Acute angle-closure glaucoma
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 8 Jun 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Glaucoma
Acute angle-closure glaucoma is a serious eye condition that occurs when the fluid pressure inside the eye rises quickly, leading to sudden, severe eye pain, a red eye and reduced or blurred vision. It is a medical emergency.
In this article:
Video picks for Eye conditions
Key points
Acute angle‑closure glaucoma happens when the eye’s drainage angle suddenly gets blocked, causing a fast rise in eye pressure.
Symptoms include sudden severe eye pain, redness, blurred vision, nausea, and vomiting.
Acute angle-closure glaucoma is a medical emergency. Urgent treatment is needed to relieve symptoms and to prevent permanent loss of vision.
Treatment includes medications to lower eye pressure, and sometimes laser therapy to open the drainage angle.
Continue reading below
What is acute angle-closure glaucoma?
What is acute angle glaucoma?
Acute angle-closure glaucoma occurs when the flow of aqueous humour (the clear fluid in the front section of the eye) out of the eye is blocked and, therefore, the pressure inside the eye becomes too high very quickly. It is an emergency because, if it is not treated quickly, it can lead to permanent loss of vision.
Acute angle-closure glaucoma is also sometimes referred to as acute closed-angle glaucoma or just acute glaucoma. For ease, this leaflet will use the term 'acute glaucoma'.
There are other types of glaucoma which occur more gradually. The most common type is chronic open-angle glaucoma (also called primary open-angle glaucoma or simply chronic glaucoma). See the separate leaflet called Chronic Open-angle Glaucoma for details.
Other, less common, types of glaucoma are secondary glaucoma and congenital glaucoma. 'Congenital' means that it is present from birth. The rest of this leaflet deals only with acute glaucoma.
What causes acute glaucoma?
Back to contentsIn acute glaucoma there is a sudden blockage of the drainage of the aqueous humour fluid from the eye. As more fluid continues to be made, the pressure inside the eye rises quickly. This can start to damage the optic nerve at the back of the eye and vision can be affected.
What causes the blockage?
Some people are more prone to develop acute glaucoma because of the structure of their eye. For example, if the area near the base of the iris is very narrow, the trabecular meshwork (spongy tissue at the edge of the eye through which the aqueous humour normally flows) can become blocked more easily. If the lens is thicker and sits further forward than normal, this can have the same effect. Both these cause what is known as a narrow drainage angle or a shallow anterior chamber and can make acute glaucoma more likely.
In other people, the iris can be thinner and more floppy than usual, making it more likely to cause blockage of the trabecular meshwork.
The muscles of the iris (coloured part of the eye) control the size of the pupil (black circle in the eye). In someone who is prone to acute glaucoma, the dilation (enlarging) of the pupil can mean their lens can 'stick' to the back of their iris. This blocks the route of the aqueous humour through the iris from the posterior chamber or through the pupil to the anterior chamber.
The aqueous fluid collects behind the iris and causes the iris to bulge forwards and block the trabecular meshwork. This further prevents drainage of the aqueous fluid from their eye. It is particularly likely to happen in people with a thinner, floppier iris or a shallow anterior chamber.
Continue reading below
What triggers acute glaucoma?
Back to contentsThere are some situations that may trigger acute glaucoma in people who have an underlying predisposition. For example, acute glaucoma is more likely to come on when the pupil is dilated. This could be whilst watching television in dim light, during stress or excitement or at night. Some medicines can also trigger acute glaucoma in people prone to it as can general anaesthetics in older people.
For the population as a whole the chance of getting acute glaucoma with these medicines is extremely small, so they are commonly prescribed without serious concern. However, if you have been warned that you may be prone to acute glaucoma, you should tell your doctor before starting new medication or eye drops, especially if it is one on the list below.
Commonly used medicines which may trigger acute glaucoma
Eye drops used to dilate the pupil - these may be used for eye check-ups.
Antidepressants of the tricyclic or selective serotonin reuptake inhibitor (SSRI) types.
Some of the medicines used to treat feeling sick and being sick (nausea and vomiting), or the mental health condition called schizophrenia. (There is a type of medicine called phenothiazines, one of which is chlorpromazine.)
Ipratropium (used for asthma).
Topiramate (used for migraines and epilepsy).
Some medicines used to treat allergies or stomach ulcers, such as chlorphenamine and cimetidine.
Medication used during a general anaesthetic.
Steroid medicines (such as those used in asthma and emphysema) can sometimes cause high pressure in the eyes when used for long periods of time (chronic open-angle glaucoma) but do not usually cause acute glaucoma.
