Barrett's oesophagus
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 17 Mar 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Acid reflux and oesophagitisHiatus herniaBarium tests
In Barrett's oesophagus the cells that line the lower gullet (oesophagus) are abnormal. The main cause is long-standing reflux of acid from the stomach into the oesophagus. People with Barrett's oesophagus have an increased risk of developing cancer of the oesophagus. The risk is small. However, you may be advised to have regular endoscopies to detect precancerous changes to the cells in the oesophagus. If precancerous changes develop then treatment to remove or destroy the precancerous cells may be advised.
In this article:
Video picks for Other digestive conditions
Continue reading below
What is Barrett's oesophagus?
Barrett's oesophagus
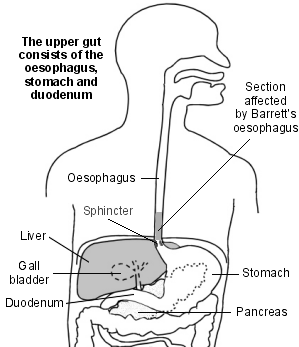
Barrett's oesophagus is a condition which affects the lower gullet (oesophagus). It is named after the doctor who first described it.
In Barrett's oesophagus, the cells lining the affected area of oesophagus become changed.
The cells of the inner lining (epithelium) of a normal oesophagus are pinkish-white, flat cells (squamous cells). The cells of the inner lining of the area affected by Barrett's oesophagus are tall, red cells (columnar cells). The columnar cells are similar to the cells that line the stomach.
Another name sometimes used by doctors for Barrett's oesophagus is columnar-lined oesophagus (CLO).
Understanding the oesophagus and stomach
When we eat, food passes down the gullet (oesophagus) into the stomach. Cells in the lining of the stomach make acid and other chemicals which help to digest food. Stomach cells also make a thick liquid (mucus) which protects them from damage caused by the acid. The cells on the inside lining of the oesophagus are different and have little protection from stomach acid.
There is a circular band of muscle (a sphincter) at the junction between the oesophagus and stomach. This relaxes to allow food down but normally tightens up and stops food and acid leaking back up (refluxing) into the oesophagus. So, the sphincter acts like a valve.
Is Barrett's oesophagus harmful?
Back to contentsThe changed cells of Barrett's oesophagus are not cancerous (malignant). However, these cells have an increased risk, compared with normal gullet (oesophageal) cells, of turning cancerous in time. The changed cells in Barrett's oesophagus can develop something called dysplasia. A cell with dysplasia is an abnormal cell. It is not cancerous but is more likely than other cells to develop into cancer. It is often called a precancerous cell.
Dysplasia
There are various degrees of dysplasia - from low-grade dysplasia to high-grade (severe) dysplasia. Cells that are classed as high-grade dysplasia have a high risk of turning cancerous at some point in the future.
But note: if you have Barrett's oesophagus, the chance that it will progress to dysplasia, then to high-grade dysplasia, and then to cancer of the oesophagus, is small. In the majority of cases with Barrett's oesophagus, the changes in the cells remain constant and do not progress. Studies have shown that, for a person diagnosed with Barrett's oesophagus, their lifetime risk of developing cancer of the oesophagus is about 1 in 20 for men and about 1 in 33 for women.
Continue reading below
Barrett's oesophagus causes
Back to contentsThe cause of Barrett's oesophagus, in most cases, is thought to be due to long-term gastro-oesophageal reflux disease (GORD), with reflux of acid and other stomach contents into the gullet (oesophagus) from the stomach. The acid irritates the lining of the lower oesophagus and causes inflammation (oesophagitis). With persistent reflux, eventually the lining (epithelial) cells change to those described above.
Risk factors
Back to contentsIt is thought that about 1 in 20 people who have recurring acid reflux eventually develop Barrett's oesophagus. The risk is mainly in people who have had severe acid reflux for many years. However, some people who have had fairly mild symptoms of reflux for years can develop Barrett's oesophagus.
Barrett's oesophagus seems to be more common in men than in women. It typically affects people between the ages of 50 and 70 years.
Other risk factors include hiatus hernia, past history of inflammation of the oesophagus (oesophagitis) or narrowing of the oesophagus (oesophageal stricture).
Continue reading below
Symptoms of Barrett's oesophagus
Back to contentsMost people with Barrett's oesophagus have symptoms of acid reflux.
