Henoch-Schönlein purpura
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 31 Oct 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
Henoch-Schönlein purpura (HSP) is a rare condition that is caused by inflammation of blood vessels (vasculitis). It particularly affects children. Blood vessels throughout the body are affected but HSP most often causes a skin rash, tummy (abdominal) pain and joint pains.
In this article:
Continue reading below
What is HSP?
Henoch-Schönlein purpura (HSP) is an immune-mediated condition. This means that it develops because of an abnormal reaction of the body's defence (immune) system. It is not clear exactly what causes this reaction but it is thought that something acts as a trigger for HSP. For example, the trigger may be a particular infection or certain medicines, such as certain antibiotics.
What causes HSP?
The trigger (called an antigen) for Henoch-Schönlein purpura stimulates the immune system to produce a chemical to fight against it (antibody) and attack it. This causes immune complexes to form which are then deposited in the small blood vessels under the skin. The immune complexes cause inflammation of the blood vessels.
Inflammation of the blood vessels is known as systemic vasculitis. It is this inflammation that causes the small, round, red spots (petechiae) and the areas of reddish-purple skin discolouration (purpura). The immune complexes can also be deposited in other tissues of the body (for example, the kidneys), causing inflammation there as well.
The most common infection that has been found to be the trigger for HSP is an infection with a group of germs (bacteria) called Group A streptococcus. This group of bacteria is a common cause of infection of the upper respiratory tract - the throat and the upper airways. So, often, particularly in children, someone who develops HSP will have had a recent upper respiratory tract infection (within the previous few weeks).
Other bacterial and viral infections may also be triggers in some people. For example, parvovirus B19, Haemophilus parainfluenzae, Coxsackievirus and adenovirus.
Continue reading below
What are the symptoms of HSP?
Henoch-Schönlein purpura
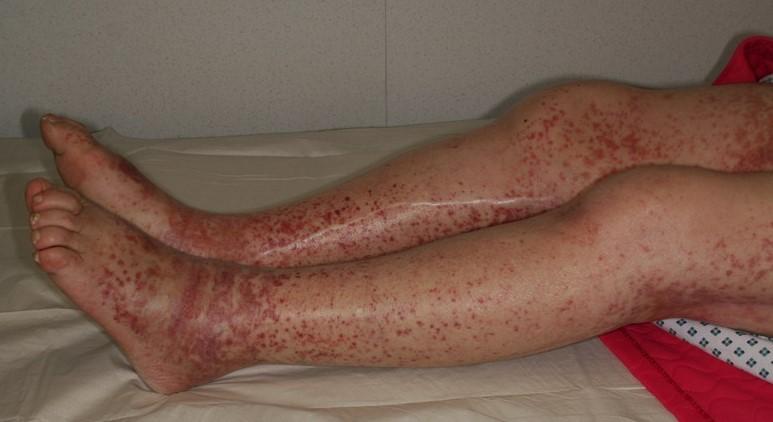
By Mnokel at Arabic Wikipedia, Public domain, via Wikimedia Commons
Flu-like symptoms
Someone with Henoch-Schönlein purpura (HSP) will often have had an upper respiratory tract infection within the few weeks before they develop the condition. So, for example, they may have had a cough, runny nose, and high temperature (fever) and have been feeling tired.
Rash
Everyone with HSP will develop a rash. This will have small, round, red spots (petechiae) and areas of reddish-purple skin discolouration (purpura).
The rash is most often seen on the legs, buttocks, and elbows and around the waistline. It affects both sides of the body. It can start off being very red in colour but then usually changes to purple and then a rusty colour over time. The rash is raised (like a bump on the skin) so you can feel it. The rash usually takes about 10 days to fade. A typical purpuric rash on an adult can be seen in the picture above.
Joint pains
About three in four people with HSP develop inflammation of their joints. Joints, particularly the knees and ankles, can become swollen, tender, warm and painful. The inflammation will gradually clear over time and there is not any lasting damage to the joints. The joint pains tend to come on after the rash has appeared in most people. However, in some people they can develop before the rash.
Tummy pain
Most but not all people with HSP develop pain in their tummy (abdomen). The pain can be very bad in some people and usually changes in severity, or comes on in waves. Tummy pain tends to come on about a week after the rash has developed in most cases of Henoch-Schönlein purpura. Some people may also experience being sick (vomiting) and having diarrhoea.
How do you test for HSP?
Henoch-Schönlein purpura (HSP) is usually suspected because of the typical symptoms. However, a number of investigations may be suggested to help doctors confirm the diagnosis and to see which body parts may be affected by the inflammation. Investigations may include the following:
Blood tests
To look at how the kidneys are working.
To look for any signs of recent Group A streptococcal infection.
To confirm that platelet levels are not low. (Platelets are a type of blood cell. In some conditions, a rash similar to that in HSP develops because platelet levels have become too low for some reason.)
To look at immunoglobulin A levels which are usually high in HSP.
Skin biopsy
If the diagnosis is uncertain, a biopsy of the skin may be suggested. A very small sample of skin affected by the rash is taken and examined underneath the microscope. There is a typical appearance under the microscope in HSP.
Urine dipstick test
This is a special testing strip can be dipped into a sample of urine to look for signs of any kidney involvement. For example, signs of traces of protein and/or blood in the urine which may not be seen by the naked eye.
A blood pressure check
Blood pressure can be raised if HSP involves the kidneys.
Kidney biopsy
If signs of more severe kidney problems develop (for example, blood tests to look at how the kidneys are working show that they are struggling), a procedure in which a sample of the kidneys is taken (a biopsy) may be suggested. This can give more information about the kidney inflammation and how severe it may be.
See the separate leaflet called Kidney biopsy (Renal biopsy) for more details.
