continue reading below
Idiopathic intracranial hypertension symptoms
Back to contentsThere may be many different symptoms associated with idiopathic intracranial hypertension (see Further Reading and References, below). However, the typical symptoms include:
Headache.
Tinnitus.
Changes in vision.
The most prominent symptom of idiopathic intracranial hypertension is headache. This can be severe and is a long-term (chronic) headache. It can vary in its location and may come and go. Often - but not always - the headache is worse in the morning, worse on lying flat, and worse when coughing, sneezing, or straining (all of these things can increase the pressure inside the skull slightly).
Some people can feel sick or be sick (vomit) with the headache. You may also notice tinnitus in one or both of your ears. This is typically a pulsating, rhythmic sound that you can hear in your ear.
You may also notice some temporary sight (visual) disturbance or temporary loss of vision. For example, you may have dimming or loss of your vision in one or both of your eyes, lasting for a few seconds. This can sometimes come on after bending over. You may have some double vision when looking from side to side, or pain behind the eyes on eye movement. You may also notice a progressive permanent loss of vision in one or both of your eyes.
How long does idiopathic intracranial hypertension last?
This differs from person to person, but idiopathic intracranial hypertension often takes several months to improve with treatment. In some people, it goes away completely after months or years. In other people, it may go away but return again in future. For some people, it is a lifelong condition.
How is idiopathic intracranial hypertension diagnosed?
Back to contentsIf you visit your doctor, complaining of headaches and/or sight (visual) symptoms, your doctor will usually discuss your symptoms with you, and examine the nerves in your arms, legs, and face.
Ophthalmoscopy
They may examine the back of the eyes with a hand-held instrument for looking in the back of the eye (an ophthalmoscope). This can also be done at an optician, who will often take photos of the back of the eye. This may show swelling at the back of the eye (papilloedema). However, not everyone with idiopathic intracranial hypertension has papilloedema.
Papilloedema is a sign of raised pressure within the skull (raised intracranial pressure). Therefore, the main thing when diagnosing idiopathic intracranial hypertension is to rule out other causes of raised pressure within the skull. These may include problems such as water on the brain (hydrocephalus) or a brain tumour.
Your doctor will usually refer you to a specialist for investigations to rule out other causes. Investigations can include, for example, MRI or CT scanning of your brain.
Eye examination
You may also have a more detailed eye examination. This will allow an eye specialist to examine the back of your eyes fully. You may have visual field testing to see if there are any signs of loss of vision in parts of one or both of your eyes. (Your visual field is the area in front of your eye in any part of which an object can be seen without moving your eye.)
You may have your colour vision tested, as this can also be affected in idiopathic intracranial hypertension.
Brain scans
A brain scan is likely to be performed to rule out other causes of raised intracranial pressure, such as a brain tumour. In idiopathic intracranial hypertension, brain scans are usually normal, although sometimes there are subtle changes of high pressure that can be seen.
This is likely to be an MRI scan, but sometimes a CT scan is used instead.
Lumbar puncture
This is one of the main tests to confirm high pressure inside the brain. CSF is found around the brain, but also around the spinal cord. A lumbar puncture (sometimes called a spinal tap) involves putting a needle into the lower part of the spine to sample some of the fluid around the spine. In idiopathic intracranial hypertension, measurements will show that the CSF is under raised pressure. A sample of CSF can also be taken and analysed to look for any other causes of raised pressure.
See the separate leaflet called Lumbar Puncture (Spinal Tap) for more details.
Continue reading below
What are the aims of idiopathic intracranial hypertension treatment?
Back to contentsThere are two main aims of treatment for idiopathic intracranial hypertension:
To improve, and hopefully cure, the headaches.
To prevent visual loss.
If you are diagnosed with idiopathic intracranial hypertension, it is important that your vision be closely monitored to look for any changes or early signs of loss of vision. This can be done by regularly measuring your 'visual acuity' (the size of letters that can be read on a wall chart), along with checking your visual fields.
Any signs of deterioration in your vision may mean that your treatment needs to be adjusted.
