Actinic keratosis
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Colin Tidy, MRCGPLast updated 12 Jul 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Actinic keratosis article more useful, or one of our other health articles.
In this article:
Synonyms: solar keratosis
Continue reading below
What is actinic keratosis?
The term actinic keratosis (AK) was coined in 1958 and means literally thickened scaly growth (keratosis) caused by sunlight (actinic). The condition is also known as solar keratosis.
Actinic keratoses are ultraviolet (UV) light-induced lesions of the skin, which are by far the most common lesions with malignant potential to arise on the skin. In some cases, they progress to invasive squamous cell carcinoma (SCC).
Actinic keratosis is seen most commonly in fair-skinned people in areas of long-term sun exposure caused by UV rays - for example, using tanning beds. Although the condition is very similar to Bowen's disease or carcinoma in situ, most lesions do not progress to malignancy. However, recognition and simple treatment help to prevent progression.
Pathophysiology1
Back to contentsThe condition is caused by UV-induced DNA damage within the skin.
Cells within AKs show characteristic UV-induced gene mutations.
Human papillomaviruses (HPVs) have been implicated as co-carcinogens in the pathogenesis.2
Histologically AKs share features with SCC. AK is an epidermal lesion characterised by:
Collections of atypical, pleomorphic keratinocytes in the basal layer which can extend to the upper granular and cornified layers.
The epidermis being abnormal in architecture, with acanthosis, parakeratosis and dyskeratoses. Cellular atypia is present with keratinocytes varying in size and shape.
Mitotic figures being present.
Limitation to within the epidermis only.
AKs can resolve spontaneously, stay stable, or progress to Bowen's disease (carcinoma in situ) or to SCC. They can be distinguished more by the degree of cellular change and the extent of the lesions rather than differences in the features of individual cells.
Actinic keratosis is considered by some to be the earliest manifestation of SCC.2
Continue reading below
How common is actinic keratosis?(epidemiology)
Back to contentsActinic keratosis occurs most often in individuals with fair skin, blonde hair and blue eyes at a rate according to cumulative UV exposure.
Frequency increases according to a number of risk factors:
Increasing age, as the dose of UV is cumulative.
Proximity to the equator, as this affects UV dosage and cumulative exposure.
Lifestyle and time spent outdoors. Outdoor lifestyles, whether with work or recreation and sport, will increase risk.
How fair the individual's skin is. Skin is graded from Fitzpatrick type I to VI according to sensitivity to sunlight, as displayed by a tendency to burn or to tan. These lesions are almost entirely confined to fair skin types I and II.
Patients who are immunosuppressed following organ transplantation have a markedly increased risk of developing AKs and of developing malignant change in the AKs. This also applies to people who have undergone chemotherapy for malignant disease and those with HIV infection.
Sunbeds and therapeutic UV radiation also increase risk. Artificial sunlight may produce lesions in unusual places
AKs are more common in men than in women. Possibly this is because traditionally men are more likely, with work and recreational activities, to spend time outdoors.
It is rare under the age of 45 years in the UK, then prevalence increases with age.3 In Australia, however, for those aged 30-39 years, the rate is 22% for men and 8% for women.4
Overall, the rate in Australia is highest with a reported prevalence of around 40-60% in white individuals over the age of 40 years.1
In the UK, prevalence has been reported to be around 19-24% of the population over the age of 60 years.5
Even where an AK does not progress, it is a sign of sun damage, and individuals with AK have a higher risk of skin malignancy in general.5
Actinic keratosis symptoms
Back to contentsLesions (skin growths) occur in fair-skinned people, in parts of the body exposed to long-term sun exposure, such as the head area (face, ears, scalp), forearms and backs of the hands. Other areas repeatedly exposed to the sun include the back, the chest and the legs.
Forehead actinic keratoses
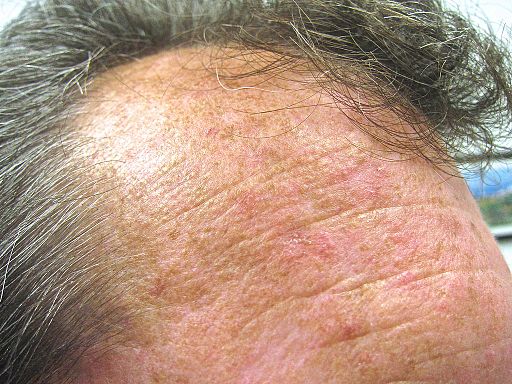
© Future FamDoc (own work), via Wikimedia Commons
There may be other features of solar damage, such as telangiectasias, elastosis and pigmented lentigines.
The first lesion is usually a single plaque on the face; however, with time and further exposure to strong sunlight, they tend to progress on the nose, forehead and cheeks.
AKs begin as small rough scaly patches that are more easily felt than seen (like rubbing sandpaper). Over several years, lesions enlarge, often becoming red and scaly. From small 3-10 mm lesions they can enlarge, although they are usually no bigger than 1 cm each.2 3
Individuals affected by actinic keratosis may develop a multiplicity of such lesions within a sun-exposed area. Lesions collide and produce confluent AK over a relatively large area. The area surrounding AKs is at risk of changes; it is called the 'field' and may be targeted for treatment along with the individual lesion(s).
