Leukoplakia
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 30 Jun 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Continue reading below
What is leukoplakia?
Leukoplakia is a white patch adhering to oral mucosa that cannot be removed by rubbing. It is usually a diagnosis of exclusion. The term should be exclusively reserved for idiopathic lesions when investigations fail to reveal any cause. The term carries no histological association.
Vulval lesions
Leukoplakia formerly also applied to vulval lesions but several international societies have developed a standardised nomenclature based on histopathological findings in vulval lesions. Leukoplakia, along with other terms, such as vulvar dystrophy, kraurosis vulvae, hyperplastic vulvitis and lichen sclerosus et atrophicus should no longer be used.
In their place the general term is 'non-neoplastic epithelial disorders', which are subdivided into three major categories: squamous cell hyperplasia, lichen sclerosus and other dermatoses. Therefore, suspicious white patches on the vulva should be biopsied to establish their correct classification and be treated accordingly. This is covered in the separate Lichen Sclerosus and Vulval Problems articles.
Leukoplakia causes (aetiology)
Back to contentsIt is considered a pre-malignant lesion. The transformation rate is between approximately 0.1-17.5%.1 A 2020 population-based cohort study found the overall 5 year absolute risk of transformation to malignancy was 3.3%.2
Factors most frequently blamed for the development of idiopathic leukoplakia include chronic irritation, candidiasis, vitamin A or vitamin B deficiency and endocrine disturbances. Tobacco use and alcohol consumption have been frequently cited but the evidence base supporting this has been questioned.3
It may also be associated with other conditions such as:
Continue reading below
Leukoplakia epidemiology
Back to contentsPrevalence - the estimated worldwide prevalence is around 2%.5
Most cases of leukoplakia occur in middle and older age.1 Less than 1% of patients are under the age of 30 years.6
Leukoplakia is more common in men than in women, with a male-to-female ratio of 2:1.7
Leukoplakia symptoms
Back to contentsLeukoplakia
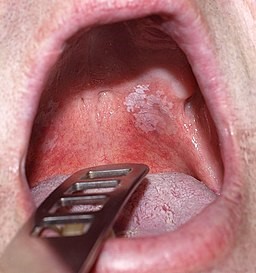
© Klaus D. Peter, Gummersbach, Germany, CC BY 3.0 DE, via Wikimedia Commons
There are three stages that have been described:
The earliest lesion is non-palpable, faintly translucent and has white discolouration.
Next, localised or diffuse, slightly elevated plaques with an irregular outline develop. These lesions are opaque white and may have a fine, granular texture.
In some instances, the lesions progress to thickened, white lesions, showing induration, fissuring and ulcer formation.
Five clinical criteria demonstrate a particularly high risk of malignant change:
The verrucous (speckled) type is considered high-risk.
Erosion or ulceration within the lesion is highly suggestive of malignancy.
The presence of a nodule indicates malignant potential.
A lesion that is hard in its periphery is predictive of malignant change.
Leukoplakia of the anterior floor of the mouth and undersurface of the tongue is strongly associated with malignant potential.
One study found that men over the age of 60 with oral leukoplakia on the lateral or ventral aspect of the tongue, who had a non-homogenous lesion with high-grade dysplasia, were most at risk of malignant change.8
Continue reading below
Investigations9
Back to contentsAny suspicious areas should be referred urgently for biopsy. Endoscopy has been used to improve the identification of oral lesions and the recognition of morphology suggestive of malignant change.10
In all cases, the relative risk of malignant potential is determined by the presence of epithelial dysplasia upon histological examination.
Biomarkers of gene instability, such as aneuploidy and allelic imbalance, are predictive of cancer risk of oral pre-malignant lesions or intra-epithelial neoplasia but have not stood the test of time with respect to malignant change in oral leukoplakia.3 However, demonstration of recurrent genomic alterations by using techniques such as gene mapping may be of value.11
Leukoplakia differential diagnosis1
Back to contentsChemical burn
Lichen planus
White sponge naevus
Leukoplakia treatment and management
Back to contentsThere is no consensus on the management of oral leukoplakia.9 There is little or no high quality evidence for effective treatment to prevent malignant change.12
General measures
Patients should abstain from alcohol and tobacco, although the evidence to support this advice has been questioned.
Pharmacological
Photodynamic therapy, the carotenoids beta-carotene and lycopene and systemic retinoic acid (vitamin A) have demonstrated limited effectiveness in speeding up the resolution of oral leukoplakia. The systemic side-effects of retinoic acid reduce the risk:benefit ratio for this indication considerably.13
Currently there is no evidence for effective treatment to prevent malignant change or recurrence.
A Cochrane review concluded that whilst there may be some benefit from vitamin A and beta-carotene in healing oral lesions, relapses and adverse effects were common. Further research of existing non-surgical therapies is needed.14
Surgical
Surgical excision of leukoplakia may be considered.
Frequent clinical observation accompanied by photographic records is recommended. Because of the unpredictable behaviour of dysplastic lesions, immediately obtain a biopsy on any areas that are suggestive, or that change in appearance.
