Pulmonary embolism
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Rachel Hudson, MRCGPLast updated 5 Sept 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
In this series:Breathlessness and difficulty breathingPulmonary fibrosisControlled breathingDealing with an adult who is unresponsive
A pulmonary embolism (embolus) is a serious, potentially life-threatening condition. It is due to a blockage in a blood vessel in the lungs. A pulmonary embolism (PE) can cause symptoms such as chest pain or breathlessness. It may have no symptoms and be hard to detect. A massive PE can cause collapse and death. PE usually happens due to an underlying blood clot in the leg - deep vein thrombosis (DVT). Prompt treatment is important and can be life-saving. Pregnancy, various medical conditions and medicines, immobility and major surgery all increase the risk of a PE. Anticoagulation, initially with heparin and then warfarin, or other oral blood thinning tablets, is the usual treatment for PE.
In this article:
Video picks for Arteries
Continue reading below
What is a pulmonary embolism?
A pulmonary embolism (PE) is a blockage in one of the blood vessels (arteries) in the lungs - usually due to a blood clot. A PE can be in an artery in the centre of the lung or one near the edge of the lung.
The clot can be large or small and there can be more than one clot. If there are severe symptoms, which occur with a large clot near the centre of the lung, this is known as a massive PE, and is very serious.
Venous thromboembolism
Pulmonary embolism (PE) is part of a group of problems together known as venous thromboembolism (VTE).
Venous means related to veins. A thrombosis is a blockage of a blood vessel by a blood clot (a thrombus). An embolism occurs when part or all of the thrombus dislodges from where it formed and travels in the blood until it becomes stuck in a narrower blood vessel, elsewhere in the body. The thrombus is then called an embolus.
A deep vein thrombosis (DVT) is the usual cause of a PE. A DVT occurs in a vein in the leg. DVT is also part of VTE.
Pulmonary embolism symptoms
Back to contentsThe symptoms will depend on how large or small the clot is, and on how well the person's lungs can cope with the clot. People who are frail or have existing illness are likely to have worse symptoms than someone who is fit and well. Symptoms often start suddenly.
A small PE may cause:
No symptoms at all (common).
Breathlessness - this can vary in degree from very mild to obvious shortness of breath.
Chest pain which is pleuritic, meaning sharp pain felt when breathing in. Often you feel like you can't breathe deeply, as this causes you to catch your breath. This happens because the blood clot may irritate the lining layer (pleura) around the lung. Shallow breathing is more comfortable.
A mildly raised temperature (fever).
A fast heart rate (tachycardia).
A massive PE or lots of clots (multiple emboli) may cause:
Severe breathlessness.
Chest pain - with a large PE the pain may be felt in the centre of the chest behind the breastbone.
Feeling faint, feeling unwell, or a collapse. This is because a large blood clot interferes with the heart and blood circulation, causing the blood pressure to drop dramatically.
Rarely, in extreme cases, a massive PE can cause cardiac arrest, where the heart stops pumping due to the clot. This can result in death, even if resuscitation is attempted.
There may be symptoms of a DVT, such as pain at the back of the calf in the leg, tenderness of the calf muscles or swelling of a leg or foot. The calf may also be warm and red.
A massive PE is so called not due to the actual size of the blood clot (embolus) but due to the size of its effect. A PE is high-risk if it causes serious problems such as a collapse or low blood pressure. Massive PEs are, by definition, high-risk.
About 1 in 7 people with a massive PE will die as a result.
Continue reading below
What causes a pulmonary embolism?
Back to contentsDiagram of leg showing veins and a Deep Vein Thrombosis
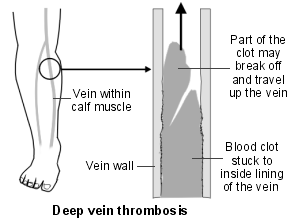
Deep vein thrombosis (DVT)
In almost all cases, the cause is a blood clot (thrombus) that has originally formed in a deep vein (known as a DVT). This clot travels through the circulation and eventually gets stuck in one of the blood vessels in the lung (pulmonary arteries).
The thrombus that has broken away is now called an embolus (and can therefore cause an embolism). Most DVTs come from veins in the legs or pelvis. Occasionally, a PE may come from a blood clot in an arm vein, or from a blood clot formed in the heart.
