Epiglottitis
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 15 Aug 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Epiglottitis is the term used to describe inflammation and swelling of the epiglottis which lies just behind the root of the tongue. It is usually caused by infection with a bacteria. The usual symptoms are a severe sore throat, pain or difficulty swallowing and a high temperature (fever). Breathing difficulties can occur. Prompt treatment is needed to ensure that enough oxygen can reach the lungs and usually includes antibiotics. If epiglottitis is treated quickly, the outlook is generally very good. Untreated, it can be life-threatening. Since immunisation against Hib was introduced, the number of children who develop epiglottitis in the UK has reduced dramatically.
At a glance
Epiglottitis is inflammation and swelling of the epiglottis, usually caused by infection.
Swelling can block the airway and make breathing difficult.
Symptoms include a high temperature, sore throat, painful swallowing, and noisy breathing.
If epiglottitis is suspected, call 999 for an ambulance immediately.
Do not lie the person down or try to look in their throat.
Treatment involves oxygen, antibiotics, and sometimes a tracheostomy or ventilator.
The Hib vaccine helps prevent epiglottitis in children.
In this article:
Video picks for Throat and tonsils
Continue reading below
What is epiglottitis?
Epiglottitis is inflammation of the epiglottis. It is almost always caused by infection with a germ (bacterium). The common bacteria that cause epiglottitis are Streptococcus pneumoniae and Haemophilus influenzae type b (Hib). It is sometimes called supraglottitis as the inflammation can affect the tissues around the epiglottis as well as or instead of the epiglottis itself.
Infection leads to inflammation and swelling of the epiglottis. Because of its position in the throat, if the epiglottis swells, it can affect breathing by blocking (obstructing) the passage of air through the voice box (larynx) to the windpipe (trachea) and the lungs.
Epiglottitis can be confused with croup which is a common childhood viral infection affecting the voice box and windpipe. Croup is far less dangerous than epiglottitis and usually improves on its own. It does not require antibiotics as it is caused by a virus. See the separate leaflet called Croup for more details.
How common is epiglottitis?
Back to contentsEpiglottitis now occurs in about 2 people per 100,000 in the UK. Around 5 in 100 of people who develop epiglottitis will die as a result.
Epiglottitis can occur at any age. In children, it most commonly affects those between the ages of 2 and 5 years. However, since the Hib vaccine was introduced in the UK and other countries in the 1990s, the number of children who develop epiglottitis has reduced dramatically. It is now extremely rare in children. See the separate leaflet called 6-in-1 Vaccine (Including DTaP, Polio, Hib and Hep B Immunisations for more details.
Following the introduction of the Hib vaccine for children, the typical person who develops epiglottitis is now an adult rather than a child (but it is still rare for adults to get epiglottitis). People are more at risk if they have a weakened immune system - for example, having had chemotherapy.
Hib infection is still the commonest cause of epiglottitis worldwide. It is now very rare but can be caused by other bacteria (eg, streptococcus which usually causes strep throat), viruses or fungi.
Continue reading below
Epiglottitis symptoms
Back to contentsSore throat.
A hoarse voice.
Pain when swallowing.
Drooling.
Noisy breathing.
Breathing difficulties.
When to get medical help
If someone has suspected epiglottitis, they should be admitted to hospital immediately. It should be treated as an emergency by calling 999/112/911 for an ambulance. Do not lay the person down or try to look in their throat, as this can cause the throat to close off completely and may cause breathing to stop altogether.
Noisy breathing and breathing difficulty need to be treated quickly. Someone with epiglottitis usually prefers to sit upright and lean slightly forwards, often with their tongue sticking out (protruding). This position helps to open up their airway to let more oxygen through to the lungs.
Someone with epiglottitis can be scared and panicked. A grunting noise may be heard as they try to breathe. As less oxygen gets through to the lungs, their skin colour can change and they can become grey or blue.
In general, older children and adults with epiglottitis tend to have less severe symptoms than children and the symptoms tend to develop more slowly.
How is epiglottitis diagnosed?
Back to contentsEpiglottitis is usually diagnosed by the typical symptoms. A procedure called a nasopharyngoscopy or laryngoscopy may be used in hospital to help confirm epiglottitis. A thin flexible tube is run down the nose into the throat. Swelling or redness of the epiglottis can be seen through the laryngoscope.
Sometimes an X-ray of the neck is taken and this can show a swollen epiglottitis. A swab is usually taken from the throat and sent to the laboratory to look for infection. A blood sample may also be taken, again to look for signs of infection. A computerised tomography (CT) scan or a magnetic resonance imaging (MRI) scan may also be needed.
Continue reading below
Epiglottitis treatment
Back to contentsOxygen
If someone has epiglottitis, the most important treatment is to ensure that they are getting enough oxygen into their lungs. Oxygen can be given using a mask over their mouth and nose but some people need additional breathing support using a ventilator. A ventilator is a machine that is mechanically operated to maintain the flow of oxygen and air into and out of the lungs.
Tracheostomy
In severe cases, if the epiglottis is swollen and blocking the airway, even if oxygen is given it would not be able to reach the lungs. So, a procedure called a tracheostomy is done. This is where a small cut is made in the windpipe (trachea). This allows a breathing tube to pass below the swollen epiglottis so that oxygen can be delivered to the lungs. Someone with a tracheostomy may also need help with their breathing using a ventilator.
Antibiotics
Antibiotics are another important part of the treatment. They help to fight the infection. An antibiotic which is capable of dealing with a wide range of germs (a broad-spectrum antibiotic) is usually used - eg, ceftriaxone. It is usually given directly into a vein (intravenously) from a drip. A steroid medicine may also be given to help reduce the inflammation around the epiglottis.
