Vomiting blood
Haematemesis
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Philippa Vincent, MRCGPLast updated 4 Jul 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
In this series:Mallory-Weiss tear
You should call an ambulance or go directly to the nearest emergency department if you are vomiting blood. Often the bleeding will stop quite quickly but in some cases it can become severe and life-threatening. So always seek medical help quickly.
There is a range of different causes - these are discussed below. Many causes can be treated but the first priority is to make sure the bleeding stops. The rest of this leaflet aims to give some background information but is not a substitute for obtaining immediate medical attention if vomiting blood.
In this article:
Video picks for Other signs and symptoms
Continue reading below
What is vomiting blood (haematemesis)?
The medical word for vomiting blood is haematemesis. Vomiting blood is usually a sign of a problem within the upper gut - the gullet (oesophagus), stomach or the first part of the gut (small intestine) known as the duodenum.
Vomiting of blood is a medical emergency. In many cases the bleeding will stop quite quickly but in some cases it can become severe and life-threatening. Therefore, call an ambulance or go directly to the nearest emergency department if you vomit blood.
What are the causes of vomiting blood?
Back to contentsCommon causes of throwing up blood include:
A tear in the gullet (oesophagus) caused by prolonged retching.
Swallowed blood from a nosebleed.
Vomiting blood needs emergency medical assessment in hospital.
Bleeding from the oesophagus
Causes include:
Oesophageal varices. Varices are enlarged, swollen blood vessels in the lining of the oesophagus or stomach. They are one of the possible complications of liver cirrhosis. In cirrhosis, scarred liver tissue blocks the blood flow through the liver. This causes an increase in pressure in the vein that takes blood from the gut to the liver (the portal vein). The increased pressure pushes back into the gut and causes the veins to swell in the oesophagus. The swellings are fragile and therefore may bleed heavily into the gullet.
Inflammation of the oesophagus (oesophagitis) is often due to acid reflux from the stomach (gastro-oesophageal reflux disease (GORD)). The inflamed oesophagus sometimes bleeds.
Oesophageal cancer sometimes causes bleeding into the oesophagus.
Mallory-Weiss syndrome is bleeding caused by a tear in the lining of the oesophagus or stomach. The tear can be caused by anything that leads to a sudden rise in pressure in the stomach or the oesophagus. For example, repeated retching or vomiting, excessive straining, violent coughing or hiccupping.
Bleeding from the stomach
Causes include:
Stomach (gastric) ulcer. An ulcer is a small breakdown in the lining of the stomach. An ulcer may bleed, sometimes heavily. There are several causes of stomach ulcers, including:
Infection with a bacteria called Helicobacter pylori. This can usually be treated quite easily.
Anti-inflammatory medicines that are used to treat conditions such as arthritis, sometimes cause stomach ulcers.
Aspirin, used commonly to prevent blood clots.
Stress.
Stomach cancer sometimes causes bleeding into the stomach.
Inflammation of the stomach lining (gastritis) has similar causes to stomach ulcers.
Varices in the lining of the stomach may occur similar to oesophageal varices described above.
Mallory-Weiss syndrome may affect the lining of the stomach - described above.
Bleeding from the duodenum
Causes include:
Duodenal ulcer. An ulcer may bleed, sometimes heavily. Like stomach ulcers, a duodenal ulcer is usually caused by an infection with the bacteria called H. pylori. This can usually be treated quite easily. Anti-inflammatory medicines and aspirin, which are common causes of stomach ulcers, are less common causes of duodenal ulcers.
Inflammation of the duodenum lining (duodenitis) has similar causes to duodenal ulcers.
Rare causes from any part of the upper gut
Include:
Radiation poisoning.
Uncommon infections of the gut (gastrointestinal tract).
Injury.
No cause identified. In some cases the cause cannot be found, even after tests.
Bleeding which has not come from the gut
Sometimes when blood is vomited, it has not come from the gut. For example, following a nosebleed, blood may be swallowed and then vomited. Sometimes it can be difficult to tell whether the blood has been vomited up from the gut, or coughed up from the lungs or throat.
A note about anticoagulants
Medicines like warfarin or the newer oral anticoagulants (such as rivaroxaban, apixaban and dabigatran - often called DOACs) do not usually cause the bleeding but, if there is an underlying problem (such as an ulcer), they will make the bleeding worse.
The upper gut
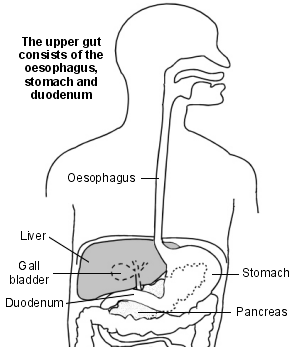
Continue reading below
Symptoms alongside vomiting blood
Back to contentsOther symptoms may occur at the same time as vomiting blood such as:
Feeling unwell.
Dizziness.
Fainting.
Other gut symptoms.
The presence and type of other symptoms may help to point to a cause of the bleeding. Sometimes there are no other symptoms at first.
What tests may be needed if I'm vomiting blood
Back to contentsA clinician's assessment
They are likely to ask various questions about the nature of the bleeding and ask about any other symptoms. They will also perform an examination.
The clinician will also try to make a judgement about how much blood has been lost, where the bleeding is coming from and how serious the situation is. They will be able to tell this from the history and also by checking the pulse and blood pressure.
If it is clear that the blood is coming from the upper gut, tests are usually done to identify the cause.
Blood tests
Blood tests will usually be done to assess the general situation, for example, how much blood has been lost, and whether intravenous fluids or a blood transfusion is needed to counter any large amount of blood loss.
Also, blood tests may help to assess the liver function if there is 'scarring' of the liver (cirrhosis), or to help diagnose other causes of the bleeding.
Gastroscopy
A gastroscopy (endoscopy) is an internal examination. It involves examining the inside of the digestive tract, using a thin, flexible tube that has a light and camera at one end.
The telescope is passed down the oesophagus into the stomach and to the upper duodenum. The cause of the bleeding can often be identified by endoscopy.
Continue reading below
Treatment for vomiting blood
Back to contentsInitial treatment
The initial treatment may require a drip into a vein to give fluid, or even a blood transfusion if a lot of blood has been lost. This may not be necessary if the bleeding has been minor and has stopped. However, if the bleeding is severe, full resuscitation and emergency fluid/blood replacement may be required.
Other treatments
This will depend on the cause. Stopping the bleeding can be done by using instruments that can be passed down the endoscope but studies have shown that this is rarely necessary as most bleeding settles on its own, even if it has been very heavy.
Sometimes, emergency surgery may be needed to control severe ongoing bleeding.
Once bleeding has stopped, further treatment depends on the cause. For details, see individual leaflets on the various diseases that can cause vomiting blood.
Types of bleeding from the upper gut
Back to contentsThe type of bleeding is sometimes described as follows:
Dark blood
This is often referred to as a 'coffee ground' colour. This suggests that the bleed has been relatively slow. The blood has been in contact with stomach acid long enough for the acid to turn the blood a dark brown/red colour. The bleeding in this situation may not yet have been heavy. However, it may become heavy at a later time.
A large amount of bright red blood suggests a rapid and large bleed.
Melaena
This is the medical word for old, dark blood in stools (faeces). With melaena, the stools become very dark or black. There is often a tar-like consistency.
Vomiting blood and having melaena are symptoms that often go together. Having both symptoms together means that there has been a lot of bleeding into the gut.
Patient picks for Other signs and symptoms

