Cataracts
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 21 Jun 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Cataracts is when the lens of an eye becomes cloudy and affects vision. It commonly occurs in older people and develops gradually. If left untreated it can lead to total loss of vision (blindness).
In this article:
Video picks for Eye conditions
Key points
A cataract is when the lens inside your eye becomes cloudy, making your vision blurry and causing glare, faded colours, and trouble seeing in bright or dim light.
It usually affects older people and is a normal part of ageing. It is caused by the gradual breakdown of proteins in the eye's lens.
Cataracts can usually be treated with surgery, where the cloudy lens is removed and is replaced with an artificial plastic lens.
Continue reading below
What are cataracts?
Cataracts are cloudy (opaque) areas that develop in the lens of the eye. The lens should normally be clear. However, with cataracts, the affected lens becomes like frosted glass.
View of eye from the side
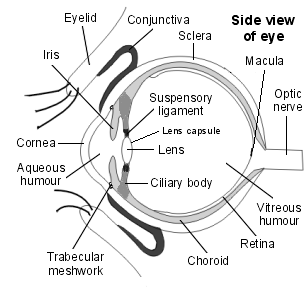
The lens of the eye sits just behind the pupil, which is the opening in the coloured part of the eye (iris). The lens is held in place by a ring of supporting tissues. Its job is to focus the image of what you see on to the back of your eye.
The lens is made of water and protein, and is normally clear because of the way the protein is arranged. With ageing and other causes of cataract, some of the protein can 'clump together' and this starts to cloud the lens.
Over time, this makes it harder to see. Things are made worse by a gradual tendency for the lens to discolour with age, acquiring a brownish tinge which can affect colour vision, and can also make reading less clear.
A cataract is a gradual change, which starts inside the lens. There are three different patterns of cataract formation:
A nuclear cataract forms deep in the central part of the lens. Nuclear cataracts are usually associated with ageing.
A subcapsular cataract forms at the back of the lens (this is also called a posterior subcapsular cataract). People with diabetes or those taking steroid medications by mouth have a greater risk of developing a subcapsular cataract.
A cortical cataract begins with white, wedge-like cloudy areas that start at the outer edges (periphery) of the lens, and gradually extend towards the centre in a spoke-like fashion.
Types of cataracts
Back to contentsSenile cataracts.
Congenital cataracts.
Continue reading below
How common are cataracts?
Back to contentsAge-related cataract (senile cataract)
This is by far the most common type, and it affects older people, becoming more common with increasing age. In the UK about 1 in 3 people over the age of 65 have at least one cataract. Men and women are equally affected. Often both eyes are affected but one eye is typically worse than the other.
Most age-related cataracts take many years to form, and at first there will be no symptoms. Many people with an early cataract do not realise they have it as there is very little cloudiness. For most, therefore, the cataract will be diagnosed at a routine eye check before symptoms ever develop.
For some people, the cataract never becomes bad enough to impair vision. However, in many cases, vision becomes gradually worse over the years.
Congenital cataracts (present at birth)
These are uncommon, but important to diagnose early, and must be removed as early as possible after birth. This is because vision and seeing have to be learnt very early in infancy. A cataract that is present at birth stops the eye from learning to see.
It can cause total loss of vision (severe sight impairment) which may then persist even if the cataract is removed later in life. Doctors examine the eyes of babies for cataracts as part of routine baby checks both at birth and at 6-8 weeks of age.
The rest of this leaflet is only about the common age-related cataract.
Cataract symptoms
Back to contentsSymptoms of cataracts include:
Blurred vision.
Spots in your vision.
Haloes around bright lights - for example, street lights.
Seeing less well in brightly lit rooms or in sunshine.
Becoming easily dazzled by bright lights such as the headlights of an oncoming car.
Washing out or fading of colours.
Over the years your vision may gradually become worse.
The visual impairment is not corrected by glasses.
Depending on the severity of the cataract, the effect on your sight can range from vision being slightly blurred to complete loss of vision in the affected eye.
Continue reading below
What causes cataracts?
Back to contentsThe cataract begins with a change to the structure of the proteins in the lens. Some of the proteins clump together in places within the lens. This causes tiny areas of cloudiness. Each tiny area of cloudiness blocks a bit of light getting through to the retina. The severity of the cataract depends on the number of areas of cloudiness that develop in the affected lens.
Most affected people develop a cataract for no apparent reason. Factors that may increase the risk of developing cataracts include:
Having a poor diet.
Steroid medicines.
Having a family history of cataracts.
Ultraviolet radiation from sunlight and other sources.
Statin medicines used to reduce cholesterol.
Previous eye injury or inflammation.
Previous eye surgery.
Significant alcohol consumption.
Use of hormone replacement therapy (HRT) for a prolonged period (more than ten years).
Severe short-sightedness (high myopia).
There are some uncommon causes of cataracts:
A cataract may develop after an injury to an eye, or as a result of radiation exposure.
Using steroid drops in the eye over a prolonged period increases the likelihood of developing a cataract.