Other causes
Rarely, the blockage in the lung blood vessel may be caused by an embolus which is not a blood clot. This can be:
Fatty material from the marrow of a broken bone (if a large, long bone is broken - such as the thigh bone (femur)).
Foreign material from an impure injection - for example, with drug misuse.
Amniotic fluid from a pregnancy or childbirth (rare).
A large air bubble in a vein (rare).
A small piece of cancerous material (tumour) that has broken off from a larger tumour in the body.
Mycotic emboli - material from a focus of fungal infection.
Risk factors for pulmonary embolism
Back to contentsNearly all cases of PE are caused by a DVT (see above). So, people more likely to get a PE are those prone to DVTs. The risk factors for DVT are explained in a separate leaflet.
Some important risk factors are:
Immobility.
Other serious illnesses eg, active cancer.
Major surgery (especially gynaecological surgery, and operations on the pelvis and legs).
Blood conditions which make it more likely for clots to form (thrombophilias)
Pregnancy and the 6 weeks immediately after giving birth.
The risk of developing a DVT or PE in hospital can be greatly reduced by getting the patient up and walking from bed rest as soon as possible. Medicine to help prevent a DVT or PE is also given to those at particular risk.
Continue reading below
How common is a pulmonary embolism?
Back to contentsIt is estimated that about 1 in 1,000 people have a DVT each year in the UK. If untreated, about 1 in 10 people with a DVT will develop a PE. Half of all people with a PE develop it when they are a hospital inpatient.
25,000 deaths per year in England are due to blood clots (PEs that have happened after a DVT) that have developed whilst a person was in hospital.
How is a pulmonary embolism diagnosed?
Back to contentsThe diagnosis is often suspected on the basis of symptoms and your medical history. For example, someone who has had major surgery, been immobile in hospital and then gets sudden breathlessness, is likely to have a PE.
A pregnant women who has symptoms and/or signs suggesting PE should be admitted to hospital quickly as PE during pregnancy is very serious and rapid diagnosis and treatment are essential.
If you are not pregnant, your healthcare professional may use the Wells' score to decide whether admission to hospital is necessary. This assesses your risk of having a PE by looking at whether you have:
Clinical features of DVT.
Heart rate greater than 100 beats per minute.
Been immobile for more than three days or had surgery in the previous four weeks.
Previous DVT or PE.
Coughing up blood (haemoptysis).
Been receiving treatment for cancer in the last six months.
An alternative diagnosis is less likely than PE, such as pneumothorax, pneumonia, heart attack or gastro-oesophageal reflux disease.
If your score is high enough, you will need to go to hospital. Various tests may be used to help confirm the diagnosis. These may include one or more of the following:
Ultrasound scan of the leg
A type of ultrasound called a duplex Doppler is used to show blood flow in the leg veins, and any blockage to blood flow. Ultrasound is useful because it is an easy, non-invasive test and may show up a DVT. If a DVT is found, then a PE can be assumed to be the cause of the other symptoms (such as breathlessness or chest pain).
Treatment (with anticoagulant medication - see below) can be started immediately for both the DVT and the suspected PE. The treatment is generally the same for both. Further tests may be unnecessary in this situation.
However, if the ultrasound is negative, a DVT or PE is not ruled out, because some clots don't show up on ultrasound. Further tests will be needed.
Lower limb compression venous ultrasound may be useful for pregnant women in whom irradiation from other imaging may be harmful.
Blood test for D-dimer
This detects fragments of breakdown products of a blood clot. The higher the level, the more likely you have a blood clot in a vein. Unfortunately, the test can be positive in a number of other situations, such as if you have had recent surgery or if you are pregnant. A positive test does not, therefore, diagnose a DVT or a PE.
The test may, however, indicate how likely it is that you have a blood clot (the clot can be either a DVT or a PE). This can help decide if further tests are needed.
A negative D-dimer result when you are at low risk of VTE means the chance of having a thrombus is extremely low. However, if your VTE risk is high, then a D-dimer test cannot rule out the possibility of a thrombus and you will need other tests.
