Oesophageal cancer
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 10 Feb 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Oesophageal cancer is cancer of the gullet (oesophagus). There are over 8,000 new cases diagnosed every year in the UK and two thirds of new diagnoses are in men.t is the 7th most common cause of cancer death in the UK and accounts for 5% of all cancer deaths. Most cases occur in people over the age of 55, although younger people are sometimes affected. Those diagnosed at an early stage have the best chance of a cure. The earliest symptom is often difficulty with swallowing (dysphagia).
In this article:
Video picks for Gastrointestinal cancers
In general, the more advanced the cancer (the more it has grown and spread), the less chance that treatment will be curative. Most cases of oesophageal cancer are diagnosed when the cancer is advanced. However, treatment can often slow the progress of the cancer or ease symptoms.
Continue reading below
What is the oesophagus?
Upper gut
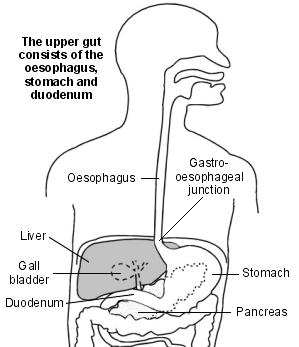
The oesophagus (gullet) is part of the gut (gastrointestinal tract). When we eat, food goes down the oesophagus into the stomach.
The upper section of the oesophagus lies behind the windpipe (trachea). The lower section lies between the heart and the spine.
There are layers of muscle in the wall of the oesophagus. These tighten (contract) to propel food down into the stomach.
There is a thickened circular band of muscle (a sphincter) at the junction between the oesophagus and stomach. This relaxes to allow food down, but normally tightens up and stops food and acid leaking back up (refluxing) into the oesophagus. In effect, the sphincter acts like a valve.
What is oesophageal cancer?
Back to contentsOesophageal cancer is cancer of the gullet (oesophagus). There are two main types:
Adenocarcinoma of the oesophagus
This occurs in about 6 out of 10 cases in the UK. This type arises from cells within mucous glands. (The lining of the oesophagus contains many tiny glands which make mucus. The mucus helps food to slide down into the stomach easily.) This type mainly occurs in the lower third of the oesophagus.
Squamous cell carcinoma of the oesophagus
This occurs in about 4 out of 10 cases in the UK. This type arises from the cells lining the oesophagus. This type mainly occurs in the upper two thirds of the oesophagus.
The symptoms, treatment and outlook are similar for both of these types. (There are some rare types of cancer which arise from other cells in the oesophagus. These are not dealt with further in this leaflet.)
See the separate leaflet called Cancer for more general information about cancer.
Continue reading below
What causes oesophageal cancer?
Back to contentsA cancerous tumour starts from one abnormal cell. The exact cause of cancerous cells is unclear. It is thought that something damages or alters certain genes in the cell. This makes the cell abnormal and multiply out of control. See the separate leaflet called Cancer for more details.
Many people develop cancer of the gullet (oesophagus) for no apparent reason. However, certain risk factors increase the chance that oesophageal cancer may develop. These include:
Ageing. It is more common in older people. Most cases are in people over the age of 55.
Being male. It is more common in men.
Diet.A high-fat diet is thought to increase the risk and eating a lot of fruit and green vegetables is thought to reduce the risk.
Obesity. Being obese can increase the risk.
Where you live. Oesophageal cancer is much more common in China and certain other Far Eastern countries than in Europe.
Smoking.
Heavy drinking - especially spirits.
Long-standing acid reflux from the stomach (gastro-oesophageal reflux disease (GORD)). This condition is common and causes inflammation at the lower end of the oesophagus. See the separate leaflet called Acid Reflux and Oesophagitis for more details. However, it has to be stressed that the risk is small - most people with acid reflux do not develop cancer.
Barrett's oesophagus. This is a condition at the lower end of the oesophagus where the cells which line the oesophagus have become changed.About 1 in 100 people with Barrett's oesophagus develop adenocarcinoma of the oesophagus at some stage - for this reason, most people with Barrett's oesophagus will have regular screening tests for oesophageal cancer.
Other uncommon conditions are associated with an increased risk and include:
Achalasia - a condition which causes a widening at the bottom of the oesophagus.
Tylosis - a very rare inherited skin condition.
Paterson-Brown-Kelly syndrome - a rare syndrome which includes iron deficiency and changes in the mouth or oesophagus.
Long-term exposure to certain chemicals and pollutants (chemical carcinogens).
Oesophageal cancer is not inherited so does not run in families. However, a family history of hiatal hernia appears to be a risk factor in developing oesophageal adenocarcinoma.
Oesophageal cancer symptoms
Back to contentsWhen a cancer of the gullet (oesophagus) first develops and is small it usually causes no symptoms. Some do not cause symptoms until they are quite advanced. As the cancer grows the symptoms of oesophageal cancer which may develop usually include one or more of the following:
Difficulty with swallowing (dysphagia). This is often the first symptom and is caused by a tumour narrowing the passage in the oesophagus. Food may appear to stick as you try to swallow. If it gets worse then drinks may also be difficult to swallow.
