Bronchiectasis
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 30 Jan 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Bronchiectasis is a problem with the lungs, where you cough up lots of phlegm, (sputum): far more than usual. It is usually caused by something that has already affected the lungs, like a bad infection; but sometimes no cause is found. It generally affects older people. There are some good treatments available to keep it under control.
At a glance
Bronchiectasis is a lung condition where airways become abnormally wider.
This widening causes a build-up of mucus in the lungs, leading to symptoms.
Symptoms include a wet cough, lots of sputum, and breathlessness.
It can be caused by severe lung infections, immune system problems, or other conditions.
Diagnosis is usually by a lung specialist using a CT scan of the lungs.
Treatment aims to manage symptoms and prevent worsening, as it cannot be reversed.
Most people with bronchiectasis have a good outlook if they manage their treatment.
In this article:
Video picks for Chest and lung problems
Continue reading below
Understanding the airways
Usually air travels from our windpipes down into our lungs through small tubes. The tubes that come off the windpipe are called bronchi; then they split into bronchioles which are a bit smaller. Finally the small bronchioles split into tiny tubes called alveoli. In a normal person all these tubes are fairly small: up to 2 cm in diameter at the windpipe, all the way down to just a few millimetres for the alveoli. Our airways are a bit like a tree: the tree trunk is the biggest bit, but it gradually splits off into branches, then twigs.
What is bronchiectasis?
Back to contentsIn bronchiectasis the airways gradually become bigger than they are meant to be. So instead of the tiny alveoli being just a few millimetres in diameter, they might be a centimetre wide. And instead of bronchioles being about a centimetre wide, they become 1.5 centimetres in diameter.
The problem then is that mucus, which we all have in our lungs to some degree, can pool and collect in the airways. And because the airways aren't meant to be that wide in the first place, they produce more mucus than usual. Mucus is the same as sputum, or phlegm: sticky, slightly thick liquid that can be white, clear, green or yellow. It can usually be coughed up.
This picture shows what happens in bronchiectasis:
Lungs and airways - bronchiectasis
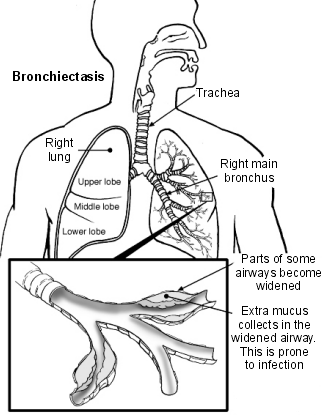
Continue reading below
What causes bronchiectasis?
Back to contentsGenerally the cause is something that has created infection or inflammation in the lungs:
A bad infection with tuberculosis.
A bad case of pneumonia.
A blood clot in the lungs, called a pulmonary embolus.
A bad infection with whooping cough (pertussis) as a child.
Or it could be from a problem with the immune system:
Having HIV.
Having a low immune system from birth.
Or a problem with how the lungs clear away mucus already, such as occurs with:
Cystic fibrosis from childhood.
Some other type of rare condition like Kartagener's syndrome.
There are other rare conditions that can cause bronchiectasis, such as:
Alpha-1 antitrypsin deficiency.
Yellow nail syndrome.
Allergic bronchopulmonary aspergillosis.
These problems could have occurred in childhood, but it's only in adulthood or even older that you develop bronchiectasis.
In at least a third of cases of bronchiectasis, no cause is found.
How common is bronchiectasis?
Back to contentsBronchiectasis is not particularly common: most family doctors in the UK will have some patients with the condition but will not see new cases very often. Around 1% of people have been diagnosed with bronchiectasis in the general population; but people with a chronic lung condition like asthma, cystic fibrosis or chronic obstructive pulmonary disease (COPD) will have a higher rate of bronchiectasis. The condition gets more common with old age.
It seems to be getting more common lately but that is probably because lung scans are more detailed and picking up on the lung changes of bronchiectasis more easily.
Continue reading below
What are the symptoms of bronchiectasis?
Back to contentsThe symptoms are caused by there being too much mucus inside the lungs:
A wet cough every day, despite taking antibiotics.
Coughing up lots of sputum (also called phlegm or mucus).
Feeling slightly breathless or unable to do as much exercise as you used to.
Frequent chest infections, particularly with a bug called Pseudomonas aeruginosa.
As a child: asthma that is difficult to control; or having recurrent chest or ear infections.
How is bronchiectasis diagnosed?
Back to contentsBronchiectasis is usually diagnosed by a lung specialist rather than a family doctor. It is usually diagnosed by:
The general clinical picture of someone with a long-term cough that produces large amounts of sputum.
A CT scan of the lungs that shows enlargement (or what is often called 'dilatation') of the airways and usually thickening of the wall of the airways.
How to treat bronchiectasis
Back to contentsOnce bronchiectasis sets in, it can't ever be reversed. However, it can be prevented from getting worse by:
Taking regular exercise.
Using 'airways clearance techniques' that help to drain off mucus from the lungs. This usually involves seeing a physiotherapist who is trained in treating the lungs: what is usually termed a respiratory physiotherapist or 'chest physio'. The patient can also be taught how to use postural drainage techniques themself, along with special breathing techniques to bring up the mucus.
Nebulised saline can help to make the sputum thinner and easier to cough up.
Nebulised bronchodilators can help the mucus to drain away too.
Long-term macrolide antibiotics such as azithromycin, can help to prevent infections and dampen down inflammation in the lungs.
Treating any underlying cause, like tuberculosis or cystic fibrosis, is also important.
Inhaled steroids or nebulised steroids do not seem to help.
If the bronchiectasis is confined to just one area of the lungs (which is unusual) then surgery can be considered.
What is the outlook?
Back to contentsMost people with bronchiectasis (with no underlying cause) have a good outlook (prognosis). Symptoms in many affected people do not become severe. Treatment, in particular with antibiotics when an infection occurs, or regularly when needed, keeps most people reasonably well.
The condition becomes worse in some cases and breathing problems may develop. In a small number of cases the condition becomes gradually worse over time as more and more of the airways become affected.
A life-threatening bleed from a damaged airway may also occur but is rare.
The outlook for people where bronchiectasis is part of another condition depends on the underlying cause. Generally it gets a little bit worse as you get older, but if you follow treatment plans then you should be able to stop it getting much worse.
Patient picks for Chest and lung problems

