Lichen sclerosus
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 19 Jun 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Synonyms: lichen sclerosus et atrophicus, balanitis xerotica obliterans, lichen albus, white spot disease, Csillag's disease, kraurosis vulvae
Continue reading below
What is lichen sclerosus?
Lichen sclerosus (LS) is a chronic inflammatory dermatosis which usually affects the skin of the anogenital region in women, and the glans penis and foreskin in men. In men this was previously called balanitis xerotica obliterans (BXO) and in women lichen sclerosus et atrophicus, terms which are no longer in use.1 It occurs less commonly in extragenital areas. It does not cause any systemic disease outside the skin.
Causes of lichen sclerosus (aetiology)12
Back to contentsThe cause is unknown:
Many findings obtained in recent years point increasingly towards an autoimmune-induced disease in genetically predisposed patients and further away from an important impact of hormonal factors.3
There is an association with other autoimmune diseases, particularly thyroid disease, in women but not in men.
There is a positive family history in 10-12% of those affected.
In men there is an association with increased BMI, coronary artery disease, diabetes and smoking.
Preceding infections may play a provocative part.
The role for borrelia infection is still controversial. There is no evidence for a link in patients in the UK and the USA.
Trauma and an occlusive moist environment may act as precipitating factors. Lichen sclerosus rarely occurs in men who are circumcised at birth, suggesting that the moist environment under the foreskin may predispose. Appearance in surgical wounds and after radiotherapy or sunburn suggests that trauma may be a precipitant.
Continue reading below
How common is lichen sclerosus? (Epidemiology)1
Back to contentsThe true incidence of LS is unknown and is probably underestimated. Incidence is higher in females than males. It is believed there is a prevalence of around 3% of adult women and 0.07% of men. Incidence in boys with phimosis may be as high as 100%, although reported ranges spread from 12-100%. The condition is extra-genital in around 6%.3
In women there are two peaks of incidence - in prepubertal girls and postmenopausal women. In males it occurs in young boys and in adult men.
Symptoms of lichen sclerosus (presentation)1
Back to contentsThe lesions are white thickened patches (porcelain-white papules and plaques). These may progress to crinkled white patches (like cigarette paper). Active lesions may have areas of ecchymosis, hyperkeratosis or bullae.
Lichen sclerosus
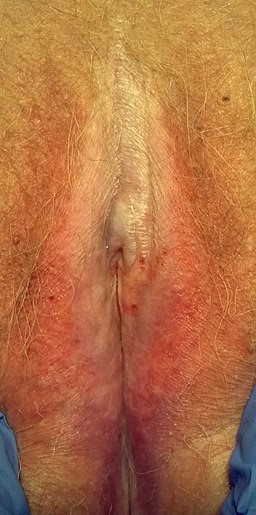
© Mikael Häggström, CC0, via Wikimedia Commons
Further images of LS in males and females as well as images of extra-genital LS are available on DermNet NZ.4
Women
Symptoms:
Itch - can be severe and disturb sleep, as it is usually worse at night. This is usually the first symptom.
Pain can occur if there are fissures or erosions, leading to dyspareunia.
Perianal lesions are common and may cause constipation.
May be asymptomatic and found incidentally.
Signs:
White lesions as above. These may be patchy, or in a figure-of-eight area around the vulva and anus.5
Destructive scarring may cause shrinking of the labia, and narrowing of the introitus, or the clitoris may be obscured by adhesions. Genital involvement does not occur; the vagina and cervix are always spared.
Perianal lesions occur in around 30% of cases.
In girls, the signs may be mistaken for sexual abuse, as ecchymosis often occurs and can be very striking.
Men
Lesions are usually on the prepuce, glans penis and coronal sulcus.
Symptoms:
Soreness, haemorrhagic blisters.
Itching is not usually a common symptom in men.
Dyspareunia, painful erections due to phimosis.
If there is meatal scarring, poor urinary stream or dysuria. There may be ballooning on urination if there is phimosis.
Signs:
White patches on the glans or prepuce.
Haemorrhagic vesicles or purpura.
Rarely, blisters or ulcers.
If scarring has occurred - phimosis, wasting of the prepuce, meatal narrowing/thickening. Balanitis may occur.
Perianal involvement rarely (if ever) occurs.
May be asymptomatic.
Extragenital sites
LS elsewhere is much less common; it is most often on the upper trunk, axillae, buttocks and lateral thighs.
More rarely sites include the face, scalp, hands, feet and nails.
Oral lesions are extremely rare, but can affect sites where there is cornified stratified squamous epithelium - eg, tongue, gingiva and hard palate.
Continue reading below
Diagnosing lichen sclerosus (investigations)15
Back to contentsThe diagnosis is usually made clinically. In primary care, if the clinician is not confident in identification and management, referral should be made to a primary care colleague with a special interest or to secondary care (usually a specialist vulval dermatology clinic or urology clinic in men). Lesions should be well documented for follow-up purposes, ideally with diagrams or photography. Other investigations may include:
Biopsy:
Is indicated only when there is diagnostic uncertainty or suspected malignancy.
