Cervical insufficiency and suture
Incompetence and cerclage
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 20 Nov 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Cervical insufficiency (sometimes called cervical incompetence) occurs when the neck of the womb (the cervix) softens, shortens and opens without any other symptoms of labour. This may be in the second trimester or early in the third, leading to premature delivery of the baby.
Cervical suture - also called cervical cerclage or cervical stitch - is a stitch placed in/around the cervix. This is to try to prevent late miscarriage or premature birth in women who are felt to be at high risk of cervical insufficiency.
At a glance
Cervical insufficiency means the cervix painlessly softens and opens too early in pregnancy.
This can lead to late miscarriage or premature birth.
A cervical suture is a stitch placed around the cervix to keep it closed.
It is most effective when planned for women at high risk of premature delivery.
Planned cervical sutures have a low risk of complications.
The suture is usually removed around 36-37 weeks of pregnancy.
Sign up for our free 8-week Healthy Pregnancy course!
Each week we’ll share useful information and essential tips on topics such as nutrition, exercise, mental health, symptoms to look out for, and preparing for childbirth, to help you navigate your pregnancy journey whatever stage you are at.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
In this article:
Video picks for Pregnancy complications
This information is about cervical insufficiency and cervical suture. It may be helpful when planning to become pregnant and there has previously been a problem with cervical insufficiency. Or, if there was a late miscarriage (after 12-14 weeks) or there was a baby born prematurely.
Continue reading below
What is cervical insufficiency?
During pregnancy the neck of the womb (cervix) normally remains closed and 'long', like a tube. As pregnancy progresses and the body prepares to give birth, the cervix gradually softens, decreases in length (effaces) and opens (dilates).
Cervical insufficiency (cervical incompetence) occurs when the cervix softens and opens painlessly, without being in labour, after 12 weeks of pregnancy but well before the baby is due to be born.
This may cause the waters to bulge and break through the open cervix, and the baby to be born prematurely. Cervical insufficiency is a painless opening of the cervix. It is not the same as premature labour, where the cervix opens because the womb (uterus) has started to contract, although it tends to lead to premature labour.
What is the cervix?
The cervix is the lower part of the womb (uterus) which extends slightly into the top of the vagina. The cervix is often called the neck of the womb.
Uterus and cervix
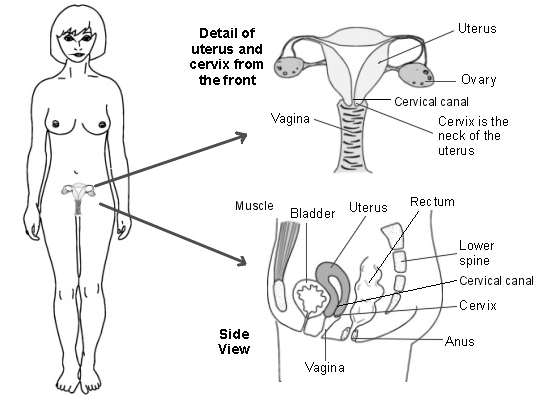
See separate leaflet called Common Problems of the Cervix.
What causes cervical insufficiency?
Back to contentsIt is not usually known why some women have this happen to their cervix. It is thought possible that, in some women, the cervix is not as strong. It is possible that infection, inflammation or previous damage to the cervix can sometimes plays a role.
Cervical insufficiency is known to be more likely in women who:
Have inherited disorders of collagen synthesis (for example, some of the Ehlers-Danlos syndromes).
Have had surgery such as a cone biopsy on the cervix in the past.
Have had injuries to the cervix during a previous birth or dilation and curettage (D&C).
Have some lifelong (congenital) abnormalities of the shape of the womb.
Have had previous miscarriages in the second trimester, particularly if this has happened more than twice.
Are known to have had cervical incompetence in a previous pregnancy.
Have a mother who took the medicine called diethylstilbestrol (DES) while she was pregnant with you. DES was used to prevent miscarriage but has not been used in the UK since 1971. It has, however, been used more recently elsewhere in the world.
Continue reading below
How common is cervical insufficiency?
Back to contentsUnfortunately there are no data on this diagnosis specifically. The closest relevant data is the rate of miscarriage that occurs as a result of the cervical incompetence. In the UK, 12-24 weeks gestational age is defined as a late miscarriage with rates varying between 0.7 and 3.0 miscarriages per 100 pregnancies. Another study showed a spontaneous miscarriage rate of 0.4 miscarriages per 100 pregnancies between 15 and 21 weeks. Other publications report the rates of second-trimester miscarriages as between 0.7-2.9 miscarriages per 100 pregnancies.