Stool test
To look for any signs of blood in the stools (faeces). If there is bleeding within the gut (gastrointestinal bleeding), this can lead to blood in the stools, which sometimes cannot be seen by the naked eye. A test on a small sample of stool can pick up microscopic traces of blood.
Other tests
If other complications develop, certain other tests may be suggested. For example, if pain in the scrotum develops, an ultrasound scan of the scrotum may be suggested.
Continue reading below
How to manage HSP
Depending on the symptoms that develop, someone with Henoch-Schönlein purpura (HSP) may be admitted to hospital for monitoring. For most people, HSP will get better on its own and so no specific treatment is needed. However, there are a number of things that can help with the symptoms. For example:
Painkillers
These may help with joint pains. Paracetamol is an example. Non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen may also be helpful. However, NSAIDs should be avoided in anyone who has suspected kidney complications or any bleeding within the gut. See the separate leaflet called Anti-inflammatory painkillers for more details.
Rest
Resting with the legs raised may help reduce the degree of rash that develops. This is because the small, round, red spots (petechiae) and areas of reddish-purple skin discolouration (purpura) tend to develop in dependent areas of the body such as the legs.
Steroid medication
This may be suggested if there are signs that the kidneys are becoming affected. Sometimes steroids are also suggested if other symptoms are severe (such as joint pains or tummy (abdominal) pain), or if boys develop scrotal pain and swelling.
In addition to this, if something is thought to have triggered HSP (for example, a specific medication that was being taken), this should be stopped.
Alternative treatments
Other treatment will depend on whether complications develop. For example, if the kidneys become involved, referral to a kidney specialist for assessment and their advice about treatment may be advised. A kidney sample (biopsy) may be suggested to help give the specialist more information and guide them as to the best treatment. Treatment may include steroids and other medicines to help suppress the body's defence (immune) system. Sometimes medication to lower blood pressure is needed if high blood pressure develops because of kidney involvement.
Plasma exchange
Occasionally a process called plasma exchange is needed if the complications caused by HSP are very serious.
Your blood is made up of blood cells and plasma. Plasma is where the damaging antibodies are present. Plasma exchange involves taking your blood out of your body and separating the blood into cells and plasma. The plasma is then removed and the blood cells are returned to the body with a plasma substitute.
A special machine is used for this treatment and only a small amount of blood is actually outside the body at any time. The sooner treatment is started after symptoms begin, the better the effect this treatment is likely to have.
Is Henoch-Schönlein purpura serious?
Henoch-Schönlein purpura (HSP) is not usually serious. But it's a really important condition because very occasionally it can cause serious complications, especially kidney damage.
In many people with Henoch-Schönlein purpura, no complications develop. But, complications sometimes develop. They can include the following:
Kidney involvement
In around half of people with Henoch-Schönlein purpura, the kidneys become affected. If immune complexes are deposited in the kidneys, this can lead to inflammation of the kidneys, known as nephritis. This complication usually develops within one month after the rash starts but can sometimes develop up to six months afterwards. In most people, kidney involvement will get better on its own. However, in some people, a more persistent and serious nephritis can develop.
Bleeding in the gut
About three in ten people with HSP develop this bleeding in the gut. If immune complexes are deposited in the blood vessels of the wall of the gut (intestine), this can cause bleeding within the gut (gastrointestinal bleeding). This can lead to symptoms such as passing blood in the stools (faeces). Rarely, bleeding in the gut can be severe and life-threatening.
Orchitis
About 3 in 10 boys with HSP develop orchitis. This is inflammation of the testicle (testis), causing pain, redness and swelling of the scrotum.
Other complications
There are also some other rare, but serious, complications. For example, inflammation can sometimes affect:
The brain and nervous system, leading to complications such as seizures).
The heart (leading to complications such as a heart attack).
The lungs (leading to complications such as a bleeding into the lungs).
What is the outlook for Henoch-Schönlein purpura?
The long-term outlook (prognosis) mainly depends on whether and how badly the kidneys have been affected:
If HSP does not affect the kidneys, most people make a full recovery within about four weeks and have no lasting problems.
Kidney damage is only serious in about 1 in every 10 people with HSP. The kidneys can become so badly affected that kidney failure can develop.
Does HSP go away?
HSP may come back within six months of first having HSP. It is more likely to come back if the kidneys have been affected.
How common is it?
Henoch-Schönlein purpura is not very common. Between 8 and 20 in 100,000 people will develop HSP each year. HSP mostly affects children with 9 out of 10 cases happening in children between the ages of 2-10 years. But HSP can also affect older children and adults. It is more common in boys than in girls.
Children with HSP under the age of 2 years tend to develop milder symptoms. Adults with HSP tend to develop more severe symptoms and are more likely to develop complications.
Further reading and references
- Henoch-Schönlein purpura; DermNet NZ
- Gohari A, Matsell DG, Mammen C, et al; Henoch-Schonlein purpura in children: Use of corticosteroids for prevention and treatment of renal disease. Can Fam Physician. 2020 Dec;66(12):895-897. doi: 10.46747/cfp.6612895.
- Leung AKC, Barankin B, Leong KF; Henoch-Schonlein Purpura in Children: An Updated Review. Curr Pediatr Rev. 2020;16(4):265-276. doi: 10.2174/1573396316666200508104708.
- Heineke MH, Ballering AV, Jamin A, et al; New insights in the pathogenesis of immunoglobulin A vasculitis (Henoch-Schonlein purpura). Autoimmun Rev. 2017 Dec;16(12):1246-1253. doi: 10.1016/j.autrev.2017.10.009. Epub 2017 Oct 14.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 30 Oct 2027
31 Oct 2022 | Latest version
25 Mar 2011 | Originally published
Authored by:
Dr Michelle Wright, MRCGP

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free