If you have Barrett's oesophagus and you develop any new symptoms, such as weight loss, bringing up (vomiting) blood or difficulty swallowing, it is very important that you see a doctor urgently. These are some of the symptoms that you may get from complications of gastro-oesophageal reflux and Barrett's oesophagus. These complications are rare but can include a sore (ulcer) or cancer of the gullet (oesophagus).
What are the symptoms of acid reflux and inflammation of the gullet (oesophagitis)?
Heartburn is the main symptom of acid reflux. It is a burning feeling that rises from the upper tummy (abdomen) or lower chest up towards the neck. (It is confusing, as it has nothing to do with the heart.) Other common acid reflux symptoms include:
Feeling sick (nauseated).
An acid taste in the mouth.
Burping (belching).
A burning pain when you swallow hot drinks.
Like heartburn, these symptoms tend to come and go and tend to be worse after a meal. People with Barrett's oesophagus will usually have (or will have had in the past) the symptoms associated with acid reflux and oesophagitis.
What causes acid reflux and who is affected by it?
The circular band of muscle at the bottom of the oesophagus is called the sphincter. It normally prevents acid reflux. Problems occur if the sphincter does not work very well. This is common but in most cases it is not known why it does not work so well.
However, having a hiatus hernia makes you more prone to reflux. A hiatus hernia occurs when part of your stomach protrudes through the lower chest muscle (diaphragm) into the lower chest. See the separate leaflet called Hiatus Hernia for more details.
How is acid reflux treated?
A medicine which prevents your stomach from making acid is a common treatment and usually works well. Some people take short courses of treatment when symptoms flare up. Some people need long-term daily treatment to keep symptoms away. An operation to tighten the sphincter muscle is an option in severe cases which do not respond to medication, or where full-dose medication is needed every day to control symptoms.
There are also various things that you can try to change in your lifestyle that may help to treat your acid reflux. These include:
Losing weight if you are overweight.
Stopping smoking if you are a smoker.
Reducing your alcohol intake if you drink a lot of alcohol.
See the separate leaflet called Acid Reflux and Oesophagitis (Heartburn) for more details.
How is Barrett's oesophagus diagnosed?
Back to contentsBarrett's oesophagus itself usually causes no symptoms. However, you are likely to have, or have had, the symptoms of long-standing or severe reflux disease described earlier.
Gastroscopy (endoscopy)
Diagnosis of Barrett's oesophagus may include a gastroscopy if you have severe or persistent symptoms of acid reflux. For this test, a thin, flexible telescope is passed down the gullet (oesophagus) into the stomach. This allows a doctor or nurse to look inside. This test can usually help to diagnose Barrett's oesophagus. The change in colour of the lining of the lower oesophagus from its normal pale white to a red colour strongly suggests that Barrett's oesophagus has developed.
A biopsy
If Barrett's oesophagus is suspected during gastroscopy then several small samples (biopsies) are taken of the lining of the oesophagus during the gastroscopy. These are sent to the laboratory to be looked at under the microscope. The characteristic columnar cells which are described above confirm the diagnosis. The cells are also examined to see if they have any signs of dysplasia (see above).
Barrett's oesophagus treatment
Back to contentsTreatment of acid reflux
This treatment is as described above. You are likely to be advised to take acid-suppressing medication for the rest of your life. It is unclear as to whether treating the acid reflux helps to treat or reverse your Barrett's oesophagus and more studies are ongoing. However, this treatment should help any symptoms that you may have.
Monitoring (surveillance)
When you have been diagnosed with Barrett's oesophagus, you may be advised to have a gastroscopy and biopsy at regular intervals to monitor the condition. This is called surveillance. The biopsy samples aim to detect whether dysplasia has developed in the cells, in particular if high-grade dysplasia has developed.
The exact time period between each gastroscopy and biopsy sample can vary from person to person. It may be every 2-5 years (depending on the length of oesophagus that is affected) if there are no dysplasia cells detected. Once dysplasia cells are found, the check may be needed more frequently. If high-grade dysplasia develops, you may be offered treatment to remove the affected cells from the gullet (oesophagus). (Treatment details are discussed below.)
Surgery may be considered
If you develop high-grade dysplasia or oesophageal cancer, the traditional treatment is to undergo surgery to remove the oesophagus (oesophagectomy). This is a major operation and complications following surgery, sometimes serious and life-threatening, are not uncommon.
But most people who develop Barrett's oesophagus do not go on to need an oesophagectomy. Also, newer therapies that have been developed are becoming more popular options if you develop high-grade dysplasia or early cancer.