Should be considered where presentation is atypical - for example, in young adult women, in extragenital lesions or pigmented lesions.
Is not always practical - eg, in children. It may be preferable to start treatment and to monitor response.
Is essential if lesions do not respond to adequate treatment.
Swabs are not required routinely but may be necessary in cases where there is erosive disease to exclude infection such as candidiasis or herpes simplex.
Blood tests: current evidence and guidelines advise that an autoantibody screen to look for associated autoimmune disease is useful only if there are clinical features to suggest an autoimmune disorder. Consider autoimmunity screen and thyroid function tests if symptoms are present. There is no evidence to support testing for autoantibodies without a clinical indication.
Differential diagnosis
Back to contentsIn children, signs may mimic those of child sexual abuse. Note that a diagnosis of LS does not automatically exclude sexual abuse. Indeed trauma related to sexual abuse may potentially be a trigger in some cases.
Various other skin, genital or mucosal conditions, including:
Bowen's disease (squamous cell carcinoma in situ (SCCIS)); if on the penis, this is Queyrat's erythroplasia).
Management of lichen sclerosus15
Back to contentsWhere should patients be treated and followed up?
LS can be managed by a GP, dermatologist or gynaecologist, depending on local expertise and protocols. Referral may be required to confirm the diagnosis.
Specialist advice on treatment may be needed - eg, if a woman does not appear to respond to treatment. Men with urinary symptoms should be referred to a urologist. Vulval clinics and urology clinics have a role, particularly if there are complications.
Long-term follow-up is needed for women with LS, particularly for patients on long-term steroids and with poorly controlled LS.
Patients who respond well to treatment and need only small amounts of topical steroids should be reviewed annually - this can be in primary care. Give patients clear instructions to report immediately any persistent new lumps, skin changes, erosions or ulcers.
Female anogenital LS
The current evidence demonstrates the efficacy of clobetasol propionate, mometasone furoate, and pimecrolimus in treating genital lichen sclerosus.6 Clobetasol has been demonstrated to be more effective than pimecrolimus.78
A reducing course of clobetasol propionate 0.05% is the usual treatment:
The usual regimen is - once-daily (at night) use for one month, alternate nights for one month, then twice-weekly for one month with review at three months.
If the patient's symptoms return during reduction of treatment, go back up to the frequency that was effective.
Advise using half a fingertip unit. A 30 g tube of clobetasol propionate should last 12 weeks; the patient should then be reviewed.
If the treatment has been successful, the hyperkeratosis, ecchymoses, fissuring and erosions should have resolved but the atrophy and colour change remain.
Maintenance treatment may be required with as-required use of very potent steroids.
Ointment bases are less allergenic, but the choice of base will depend on patient preference.
Intralesional triamcinolone may be used in specialist settings for those who have been resistant to initial steroid treatment, after biopsy.
Detailed information should be given to patients which includes information about using topical steroids.
Although some studies have demonstrated some benefit of (unlicensed) topical tacrolimus and pimecrolimus, long-term safety of these drugs is not established and there are concerns about an increased risk of malignancy with their use in this condition, which already has a premalignant potential. Therefore, these medications should not be used as first-line treatment. They are not recommended for use at any point in the current British Association of Dermatologists guideline.
NB: oestrogen or testosterone creams should not be used to treat LS. Testosterone is no better than petroleum jelly and there may be adverse effects. It must not be used in children.
Male anogenital LS
Use ultra-potent topical steroids (clobetasol propionate 0.05%) applied once-daily until remission, then gradually reduced.
May need repeat courses if there is relapse or intermittent use (eg, once weekly) to maintain remission.
Again, intralesional triamcinolone can be used where there is treatment failure, after biopsy has taken place.
Referral for consideration of circumcision is recommended if there is phimosis and there has been no response to steroid treatment after 1-3 months.
Other treatments for anogenital LS
Treat any secondary infection.
Advice to patients:
Wash with bland emollients - eg, aqueous cream; avoid topical irritants and tight clothing; use lubricants if necessary; give details of support groups.
Warn patients to seek medical attention if there are possible signs of malignancy, ie if the area develops a persistent lump, change in texture of the skin (such as thickening) or a non-healing ulcer/erosion.
If relevant, advise which creams/ointments may be used with condoms.
If there is apparent treatment failure, consider:
Compliance: for example, patients may be deterred by side-effect warnings on steroid preparations; elderly patients may have difficulty applying the creams.
Whether the diagnosis is correct. There may be an additional problem - eg, infection or allergy to the preparation.
Whether there is a complication. (See 'Complications and their treatment', below.)
Extragenital LS
Options used include potent topical steroids, acitretin, methotrexate and UVA-1 phototherapy. Shave excision and CO2 laser have also been used successfully, treating symptoms and appearance.
Asymptomatic patients
Treatment is recommended if patients have features of active disease - eg, ecchymosis, hyperkeratosis or progressive atrophy.