The rate of cervical incompetence will be less than these figures however, because there are other reasons that miscarriages happen at this stage, such as infections. Overall cervical incompetence is not common.
How is cervical insufficiency detected?
Back to contentsThere are usually no symptoms at all. Some women who have cervical insufficiency do notice vague symptoms, which can include:
Pelvic pressure.
Period pain-type cramping.
Vaginal discharge that increases in volume, becomes wetter or changes from clear, white, or light yellow to pink or bloody.
Losing the mucus plug from the neck of the womb (cervix).
Most women with these symptoms will not have cervical insufficiency. If there is a risk from cervical insufficiency or premature delivery then the obstetrician or midwife may arrange regular transvaginal ultrasound tests, beginning at 14-16 weeks, to measure the length of the cervix and check for signs of early shortening.
Continue reading below
When might a cervical suture be advised?
Back to contentsHaving a premature birth or late miscarriage is a devastating experience. There are likely to be worries about a future pregnancy and concerns about making sure this doesn't happen again.
After a late miscarriage or premature delivery, the woman is referred to a specialist who will talk about plans for any future pregnancy. Depending on the situation, a cervical suture may be one of the options recommended for the next pregnancy.
Planned cervical suture
Cervical suture is generally planned if there is a high risk of premature labour which could be due to cervical insufficiency. It might be one of the following situations:
Previous late miscarriages or premature births (before 34 weeks), when ultrasound scans are offered between 16 and 24 weeks of pregnancy to measure the length of the neck of the womb (cervix). If the scans show that it has shortened to less than 25 mm, the advice will be to have a cervical suture.
Three or more late miscarriages or three or more premature births when the advice will be to have a cervical suture inserted at about 12-14 weeks of pregnancy even if the cervix is not shortened.
In the cases above you would have a planned cervical suture inserted as soon as advised .
Emergency and rescue cervical suture
Sometimes it is noticed during a vaginal examination or a routine ultrasound scan that the cervix has started to open. Depending on the circumstances, an emergency cervical suture might be offered. A 'rescue cervical suture' is an emergency suture which is put in when the cervix is partly open and the waters are bulging through.
Emergency cervical suture carries a higher risk of complications than planned cervical suture. In this situation, a senior obstetrician will discuss the risks and benefits of having a rescue suture.
Beyond 24 weeks pregnant in the UK, a cervical suture is generally not advised. This is because the treatment of premature babies in the UK is of a high standard. It is therefore felt that, at this point, the risks to the baby of attempting to delay labour with an emergency suture (particularly the risk of membrane rupture and infection) are greater than the risks of being born early.
What other treatments might I be offered?
Back to contentsProgesterone
If the pregnancy ultrasound between 16 and 24 weeks of pregnancy reveals that the neck of the womb (cervix) is short, or shortening, but the pregnant woman has not had an early delivery before, they will not usually be offered cervical suture, because they will not be considered at high enough risk of premature delivery to justify the (small but real) risks associated with cervical suture..
In this case they may be offered vaginal progesterone treatment. Evidence suggests that this reduces premature birth in women in whom the cervix is short, even if they have no other reason to think they are at risk of premature birth. Treatment is usually with nightly progesterone pessaries, used up to 34 weeks of pregnancy.
Antibiotics
Antibiotic treatment will be offered if there is any sign of infection. Some doctors give antibiotics as a preventative measure even when there is no sign of infection - for example, an antibiotic pessary that is inserted for one week of each month to try to prevent an infection happening. There is no evidence that this reduces the risk of early delivery.
Arabin pessary
The Arabin pessary is a soft silicone bowl-shaped pessary that is inserted into the vagina by the obstetrician and placed so that the cervix sits inside it. It is designed to support and compress the cervix but also to tilt and slightly rotate it.
This is believed both to take the pressure off the weakest points in the cervix and to protect the mucus plug from being dislodged. There is increasing evidence that, where the cervix is short, the Arabin pessary can delay labour.
Different-sized pessaries are available, and the device is removed at 37 weeks, or when labour begins, if this is sooner.
How is a cervical suture put in?
Back to contentsIn cervical cerclage a stitch (suture) consisting of a band of strong thread is placed around the neck of the womb (cervix). It is usually done sometime between 12 and 24 weeks of pregnancy. Very occasionally it is done as an emergency, usually up to 24 weeks.
Rarely, as the risks to mother and baby are greater, it is offered up to 28 weeks, although more commonly in countries in which the outcomes for babies born at 24-28 weeks are less good than in the UK.
One of two different techniques (the Shirodkar suture or the McDonald suture) may be offered but the principles are similar. The Shirodkar suture is placed a little higher and deeper than the McDonald. The procedure uses a band of strong thread being stitched around the cervix to reinforce it and help hold it closed.