Idiopathic intracranial hypertension treatment
Back to contentsWeight loss
For people with overweight or obesity, weight loss can be a very effective treatment for idiopathic intracranial hypertension. Research shows that losing 5-10% of body weight can significantly improve symptoms of IIH, and sometimes causes the condition to go into remission.
Medical treatment
The most commonly-used medication for idiopathic intracranial hypertension is acetazolamide. Acetazolamide reduces CSF production. Acetazolamide is a safe medication, but commonly causes tingling of the fingers and toes as a side-effect. It may also cause birth defects in pregnancy; speak to your doctor if you are considering or planning a pregnancy.
Other medicines that are used less commonly include topiramate and furosemide.
Various painkillers may also be used to help relieve headaches. A short course of steroid tablets is also sometimes used.
Treatment with medicines can work well for many people. However, if your symptoms do not improve with medical treatment or you have new loss of vision, surgery may be considered.
Surgical treatment
Surgery aims to reduce the pressure within the skull (intracranial pressure). There are two main procedures that are done. The first is to put in place a tube (called a shunt) to drain away the excess CSF. This is probably the most common surgical procedure that is used. The shunt is run from either of the following:
The subarachnoid space in the lower part of the spine into the tummy (abdomen) - called a lumbar-peritoneal shunt.
The ventricles in the brain into the abdomen (called a ventriculo-peritoneal shunt).
However, there can be problems with a shunt. It can become infected, it can drain away too much CSF, or sometimes it can become blocked. Therefore, someone who has had a shunt inserted needs regular check-ups to make sure that it is working normally.
The second type of surgical treatment is around the eye. A procedure called optic nerve sheath fenestration can be carried out. Small cuts are made in the protective sheath around the optic nerve. This allows CSF to escape and the pressure on the optic nerve is reduced. This procedure can be very good at helping sight (visual) symptoms associated with idiopathic intracranial hypertension. However, it may have little effect on other symptoms, including headache. This is because it tends to have little effect on reducing overall pressure within the skull.
Some anatomy around the brain
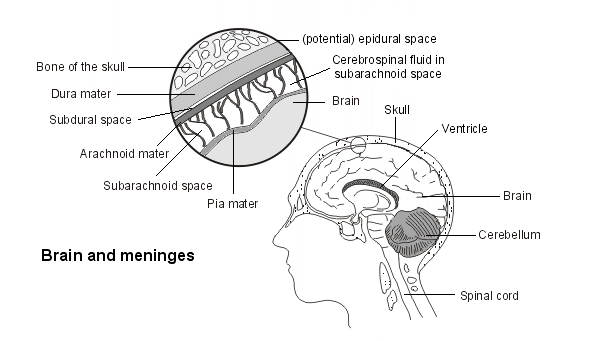
Back to contentsThe meninges form the protective lining that surrounds the brain and spinal cord within the backbone (vertebral column). There are three layers of meninges:
The outermost layer that lies next to the skull or the vertebral column is called the dura mater.
The middle layer is called the arachnoid mater.
The inner layer that is closest to the brain or the spinal cord is called the pia mater.
There are also three spaces between the layers of meninges:
The epidural space - the space between the vertebral column and the dura mater. (This is only a potential space in the head between the skull and the dura mater.)
The subdural space - the space between the dura mater and the arachnoid mater.
The subarachnoid space - the space between the arachnoid mater and pia mater.
Brain and meninges
Understanding cerebrospinal fluid
Back to contentsThe brain and the spinal cord are bathed in a clear, watery fluid called cerebrospinal fluid (CSF). This fluid helps to cushion the brain from contact with the skull when the head is moved vigorously.
CSF is made by a network of blood vessels inside the ventricles of the brain. The ventricles are essentially four cavities within the brain. The CSF circulates through the brain ventricles into the subarachnoid space. Eventually, CSF is absorbed into the bloodstream through some one-way valves called the arachnoid villi.
What is the outlook (prognosis)?
Back to contentsIt is essential to detect idiopathic intracranial hypertension early and to start treatment early to prevent permanent loss of vision occurring.
