Common cold
Peer reviewed by Dr Surangi Mendis, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 9 Jan 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:CoughViral coughCoughs and colds in childrenChronic persistent cough in adultsCoughing up bloodCough medicines
The common cold is a viral infection that causes symptoms such as a runny or blocked nose, sneezing, sore throat, cough, and feeling generally unwell. Most colds improve within 7–10 days with home remedies and over-the-counter medication. Practicing good hygiene helps prevent spreading it to others.
This leaflet explains what causes the common cold, how to ease discomfort at home, and when to see a doctor.
In this article:
Video picks for Viral infections
The common cold is an infection of the nose and throat that causes symptoms such as sneezing, a runny or blocked nose, sore throat, a cough, and tiredness.
It is caused by a virus, and spreads through droplets in the air or by having direct contact with an infected person.
Treatment includes plenty of rest, hydration, pain relief, and over-the-counter remedies.
You can help prevent the spread of colds or catching them by washing your hands regularly, avoiding close contact with sick people, and practicing good hygiene.
Continue reading below
What is the common cold?
What is a cold?
A common cold is an infection of the nose and upper airways (upper respiratory tract infection) caused by a virus. As the name suggests, a common cold is extremely common. An adult can expect to get 2-4 colds a year and an older child can expect to get about 5-6 colds a year. Infants and young children (of nursery and school reception age) may get as many as 12 colds a year - it may feel as though they have cold more often than they don't.
Many different viruses cause the common cold. This is why people get colds multiple times and why immunisation against the common cold is not possible.
Respiratory tract
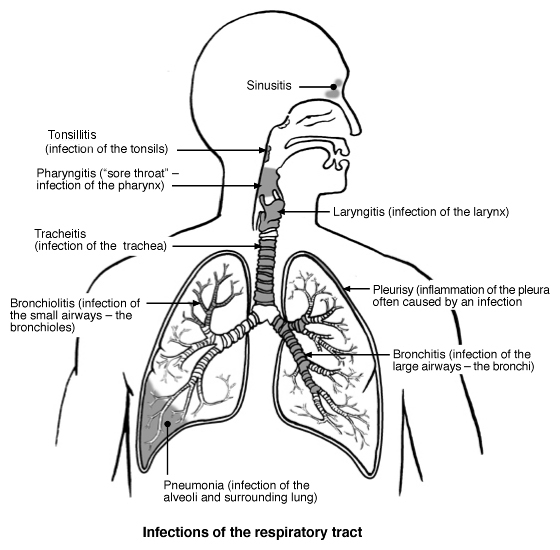
The diagram above shows the sites of a range of respiratory infections. This leaflet just deals with the common cold (an upper respiratory tract infection).
Common cold symptoms
Back to contentsThe main symptoms of a common cold are:
A blocked (congested) nose.
A runny nose.
Coughing.
Sneezing.
Feeling generally unwell.
Feeling tired.
Headache.
Body aches and pains.
At first there is a clear discharge (mucus) from the nose. This often becomes thick and yellow/green after 2-3 days. It may be difficult to sleep due to a blocked nose.
The cough often is associated with phlegm which can be clear or coloured - green phlegm (sputum) does not indicate a bacterial lower respiratory tract infection and is commonly associated with the common cold.
Continue reading below
How long does the common cold last?
Back to contentsCold symptoms are typically at their worst after 2-3 days and then gradually clear. However, the cough may carry on for up to 3 weeks after the infection has gone. This is because swelling (inflammation) in the airways, caused by the infection, can take a while to settle.
How long is the cold contagious?
Most people with the common cold will be infectious for around two weeks. However, symptoms are usually worse during the first 2-3 days, which is when they're most likely to spread the cold.
Common cold treatments
Back to contentsA main aim of treatment for the common cold is to ease symptoms whilst the immune system clears the infection.
No medications get rid of the common cold or shorten the course of the illness. The immune system will fight it off in its own time.
One or more of the following may be helpful:
Taking paracetamol or ibuprofen
Paracetamol and ibuprofen will reduce a high temperature (fever) and ease aches, pains and headaches. It is important to follow the instructions given with the medicine carefully and not to take more than the advised dose.
Children under the age of 5 years only need these medications if they have a fever or appear distressed by their symptoms.
Having plenty to drink
A mild lack of fluid in the body (dehydration) can result from a fever and therefore drinking more fluid is advised. If there is no fever, there is no evidence that drinking more fluid than usual makes a difference.
Smokers should try to stop for good. Common colds (and more serious lung diseases) tend to last longer in smokers.