A cervical suture is usually done as an outpatient or day-case procedure using a spinal anaesthetic. In the operating theatre, the woman's legs will be put in supports. The doctor will insert a speculum (a plastic or metal instrument used to separate the walls of the vagina) into the vagina and put the suture around the cervix. The procedure should take less than 30 minutes.
Afterwards, antibiotics are prescribed to help prevent infection and medication is also offered to ease any discomfort. The woman should be able to go home the same day but they should take things easy for a few days and may experience light bleeding or cramping.
After this they can get back to normal. Having sex (intercourse) may be continued when they feel comfortable to do so, unless their doctor advises otherwise. An exception is after emergency cervical cerclage, where the doctor may suggest avoiding sex for a time, sometimes up to 32-34 weeks of pregnancy.
Are cervical sutures sometimes inserted through the abdomen?
Back to contentsYes, very rarely a third technique, in which the suture is put in abdominally through open surgery, is used. This can be done in between pregnancies, or early in the first trimester, before 12 weeks.
It is offered in cases where there have been previous premature deliveries and a cervical suture has been recommended, but it is not technically possible to perform the process vaginally.
This type of suture is usually left in place, meaning that the baby needs to be born by planned caesarean section.
How effective is the cervical suture?
Back to contentsThe cervical stitch (suture) appears most effective when put in in a planned way in women who are at high risk of premature delivery of their baby.
The research into how well a cervical suture stops preterm birth is still inconclusive, but women who have a cervical suture carry their babies for longer than those who do not. The suture is thought to reduce the risk of early delivery (delivery before 37 weeks) in high-risk women by 30-50% .
What are the risks of having a cervical suture?
Back to contentsPlanned cervical suture risks
In planned cervical stitch (suture) the risk of complications is low. There is a small risk that the bladder or the neck of the womb (cervix), or a small blood vessel, may be damaged at the time of the operation.
Rarely, the membranes may rupture during or just after the procedure, and there is a very small risk of infection inside the waters in the womb (uterus). A planned cervical suture does not increase the risk of miscarriage, or premature labour. It does not increase the risk of having to be started off in labour (be induced) or needing a caesarean section.
The risks associated with planned cervical suture go up slightly with gestation, so a planned suture has the least risk of complications if put in as early as possible.
Emergency cervical suture risks
For emergency cervical suture the risk of complications is much higher, particularly if the cervix has not only shortened but is already partly open when the suture is put in. There is a higher rate, in particular, of the waters breaking and of infection developing.
In some cases this may be because the procedure was done so late that the waters were breaking anyway. However, for this reason emergency cervical suturing is a less common procedure.
Are there situations when a cervical suture would not be put in?
Back to contentsSometimes a cervical stitch (suture) is not advised. It will not normally improve the well-being of your baby/babies and may carry risks if:
The pregnancy is more than 24 weeks gestation. In some countries it is used up to 28 weeks, but where care of premature babies is good it is felt to be safer for the baby to be born at 24-28 weeks than for the mother to have the suture).
The pregnancy has twins or triplets.
The womb (uterus) is an abnormal shape.
An ultrasound scan done for another reason happens to show that the neck of your womb (cervix) is short, but you have not previously had an early delivery.
There has been treatment to the cervix for an abnormal smear.
A suture absolutely cannot be put in if:
Labour has already started or your waters have broken.
There are signs of infection in the womb.
There is vaginal bleeding.
There are concerns about the baby's well-being.
If any of these apply but there is a risk of premature labour, the woman is closely monitored. This may include regular vaginal ultrasound scans to measure the length of the cervix until 24 weeks of pregnancy.
The woman may be offered corticosteroid injections after 23 weeks to increase the chance of the baby surviving if born early. Find out more about corticosteroids in pregnancy to reduce complications from being born prematurely.
How is a cervical suture removed?
Back to contentsThe cervical stitch (suture) is not made of dissolving material; it stays in place in the neck of the womb (cervix) until it is removed. It is usually removed at 36-37 weeks, or if you go into labour before then, as if it was left in place it could injure the cervix as it opens.
The McDonald suture can usually be removed quickly without anaesthetic during a vaginal examination, but the deeper, Shirodkar suture may need a short anaesthetic for removal. This suture can sometimes be left in place if there is a planned caesarean delivery and hope to have further pregnancies.
There may be a small amount of bleeding afterwards. Any red bleeding should settle within 24 hours but you may have a brownish discharge for longer than this. If labour begins before the cervical suture has been removed, it is very important to have it removed promptly to prevent it causing damage to your cervix. If the woman believes they are in labour, contact the maternity unit at once and explain the situation.
