Erythema chronicum migrans
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 12 Jun 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Continue reading below
What is erythema chronicum migrans?
Erythema chronicum migrans is a characteristic clinical feature of Lyme disease (Lyme borreliosis). It is a distinctive rash, which occurs in the majority of people infected with Borrelia burgdorferi. This infection is transmitted to humans by the bite of a tick from the genus Ixodes.
How common is erythema chronicum migrans? (Epidemiology)1
Back to contentsLyme disease is not common in the UK, with an estimated 2,000 to 3,000 new cases each year in England and Wales.
In the UK, areas where infection is acquired include Exmoor, the New Forest, the South Downs, parts of Wiltshire and Berkshire, Surrey, West Sussex, Thetford Forest, the Lake District, the North Yorkshire moors and the Scottish Highlands.
Infection may also be acquired abroad and mostly by holidaymakers. The majority are acquired in the USA, France, Germany, Scandinavia and other northern, eastern and central European countries. The infection can also be found in temperate forested areas of Asia, including Russia, China and Japan.
In Europe erythema chronicum migrans occurs as a presenting feature in up to 90% of those infected.2 Presentation does appear to depend upon the Borrelia species involved; therefore, in other parts of the world the rash may be a less common presenting sign.
Continue reading below
Symptoms of erythema chronicum migrans (presentation)3
Back to contentsThe characteristic manifestation of early Lyme disease (stage 1) is erythema chronicum migrans: a circular rash at the site of the infectious tick attachment, which radiates from the bite. It can appear within 3-36 days, but typically in 7-10.
It starts as a red macule or papule at the site of the tick bite after a (typically 7- to 10-day) delay.
The rash is round or oval, and pink, red or purple. There is often central sparing giving a target-like appearance, and the diameter is usually larger than 5 cm. The nature of the rash and the likelihood of its presence are partly dependent on the species involved and therefore differ between continents.
Erythema migrans 'bullseye" rash of Lyme disease
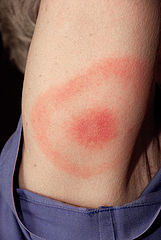
© CDC/James Gathany, Public domain, via Wikimedia Commons
Untreated, this can last for some weeks, but eventually resolves.
Common areas include the popliteal fossa, groin, the axilla, the thorax and the trunk. The hairline and scalp are especially common in children.
It may be associated with other symptoms of infection, including fatigue, myalgia, arthralgia, headache, fever, stiff neck, and regional lymphadenopathy.
It may also be associated with later developments such as carditis, neurological disease, arthritis, and acrodermatitis chronica atrophicans (a swollen, bluish-red skin lesion on a distal extremity).
The National Institute for Health and Care Excellence (NICE) recommends diagnosing Lyme disease in people with erythema migrans that:4
Increases in size and may sometimes have a central clearing.
Is not usually itchy, hot or painful.
Usually becomes visible from 1 to 4 weeks (but can appear from 3 days to 3 months) after a tick bite and lasts for several weeks.
Is usually at the site of a tick bite.
In the absence of erythema migrans, the diagnosis of Lyme disease can be very difficult with non-specific clinical signs and symptoms that may or may not be supported by laboratory evidence.5
Differential diagnosis6
Back to contentsLocal tick bite reactions.
Continue reading below
Investigations1 3
Back to contentsFor anyone with erythema migrans who have no evidence of focal symptoms of Lyme disease (eg neurological, cardiac, or joint involvement), investigations are not required and start treatment with oral antibiotics (see below).
Management of erythema chronicum migrans4 7
Back to contentsAlthough the rash will resolve spontaneously over weeks or months, antibiotics help prevent progression to disseminated Lyme disease.
For the treatment of Lyme disease without focal symptoms (eg, neurological, carditis) but with erythema migrans and/or non-focal symptoms, NICE recommends:
First choice: oral doxycycline: 100 mg twice per day or 200 mg once per day for 21 days.
First alternative: oral amoxicillin: 1 g 3 times per day for 21 days.
Second alternative: oral azithromycin: 500 mg daily for 17 days (azithromycin should not be used to treat people with cardiac abnormalities associated with Lyme disease because of its effect on QT interval).
Prevention of erythema chronicum migrans
Back to contentsAvoid exposure to tick bites.
Remove ticks as soon as possible. Ticks take some time to transmit infection, so this may be prevented if removed quickly.
Antibiotic prophylaxis can be offered in endemic areas under certain circumstances if the tick bite can be positively identified.
Further reading and references
- Mygland A, Ljostad U, Fingerle V, et al; EFNS guidelines on the diagnosis and management of European Lyme neuroborreliosis. Eur J Neurol. 2010 Jan;17(1):8-16, e1-4. doi: 10.1111/j.1468-1331.2009.02862.x. Epub 2009 Nov 23.
- Erythema chronicum migrans; DermIS (Dermatology Information System)
- Prevention and control of tick-borne disease in Europe - Information to healthcare professionals; European Centre for Disease Prevention and Control
- Coburn J, Garcia B, Hu LT, et al; Lyme Disease Pathogenesis. Curr Issues Mol Biol. 2021;42:473-518. doi: 10.21775/cimb.042.473. Epub 2020 Dec 23.
- Lyme disease (and erythema migrans); Primary Care Dermatology Society (PCDS). Last updated May 2022.
- Lyme disease; DermNet.
- Lyme disease: guidance, data and analysis; Public Health England - now UK Health Security Agency (last updated 2022)
- The epidemiology, prevention, investigation and treatment of Lyme borreliosis in United Kingdom patients: a position statement by the British Infection Association; J Infect. 2011 May;62(5):329-38. doi: 10.1016/j.jinf.2011.03.006. Epub 2011 Mar 21.
- Lyme disease; NICE CKS, November 2022 (UK access only)
- Lyme disease; NICE Guidance (April 2018 - last updated October 2018)
- Bobe JR, Jutras BL, Horn EJ, et al; Recent Progress in Lyme Disease and Remaining Challenges. Front Med (Lausanne). 2021 Aug 18;8:666554. doi: 10.3389/fmed.2021.666554. eCollection 2021.
- Shapiro ED; Clinical practice. Lyme disease. N Engl J Med. 2014 May 1;370(18):1724-31. doi: 10.1056/NEJMcp1314325.
- British National Formulary (BNF); NICE Evidence Services (UK access only)
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
12 Jun 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free