Varicose eczema
Gravitational eczema
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 21 Feb 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Varicose veinsVenous leg ulcersSuperficial thrombophlebitis
Varicose eczema is a tightened skin condition that affects the lower legs, mainly occurring in the elderly. It initially causes your skin on the lower legs to become pale red, and then darker red, often becoming stained brown. With varicose eczema the skin on your lower legs also gets slightly thicker and bumpy. It may be very painful but there may be no pain. Itchiness is also variable from mild to severe. Because your skin is red with varicose eczema, it is often mistaken for an infection. The treatment is to keep your legs up when you're sitting down, to stay active and to apply moisturisers. Occasionally steroid ointments are used, which are prescribed by a doctor.
In this article:
Video picks for Veins
Continue reading below
What is varicose eczema?
This is the term used for skin changes that happen when the pressure in the veins of the legs increases. You may also hear it called gravitational eczema, stasis eczema or venous eczema.
What does varicose eczema look like?
Back to contentsThis is a photo of varicose eczema in an elderly man. It's an example of long-standing varicose eczema, as seen by the thickened, dark-stained skin:
Varicose eczema
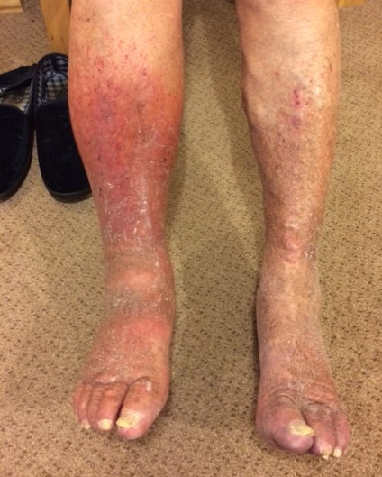
Image featured here with full consent from patient for use by Patient.info
Continue reading below
Varicose eczema symptoms
Back to contentsSymptoms of varicose eczema may include:
The skin looks red and can be slightly shiny (which is why some people mistake varicose eczema for an infection).
The skin should feel cool to the touch, not warm.
The skin gets flaky and scaly.
The skin may also look 'rusty' or brown in colour.
The skin, particularly the skin around your ankle, may feel hard or tight.
You can get little raised bumpy 'blisters' in the skin. Sometimes these are hard; other times they might leak a drop of clear fluid if you press them.
Pain and itchiness are variable, ranging from absent to severe.
It can feel like your legs are warm, although they are not warm to the touch.
Generally it all starts in the skin around the inside of your calf, above your ankle.
Some skin may 'break down' into an ulcer. See the separate leaflet called Venous Leg Ulcers for more information on this condition. If the ulcer is small and heals up, it can leave a star-shaped white mark.
Who gets varicose eczema?
Back to contentsVaricose eczema mainly affects older people. As many as one in five people over the age of 70 develop varicose eczema. People most at risk are those who have varicose veins, who have had varicose vein surgery, or who have had a thrombosis in a deep leg vein (deep vein thrombosis - a DVT). Varicose eczema is more common in women.
Continue reading below
What causes varicose eczema?
Back to contentsVaricose eczema is caused when pressure increases in the veins running under the skin and in the deep muscles of the legs. This raised pressure is due to leaky valves in the veins. When the valves are not working well, it is difficult for the blood to flow back up the legs against gravity. So they are more full of blood than they should be, which means the pressure inside them is higher.
The increased pressure in the veins makes them leak. Fluid and blood cells leak out of the veins and under the skin. This can sometimes be triggered when you have had surgery or injury to your legs.This sets off a reaction under the skin. The effect of this is inflammation of the skin and then eczema. Over time the affected skin becomes harder and discoloured. Because skin with eczema is scaly and can become broken, it is more prone to developing ulcers.
Other causes of varicose eczema
These include:
Pregnancy - this can increase the pressure in your leg veins.
Obesity - more weight can also increase pressure in your leg veins.
Health conditions - varicose eczema can also occur after a blood clot (thrombosis) forms in the deep veins.
What is the best treatment for varicose eczema?