Ultrasound scanning of the heart (echocardiography)
An echocardiogram is useful for people who may have a massive PE, as it can show the effect on the heart. If there is a massive PE then this puts strain on the right-hand side of the heart. It can be done at the bedside.
Isotope scan and CTPA scan
These are specialised scans which look at the circulation in the lung. They are useful, because they can show quite accurately whether or not a PE is present. See the separate leaflet called Radionuclide (Isotope) Scan.
The isotope scan is also called a V/Q scan, or ventilation/perfusion scan. The CTPA scan is a type of CT scan looking at the lung arteries - the full name is computerised tomographic pulmonary angiography scan. Both involve X-rays and the CTPA scan is the more accurate test.
V/Q scans are used in some circumstances. For example, if you are allergic to the dye (contrast) used in CTPA scanning, if you have chronic kidney disease, or if CTPA is unavailable.
General tests
Other tests on the heart, lung and blood are usually done. These may help with the diagnosis or may show up other conditions:
A heart tracing (electrocardiogram, or ECG) is often done. This is to look for any signs of strain on the heart that can occur with a PE. It can also look for any abnormal heart rhythms, such as atrial fibrillation (AF) which can occur as a result of a PE.
Blood tests to look for signs of a heart attack, infection or inflammation. Also, a test for arterial blood gases may be taken, which involves taking the blood sample from an artery rather than from a vein. This is to check the level of oxygen in the blood.
A chest X-ray to look for pneumonia or other chest conditions.
Pulmonary embolism treatment
Back to contentsThis section deals with PE due to a blood clot, not with the rare causes listed above. The main treatments for pulmonary embolism are:
Anticoagulant treatment.
Oxygen given in the early stages to help with breathlessness and low oxygen level.
Patients who have features suggestive of a large/massive PE or who have worrying features, such as low blood pressure, fast heart rate and/or low blood oxygen levels, will need to be admitted to hospital. If no concerning features are present then patients can be assessed in hospital and blood samples sent off.
If there is still a possibility of PE you may be started on low molecular weight heparin (LMWH) injections and sent home to then return and have further scans the next day. You will then return for the result where either treatment will stop or further treatment and advice will be given.
Anticoagulant treatment (blood thinners)
Anticoagulation is often called thinning the blood. However, it does not actually thin the blood. It alters certain chemicals in the blood to stop clots forming so easily. It doesn't dissolve the clot either (as some people incorrectly think). Anticoagulation prevents a PE from getting larger and prevents any new clots from forming. The body's own healing mechanisms can then get to work to break up the clot.
Anticoagulation treatment is usually started immediately (as soon as a PE is suspected) in order to prevent the clot worsening, while waiting for test results.
Anticoagulation medication comes in two forms: injections and tablets (or syrup for those who cannot swallow tablets).
Either apixaban or rivaroxaban (tablets) are offered to most people with confirmed PE. If neither apixaban nor rivaroxaban is suitable, low molecular weight heparin (LMWH) is offered for at least five days followed by dabigatran or edoxaban tablets.
Alternatively LMWH is taken at the same time as warfarin for at least five days, or until the INR is stable, followed by warfarin on its own. Warfarin used to be the main oral (tablet or syrup) treatment before the newer drugs listed above were introduced and some people still take it if they have been on it for a long time.
Heparin (or similar injections called LMWH) is an injectable form of anticoagulant. Standard heparin is given intravenously (IV), which means directly into a vein - usually in the arm. It is used for high-risk PEs and also in patients with certain medical problems - such as chronic kidney disease. LMWH is injected into the skin on the lower tummy (abdomen). There are different brands of heparin injection; the common ones you might see used are Clexane® and Fragmin®.
Note: LMWH is also used, in lower doses, to try to prevent VTE (PEs and DVTs) in hospital inpatients, especially those who are having, or who have had, major surgery.
Warfarin is available as a tablet or syrup.
Outside the UK, other medicines may be used which are similar to warfarin. They all belong to the group known as oral anticoagulants.
Anticoagulant treatment is continued until three months after a PE in most cases. Sometimes longer treatment is advised, especially if there is a high risk of a further embolism. Your anticoagulant clinic or doctor will be able to advise you further. If you are pregnant, regular heparin injections rather than warfarin tablets may be used. This is because warfarin can potentially cause harm (birth defects) to the unborn child. The new anticoagulants are also not suitable in pregnancy.
