Presbyopia
Age-related long sight
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 15 Jan 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Hypermetropia
Age-related long-sight (presbyopia) is a normal part of ageing and is not a disease. As you get older, you find it more difficult to see (focus on) near objects. The problem can be corrected by wearing reading glasses or contact lenses. Presbyopia is a type of sight problem called a refractive error.
At a glance
Presbyopia is a type of long-sight caused by ageing, usually noticed around age 40.
It makes it harder for the eye's lens to change shape to focus on close objects.
Symptoms include difficulty reading small print, blurred close vision, headaches, and eye strain.
Presbyopia can be managed with reading glasses, contact lenses, or various surgical options.
Regular eye tests are recommended every two years, or more often for those at higher risk.
In this article:
Video picks for Eye conditions
Continue reading below
What is presbyopia?
Presbyopia is a long-sight (hypermetropia) eye condition, caused by age.
As part of the ageing process the lens becomes more stiff and less elastic. This makes it more difficult for the lens to change shape - the ciliary muscles have to work harder to make it do so.
Eventually they are unable to do this at all and the lens cannot be thickened. With the lens in its normal resting position you are still able to focus on objects in the distance. However, because the lens cannot thicken, it cannot manage the extra degree of focus (accommodation) which is needed for near objects.
In order to see close-up objects, our eyes have to accommodate. This means that the lens has to change its thickness. Its thickness is adjusted by the ciliary muscles that attach to the suspensory ligaments at either end.
As these muscles tighten, the ligaments lengthen and the lens becomes more thickened and curved. Light rays entering your eye from close objects are brought into sharp focus on the retina.
At what age does presbyopia start?
Back to contentsPresbyopia is a normal part of the ageing process and usually becomes noticeable at around age 40.
By the age of 45 years, most people will need reading glasses. If you already wear glasses or contact lenses, your prescription may alter as a result of age-related long sight.
Continue reading below
Types of presbyopia
Back to contentsThere are five types of presbyopia:
Incipient presbyopia. This is the very earliest stage, when it may be a bit more difficult to read small print.
Functional presbyopia. This occurs when you begin to notice more problems with near sight.
Absolute presbyopia. If you have this type, your eyes cannot focus on near objects at all (farsightedness).
Premature presbyopia. This term is used when presbyopia occurs before the age of 40 years.
Nocturnal presbyopia. When this occurs, focusing on near objects is particularly difficult in low light conditions.
Presbyopia symptoms
Back to contentsPresbyopia symptoms may start with difficulties with prolonged close-up work, with tiring (eye strain) of the eyes. This may be worse in dim light.
People with presbyopia may also notice:
Difficulty in adjusting vision if you look quickly from a near object to a faraway one.
Blurred vision when looking at objects close up such as reading material.
Headaches.
Eye strain when focusing on close work.
Continue reading below
What causes presbyopia?
Back to contentsPresbyopia is a refractive error (see below) caused by normal ageing.
People who have a job that requires a lot of close-up work and people who live and work in a hot climate with lots of ultraviolet sunlight exposure are also at higher risk of premature age-related long sight.
What is a refractive error?
Back to contentsTo understand what causes presbyopia, we need to understand what a refractive error is. . Refractive errors are an eyesight problem and a common reason for reduced level of eyesight (visual acuity).
Eye cross-section
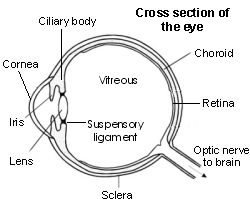
Refraction refers to the bending of light, in this case by the eye, in order to focus it. A refractive error means that the eye cannot focus light on to the retina properly. This usually occurs either due to abnormalities in the shape of the eyeball, or because age has affected the workings of the focusing parts of the eye.
There are four types of refractive error:
Age-related long sight (presbyopia).
Astigmatism (a refractive error due to an unevenly curved cornea).
In order to understand refractive errors fully, it is useful to know how we see.
When we look at an object, light rays from the object pass through the eye to reach the retina. This causes nerve messages to be sent from the cells of the retina down the optic nerve to the vision centres in the brain. The brain processes the information it receives, so that in turn, we can see.
Focusing the eye
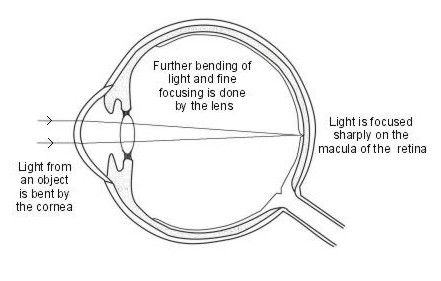
Light rays come off an object in all directions, as they result from the light around us from sun, moon and artificial light bouncing back off the object. The part of this bounced light that come into the eye from an object needs to be focused on a small area of the retina. If this doesn't happen, what we look at will be blurred.