In some people, idiopathic intracranial hypertension can get better by itself but recurrence (relapse) of symptoms is common. For many other people, a combination of medical and surgical treatment can help to control their symptoms well. However, some people can still have troublesome symptoms despite treatment.
Patient picks for Headache

Brain and nerves
Headache
Headaches are very common and can affect people of all ages, often triggered by everyday factors. Most are not serious and improve with rest, fluids, or simple pain relief. However, some headaches can be more serious and may need medical attention.
by Dr Toni Hazell, MRCGP

Brain and nerves
Medication-overuse headache
Medication-overuse headache is a cause of frequent headaches caused by taking painkillers or triptan medicines regularly for headaches or migraine.
by Dr Doug McKechnie, MRCGP
Frequently asked questions
Can IIH be caused by problems with the blood vessels in the brain?
No, IIH is a condition where the cause of raised pressure inside the skull is unknown. While there are other causes of raised intracranial pressure, such as a brain tumour, IIH specifically means there is no clear identifiable cause like a problem with blood vessels, or any other underlying condition.
If I have IIH, will I definitely experience vision loss?
Not necessarily. Early detection and treatment of IIH are essential to prevent permanent loss of vision. If papilloedema (swelling of the optic nerve) is not recognised and treated, it can lead to vision problems, including blindness, but treatments are available to manage the condition and protect your sight.
Are there any specific lifestyle changes, besides weight loss, that can help manage IIH?
The article primarily highlights weight loss as a very effective treatment for people with overweight or obesity, noting that losing 5-10% of body weight can significantly improve symptoms. It does not mention other specific lifestyle changes apart from this.
What kind of specialist will I be referred to for investigations if IIH is suspected?
If your doctor suspects IIH, they will usually refer you to a specialist for further investigations. These investigations are primarily to rule out other causes of raised intracranial pressure like brain tumours or hydrocephalus. The article does not specify the exact type of specialist, but implies a medical professional who can order and interpret detailed brain scans and perform other diagnostic tests like a lumbar puncture.
What are the common side effects of acetazolamide, the main medication for IIH?
Acetazolamide, the most commonly used medication for IIH, can cause tingling of the fingers and toes as a common side-effect. It is also important to note that it may cause birth defects in pregnancy, so it is crucial to discuss any pregnancy plans with your doctor.
If surgery is performed, how long does the shunt typically last, and are there common issues I should be aware of?
The article does not specify how long a shunt typically lasts. However, it does state that there can be problems with a shunt, such as infection, draining away too much cerebrospinal fluid (CSF), or becoming blocked. Regular check-ups are needed to ensure it is working correctly.
Can IIH affect my daily activities, and if so, how?
Yes, IIH can lead to quite disabling symptoms. The prominent symptom is a severe, long-term headache that can vary in location and intensity. It can be worse in the mornings or when lying flat, coughing, sneezing, or straining. You may also experience tinnitus, nausea, vomiting, or temporary visual disturbances, which can affect your ability to perform daily tasks.
Further reading and references
- Piper RJ, Kalyvas AV, Young AM, et al; Interventions for idiopathic intracranial hypertension. Cochrane Database Syst Rev. 2015 Aug 7;8:CD003434. doi: 10.1002/14651858.CD003434.pub3.
- Wall M; Update on Idiopathic Intracranial Hypertension. Neurol Clin. 2017 Feb;35(1):45-57. doi: 10.1016/j.ncl.2016.08.004.
- Mitchell JL, Mollan SP, Vijay V, et al; Novel advances in monitoring and therapeutic approaches in idiopathic intracranial hypertension. Curr Opin Neurol. 2019 Jun;32(3):422-431. doi: 10.1097/WCO.0000000000000690.
- Kalyvas A, Neromyliotis E, Koutsarnakis C, et al; A systematic review of surgical treatments of idiopathic intracranial hypertension (IIH). Neurosurg Rev. 2020 Apr 25. pii: 10.1007/s10143-020-01288-1. doi: 10.1007/s10143-020-01288-1.
Continue reading below
About the authorView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 17 Sept 2028
19 Sept 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.