Carbon dioxide laser ablation is the most commonly used surgical therapy:15
The area heals rapidly and apparently healthy mucosa is left behind. One study found that carbon dioxide laser ablation caused less pain and swelling than conventional surgery.5
Uncertainty remains regarding the risk of invasive carcinomas subsequently arising in sites previously treated. The recurrence rate after laser surgery has varied widely in the literature and studies have reported a range from 7.7% to 38.1%. It is thought that these differences have been dependent on differences in the variety and conditions of the laser beams, the follow-up period and race. Therefore, regular follow-up is obligatory after treatment.16
Erbium, chromium: yttrium-scandium-gallium-garnet (Er,Cr:YSGG) lasers appear to give less morphological distortion simulating cellular atypia than other types of lasers.17
Prognosis
Back to contentsBetween 1 and 9% of people with oral leukoplakia will develop invasive cancer in the lesion or a frank malignancy.1 Parameters associated with an increased risk of malignant transformation were female gender and smoking.
The malignant potential of non-homogeneous lesions is almost seven times higher compared to homogeneous types.18 19
Despite excision, small dysplastic lesions can be followed by multiple carcinomas and a fatal outcome.1 In addition, some dysplastic lesions may have a worse prognosis than isolated carcinomas without leukoplakia. However, dysplastic lesions can regress spontaneously. Therefore, the behaviour of dysplastic lesions is unpredictable and once dysplasia has been found in a lesion, the outcomes are guarded.
There is currently no reliable management protocol. Prolonged and close follow-up care is essential but the prognosis may still be poor.
'Hairy' leukoplakia20
Back to contentsThis is associated with Epstein-Barr virus (EBV) and occurs mostly in people with HIV who are severely immunocompromised.21 It can affect patients who are HIV negative and many cases have been reported in heart, kidney and bone marrow transplant recipients and in patients with haematological malignancies.22 23
To view the appearance of hairy leukoplakia please refer to the DermNet New Zealand photos below.24 25
The natural history of hairy leukoplakia is variable. Lesions may frequently appear and disappear spontaneously. Hairy leukoplakia is often asymptomatic and many patients are unaware of its presence. Some patients with hairy leukoplakia do experience symptoms including mild pain, dysaesthesia, alteration of taste and the psychological impact of its unsightly cosmetic appearance.
Management of hairy leukoplakia26
As a benign lesion with low morbidity, hairy leukoplakia does not require specific treatment in every case. Indications for treatment include symptoms attributable to the lesion or a patient's desire to eliminate the lesion for cosmetic reasons. The variable natural history of the lesion and its tendency toward spontaneous resolution should be considered in any management decision.
Options include:27
Systemic antiviral therapy, which usually achieves resolution of the lesion within 1-2 weeks of therapy.20
Topical therapy with podophyllin resin 25% solution, which usually achieves resolution after 1-2 treatment applications.28
Topical therapy with retinoic acid (tretinoin), which has been reported to resolve hairy leukoplakia.
Ablative therapy, which can also be considered for small hairy leukoplakia lesions. Cryotherapy has been reported as successful but is not widely used.
Further reading and references
- Feller L, Lemmer J; Oral Leukoplakia as It Relates to HPV Infection: A Review. Int J Dent. 2012;2012:540561. doi: 10.1155/2012/540561. Epub 2012 Feb 28.
- Yanik EL, Katki HA, Silverberg MJ, et al; Leukoplakia, Oral Cavity Cancer Risk, and Cancer Survival in the U.S. Elderly. Cancer Prev Res (Phila). 2015 Sep;8(9):857-63. doi: 10.1158/1940-6207.CAPR-15-0091. Epub 2015 Jul 9.
- van der Waal I; Oral leukoplakia; a proposal for simplification and consistency of the clinical classification and terminology. Med Oral Patol Oral Cir Bucal. 2019 Nov 1;24(6):e799-e803. doi: 10.4317/medoral.23372.
- Mohammed F, Fairozekhan AT; Oral Leukoplakia
- Chaturvedi AK, Udaltsova N, Engels EA, et al; Oral Leukoplakia and Risk of Progression to Oral Cancer: A Population-Based Cohort Study. J Natl Cancer Inst. 2020 Oct 1;112(10):1047-1054. doi: 10.1093/jnci/djz238.
- Arduino P, Bagan J, El-Naggar A, et al; Urban legends series: oral leukoplakia. Oral Dis. 2013 Jan 11. doi: 10.1111/odi.12065.
- Meisel P, Holtfreter B, Biffar R, et al; Association of periodontitis with the risk of oral leukoplakia. Oral Oncol. 2012 Sep;48(9):859-63. doi: 10.1016/j.oraloncology.2012.02.022. Epub 2012 Mar 20.
- Lopez-Jornet P, Camacho-Alonso F; Comparison of pain and swelling after removal of oral leukoplakia with CO(2) laser and cold knife: a randomized clinical trial. Med Oral Patol Oral Cir Bucal. 2013 Jan 1;18(1):e38-44.