The cornea and lens have the job of focusing light. The cornea does most of the work, as it (refracts) the light rays which then go through the lens, which finely adjusts the focusing. The lens does this by changing its thickness. This is called accommodation. The lens is elastic and can become flatter or more rounded. The more rounded (convex) the lens, the more the light rays can be bent inwards.
The shape of the lens is varied by the small muscles in the ciliary body. Tiny string-like structures called the suspensory ligaments are attached at one end to the lens and at the other to the ciliary body. This is a bit like a trampoline with the central bouncy bit being the lens, the suspensory ligaments being the springs and the ciliary muscles being the rim around the edge.
When the ciliary muscles in the ciliary body tighten, the suspensory ligaments slacken, causing the lens to become fatter. This happens for near objects. For looking at far objects, the ciliary muscle relaxes, making the suspensory ligaments tighten, and the lens thins out.
More bending (refraction) of the light rays is needed to focus on nearby objects, such as when reading. Less bending of light is needed to focus on objects far away.
Presbyopia treatment
Back to contentsGlasses
Presbyopia can be corrected by wearing reading glasses; often the lenses are similar to bifocal lenses. If you already have glasses, bifocal or varifocal lenses may be prescribed to treat your age-related long sight. With these lenses, different parts of the lens have different prescriptions.
Bifocal ('bi' means two) lenses have a lens at the bottom for long sight (to allow close-up vision) and the rest of the lens above (allowing distant vision). Multifocal lenses have at least three focus 'zones' - for distant, middle and near vision, with gradual changes between them. Middle vision is best imagined as that needed for computer screen work.
Contact lenses
For people who already have contact lenses, reading glasses may be prescribed in addition to these to treat presbyopia.
Other options include bifocal or multifocal contact lenses, or wearing a different contact lens in each eye - one to allow near vision, the other for distance vision (monovision contact lenses).
The disadvantage of correcting one eye (effectively to make it slightly short-sighted) is some loss of distance vision in that eye - but the other eye retains good distance vision. Usually the two eyes adapt to the differences between them, so that the patient can see near and far equally well.
Distance vision can be slightly compromised - and some patients notice 'ghosting' (faint double vision) on distant objects which does not always resolve with time.
Surgery
Various surgical options are now offered to correct presbyopia. Some of these work on the principle of correcting one eye for near vision, whilst correcting the other eye to give good distant vision:
Kamra® corneal inlay
The Kamra® corneal inlay was approved by the US FDA in 2015. The inlay is designed to eliminate the need for reading glasses among people between the ages of 45 and 60 years who have good distance vision without glasses but have problems seeing up close due to age-related long sight.
The inlay is a small, thin opaque device with a tiny opening in the centre. It is surgically implanted in the central cornea, directly in front of the pupil of the eye. The central opening in the inlay creates a 'pinhole camera' effect. This effect, also seen if you look through a pinhole in a piece of paper, sharpens near vision while maintaining clear distance vision.
The inlay typically is implanted in the non-dominant eye. This allows both eyes to be used for distance vision, while the inlay sharpens near vision in the non-dominant eye.
Laser eye surgery
Monovision LASIK® (Laser-Assisted In situ Keratomileusis) and PRK® (Photo-Refractive Keratectomy) can be used to remove corneal tissue and reshape the cornea to reduce the need for reading glasses. In monovision laser surgery for presbyopia, this is done for one eye only.
The surgeon fully corrects the distance vision of one eye (usually the dominant eye), and intentionally makes the non-dominant eye mildly short-sighted.
The newly short-sighted eye sees near objects clearly without glasses, although its distant vision may be less good. So, after monovision laser surgery, the dominant eye takes the lead to provide clear distance vision and the non-dominant eye is responsible for sharpening near vision.
See the leaflet on Laser Eye Surgery for further information.
Monovision conductive keratoplasty (CK)
CK uses low-level, radiofrequency energy to shrink fibres in the edge of the cornea to increase the curve and therefore increase its focusing power. Like monovision laser eye surgery, one eye is corrected for close vision and the other left for distance vision.
Monovision of any kind involves some compromise and not everyone adapts well to it. It's a good idea to try monovision with contact lenses before committing to a permanent surgical procedure, in case you don't adapt to it.
Refractive lens exchange (RLE)
RLE is the removal and replacement of the eye's natural lens with an artificial lens to improve vision. The procedure is very similar to cataract surgery. The artificial lens is usually a multifocal lens, but various types are available.
RLE can reduce the need for reading glasses while providing clear distance vision without glasses. It is particularly helpful for patients with age-related long sight who are developing cataracts.
Several other surgical procedures to correct presbyopia are either available or in development, depending on which country you live in. In the UK, these procedures are not routinely done in the NHS.