Being sick (vomiting) after eating (which is really regurgitating food which has become stuck).
Pain in the chest or in the back of the chest when you swallow (odynophagia).
Losing weight.
Vomiting blood.
Coughing. Particularly when you swallow.
A hoarse voice.
Acid reflux symptoms may first develop, or get worse, when you develop a cancer at the lower oesophagus next to the stomach. Symptoms include pains in the chest (heartburn). Note: acid reflux is common and most people with acid reflux do not have cancer.
If the cancer spreads to other parts of the body, various other symptoms can develop.
All the above symptoms can be due to other conditions, so tests are needed to confirm oesophageal cancer.
Continue reading below
How is oesophageal cancer diagnosed and assessed?
Back to contentsInitial assessment, barium swallow and gastroscopy (endoscopy)
If a doctor suspects that you may have cancer of the gullet (oesophagus), he or she will examine you to look for signs such as a lump in your tummy (abdomen). The examination is often normal, especially if the cancer is at an early stage. Therefore, a gastroscopy is usually arranged. In some cases a test called a barium swallow may be done before the gastroscopy - in this test you are X-rayed while swallowing liquid which shows up on X-ray in order to spot any masses in the oesophagus. Barium swallows are not very commonly used these days.
A gastroscope (endoscope) is a thin, flexible tube. It is passed through the mouth, into the oesophagus and down towards the stomach. The endoscope contains fibre-optic channels which allow light to shine down so the doctor or nurse can see inside. See the separate leaflet called Gastroscopy (Endoscopy) for more details.
Biopsy - to confirm the diagnosis
When a small sample of tissue is removed from a part of the body, the procedure is called a biopsy. The sample is then examined under the microscope to look for abnormal cells. When you have a gastroscopy, if anything abnormal is seen, the doctor or nurse can take a biopsy. This is done by passing a thin grabbing instrument down a side channel of the gastroscope. It can take two weeks for the result of a biopsy.
Assessing the extent and spread
If you are confirmed to have oesophageal cancer, further tests may be done to provide a more detailed picture. For example, a special ultrasound scan, which uses a probe at the end of a gastroscope (an endoscopic ultrasound), can assess how far the cancer has grown through the wall of the oesophagus.
Other tests may be arranged to see if the cancer has spread to other parts of the body. For example, a computerised tomography (CT) scan, an ultrasound scan of the abdomen, a positron emission tomography (PET) scan or other tests.
This assessment is called staging of the cancer. The aim of staging is to find out:
How much the tumour in the oesophagus has grown and whether it has grown partially or fully through the wall of the oesophagus.
Whether the cancer has spread to local lymph nodes.
Whether the cancer has spread to other areas of the body (metastasised).
By finding out the stage of the cancer it helps doctors to advise on the best treatment options. It also gives a reasonable indication of outlook (prognosis).
See the separate leaflet called Stages of Cancer for more details.
Treatment for oesophageal cancer
Back to contentsTreatment options which may be considered include surgery, chemotherapy and radiotherapy. The treatment advised for each case depends on various factors, such as:
The exact site of the primary tumour in the gullet (oesophagus).
How large the cancer is and whether it has spread (the stage of the cancer).
Your general health.
You should have a full discussion with a specialist who knows your case. They will be able to give the pros and cons and the likely success rate for your type of cancer. They will also be able to outline possible side-effects and other details about the possible treatment options.
Oesophageal cancer surgery
It may be possible to remove the tumour. To do this, the operation is to remove part or all of the oesophagus, depending on the site and size of the tumour.
There are various ways a surgeon can get to the oesophagus and various types of operation. If the lower part of the oesophagus is removed, it may be possible to sew the stomach back on to the remaining section of oesophagus if the stomach is brought up into the chest area.
If all of the oesophagus is removed, the surgeon may use a section of your gut (intestine) to create a new artificial oesophagus. Some lymph glands around the oesophagus are also removed at the same time of the operation to see if any cancer has spread to them.
Even if the cancer is advanced and it is not possible to remove it, some surgical techniques may still have a place to ease symptoms. For example, a blockage may be eased by:
Using laser surgery.
Inserting a rigid tube (a stent).
Stretching of the oesophagus, which allows food and drink to pass through the blockage to the stomach.
Chemotherapy
Chemotherapy is a treatment of cancer by using anti-cancer medicines which kill cancer cells, or stop them from multiplying. See the separate leaflet called Chemotherapy for more details.
Chemotherapy may be used in addition to surgery or radiotherapy. For example, following surgery you may be given a course of chemotherapy. This aims to kill any cancer cells which may have spread away from the primary tumour.
When chemotherapy is used after surgery it is called adjuvant chemotherapy. In some cases, chemotherapy is given before surgery, to shrink a large tumour so that surgery is more likely to be successful. This is called neoadjuvant chemotherapy.
Radiotherapy
Radiotherapy is a treatment which uses high-energy beams of radiation which are focused on cancerous tissue. This kills cancer cells, or stops cancer cells from multiplying. See the separate leaflet called Radiotherapy for more details.
When radiotherapy is used to treat cancer of the oesophagus it is commonly used in addition to either surgery or chemotherapy. The exact combination of treatments advised depends on various factors.