Complications of lichen sclerosus1
Back to contentsScarring:
This is common and may cause urinary symptoms or sexual dysfunction.
May require surgery - eg, circumcision, meatal dilatation or vulval surgery. Labial fusing can cause dyspareunia or urinary difficulties.
Urethral involvement occurs in 20% of men which can cause urethral stricture.
One-stage or staged repairs using oral mucosa grafts are the most recommended procedures for the treatment of LS urethral strictures in men9.
Constipation due to perianal fissures - prescribe softening laxatives.
Squamous cell carcinoma (SCC):
There is a small risk of SCC of the vulva (3.5-5% lifetime risk). About 60% of cases of vulval SCC arise on a background of LS however.
It has been estimated that around 4-5% of men with LS will develop SCC of the penis . However, it is unclear if LS itself causes the development of SCC or if it is due to co-existent infection with human papillomavirus.
Long-term follow-up is advisable.
Warn patients about signs of malignancy and biopsy any suspicious lesions.
Extragenital lesions do not appear to have any increased risk of malignancy.
Dysaesthesia:
Vulvodynia or penile dysaesthesia can occur following inflammatory conditions of the genitalia. This is a neuropathic type of pain and does not respond to steroid treatment.
Topical local anaesthetics (eg, 5% lidocaine ointment) can be given to those with vestibulodynia and vulvodynia or penile dysaesthesia.
Development of a clitoral pseudocyst. This occurs due to a build-up of debris under clitoral adhesions. Refer to a gynaecologist if there is pain or recurrent infection.
Sexual dysfunction. Be aware this may be a complication and can have a significant impact on quality of life; offer referral.
Prognosis23
Back to contentsIn most females it is a chronic condition, although symptom control is often successful. In men there is a higher chance of remission or cure. Scarring is not reversible with pharmacological treatment.
Symptom remission can be achieved in 98% of compliant and 75% of non-compliant women by using potent topical steroids.
In males, particularly young boys, a course of steroids may prevent the need for circumcision.
Most men are either cured by topical treatment with ultrapotent steroid (50-60%) or by circumcision (>75%).10
However, in some cases LS recurs. More complex cases may be an overlap syndrome with lichen planus, and may be more difficult to treat.
75% of girls who develop LS prepubertally will continue to need maintenance treatment after menarche.
The lifetime risk of SCC is around 4-5% in both males and females.
Extragenital lesions are less likely to be chronic, and have a better chance of cure.
Further reading and references
- Lichen sclerosus; Primary Care Dermatology Society
- Lewis FM, Tatnall FM, Velangi SS, et al; British Association of Dermatologists guidelines for the management of lichen sclerosus, 2018. Br J Dermatol. 2018 Apr;178(4):839-853. doi: 10.1111/bjd.16241.
- Kirtschig G; Lichen Sclerosus-Presentation, Diagnosis and Management. Dtsch Arztebl Int. 2016 May 13;113(19):337-43. doi: 10.3238/arztebl.2016.0337.
- Fistarol SK, Itin PH; Diagnosis and treatment of lichen sclerosus: an update. Am J Clin Dermatol. 2013 Feb;14(1):27-47. doi: 10.1007/s40257-012-0006-4.
- Lichen sclerosus; DermNet NZ
- UK National Guideline on the Management of Vulval Conditions; British Association for Sexual Health and HIV (2014)
- Chi CC, Kirtschig G, Baldo M, et al; Topical interventions for genital lichen sclerosus. Cochrane Database Syst Rev. 2011 Dec 7;(12):CD008240. doi: 10.1002/14651858.CD008240.pub2.
- Goldstein AT, Creasey A, Pfau R, et al; A double-blind, randomized controlled trial of clobetasol versus pimecrolimus in patients with vulvar lichen sclerosus. J Am Acad Dermatol. 2011 Jun;64(6):e99-104. doi: 10.1016/j.jaad.2010.06.011. Epub 2011 Feb 25.
- Funaro D, Lovett A, Leroux N, et al; A double-blind, randomized prospective study evaluating topical clobetasol propionate 0.05% versus topical tacrolimus 0.1% in patients with vulvar lichen sclerosus. J Am Acad Dermatol. 2014 Jul;71(1):84-91. doi: 10.1016/j.jaad.2014.02.019. Epub 2014 Apr 3.
- Palminteri E, Brandes SB, Djordjevic M; Urethral reconstruction in lichen sclerosus. Curr Opin Urol. 2012 Nov;22(6):478-83. doi: 10.1097/MOU.0b013e328358191c.
- Edmonds EV, Hunt S, Hawkins D, et al; Clinical parameters in male genital lichen sclerosus: a case series of 329 patients. J Eur Acad Dermatol Venereol. 2012 Jun;26(6):730-7. doi: 10.1111/j.1468-3083.2011.04155.x. Epub 2011 Jun 27.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 18 Jun 2027
19 Jun 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free