Steam inhalation
There is not very much evidence that this helps but some people report finding it useful. It is very important to be careful to avoid burns and scalds, particularly with children. The safest way to inhale steam is to sit in the bathroom with the door closed whilst running a hot shower to make the room steamy.
Vapour rubs
Vapour rubs can be bought in pharmacies and supermarkets. Some people find they help with a blocked nose. The vapour can be rubbed on to the chest and/or back of the person with the cold but the area under the nose should be avoided.
Sore throat lozenges
Sucking sore throat lozenges (available from pharmacies and supermarkets) or boiled sweets may help to ease a sore throat.
Warm drinks with honey and lemon
This may help to ease a sore throat. (It is advised not to give honey to babies less than 1 year old as it is not known if this is safe.) Similarly, gargling salt water may temporarily ease symptoms of a sore throat.
Salt (saline) nose drops
These are nose drops made of a salty solution which may help clear a blocked nose. They are sometimes helpful for babies who are having difficulty breathing through a blocked nose as they feed. They can be bought from a pharmacy.
What about cold and flu remedies?
Many other cold and cough remedies at pharmacies can be bought which are only suitable for adults and older children. See the additional information below about giving these remedies to children, and also the separate leaflet Coughs and Colds in Children.
These remedies do not help fight the infection but they may be useful for certain symptoms. For example, a decongestant nasal spray may help to clear a blocked nose.
It is important to remember that cold and cough remedies often contain several ingredients and therefore it is vital to be careful about taking more than one remedy due to the risk of taking too much of one ingredient. For example, some cold remedies contain paracetamol and a decongestant, so if taking that and paracetamol as well, too much paracetamol could be ingested which could be dangerous.
Some cold and cough remedies cause drowsiness. This may be welcome at bedtime if there is difficulty sleeping due to the cold but it is important not to drive if feeling drowsy.
Using nasal sprays
A decongestant spray can be used to ease nasal congestion but must not be used for more than a few days. It can have an immediate effect to clear a blocked nose although the effect does not last very long. If a decongestant nasal spray is used for more than 7 days, it may cause the nose to become more blocked again. This is called a rebound effect.
Use of over-the-counter cough and cold medicines in children
In March 2009 an important statement was issued by the Medicines and Healthcare products Regulatory Agency (MHRA) which says:
"The new advice is that parents and carers should no longer use over-the-counter (OTC) cough and cold medicines in children under 6. There is no evidence that they work and they can cause side-effects, such as allergic reactions, effects on sleep or hallucinations.
"For 6 to 12 year olds these medicines will continue to be available but will only be sold in pharmacies, with clearer advice on the packaging and from the pharmacist. This is because the risk of side-effects is reduced in older children because they weigh more, get fewer colds and can say if the medicine is doing any good. More research is being done by industry on how well these medicines work in children aged 6-12 years."
Note: paracetamol and ibuprofen are not classed as cough and cold medicines and can still be given to children.
What about antibiotic medicines?
Antibiotics are not advised for the common cold as antibiotics do not kill viruses. The immune system can clear the infection. Even if there is bacterial involvement, antibiotics do little to speed up recovery from the common cold.
Antibiotics may make symptoms worse, as many people develop side-effects such as diarrhoea, feeling sick or a rash. Antibiotics may be prescribed if there is an underlying (chronic) lung disease such as COPD. They may also be prescribed if a complication develops, such as pneumonia - but this is unlikely to occur if you are otherwise healthy. They do not prevent complications from developing.
Continue reading below
Supplements and home remedies for the common cold
Back to contentsMany research studies have been done to try to find something which cures or prevents the common cold. So far there has been no success. Currently there is no good evidence to suggest that any of the following remedies should be used:
Garlic.
Vitamin C.
Echinacea.
Chinese herbal remedies.
There is some limited evidence that zinc supplementation may reduce the duration of a cold by two days.
Can a cold turn into pneumonia?
Most common colds do not cause complications. A common cold may trigger coughing, wheezing and shortness of breath in people with asthma, although people with asthma are no more likely to develop bacterial lower respiratory tract infections, or other lung diseases.
Sometimes the infection travels to the lung tissue, sinuses, or ears. Bacteria may thrive in the mucus so a few people with colds may go on to develop a bacterial infection of the lung tissue (pneumonia), ears or sinuses.
See your doctor if symptoms do not start to ease within two weeks or if there is a suspicion that a complication is developing. In particular, symptoms to look out for that may mean more than just a URTI include:
Headaches becoming worse or severe.
Fast breathing, shortness of breath, wheezing or chest pains.
Coughing up blood or if the phlegm (sputum) becomes rusty-coloured.
Becoming drowsy or confused.
A cough persisting for longer than 3-4 weeks.