Two types of radiotherapy are used for oesophageal cancer - external and internal:
External radiotherapy. In this procedure, radiation is targeted on the cancer from a machine. (This is the common type of radiotherapy which is used for many types of cancer.)
Internal radiotherapy (brachytherapy). This treatment involves placing a small radioactive implant next to the cancerous tumour for a short time. It is then removed. (It is put in position via the oesophagus, usually by a gastroscope (endoscope).
Photodynamic therapy
A newer treatment called photodynamic therapy (PDT) uses low-powered lasers combined with a light-sensitive medicine to destroy cancer cells. In the UK it is still only carried out in a few specialist hospitals. It is more commonly used as a treatment to relieve the difficulty in swallowing caused by cancer of the oesophagus. PDT is being used in trials for the treatment of early oesophageal cancer, instead of surgery.
Monoclonal antibodies
Nivolumab® is a type of targeted treatment called a monoclonal antibody. It is sometimes used after chemotherapy and/or radiotherapy and surgery to lengthen the time before any recurrence of the cancer, and increase survival rates.
What are the aims of oesophageal cancer treatment?
Back to contentsThere are three aims when it comes to cancer treatment. You should also discuss with your specialist the aims of treatment. These are:
The aim is to cure the cancer
Some cancers of the oesophagus can be cured, particularly if they are treated in the early stages of the disease. (Doctors tend to use the word remission rather than the word cured. Remission means there is no evidence of cancer following treatment. If you are in remission, you may be cured. However, in some cases a cancer returns months or years later. This is why doctors are sometimes reluctant to use the word cured.)
The aim is to control the cancer
If a cure is not realistic, with treatment it is often possible to limit the growth or spread of the cancer so that it progresses less rapidly. This may keep you free of symptoms for some time.
The aim is to ease symptoms
If a cure is not possible, treatments may be used to reduce the size of a cancer, which may ease symptoms such as pain or difficulty with swallowing. If a cancer is advanced, you may require treatments such as nutritional supplements, painkillers, or other techniques to help keep you free of pain or other symptoms.
Oesophageal cancer prognosis
Back to contentsWithout treatment, cancer of the gullet (oesophagus) is likely to get larger, and spread to other parts of the body. If it is diagnosed and treated at an early stage, there is a chance of a cure with treatment.
An 'early stage' would be before the cancer has grown through the wall of the oesophagus or spread to lymph nodes or other areas of the body. Unfortunately, most cases in the UK are not diagnosed at an early stage. This is because symptoms do not tend to develop until the cancer is already fairly large.
If the cancer is diagnosed when it has grown through the wall of the oesophagus, or spread to other parts of the body, a cure is less likely. However, treatment can often slow down the progression of the cancer. Currently, about a quarter of people diagnosed with oesophageal cancer are still alive five years after diagnosis.
Studies have suggested that a combination of the treatment esomeprazole - a type of medicine known as a proton pump inhibitor - and low-dose aspirin may help in preventing the development of oesophageal adenocarcinoma. Further evaluation of this finding is now ongoing.
The treatment of cancer is a developing area of medicine. New treatments continue to be developed and the information on outlook (prognosis) above is very general. The specialist who knows your case can give more accurate information about your particular outlook, and how well your type of cancer and stage of cancer are likely to respond to treatment.
Patient picks for Gastrointestinal cancers

Cancer
Stomach cancer
Although stomach (gastric) cancer is common worldwide, it is not so common in the UK. Most cases occur in people over the age of 55. If stomach cancer is diagnosed at an early stage, there is a good chance of a cure. In general, the more advanced the cancer (the more it has grown and spread), the less chance that treatment will be curative. However, treatment can often slow the progress of the cancer.
by Dr Doug McKechnie, MRCGP

Cancer
Pancreatic cancer
Pancreatic cancer (cancer of the pancreas) is largely a disease of older age - 47% of UK cases occur in those aged 75 or over and the most common age to be diagnosed is 85 - 89. If it is diagnosed at an early stage then an operation to remove the cancer gives some chance of a cure. In general, the more the cancer has grown and spread (the more advanced the cancer), the less chance that treatment will be curative. However, treatment can often slow the progress of the cancer.
by Dr Toni Hazell, MRCGP
Further reading and references
- Photo-dynamic therapy for early oesophageal cancer; NICE Interventional Procedure Guidance, December 2006
- Endoscopic submucosal dissection (ESD) of oesophageal dysplasia and neoplasia; NICE Interventional Procedure Guidance, September 2010
- Minimally invasive oesophagectomy for cancer or high-grade dysplasia of the oesophagus; NICE Interventional Procedure Guidance, September 2011
- Sohda M, Kuwano H; Current Status and Future Prospects for Esophageal Cancer Treatment. Ann Thorac Cardiovasc Surg. 2017 Feb 20;23(1):1-11. doi: 10.5761/atcs.ra.16-00162. Epub 2016 Dec 21.
- Nivolumab for adjuvant treatment of resected oesophageal or gastro-oesophageal junction cancer; NICE Technology appraisal guidance, November 2021
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 9 Feb 2028
10 Feb 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.