How common is acute glaucoma?
Back to contentsAbout 1 in 1,000 people develop acute glaucoma in their lifetime so it is a rare condition. It is commoner in people over the age of 40 years though it most often happens at around age 60-70 years. It is more common in long-sighted people and in women. It is also more common in people of South-East Asian or Inuit origin.
There is an increased risk of developing acute glaucoma where a close relative (parent or sibling) has also had acute glaucoma. This is because an eye shape may have been inherited which makes acute glaucoma more likely. An optician would be able to advise when, and how often, eye checks should be carried out in someone with a family history of acute glaucoma.
Continue reading below
Acute glaucoma symptoms
Back to contentsThe symptoms usually start suddenly. They include:
Sudden, severe pain within one eye and an ache around the eye.
Redness of the eye.
The pupil is usually fixed (does not expand or contract as normal) in a "mid-point" position and, therefore, looks different from the other pupil.
Blurred or reduced vision, often with circles (haloes) seen around lights.
The pain may spread around the head and be felt as a severe headache.
Some people develop a feeling of sickness (nausea) and are sick (vomit).
The eye usually feels hard and tender.
Some people feel generally unwell.
The clear surface of the eye (your cornea) can look hazy.
This photo shows what the eye looks like in acute glaucoma:
Acute angle closure glaucoma of the right eye
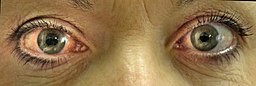
© James Heilman, MD, CC BY-SA 3.0, via Wikimedia Commons
Symptoms may begin in a situation of dim lighting, sudden excitement, after taking certain medicines or after a general anaesthetic.
The symptoms usually continue to worsen unless treated and help should be sought immediately. Either an optician or an eye specialist (ophthalmologist) can make the diagnosis. A family doctor will able to recognise the symptoms and will know to send the person directly to hospital.
Some people have milder symptoms, sometimes with intermittent attacks of blurring and haloes without pain. The attack may end when they go into a brighter room. Both of these cause the pupil to constrict and pull the iris away from the drainage channels.
This is called intermittent acute glaucoma. The attack of acute glaucoma can last for a few hours and then symptoms can improve again. However, attacks will usually happen again and, with each attack, vision may be damaged further. With these symptoms an optician or ophthalmologist should be seen urgently, in case treatment is needed to prevent a more severe attack.
How is acute glaucoma diagnosed?
Back to contentsThe diagnosis is made from the symptoms and the appearance of your eye. A likely diagnosis may be made by a GP, by an emergency doctor or by an optician. The diagnosis is confirmed by an examination done by an eye specialist (an ophthalmologist).
This usually involves examining the eye using a special light and magnifier called a slit lamp and measuring the pressure in the eye. A specialist can also use a gonioscope to directly examine the outflow channels around the trabecular meshwork area of the eye.
Acute glaucoma treatment
Back to contentsInitial treatment
Quick treatment is needed for acute glaucoma. It is considered a medical emergency. An eye specialist should be seen as soon as possible, usually via an Emergency Department in hospital. If it will take time getting to the ophthalmologist, some treatment can sometimes be started in the Emergency Department.
It is important not to cover the affected eye with a patch or a blindfold which would cause the pupil to dilate further and worsen the situation. It is also important not to lie down in a darkened room - lying down can tend to raise the pressure in the eye still further. A darkened room will further dilate the pupil, making things worse.
Medication
The first treatment is medication to lower the pressure within the eye. There are various types of medicine and eye drops that may be used in different combinations. Treatments may include:
Eye drops containing beta-blocker medication (to reduce fluid production in the eye) - for example, timolol.
An injection of a medicine called acetazolamide.
Pilocarpine eye drops which can cause the pupil to become smaller (constrict) and help to move the iris away from the trabecular meshwork. This helps to open up the obstruction to the flow of aqueous humour fluid.
Other types of eye drops are also used, including steroid eye drops which reduce inflammation.
Other fluid-reducing medication such as mannitol which is given into a vein (intravenously).
Painkillers and antisickness medication can be used if needed.
Further treatment
When the acute pressure in the eye has reduced, further treatment is needed to prevent acute glaucoma from coming back. This involves using laser treatment or surgery to make a small hole in the iris. The hole allows fluid to flow freely around the iris and can stop the iris bulging forwards and blocking the trabecular meshwork in the future.
Laser treatment is called peripheral iridotomy. This is the usual treatment. Usually two small holes are made in the iris, using a laser. The holes are almost unnoticeable to other people. Laser treatment is done using local anaesthetic in an outpatient clinic.