Cataracts sometimes develop as a complication of some other eye conditions. For example, there is an increased risk of cataracts in people who have diabetes.
Some studies have raised the possibility that cataract formation might relate to diet, with the thought that eating less meat or increasing intake of antioxidant vitamins might be helpful.
Research continues in this area. However, it is not clear that taking vitamin supplements is of benefit to eye health in those whose diet is already good and well balanced.
What other conditions could cause similar symptoms to cataracts?
Back to contentsCataracts cause clouding of the lens and gradual loss of vision, which you may not notice at first, together with symptoms such as dazzling and haloes listed above.
There are several other common conditions which can affect your vision. Some of these have symptoms which overlap or can resemble those of cataracts. Two of the most important are macular degeneration and glaucoma.
Symptoms of macular degeneration
Macular degeneration is also mainly associated with getting older. It affects the central part of your vision.
The main early symptom is worsening of central vision despite using your usual glasses. You may notice that you need brighter light to read by. Words in a book or newspaper may become blurred. Colours may appear less bright and you may have difficulty recognising faces and facial expressions. As the condition worsens, you can start to develop a 'blind spot' in the middle of your visual field.
For more information, see the separate leaflet called Macular Degeneration.
Symptoms of glaucoma
Most people whose vision is affected by chronic glaucoma do not notice any symptoms at first. This is because the first part of the vision to be affected by glaucoma is the outer (peripheral) field of vision and when we look at the world most of us do so with two eyes.
Areas that one eye does not see, the other eye will cover for; so we continue to see a complete picture until both eyes are badly affected.
Untreated glaucoma is one of the world's leading causes of total loss of vision (severe sight impairment). This can be prevented if glaucoma is diagnosed and treated early enough.
Getting tested is simple and painless: every high-street opticians should be able to check you for glaucoma.
For more information, see the separate leaflet called Chronic Open-angle Glaucoma.
How is a cataract diagnosed?
Back to contentsA cataract can usually be seen easily by a doctor or optician (optometrist) when they perform an eye test. This may be done because you have noticed a problem with vision, or during a routine eye check.
Do I need treatment for cataracts?
Back to contentsAn early cataract may not cause any noticeable problem. The rate of decline in vision varies considerably from person to person.
Most people opt to have their cataract treated at an early stage when the cataract is just beginning to affect ability to function normally. For example, you might be offered surgery if you are having problems reading the paper, watching TV, driving, or cooking. Treatment is usually successful.
Cataract treatment
Back to contentsWhen symptoms begin to appear, you may be able to improve your vision for a while by using new glasses, magnification, appropriate lighting or other visual aids.
There are currently no medicines, eye drops or lasers that treat cataracts, although research in this area is going on. For now, surgery is the only way of treating cataracts. Around 300,000 cataract operations are performed each year in the UK.
The operation involves removing the cloudy lens and replacing it with an artificial plastic lens (an intraocular implant). It usually takes 10-20 minutes, and is often done as a day case.
The majority of people who have cataract surgery experience a marked improvement in their vision.
The decision on whether or not to have cataract surgery is a personal one which you should make after talking with your doctor or eye specialist. It will be affected by factors such as your general health and fitness, your wish to read or drive and the presence of any other eye problems which might mean that removing the cataract will not restore your vision.
Cataract surgery
Back to contentsThe operation is usually done under local anaesthetic, so you are awake during the operation. The operation should be painless, as local anaesthetic eye drops are used to numb your eye. (Occasionally, local anaesthetic injections are also used around the eye.) Normally one eye is operated on at a time.
The operation is performed, using a microscope, through a very small opening in the eye. When the eye is numb, the surgeon makes a tiny hole in the front of the eye at the edge of the cornea. Then, the surgeon removes the inside of the lens. He/she may first break up the lens with ultrasound to allow it to be extracted through a smaller incision (this technique is called phacoemulsification).
A clear plastic lens is placed within the lens capsule. Usually no stitches are needed. You may have to wear a pad over your eye after the operation.
The standard plastic lens can't change its focus - to look at near objects versus distant objects, for example. So, if you have a standard plastic lens inserted you will probably still need to wear glasses or contact lenses (assuming that you did before the operation).
It is sometimes possible to have an accommodating lens inserted which allows focusing on near as well as distant objects. Multifocal lenses which are even more versatile are now also available. Your surgeon will be able to discuss with you whether these are suitable for you, although these types of lens are not usually available on the NHS.
Complications of cataract surgery
Back to contentsIn the vast majority of cases, the operation is successful and vision improves immediately. In a small number of cases, complications occur. These may include
Damage to the lens capsule at the back of the eye with leakage of the jelly (the vitreous) inside the eye.
Bleeding into the eye.
Infection of the eye, which can be serious.
Inflammation of the eye.
Damage to the cornea or to other parts of the eye.
Detachment of the retina at the back of the eye.