Supportive treatment
This means treatment to help the body cope with the effects of the PE.
Oxygen to reduce breathlessness.
In some cases, IV fluids are given to support the circulation.
Close monitoring and possibly intensive care are needed if the patient is unwell or has a massive PE.
Additional treatments
Back to contentsThese may be used to treat a high-risk or massive PE where the patient is very unwell, or where anticoagulant treatment cannot be given.
Clot-dissolving injection (thrombolysis)
This is medication given to help dissolve the blood clot. Alteplase is the medication usually used; streptokinase or urokinase are alternatives. They are more powerful than the anticoagulant treatments heparin and warfarin, described above. However, there is a greater risk of side-effects such as unwanted bleeding. Unwanted bleeding would include bleeding into the brain (intracerebral haemorrhage) - this is a type of stroke.
Filters
These can be used to stop any more blood clots from reaching the lung. The filter is placed in a large vein called the inferior vena cava (IVC). The filter is inserted via a thin tube, which is put into a large vein and then fed along the vein into the correct position. This procedure does not need an anaesthetic and can be done at the bedside.
Filters are useful if anticoagulant treatment on its own is insufficient, or for patients who cannot have anticoagulant treatment for some reason.
Surgery (embolectomy)
In some cases, it may be possible to remove the embolus surgically. This is called embolectomy. This is a major operation because it involves surgery inside the chest, close to the heart. It requires a specialist hospital and surgical team. It is generally considered as a last resort for very ill patients. The operation carries a significant risk of death. However, it would only be considered as an option if you had a massive PE which, in itself, gave a high risk of death if it were not treated.
Surgery may also be used in place of anticoagulant or clot-dissolving treatment, for patients who cannot have those treatments. This would usually be because they were at a high risk of bleeding.
Heart-lung bypass (extracorporeal life support) has (rarely) been used in some cases to treat a massive PE.
Treating the clot through a fine tube (catheter)
This type of treatment is called catheter embolectomy or catheter fragmentation of the clot. It involves threading a catheter through blood vessels until it reaches the blood clot in the lung. Once the clot is reached it may be possible to remove it or break it up (fragment it) using treatment given through the tube. This is highly specialised treatment and so is only available at certain hospitals.
Pregnancy and postnatal period
Back to contentsThere is an increased risk of PE at any stage of the pregnancy until six weeks postnatally. Any symptoms of DVT or a PE in a pregnant or postnatal woman should be taken seriously and investigated immediately.
Treatment in pregnancy is with heparin injections rather than warfarin or other tablets. This is because warfarin can potentially cause harm (birth defects) to the unborn child. For a massive PE where the patient is unwell, any of the additional treatments listed above may be used.
Treatment in pregnancy is continued until three months after the embolism or until six weeks postnatally, whichever is longer.
Postnatally, warfarin can be started in place of heparin, once bleeding from the birth has settled.
Heparin and warfarin can be taken by breastfeeding mothers. If taking warfarin and breastfeeding, it is advisable to ensure that the baby has had its routine vitamin K injection. This is because vitamin K helps counteract the effects of warfarin. (In the UK, all babies are routinely given a vitamin K injection at birth, unless parents object. Vitamin K helps prevent clotting problems in newborn babies anyway, regardless of whether the mother is taking treatment.)
Apixaban and rivaroxaban are not suitable to be taken when breast feeding.
Complications of a pulmonary embolism
Back to contentsMost people with a PE are treated successfully and do not get complications. However, there are some possible, serious complications and these include:
Collapse - due to the effects of the blood clot on the heart and circulation. This can cause a cardiac arrest where the heart stops, and may be fatal.
The PE can cause a strain on the heart. This may lead to a condition called heart failure, where the heart pumps less strongly than normal.
Blood clots can occur again later (known as a recurrent PE). Anticoagulant treatment helps to prevent this.