Surgical treatment called surgical iridectomy is another option. A small, triangular hole is made in the iris. The hole is visible afterwards as a very small, black triangle at the edge of the iris.
Usually, laser or surgical treatment will be advised for the other eye, often at the same time. This is to prevent acute glaucoma in the other eye (as the second eye is more prone to acute glaucoma as well). Sometimes eye drops are needed longer-term to help keep eye pressure under control.
What is the outlook for acute glaucoma?
Back to contentsThe outlook (prognosis) is good if treatment is started quickly. The eye can recover and laser treatment or surgery can prevent the problem coming back. If the attack is severe, or if treatment is delayed, the high pressure in the eye can damage the optic nerve and blood vessels. If this is the case, there is a risk that vision will be permanently reduced in the affected eye.
Driving and glaucoma
Back to contentsMost people will be allowed to drive after recovering from acute angle-closure glaucoma. Even if vision is reduced in one eye, driving may be permitted if the vision is good enough in the other eye.
However, advice will be needed from an eye specialist. A driver in the UK with glaucoma causing loss of vision in both eyes must inform the Driver and Vehicle Licensing Authority (DVLA) by law.
The DVLA will usually contact the eye specialist (ophthalmologist) and ask them for a report about the eye problems. They may also arrange an eyesight examination with an optician.
Can acute glaucoma be prevented?
Back to contentsAs mentioned above, some people have an increased risk of developing acute glaucoma because they have a shallow anterior chamber or narrow angle for drainage. Sometimes this is noticed at a routine eye examination.
If this has been seen then it is advised to be careful with certain medicines and eye drops (see above). Someone at very high risk of acute glaucoma, you may be advised to have preventative treatment such as laser iridotomy (see above).
When to see a doctor
Acute glaucoma is a medical emergency. Be aware of the symptoms of acute glaucoma. You should seek medical advice immediately if you develop a red eye with any of the following:
Pain.
Being sick (vomiting).
Reduced vision.
If you take a new medication or have eye drops to enlarge (dilate) your pupil and then you develop symptoms of acute glaucoma, seek medical advice straightaway. Tell your doctor about the medication and symptoms. This makes it easier for the problem to be recognised early.
Structure (anatomy) of your eye
Back to contentsYou can learn more about how the eye works and the structure of the eye in the separate leaflet called Anatomy of the eye. Glaucoma is mainly to do with the fluid in the eye, called aqueous humour, not being able to drain away properly.
Frequently asked questions
Back to contentsCan acute glaucoma be cured?
Acute glaucoma cannot be cured, but prompt treatment can relieve pressure and prevent permanent damage to your vision. Ongoing monitoring and medication may be needed to protect your eyesight.
What is the difference between glaucoma and acute glaucoma?
Glaucoma is a group of eye conditions that damage the optic nerve, often caused by an increase in eye pressure. Acute glaucoma, or acute angle-closure glaucoma, is a sudden and severe form that causes rapid pressure buildup and needs urgent medical attention to prevent vision loss.
What is the life expectancy of a glaucoma patient?
Acute glaucoma does not usually affect life expectancy, but it can cause permanent vision loss if not treated quickly. With prompt care and regular eye checks, most people can manage the condition and maintain good quality of life.
Dr Mary Lowth is an author or the original author of this leaflet.
Patient picks for Eye conditions

Eye health
Vitreous haemorrhage
Vitreous haemorrhage is bleeding into the jelly-like filling of the back part of your eye. This substance is the vitreous humour. It helps the eye keep its shape and is normally clear, allowing light from outside the eye to pass through it to reach the retina. Vitreous haemorrhage varies in degree from mild, with 'floaters' and haziness in the vision, to complete loss of vision. It is painless and it comes on quite quickly. Usually only one eye is affected. Whilst it is very alarming, once the bleeding has been treated, many cases resolve and vision is restored to where it was before.
by Dr Colin Tidy, MRCGP

Eye health
Colour vision deficiency
Colour vision deficiency, also called colour blindness, is when you are unable to see certain colours. The most common form of the condition is red-green colour vision deficiency.
by Dr Hayley Willacy, FRCGP
Further reading and references
- Assessing fitness to drive: guide for medical professionals; Driver and Vehicle Licensing Agency
- Khazaeni B, Khazaeni L; Acute Closed Angle Glaucoma. StatPearls, January 2025.
- Glaucoma; NICE CKS, February 2023 (UK access only)
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
8 Jun 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.