Can the common cold be prevented?
Prevention is difficult as many different viruses can cause a common cold. However, the following are suggestions that may reduce the risk of catching a cold or of passing one on. People with a common cold should:
Try to avoid close contact with others - for example, kissing, hugging, etc.
Wash their hands often with soap and water. Many viruses are passed on by touch, especially from hands that are contaminated with a virus.
Avoid sharing towels, flannels, etc.
Children should be discouraged from sharing toys belonging to a child with a URTI. If a child has a URTI, toys should be washed with soapy water after use.
Basically, common sense and good hygiene may prevent the passing on of some viruses that cause URTIs.
Can exercise prevent a common cold?
An interesting research study (see references, below) showed that people who exercise regularly are less likely to get the common cold.
The study reviewed 1,002 people over 12 weeks during the winter. It found that the people who exercised on five or more days a week had a much lower chance of developing a common cold compared with those who did little exercise.
Frequently asked questions
Back to contentsWhy is there no cure for the common cold?
There is no cure for the common cold because it isn’t caused by just one virus. Over 200 different viruses can trigger cold symptoms, and they can change and adapt quickly. This makes it very difficult to create one treatment or vaccine that works for all types.
Can common cold cause blurry vision?
A common cold doesn’t usually cause blurry vision, but it can sometimes make your eyes feel sore, watery or irritated. If you have sinus congestion, pressure around the eyes can also make your vision feel slightly unclear for a short time.
How to make a cold go away faster?
There’s no way to cure a cold instantly, but you can help your body recover more quickly. Rest and sleep give your immune system a boost, while drinking plenty of fluids helps keep mucus thin and prevents dehydration.
Patient picks for Viral infections
%20/og.png)
Infections
Respiratory syncytial virus (RSV)
Respiratory syncytial virus (RSV) is a common infection which usually causes mild cold-like symptoms but can be more serious especially for babies, toddlers, and older people. Here we explain what causes it, what its symptoms are, and how it is treated.
by Dr Doug McKechnie, MRCGP

Infections
Bornholm disease
Bornholm disease is an illness which causes flu-like symptoms, together with pain in the chest or tummy (abdomen). It usually lasts for only a few days. Complications rarely occur. Young babies are most at risk of serious complications. Babies may need preventative treatment (immunoglobulin) to help prevent complications.
by Dr Toni Hazell, MRCGP
Further reading and references
- Over-the-counter cough and cold medicines for children; Medicines and Healthcare products Regulatory Agency (MHRA), 2014
- Nieman DC, Henson DA, Austin MD, et al; Upper respiratory tract infection is reduced in physically fit and active adults. Br J Sports Med. 2010 Nov 1.
- Hemila H, Chalker E; Vitamin C for preventing and treating the common cold. Cochrane Database Syst Rev. 2013 Jan 31;1:CD000980. doi: 10.1002/14651858.CD000980.pub4.
- Wu T, Zhang J, Qiu Y, et al; Chinese medicinal herbs for the common cold. Cochrane Database Syst Rev. 2007 Jan 24;(1):CD004782.
- Karsch-Volk M, Barrett B, Kiefer D, et al; Echinacea for preventing and treating the common cold. Cochrane Database Syst Rev. 2014 Feb 20;2:CD000530. doi: 10.1002/14651858.CD000530.pub3.
- Lissiman E, Bhasale AL, Cohen M; Garlic for the common cold. Cochrane Database Syst Rev. 2014 Nov 11;(11):CD006206. doi: 10.1002/14651858.CD006206.pub4.
- Common cold; NICE CKS, February 2022 (UK access only)
- DeGeorge KC, Ring DJ, Dalrymple SN; Treatment of the Common Cold. Am Fam Physician. 2019 Sep 1;100(5):281-289.
- Wang MX, Win SS, Pang J; Zinc Supplementation Reduces Common Cold Duration among Healthy Adults: A Systematic Review of Randomized Controlled Trials with Micronutrients Supplementation. Am J Trop Med Hyg. 2020 Jul;103(1):86-99. doi: 10.4269/ajtmh.19-0718. Epub 2020 Apr 23.
- Rao G, Rowland K; PURLs: Zinc for the common cold--not if, but when. J Fam Pract. 2011 Nov;60(11):669-71.
Continue reading below
About the author

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Surangi Mendis, MRCGP
Consultant and Medical Author
MBBS, BSc (1st), MRCGP (2014), DFSRH, PGcert otology and audiology
Surangi Mendis is a consultant in Audiovestibular Medicine and Neuro-otology at The Royal National ENT and Eastman Dental Hospitals, UCLH.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 7 Jan 2029
9 Jan 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.