Complications due to treatment. The anticoagulant treatment can have side-effects. The main one is bleeding elsewhere in the body - for example, from a stomach ulcer. About 3 in 100 patients will get significant bleeding due to anticoagulant treatment for a PE. Usually this type of bleeding can be treated successfully. This type of bleeding can (rarely) be fatal (in about 3 in 1,000 cases of PE). However, it is almost always safer to take the anti-clotting treatment than not to, so as to prevent another PE which could be serious.
If there are repeated small PEs, they may (rarely) contribute to a condition where there is high pressure in the lung blood vessels (called primary pulmonary hypertension).
What is the outlook for a pulmonary embolism?
Back to contentsThis depends on the type of PE and on whether there are any other medical problems.
If a PE is treated promptly, the outlook (prognosis) is good, and most people can make a full recovery.
The outlook is less good if there is an existing serious illness which helped to cause the embolism - for example, advanced cancer. A massive PE is more difficult to treat and is life-threatening.
A PE is a serious condition and can have a high risk of death but this is greatly reduced by early treatment in hospital.
The most risky time for complications or death is in the first few hours after the embolism occurs. Also, there is a high risk of another PE occurring within six weeks of the first one. This is why treatment is needed immediately and is continued for about three months.
How can a pulmonary embolism be prevented?
Back to contentsThis involves preventing a DVT.
People having major surgery should be assessed for their DVT risk, and people at high risk of DVT may need preventative (prophylactic) doses of heparin or a similar medicine before and after surgery. Other preventative measures are also possible while in hospital.
Patient picks for Arteries

Heart health and blood vessels
Aortic dissection
An aortic dissection is a rare, serious condition. The inner layer of the aorta (the biggest blood vessel in the body, coming directly from the heart) tears. Blood then surges through the tear. This causes the inner and middle layers of the aorta to separate (dissect). Aortic dissection is a medical emergency and needs urgent treatment. The treatment for aortic dissection includes an operation to repair the wall of the aorta. Medicines to reduce blood pressure are also used. Aortic dissection is often fatal but early diagnosis and treatment of aortic dissection can greatly improve survival.
by Dr Colin Tidy, MRCGP
Heart health and blood vessels
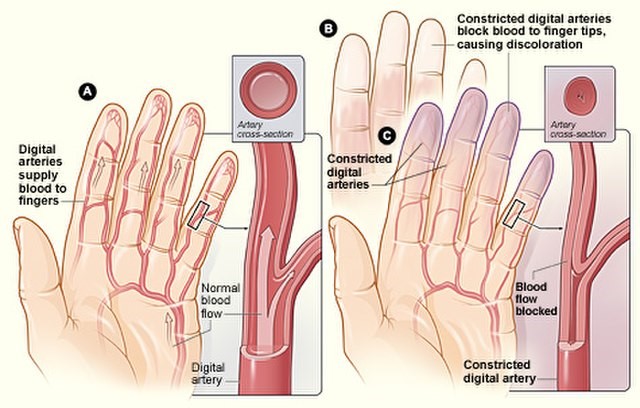
Raynaud's phenomenon
Raynaud's phenomenon (often just called Raynaud's), is a condition where the small blood vessels of the fingers become narrow (constrict). This happens most often when they are in a cool environment. Blood vessels to other extremities such as the toes, ears and nose may also be affected. It is named after Dr Maurice Raynaud, the man who first described it in 1862.
by Dr Hayley Willacy, FRCGP
Further reading and references
- Rivaroxaban for treating pulmonary embolism and preventing recurrent venous thromboembolism; NICE Technology Appraisal Guidance, June 2013
- Thrombosis and Embolism during Pregnancy and the Puerperium, the Acute Management of; Royal College of Obstetricians and Gynaecologists (April 2015)
- British Thoracic Society Guideline for the initial outpatient management of pulmonary embolism (PE); British Thoracic Society (June 2018)
- Venous thromboembolic diseases: diagnosis, management and thrombophilia testing; NICE Guidance (March 2020 - last updated August 2023)
- Guidelines for the diagnosis and management of acute pulmonary embolism developed in collaboration with the European Respiratory Society (ERS): The Task Force for the diagnosis and management of acute pulmonary embolism of the European Society of Cardiology, 2019
- Pulmonary embolism; NICE CKS, June 2023 (UK access only)
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 3 Sept 2028
5 Sept 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.