Dysphotopsias (see below) These are visual symptoms that result from light reflecting off the replacement intraocular lens on to the retina. 'Positive' dysphotopsias are more common and involve symptoms of brightness such as glare, star bursts or haloes. 'Negative' dysphotopsias are shadows or dark areas. In most cases symptoms subside within several weeks of surgery as the brain adapts and screens out the symptoms, but in a small percentage of patients symptoms persist, in which case further surgery may be helpful.
These are all uncommon and can usually be treated. However, they are very occasionally serious enough to cause permanent visual problems.
Complications which can occur some time after surgery include:
Problems with glare.
Slippage (dislocation) of the plastic lens.
Increased pressure in the eye (glaucoma).
Squint (strabismus).
Posterior capsule cloudiness (opacification): the back part of the lens capsule, which is left in place, can become cloudy. This cloudiness can usually be easily treated with a laser, although a laser cannot be used to treat a cataract itself.
Recovering from cataract surgery
Back to contentsYou are usually able to go home the same day after your surgery. When you leave you will have some protection over the treated eye and this is usually a pad and a plastic shield. This can be removed the following day. You should wear the shield at night for at least a week.
The local anaesthetic will wear off after a few hours, so feeling will return. You can take simple painkillers if needed. You may feel grittiness in the eye and it may look red or bloodshot. The eye may water and you may have blurred or double vision. These are all normal at this stage. These effects may last a few days but it may take 4-6 weeks for them totally resolve. It may take a few days for the sight to return completely in your eye.
If you need new glasses you should not order them until the eye has healed - usually at 6 weeks.
You should take it easy for the first 2-3 days. When you return to work will depend on your job type and whether you need new glasses.
You can shower and wash your hair as normal, but use the eye shield when washing your hair. If you go outdoors wear the shield, your old glasses or sunglasses. Avoid swimming for 4-6 weeks.
Cataracts and driving
Back to contentsCataracts may affect your ability to drive, either:
By visual clouding (if severe); or
By causing pronounced glare which can dazzle you when driving at night.
It is your legal obligation to inform the DVLA about any medical condition which could affect your safety behind the wheel. If you are uncertain, you should discuss this with your doctor and/or optician (optometrist).
The DVLA prescribed eyesight requirements are:
To read in good daylight (with the aid of glasses or contact lenses if worn) a registration mark fixed to a motor vehicle and containing letters and figures 79 millimetres high and 50 millimetres wide at a distance of 20 metres, or at a distance of 20.5 metres where the characters are 79 millimetres high and 57 millimetres wide.
Visual acuity (with the aid of glasses or contact lenses if needed) must be at least 6/12 with both eyes open (or in the only eye if you have vision in one eye only).
Note that in the presence of cataract, glare may affect your ability to meet the number plate requirements, even if your acuity is good enough.
Frequently asked questions
Back to contentsHow long can you have cataracts for before needing treatment?
There’s no set time limit for how long you can have cataracts before needing treatment. Cataracts usually develop slowly over years, and treatment is only needed when they start to significantly affect your vision or daily activities such as reading and driving.
Can cataracts come back?
Once a cataract is removed, it cannot grow back. However, some people may develop a cloudy layer behind the new lens months or years after surgery, known as posterior capsule opacification (PCO). This can be easily treated with a quick laser procedure to restore clear vision.
Can you prevent cataracts?
You can’t always prevent cataracts, as they’re often linked to ageing. However, protecting your eyes from UV light, eating a healthy diet rich in antioxidants, not smoking, and managing health conditions like diabetes may help reduce your risk or slow their development.
Dr Mary Lowth is an author or the original author of this leaflet.
Patient picks for Eye conditions

Eye health
Acute angle-closure glaucoma
Acute angle-closure glaucoma is a serious eye condition that occurs when the fluid pressure inside the eye rises quickly, leading to sudden, severe eye pain, a red eye and reduced or blurred vision. It is a medical emergency.
by Dr Philippa Vincent, MRCGP

Eye health
Eye problems
Eye problems range from everyday irritations to serious internal conditions. This leaflet contains a list of conditions which affect the eye, grouped together by the part of the eye which is affected or involved.
by Dr Toni Hazell, MRCGP
Further reading and references
- Implantation of accommodating intraocular lenses for cataract; NICE Interventional Procedure Guidance, February 2007
- Implantation of multifocal (non-accommodative) intraocular lenses during cataract surgery; NICE Interventional Procedure Guidance, June 2008
- Zhao L, Chen XJ, Zhu J, et al; Lanosterol reverses protein aggregation in cataracts. Nature. 2015 Jul 30;523(7562):607-11. doi: 10.1038/nature14650. Epub 2015 Jul 22.
- Cataracts in adults: management; NICE Guideline (Nov 2017)
- Nizami AA, Gulani AC; Cataract
- Moshirfar M, Milner D, Patel BC; Cataract Surgery
- Hamid M, Shiwani HA, Hamid F; A survey of anaesthetic preferences in cataract surgery. Int J Ophthalmol. 2022 Feb 18;15(2):342-345. doi: 10.18240/ijo.2022.02.22. eCollection 2022.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
21 Jun 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.