Back to contentsGeneral advice for treating varicose eczema
The most important thing is to put your legs up as high as possible when sitting. Most pouffes or footstools just aren't high enough: it's best to have your feet as high as your hips, or even a bit higher! (When your legs are up, gravity helps the blood flow back up the legs.)
Try to avoid injuring the skin (for example, against furniture).
Keep active and go for regular walks. (When the muscles in your legs are active, they help push the blood in the veins back up the legs.)
Avoid standing still for a long period of time. (In this position there is more pressure on the veins in the legs. The muscles are not squeezing the veins, as they do when you are walking.)
Make sure the skin does not become too dry, by using regular moisturising creams (emollients). See the separate leaflet called Moisturisers (Emollients) for Eczema for more details.
Steroid applied to the skin
If the skin becomes very inflamed, your doctor may prescribe a topical steroid (steroid creams or ointments applied to the skin). Topical steroids work by reducing inflammation in the skin. The steroid is applied as an ointment rather than a cream if the skin is very dry. A moderate-strength steroid is usually prescribed unless the skin is very inflamed, in which case a very strong ointment may be needed.
Topical steroids are usually applied once a day (sometimes twice a day - your doctor will advise). Rub a small amount thinly and evenly just on to areas of skin which are inflamed. (This is in contrast to emollients described earlier which are applied generously.)
To work out how much you should use for each dose, squeeze out some ointment from the tube on to the end of an adult finger - from the tip of the finger to the first crease. This is called a fingertip unit. One fingertip unit is enough to treat an area of skin twice the size of the flat of an adult's hand with the fingers together. Gently rub the cream or ointment into the skin until it has disappeared. Then wash your hands.
Compression stockings
Compression stockings are also known as compression hosiery. The stockings work by applying pressure from outside the veins. This helps squeeze the blood in the veins back up the legs. This then makes the pressure inside the veins less. In turn this prevents leakage of blood into the surrounding tissues.
Before compression stockings are advised you will need to have a test to check that the circulation through the arteries of your legs is normal. This is usually done by the practice nurse, with a handheld machine called a Doppler. This measures the pressure in your arteries.
Compression stockings come in light, medium or strong material (class 1, 2 or 3) and are worn below the knee. Most people can tolerate class 2. If class 2 is too uncomfortable or difficult, class 1 is prescribed. If class 2 stockings do not work, it may be necessary to try class 3, although many people find these difficult to wear for any length of time.
These can be prescribed by your doctor and obtained at the chemist. People often do not like wearing these stockings because they are uncomfortable, or difficult to put on, or don't look very nice. But they really help your circulation and can prevent serious problems such as ulcers.
Further tips on support stockings
They are available in different colours, so do ask for the one that suits you best. That way, you are more likely to use them.
They should be removed at bedtime and put on first thing in the morning. It is important to put them on before your legs start to swell in the mornings.
There are open or closed toe options. Open toe stockings may be useful if:
You have painful toes due to arthritis or infection.
You have large feet.
You want to wear socks over your support stockings.
You prefer them.
Stockings should be replaced every 3-6 months. Each time you should be measured again, just in case the size needs to be changed.
You should always have at least two pairs prescribed so that one pair can be washed and dried while the other is worn.
Do not tumble dry support stockings, as this may damage the elastic.
They can be made to measure if the standard sizes don't fit you. This can still be done with a prescription.
Support stocking applicator aids are available if you are unable to get them on. You can discuss this with your pharmacist or nurse.
Can you fly with varicose eczema?
Varicose eczema is seen in people who have varicose veins, or have had a deep venous thrombosis (DVT). These conditions are an increased risk for forming a (further) deep venous thrombosis. This is a blood clot in the leg which can have serious consequences. During a flight this risk increases because you are relatively immobile for long periods of time. It is estimated your risk of having a DVT increases 2-3 times from a long-haul flight.
You can fly but if there is an alternative way to travel where you can walk about more, it would be safer to do so. If you have to fly you should take sensible precautions, such as:
Remaining adequately hydrated.
Exercising the calves.
Spending time out of the seat.
Avoiding excess alcohol.
Avoiding tight-fitting socks or stockings.
Perhaps using graduated compression stockings.