- Oral Leukoplakia; DermNet NZ
- Shen ZY, Liu W, Zhu LK, et al; A retrospective clinicopathological study on oral lichen planus and malignant transformation: analysis of 518 cases. Med Oral Patol Oral Cir Bucal. 2012 Nov 1;17(6):e943-7.
- Liu W, Shi LJ, Wu L, et al; Oral cancer development in patients with leukoplakia--clinicopathological factors affecting outcome. PLoS One. 2012;7(4):e34773. doi: 10.1371/journal.pone.0034773. Epub 2012 Apr 13.
- Kumar A, Cascarini L, McCaul JA, et al; How should we manage oral leukoplakia? Br J Oral Maxillofac Surg. 2012 Nov 14. pii: S0266-4356(12)00598-0. doi: 10.1016/j.bjoms.2012.10.018.
- Yang SW, Lee YS, Chang LC, et al; Use of endoscopy with narrow-band imaging system in evaluating oral leukoplakia. Head Neck. 2012 Jul;34(7):1015-22. doi: 10.1002/hed.21857. Epub 2011 Nov 3.
- Cervigne NK, Machado J, Goswami RS, et al; Recurrent genomic alterations in sequential progressive leukoplakia and oral cancer: drivers of oral tumorigenesis? Hum Mol Genet. 2014 May 15;23(10):2618-28. doi: 10.1093/hmg/ddt657. Epub 2014 Jan 8.
- Lodi G, Franchini R, Warnakulasuriya S, et al; Interventions for treating oral leukoplakia to prevent oral cancer. Cochrane Database Syst Rev. 2016 Jul 29;7:CD001829. doi: 10.1002/14651858.CD001829.pub4.
- Ribeiro AS, Salles PR, da Silva TA, et al; A review of the nonsurgical treatment of oral leukoplakia. Int J Dent. 2010;2010:186018. doi: 10.1155/2010/186018. Epub 2010 Feb 23.
- Lod G et al; Interventions for treating oral leukoplakia to prevent oral cancer, Cochrane, 2016.
- de Pauli Paglioni M, Migliorati CA, Schausltz Pereira Faustino I, et al; Laser excision of oral leukoplakia: Does it affect recurrence and malignant transformation? A systematic review and meta-analysis. Oral Oncol. 2020 Jun 12;109:104850. doi: 10.1016/j.oraloncology.2020.104850.
- Chiniforush N et al; Leukoplakia Removal by Carbon Dioxide Laser (CO2) Laser, Journal of Lasers in Medical Sciences Volume 3 Number 1 Winter 2012.
- Seoane J, Gonzalez-Mosquera A, Lopez-Nino J, et al; Er,Cr:YSGG laser therapy for oral leukoplakia minimizes thermal artifacts on surgical margins: a pilot study. Lasers Med Sci. 2013 Jan 17.
- Leukoplakia; WHO International Agency for Research on Cancer, 2013
- Brzak BL, Mravak-Stipetic M, Canjuga I, et al; The frequency and malignant transformation rate of oral lichen planus and leukoplakia--a retrospective study. Coll Antropol. 2012 Sep;36(3):773-7.
- Alramadhan SA, Bhattacharyya I, Cohen DM, et al; Oral Hairy Leukoplakia in Immunocompetent Patients Revisited with Literature Review. Head Neck Pathol. 2021 Sep;15(3):989-993. doi: 10.1007/s12105-021-01287-8. Epub 2021 Jan 11.
- Khammissa RA, Fourie J, Chandran R, et al; Epstein-Barr Virus and Its Association with Oral Hairy Leukoplakia: A Short Review. Int J Dent. 2016;2016:4941783. doi: 10.1155/2016/4941783. Epub 2016 Mar 7.
- Cho HH, Kim SH, Seo SH, et al; Oral hairy leukoplakia which occurred as a presenting sign of acute myeloid leukemia in a child. Ann Dermatol. 2010 Feb;22(1):73-6. doi: 10.5021/ad.2010.22.1.73. Epub 2010 Feb 28.
- Davis G, Perks A, Liyanage P, et al; Oral hairy leukoplakia arising in a patient with hairy cell leukaemia: the first reported case. BMJ Case Rep. 2017 Apr 6;2017. pii: bcr-2016-218663. doi: 10.1136/bcr-2016-218663.
- Parlatescu I, Gheorghe C, Coculescu E, et al; Oral leukoplakia - an update. Maedica (Buchar). 2014 Mar;9(1):88-93.
- Oral hairy Leukaemia; DermNet NZ - image example
- Rathee M, Jain P; Hairy Leukoplakia
- Mortazavi H, Safi Y, Baharvand M, et al; Oral White Lesions: An Updated Clinical Diagnostic Decision Tree. Dent J (Basel). 2019 Feb 7;7(1). pii: dj7010015. doi: 10.3390/dj7010015.
- Brasileiro CB, Abreu MH, Mesquita RA; Critical review of topical management of oral hairy leukoplakia. World J Clin Cases. 2014 Jul 16;2(7):253-6. doi: 10.12998/wjcc.v2.i7.253.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 29 Jun 2027
30 Jun 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free