Chest and lungs
Pulmonary fibrosis
Pulmonary fibrosis is a serious lung disease where the tiny air sacs of the lungs (the alveoli) and the lung tissue next to the alveoli become damaged and scarred, resulting in lung fibrosis. The main symptom is shortness of breath that gradually gets worse. The cause is often not known but pulmonary fibrosis can be caused by a variety of underlying conditions. Treatments include treating any underlying cause in addition to steroids and other medicines. Increasingly lung transplantation may be considered.
by Dr Toni Hazell, MRCGP

Chest and lungs
Pleural effusion
A pleural effusion is a collection of fluid next to the lung. There are various causes. The effusion may cause you to become breathless. The fluid can be drained if necessary. Treatment is mainly aimed at the underlying cause.
by Dr Hayley Willacy, FRCGP
Frequently asked questions
Can bronchiectasis be cured?
Once bronchiectasis has developed, it cannot be reversed. However, various treatments and lifestyle adjustments can help prevent the condition from worsening and manage its symptoms effectively.
If I have asthma or COPD, am I more likely to get bronchiectasis?
Yes, individuals with chronic lung conditions such as asthma, cystic fibrosis, or chronic obstructive pulmonary disease (COPD) have a higher rate of bronchiectasis compared to the general population. The condition also becomes more common with old age.
What is 'airways clearance techniques' and how does it help with bronchiectasis?
Airways clearance techniques are methods used to help drain mucus from the lungs. This often involves working with a respiratory physiotherapist, who can teach patients techniques like postural drainage and special breathing exercises to help bring up mucus. Nebulised saline and bronchodilators can also be used to make sputum thinner and easier to cough up or to help mucus drain away.
Why do people with bronchiectasis cough up a lot of mucus?
In bronchiectasis, the airways become wider than normal. This leads to an increased production of mucus, which can then pool and collect in the enlarged airways. This excess mucus is what causes the symptom of a wet cough and coughing up large amounts of sputum.
Can childhood illnesses lead to bronchiectasis later in life?
Yes, some problems experienced in childhood, such as a severe infection with whooping cough (pertussis), certain immune system problems present from birth, or cystic fibrosis, can contribute to the development of bronchiectasis later in adulthood, or even older age.
Is it possible to have bronchiectasis without knowing the cause?
Yes, in at least a third of all bronchiectasis cases, medical professionals are unable to identify a specific cause for the condition.
What kind of doctor diagnoses bronchiectasis?
Bronchiectasis is usually diagnosed by a lung specialist, rather than a general family doctor. The diagnosis is typically made based on the overall clinical presentation, including a long-term cough with significant sputum, and confirmed by a CT scan of the lungs that shows enlarged and often thickened airways.
Further reading and references
- Bronchiectasis; NICE CKS, March 2024 (UK access only)
- Snell N, Gibson J, Jarrold I, et al; Epidemiology of bronchiectasis in the UK: Findings from the British lung foundation's 'Respiratory health of the nation' project. Respir Med. 2019 Oct-Nov;158:21-23. doi: 10.1016/j.rmed.2019.09.012. Epub 2019 Sep 17.
- Hill AT, Sullivan AL, Chalmers JD, et al; British Thoracic Society Guideline for bronchiectasis in adults. Thorax. 2019 Jan;74(Suppl 1):1-69. doi: 10.1136/thoraxjnl-2018-212463.
- Lee AL, Burge AT, Holland AE; Positive expiratory pressure therapy versus other airway clearance techniques for bronchiectasis. Cochrane Database Syst Rev. 2017 Sep 27;9(9):CD011699. doi: 10.1002/14651858.CD011699.pub2.
Continue reading below
About the authorView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
About the reviewerView full bio

Dr Krishna Vakharia, MRCGP
Chief Medical Officer for Health, Optum UK
MBChB, MRCGP(2013), BMedSci (hons), DFSRH, DRCOG, PGDipDerm (Distn)
Dr Krishna Vakharia is an NHS GP. She is also a regular examiner for the postgraduate Diploma in Practical Dermatology at Cardiff University as well as being the Chief Medical Officer for health at Optum UK.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 29 Jan 2028
30 Jan 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.