It is important that you know your facts, including what the procedure involves, the failure rate, side-effects, the risk of complications, and the level of aftercare provided.
You should be given the opportunity to discuss these facts in advance with the surgeon who will be carrying out the procedure.
How often should you have an eye test?
Back to contentsThe NHS recommends that most people should get their eyesight tested every two years. Children will routinely be offered eye checks at various stages from birth to school age.
People at high risk of sight problems need more frequent eyesight checks.
This includes people with:
A family history of these conditions.
People over the age of 70 years and children who wear glasses may also need more frequent eye tests.
You should get your eyes checked if you notice any changes in your vision.
Dr Mary Lowth is an author or the original author of this leaflet.
Patient picks for Eye conditions

Eye health
Visual problems
Most people are concerned when they develop problems affecting their eyes, particularly if this affects their ability to see clearly. This leaflet describes most eye conditions which can affect vision, either temporarily or permanently. It explains what symptoms might be expected and what can be done about them.
by Dr Philippa Vincent, MRCGP

Eye health
Eye floaters, flashes and haloes
Eye floaters and flashes are common and are usually nothing to worry about. They usually occur because of normal changes that happen in the jelly-like substance inside the eye (vitreous humour) as you age. Haloes are bright circles around a source of light. They are also referred to as glare. They are a common symptom, particularly in older people. They can sometimes be a sign of underlying eye conditions such as glaucoma.
by Dr Philippa Vincent, MRCGP
Frequently asked questions
If I already have short-sight, how might presbyopia affect my vision?
If you are already short-sighted, your existing glasses or contact lens prescription may need to change as a result of age-related long sight (presbyopia). It's also possible that you may find a period where your short-sightedness and presbyopia cancel each other out, allowing you to see things up close without glasses. However, once presbyopia progresses, you will likely need reading glasses or multifocal lenses.
Can presbyopia cause problems when switching focus between different distances?
Yes, a common symptom of presbyopia is difficulty in adjusting your vision quickly when you look from a near object to a faraway one. This indicates your eyes are struggling to accommodate the changing focus requirements.
Are there specific jobs or environmental factors that increase the risk of developing presbyopia earlier?
People who have jobs requiring extensive close-up work, or those who live and work in hot climates with significant ultraviolet sunlight exposure, are at a higher risk of developing premature age-related long sight (presbyopia).
What is the 'pinhole camera' effect mentioned with the Kamra corneal inlay?
The Kamra corneal inlay has a tiny central opening. This opening creates a 'pinhole camera' effect, which sharpens near vision while maintaining clear distance vision. This effect can also be observed if you look through a pinhole in a piece of paper.
How long does it take to adapt to monovision correction for presbyopia?
With monovision correction, where one eye is adjusted for near vision and the other for distance, the two eyes usually adapt to the differences between them. This allows the patient to eventually see near and far equally well. However, some people may experience 'ghosting' or faint double vision on distant objects, which doesn't always resolve with time, and not everyone adapts well to this method.
If I'm considering surgical options for presbyopia, what should I discuss with my surgeon beforehand?
Before undergoing a surgical procedure for presbyopia, it's important to discuss several factors with your surgeon. These include what the procedure involves, its failure rate, potential side-effects, the risk of complications, and the level of aftercare provided. You should be given the opportunity to understand all these facts in advance.
Why is regular eye testing important for people with conditions like diabetes or glaucoma?
People with certain conditions like diabetes, raised pressure in the eye (glaucoma), macular degeneration, or a family history of these conditions, are at a higher risk of sight problems. Therefore, they require more frequent eyesight checks than the recommended standard two-year interval for most people.
Further reading and references
- Laser correction of refractive error following non-refractive ophthalmic surgery; NICE Interventional procedures guidance, March 2011
- Corneal inlay implantation for correction of Presbyopia; NICE Interventional Procedure Guidance, April 2013
- Torricelli AA, Junior JB, Santhiago MR, et al; Surgical management of presbyopia. Clin Ophthalmol. 2012;6:1459-66. doi: 10.2147/OPTH.S35533. Epub 2012 Sep 6.
- Professional Standards for Refractive Surgery; Royal College of Ophthalmologists (Dec 2021)
- Katz JA, Karpecki PM, Dorca A, et al; Presbyopia - A Review of Current Treatment Options and Emerging Therapies. Clin Ophthalmol. 2021 May 24;15:2167-2178. doi: 10.2147/OPTH.S259011. eCollection 2021.
- Wolffsohn JS, Davies LN, Sheppard AL; New insights in presbyopia: impact of correction strategies. BMJ Open Ophthalmol. 2023 Jan;8(1):e001122. doi: 10.1136/bmjophth-2022-001122.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 11 Jan 2029
15 Jan 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.