Ventilation
If someone with epiglottitis is having trouble with their breathing and they need to be ventilated or need a tracheostomy, they will need to be transferred to an intensive care unit. They will be kept on the ventilator until the antibiotics have started to work and the inflammation of the epiglottis has had time to improve.
Epiglottitis is a medical emergency that needs to be treated in hospital. This is because the person's breathing needs to be monitored and medicines need to be given intravenously. Also, if there is difficulty swallowing, a drip may be needed to provide nourishment and fluid directly into a vein.
If treatment is not started quickly, the swelling of the epiglottis can totally block (obstruct) the airway. This means that air is not able to reach the lungs and this can cause collapse and death.
With prompt treatment, most people recover in a few days and are able to leave hospital in about a week.
Complications of epiglottitis
Back to contentsIf epiglottitis is not treated quickly, the airway can become totally blocked. This means that air is not able to get into the lungs and the person can die. However, if epiglottitis is treated quickly, the outlook is generally good. Recovery usually takes about seven days in children and may be a little longer in adults.
Occasionally, a collection of pus can collect in the area of the epiglottis (an epiglottic abscess). This is mainly seen in adults. It sometimes requires surgical drainage.
Rarely, infection can spread from the epiglottis to other parts of the body, including the ear, the brain, the heart and the lungs.
Preventing epiglottitis
Back to contentsThe Hib vaccine
The Hib vaccine is advised for all babies at 2 months, 3 months, 4 months and 12 months. It is part of the routine vaccination programme in the UK. This has led to a dramatic reduction in cases of epiglottitis in children. The Hib vaccine is over 95% effective.
Antibiotics
Close contacts of someone who has been diagnosed with epiglottitis (for example, people who live in the same household) may be given antibiotics to help reduce the chance of them developing the infection.
What is the epiglottis?
Back to contentsHead and neck showing larynx
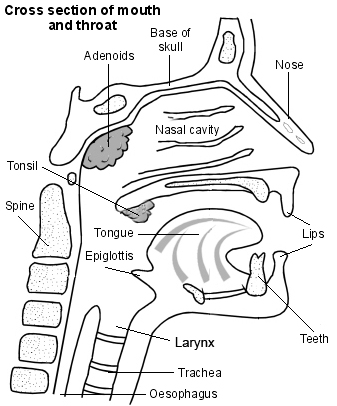
The epiglottis is a leaf-shaped flap of cartilage tissue that lies just behind the back of the tongue.
When swallowing, the epiglottis covers the voice box (larynx), stopping food from entering the windpipe (trachea). The voice box is in the front of the neck above the windpipe. It contains the vocal cords and also allows air to pass from the mouth into the windpipe and from there to the lungs.
Patient picks for Throat and tonsils

Ear, nose and throat
Tonsil stones
Tonsil stones are stones which can form at the back of the throat within the tonsils. They are not serious but can sometimes cause problems with a sore throat or bad breath.
by Dr Philippa Vincent, MRCGP

Ear, nose and throat
Glandular fever
Glandular fever (also known as infectious mononucleosis) is a viral infection that most often affects teenagers and young adults. Although it can make some people feel quite ill, full recovery is usual.
by Dr Philippa Vincent, MRCGP
Frequently asked questions
Can adults expect a similar recovery time to children if they get epiglottitis?
While most people recover in a few days and are able to leave hospital in about a week, recovery times can sometimes differ between adults and children. The article mentions that recovery usually takes about seven days in children, but it may be a little longer in adults.
If I am a close contact of someone with epiglottitis, will I automatically be given antibiotics?
Close contacts, such as household members, may be given antibiotics. This is done to help reduce the chance of them developing the infection, but it is not stated as an automatic or universal measure. The decision would likely be made by a medical professional.
How long will I need to stay in hospital if I'm diagnosed with epiglottitis?
With prompt treatment, most people recover in a few days and are able to leave hospital in about a week. The hospital stay also allows for continuous monitoring of breathing and intravenous administration of medicines.
Why is it dangerous to lie someone down or look in their throat if epiglottitis is suspected?
It is crucial not to lay the person down or try to look in their throat if epiglottitis is suspected. Doing so can cause the throat to close off completely, which may lead to breathing stopping altogether.
What is the typical position a person with epiglottitis might adopt to help with their breathing?
Someone with epiglottitis usually prefers to sit upright and lean slightly forwards, often with their tongue sticking out (protruding). This position helps to open up their airway, allowing more oxygen to reach the lungs.
Further reading and references
- Glynn F, Fenton JE; Diagnosis and management of supraglottitis (epiglottitis). Curr Infect Dis Rep. 2008 May;10(3):200-4.
- Chen C, Natarajan M, Bianchi D, et al; Acute Epiglottitis in the Immunocompromised Host: Case Report and Review of the Literature. Open Forum Infect Dis. 2018 Feb 17;5(3):ofy038. doi: 10.1093/ofid/ofy038. eCollection 2018 Mar.
- O'Bryant SC, Lewis JD, Cruz AT, et al; Influenza A-Associated Epiglottitis and Compensatory Pursed Lip Breathing in an Infant. Pediatr Emerg Care. 2018 Sep 21. doi: 10.1097/PEC.0000000000001589.
- Guerra AM, Waseem M; Epiglottitis.
- Apuy M, Yock-Corrales A, Moreno AM, et al; Streptococcus Pyogenes Epiglottitis in a Child: A Case Report. Cureus. 2022 Apr 13;14(4):e24123. doi: 10.7759/cureus.24123. eCollection 2022 Apr.
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 13 Aug 2028
15 Aug 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.