
How the seasons affect your eczema
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Lynn StephenLast updated 12 Feb 2026
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
As we battle through the final stretches of winter, many of us are eyeing our coats and scarves with disdain and fantasising about sunnier days to come. This applies doubly so to people with eczema - many of whom find their symptoms peak in winter and recede with the onset of spring.
In this article:
Video picks for Eczema
Dr Anton Alexandroff, a Consultant Dermatologist, explains that eczema usually improves in summer with some natural sunlight and gets worse in winter when it is cold and damp.
He says: "Skin can also get drier with central heating in winter, especially for those with asteatotic eczema, which is more common in senior people and is mostly due to skin drying out too much."
While every person with eczema has their own triggers, in many cases flare-ups can follow a seasonal pattern. So much so, in fact, that asteatotic eczema is often known as 'winter itch'. It's not uncommon to find that your eczema lies dormant most of the year, only to reignite in response to cold or heat.
So why is this the case? And other than waiting stoically till summer, is there anything people can do?
Continue reading below
What is eczema?
Eczema, also known as dermatitis, is a common itchy inflammatory skin condition, often associated with an abnormal skin barrier. It looks different for every person, but you may experience patches of dry scaly skin, small raised bumps, and severe itching. This might occur in just a few small patches or may be more widely spread across your body.
There are several variants - for instance, allergic contact dermatitis - in which your skin flares up in response to external agents, for example, fragrances or preservatives - or irritant contact dermatitis - caused by a persistent irritation of the skin.
However, the most common type is atopic (allergic) dermatitis, which usually begins in infancy or childhood and affects up to 1 in 3 children, and 1 in 10 adults, in the UK. Although many children find the condition clears up naturally as they get older, many people continue to experience flare-ups throughout their lives.
"It's due to a genetic predisposition which affects the integrity of the skin barrier, and is often associated with a mutation in the so-called filaggrin gene," explains Alexandroff. "As a result, environmental and/or microbial allergens penetrate the skin barrier more easily and cause inflammation of the skin."
This condition is associated with asthma and hay fever, meaning that if you or a family member have one of the three, you're more likely to have the others. Research studies have shed some light on why, pinpointing a cluster of genetic risk factors that predispose you to all three allergic conditions.
Despite learning more about the causes, researchers haven't yet developed a cure. This means, if you or your child have eczema, it's important to work out the individual triggers and adopt strategies for managing the symptoms.
The winter itch
Back to contentsIf your flare-ups happen predominantly in winter, this is likely due to switching between cold and hot environments. Harsh, windy conditions outside - followed by dry, centrally heated environments inside - can wreak havoc on your skin.
As if that were not enough, some people find their eczema triggered by dust mites - which thrive in warm indoor environments. On top of this, many people experience a vitamin D deficiency during winter, which some studies have linked to higher rates of eczema, although the evidence is not conclusive on this front.
"Infections, such as colds, non-specifically flare up dermatitis because they upset the immune system in general," adds Alexandroff.
Perhaps paradoxically, many winter eczema management strategies come down to avoiding extremes of heat. First up, make sure your home isn't overheated, and invest in a humidifier if dry air inside is a concern. When you bathe or shower, lukewarm - not hot - temperatures are best for your skin. And, since heavy winter clothing can cause sweating, the National Eczema Society advises layering up - clothing made from cotton or silk is best.
Above all, it's critical to maintain a rigorous moisturising routine. According to Allergy UK, you should continue this routine all year round, not just during flare ups.
"Greasier moisturisers are more effective so ointments are better than creams and lotions," says Alexandroff. "Wash with moisturiser and add bath oils to your bath, avoiding soaps, shower gels, and bubble bath, which de-grease the skin."
Continue reading below
Eczema at other times of year
Back to contentsAlthough eczema generally improves in the spring, for some people the opposite holds true. Seasonal pollen can be a trigger, causing eczema flare-ups alongside hay fever. You may wish to take an antihistamine if this applies to you. Some people also find their symptoms exacerbated by temperature changes, and get flare-ups during the transitional seasons - for example, spring and autumn.
Others find that their symptoms worsen in the summer months. Typically, this is due to the heat itself, which may cause sweating, coupled with the drying effects of air conditioning once you get inside. There may also be further triggers at this time of year, such as swimming in a chlorinated pool or sitting on grass.
In each of these cases, the usual advice applies - try to pinpoint any environmental triggers and minimise your exposure to them wherever possible. Try to stay cool, rinse off chlorine straightaway, and always make sure to moisturise.
Further tips
Back to contentsIt's also advisable to see a health professional if anything changes, or your symptoms are proving hard to manage on your own.
"If your eczema suddenly gets out control, it may be possible that you have developed an allergy to something you have come in contact with, such as fragrance, dyes or preservatives," says Alexandroff. "A dermatologist can arrange a patch allergy test for you to make sure you have not developed allergic contact dermatitis."
It's worth being aware that this service isn't always available on the NHS, and that if it is, waiting times can be long.
If your eczema is severe, you may need a prescription treatment.
"See your doctor or dermatologist to get more intensive treatment - for example, with appropriate creams and non-steroidal cream such as pimecrolimus cream," says Alexandroff.
Patient picks for Eczema

Skin, nail and hair health
What causes sudden eczema in adults?
A flare-up of eczema can be caused by any number of things, from using washing-up liquid to being exposed to cold air. However, it can be difficult to pinpoint what has triggered a sudden bout of eczema and caused your skin to become red, itchy or sore.
by Lydia Smith
Skin, nail and hair health
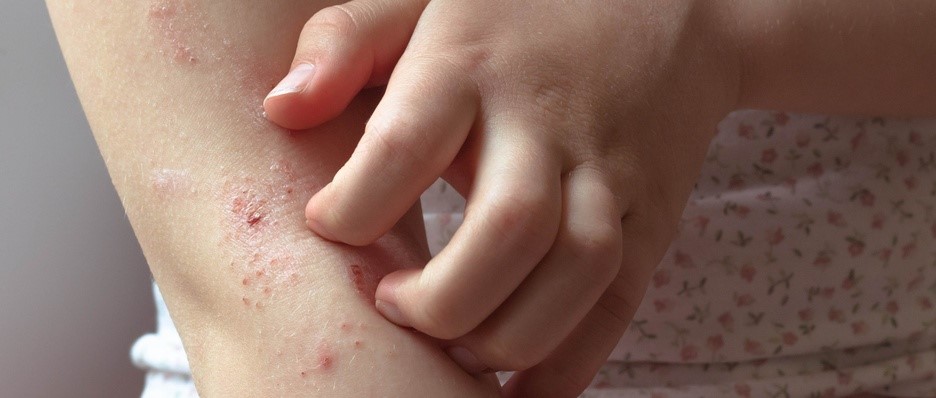
Why eczema itches - and how to stop it
Itchiness is one of the most uncomfortable symptoms of eczema - and the urge to scratch can be unbearable. Itchy skin can also lead to sleep problems and make it hard to concentrate, but scratching can make the skin feel sore and lead to infections. So what can you do to ease the itchiness of eczema?
by Lydia Smith
Continue reading below
About the authorView full bio

Abi Millar
Freelance Journalist
BA (Hons), MA
Abi is a freelance journalist with a special interest in health and medicine writing.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is peer reviewed by qualified clinicians.
Next review due: 12 Feb 2029
12 Feb 2026 | Latest version
9 Mar 2018 | Originally published
Authored by:
Abi Millar

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.