If the waters break early but there are no signs of labour, the suture will usually be removed because of the increased risk of infection. The timing of this will be decided by the team looking after you, but the woman generally needs to go into the labour unit to be seen.
Once the suture has been removed, do I need to take any special precautions?
Back to contentsNo, when the cervical stitch (suture) has been removed it has served its purpose. Labour may begin soon after it has been removed, as it often does - but this may does not always happen immediately.
Full-term pregnancy is an average of 40 weeks from the last menstrual period and as the suture is removed at 37 weeks, if removing the suture doesn't trigger labour the woman will be in the same boat as everyone else, and may even go beyond the delivery date before labour begins.
Dr Mary Lowth is an author or the original author of this leaflet.
Patient picks for Pregnancy complications

Pregnancy
Pre-eclampsia
Pre-eclampsia involves high blood pressure and protein in the urine. It can have no symptoms but some women may have headache, blurred vision, tummy pain and swollen ankles. The severity of pre-eclampsia is usually (but not always) related to your blood pressure level. It can be a serious condition but specialist care will help mother and baby stay safe.
by Dr Toni Hazell, MRCGP

Pregnancy
Obstetric cholestasis
Obstetric cholestasis is a rare condition. It only affects pregnant women. In the UK fewer than 1 in 100 pregnant women will develop it.
by Dr Philippa Vincent, MRCGP
Sign up for our free 8-week Healthy Pregnancy course!
Each week we’ll share useful information and essential tips on topics such as nutrition, exercise, mental health, symptoms to look out for, and preparing for childbirth, to help you navigate your pregnancy journey whatever stage you are at.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Frequently asked questions
What is the difference between cervical insufficiency and premature labour?
Cervical insufficiency occurs when the cervix softens and opens painlessly, without being in labour, usually after 12 weeks of pregnancy. Premature labour, on the other hand, is when the cervix opens because the womb has started to contract. Although cervical insufficiency often leads to premature labour, the cause of the cervical opening is different.
If I've had cervical insufficiency before, will I definitely experience it in future pregnancies?
Not necessarily. While having cervical incompetence in a previous pregnancy makes it more likely to happen again, it is not a definite outcome. If you have had a late miscarriage or premature delivery, you will be referred to a specialist to discuss plans for future pregnancies, which may include recommending a cervical suture.
Why is a cervical suture not usually advised after 24 weeks of pregnancy in the UK?
After 24 weeks of pregnancy, a cervical suture is generally not advised in the UK due to the high standard of care for premature babies. At this stage, it's felt that the risks to the baby of attempting to delay labour with an emergency suture (such as membrane rupture and infection) are greater than the risks associated with being born early.
Can I have sex after a cervical suture is put in?
After a planned cervical suture, you can usually continue having sex when you feel comfortable, unless your doctor advises otherwise. However, if you've had an emergency cervical suture, your doctor might suggest avoiding sex for a period, sometimes until 32-34 weeks of pregnancy.
What happens if I go into labour before my cervical suture is removed?
If you go into labour before your cervical suture is removed, it is very important to have it removed promptly to prevent damage to your cervix as it opens. You should contact your maternity unit immediately and explain your situation.
Does having twins or triplets affect whether I can have a cervical suture?
Yes, a cervical suture is generally not advised if you are pregnant with twins or triplets. There are situations where a cervical stitch is not recommended because it may not improve your babies' well-being and could carry risks.
What should I expect shortly after a cervical suture is put in?
After a cervical suture procedure, you may be prescribed antibiotics to help prevent infection and medication to ease any discomfort. You should be able to go home the same day but should take things easy for a few days. It's common to experience light bleeding or cramping. After this initial period, you can usually return to your normal activities.
Further reading and references
- Preterm labour and birth; NICE Guidelines (November 2015 - last updated June 2022)
- Alfirevic Z, Stampalija T, Medley N; Cervical stitch (cerclage) for preventing preterm birth in singleton pregnancy. Cochrane Database Syst Rev. 2017 Jun 6;6:CD008991. doi: 10.1002/14651858.CD008991.pub3.
- Cervical cerclage (Green-top Guideline No. 75); Royal College of Obstetricians and Gynaecologists (February 2022)
- Abdel-Aleem H, Shaaban OM, Abdel-Aleem MA, et al; Cervical pessary for preventing preterm birth in singleton pregnancies. Cochrane Database Syst Rev. 2022 Dec 1;12(12):CD014508. doi: 10.1002/14651858.CD014508.
Continue reading below
About the authorView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 18 Nov 2028
20 Nov 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.