Signs and symptoms
Dry eyes
Dry eyes can affect anyone. They are usually nothing to worry about and can often be treated at home. Artificial tears, gels, and soothing ointments usually ease symptoms.
by Dr Colin Tidy, MRCGP

Signs and symptoms
Pins and needles
Numbness is a condition where you can't feel anything in part of your body, some describe it as a 'limb falling asleep'. Pins and needles are a tingling or numbness feeling or prickling sensation that is often felt in hands or feet. Usually this is due to pressure on nerves/nerve cells or the blood vessels that supply nerves. This often happens after you've been in an awkward position, like sitting cross-legged, or it may be the sign of a trapped nerve. Occasionally, it may be the sign of a more serious underlying problem such as diabetes. The most common causes are mentioned below.
by Dr Hayley Willacy, FRCGP
Further reading and references
- Acute upper gastrointestinal bleeding in over 16s: management; NICE Clinical Guideline (August 2016)
- Baumer TE; Haemoptysis or haematemesis? The not so bleeding obvious. BMJ Case Rep. 2014 Apr 29;2014:bcr2014204059. doi: 10.1136/bcr-2014-204059.
- Khoury L, Hill DA MD, Panzo M, et al; The Natural History of Hematemesis in the 21st Century. Cureus. 2018 Jul 23;10(7):e3029. doi: 10.7759/cureus.3029.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 3 Jul 2027
4 Jul 2024 | Latest version
11 Dec 2012 | Originally published
Authored by:
Dr Tim Kenny, MRCGP

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.