Does varicose eczema go away?
Back to contentsIf your condition does not seem to be responding to treatment, your doctor may consider patch testing to check if you have developed contact dermatitis. This is a sensitivity to any of the creams, ointments or dressings you have applied to the skin. Patch testing involves putting various chemicals in patches on to the skin to see whether a reaction develops. This is usually done by a skin specialist (dermatologist).
You may also be referred to a dermatologist for more specialised advice about your skin problem.
Lack of progress sometimes means that infection has set in. Antibiotic tablets, such as flucloxacillin, may be needed if this is the case.
You may need to be referred to a surgeon who specialises in arteries and veins (a vascular surgeon). You may require an operation if:
Your varicose eczema will only get better if underlying varicose veins are treated.
You have a leg ulcer which is not responding to medical treatment.
You have a blockage in the arteries of the leg.
Can you treat varicose eczema naturally?
Back to contentsHerbal preparations applied to the skin have been known to cause allergic reactions and are best avoided. It may be that a herbal treatment made from horse chestnut seed extract and taken by mouth can help. However, more tests are needed on this to decide on the best dose to take. It cannot be prescribed by your doctor, but may be available from health food shops, etc.
Patient picks for Veins
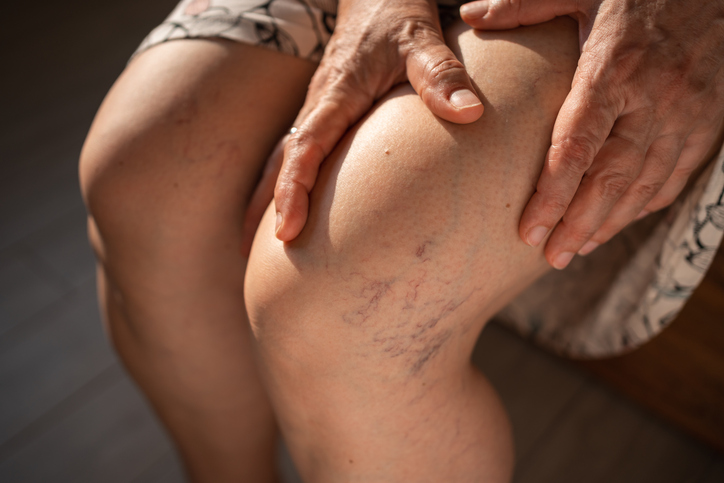
Heart health and blood vessels
Varicose veins
Studies suggest that varicose veins occur in 10-20 out of 100 men and 25-33 out of 100 women. Most people with varicose veins do not have an underlying disease. They often occur for no apparent reason, although they are associated with lifestyle factors in some cases. Varicose veins do not cause symptoms or complications in most cases, although some people find them unsightly. If treatment is advised, or wanted for cosmetic reasons, a procedure to seal them off is used. There are several procedures available: heat, lasers or chemicals injected into the veins. These methods have largely replaced the old-fashioned surgical methods such as stripping the veins out.
by Dr Colin Tidy, MRCGP

Heart health and blood vessels
Venous leg ulcers
Venous leg ulcers are common in older people. The most important part of treatment is for compression bandages to be applied correctly by a nurse. Keep as active as possible but elevate your leg when you are resting. Other treatments may be advised in some cases, such as a skin graft or vein surgery. After an ulcer has healed you should wear a support stocking each day, which helps to prevent it recurring.
by Dr Hayley Willacy, FRCGP
Further reading and references
- Venous Eczema; DermNet
- Venous eczema and lipodermatosclerosis; NICE CKS, March 2022 (UK access only)
- Compression stockings; NICE CKS, May 2022 (UK access only)
- Yao P, Mukhdomi T; Varicose Vein Endovenous Laser Therapy.
Continue reading below
About the author

Dr Laurence Knott
General Practitioner, Medical Author
BSc (Hons) Biochemistry, MBBS
Dr Laurence Knott qualified in 1973 and has had extensive experience as a General Practitioner.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 20 Feb 2028
21 Feb 2023 | Latest version
28 Sept 2011 | Originally published
Authored by:
Dr Laurence Knott

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.