Newer treatments for Barrett's oesophagus
Back to contentsResearch continues to find out which treatment is best. If you are diagnosed with Barrett's oesophagus, your specialist should be able to give you up-to-date information on the pros and cons of surveillance. They should also be able to advise on the current situation about the various treatment options should you develop dysplastic changes to the cells.
Various ways of removing just the abnormal dysplastic cells from the lining of the oesophagus (or even early cancers that just affect the lining on the oesophagus) have recently been developed. These include the following:
Photodynamic therapy (PDT)
This is a type of laser treatment. It has been used in the past but has been largely replaced by radiofrequency ablation.
Epithelial radiofrequency ablation (EFA)
This treatment uses a radiofrequency energy coil. Again, this involves a gastroscopy. During the procedure a small coil is guided towards the abnormal section of your oesophagus. The coil then emits heat energy which destroys the abnormal cells. Nearby normal cells then multiply and replace the destroyed abnormal cells.
Argon plasma coagulation
This treatment uses a jet of argon gas, together with an electric current, to burn away dysplastic cells.
Endoscopic mucosal resection (EMR)
This is a procedure that is done via instruments passed down the side of a gastroscope. Basically, the affected inner lining of the oesophagus is stripped off.
Balloon cryotherapy
The National Institute for Health and Care Excellence (NICE) has looked at the evidence for effectiveness and safety of a procedure called balloon cryoablation in treating Barrett's oesophagus.
This procedure is usually done using sedation. A balloon catheter (a thin tube with a deflated balloon on the end) is passed into the oesophagus, using a small flexible telescope. It is lined up with the abnormal tissue and inflated. Nitrous oxide is then sprayed through very precisely into the area to destroy abnormal cells by the extreme cold.
The committee found that there was not enough evidence that it was safe and effective. They have therefore recommended that until there is more evidence, it should only be offered as part of a research study.
What is the outcome (prognosis) for Barrett's oesophagus?
Back to contentsBarrett's oesophagus increases the risk of oesophageal cancer, but most people with Barrett's oesophagus will not develop oesophageal cancer.
It is estimated that, without treatment, between 5 and 10 out of 100 people with Barrett's oesophagus will develop oesophageal cancer over 10-20 years.
Patient picks for Other digestive conditions

Digestive health
Mallory-Weiss tear
Mallory-Weiss syndrome (also called Mallory-Weiss tear) is the name given to bleeding and other symptoms caused by a tear in the lining of the upper part of the gut (gastrointestinal tract). It is usually diagnosed by having a test called a gastroscopy (endoscopy). This involves a tube being passed down through the gullet (oesophagus) into the stomach. In many cases, the bleeding has stopped by the time gastroscopy takes place and specific treatment is not needed. The tear usually heals by itself after a few days.
by Dr Philippa Vincent, MRCGP

Digestive health
Gastroparesis
Gastroparesis is now more commonly known as delayed gastric emptying. It is a chronic condition in which food passes through the stomach and into the gut (intestine) more slowly than usual. The nerves that usually trigger the stomach muscles to move food out of the stomach and into the intestine don't work as effectively as normal. This is not caused by an obstruction or structural abnormality but by a failure of the normal mechanisms.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Fitzgerald RC, di Pietro M, Ragunath K, et al; British Society of Gastroenterology guidelines on the diagnosis and management of Barrett's oesophagus. Gut. 2014 Jan (updated 2015).
- Epithelial radiofrequency ablation for Barrett's oesophagus; NICE Interventional procedures guidance, May 2010
- Photodynamic therapy for Barrett's oesophagus; NICE Interventional procedures guidance, June 2010
- Balloon cryoablation for Barrett’s oesophagus; NICE Interventional procedures guidance, October 2020
- Bujanda DE, Hachem C; Barrett's Esophagus. Mo Med. 2018 May-Jun;115(3):211-213.
- Eluri S, Shaheen NJ; Barrett's esophagus: diagnosis and management. Gastrointest Endosc. 2017 May;85(5):889-903. doi: 10.1016/j.gie.2017.01.007. Epub 2017 Jan 18.
- Amadi C, Gatenby P; Barrett's oesophagus: Current controversies. World J Gastroenterol. 2017 Jul 28;23(28):5051-5067. doi: 10.3748/wjg.v23.i28.5051.
- Barrett's oesophagus and stage 1 oesophageal adenocarcinoma: monitoring and management; NICE guideline (February 2023)
- Endoscopic radiofrequency ablation for Barrett's oesophagus with low‑grade dysplasia or no dysplasia; NICE Interventional procedures guidance, July 2014.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 16 Feb 2028
17 Mar 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.