Variations on this theme include brown (pigmented AK), lichen planus-like areas, and exaggerated hyperkeratosis (the horn-like projection known as a cutaneous horn, for example).
They flare and become more erythematous when immunity is suppressed. This may be with systemic disease or its treatment (such as chemotherapy for malignancy) but it can also be the result of too much UV light.
In time, and especially with continued exposure to strong sunlight, there is a risk of malignant change. In an individual with an average of 7.7 AKs, the risk of one becoming malignant within 10 years is about 10%.5 This is more likely in those that are erythematous, elevated and indurated. It may be necessary to remove the layer of keratin to see this.
For more images of AKs, see the websites of the Primary Care Dermatology Society (PCDS) and DermNet NZ.3 6
Continue reading below
Actinic keratosis diagnosis2 7
Back to contentsDiagnosis of actinic keratosis is usually clinical, ideally with the help of a dermatoscope. Confocal laser microscopy and optical coherence tomography can also help in diagnosis. Skin biopsy is used where there are features which are high risk for malignant change.
Clinical classification of individual lesions is as follows:
Grade 1: slightly palpable (better felt than seen).
Grade 2: moderately thick (easily felt and seen).
Grade 3: very thick, hyperkeratotic and/or obvious.
There may also be field damage: Large areas of multiple AKs on a background of erythema and sun damage.
Differential diagnosis
Back to contentsBasal cell carcinoma (BCC) and squamous cell carcinomas (SCCs) (these are indurated nodular lesions reflecting more rapid growth and tend to be eroded or ulcerated on the surface).
Seborrhoeic warts (produces greasy, brown crusts with sharply demarcated borders and a non-erythematous base. They may occur in areas that are not exposed to sun).
Bowen's disease (tends to be a large plaque with a sharp outline).
Discoid lupus erythematosus (shows abnormal pigmentation, dilated follicles and atrophy).
Referral8
Back to contentsMany cases can be managed in primary care by a GP with special interest (GPwSI).
Refer through the two-week suspected cancer pathway if there are features suspicious of SCC:
Recent growth/tenderness/inflammation.
A nodular lesion.
Bleeding/ulceration.
Lesions on the lips.
Refer non-urgently for the following:
Diagnostic uncertainty.
People with more widespread/severe actinic damage.
Immunosuppressed people, particularly post-transplant.
Very young patients presenting with AK (consider xeroderma pigmentosum).
Actinic keratosis treatment and management2 5 8
Back to contentsThe British Association of Dermatologists guideline recommends that most lesions can be treated in primary care with topical treatments and trying to classify them into grades 1–3, which will help direct management. It is also useful to consider that treatment is not always required, and if it is, patients should be encouraged to participate in their treatment. When there is a suspicion that an AK is transforming into SCC, patients should be referred expediently along the 2-week wait pathway. This is particularly important in patients who are immunosuppressed and are therefore at increased risk of SCC.
General
People with actinic keratosis should be advised:
To limit sun exposure and use sun protection to protect your skin.
About the use of emollients where required for symptomatic relief. Emollients used regularly may also help distinguish treated areas of dry skin from AK.
To report changes in existing lesions, or development of new ones. Explain there is a high chance of developing more areas of AK.
That AK is a marker for skin cancer and to be vigilant and report any skin changes.
That topical treatments cause inflammation, which is how they work, and that they should expect the skin to look worse before it starts to get better. Pictures are helpful.
Perform a full skin examination to check for other suspicious skin lesions.
Treatment options4
There are a number of options available to treat AKS. Choice depends on the clinical grade, site, the number of lesions, presence or absence of field damage, and size of the area of skin affected.
Topical treatment options for actinic keratosis include:
5-fluorouracil (5-FU) cream: used for individual lesions or small areas of field damage.
5-FU 0.5% and salicylic acid 10%: used once a day for 6-12 weeks. Used for moderately thick hyperkeratotic lesions. Very thick lesions will need ablative therapy.
3% diclofenac gel in sodium hyaluronate: used twice a day for 12 weeks. Used for thin areas or larger areas of field damage.
5% imiquimod cream: for multiple lesions and small areas of field damage.
3.75% imiquimod cream: used for multiple lesions and larger areas of field damage.
Ablative treatment options include:
Cryotherapy. Used for single or multiple discrete lesions, but not for field damage.
Photodynamic therapy (PDT). Used for individual lesions; this has been found to be more effective than cryotherapy and to give a better cosmetic result.
Curettage or excisional surgery. Used for discrete hyperkeratotic lesions.
Complications
Back to contentsThe most important complication is the progression to malignant change if left untreated.
Actinic keratosis prognosis
Back to contentsMany individual AKs regress spontaneously, however there is a high risk of recurrence or the development of new lesions.9
Progression to SCC occurs slowly. Although known to be pre-malignant, the probability of a lesion undergoing transformation to SCC is not known; however, evidence suggests this ranges from 0.025% to 16% per year.4 When progression to malignancy does occur, it tends not to be an aggressive cancer and distant metastases are rare.
Actinic keratosis prevention6
Back to contentsIt is important to educate patients that AKs can be reduced or delayed by use of sunscreens but, most importantly, by reducing sun exposure:
Patients should limit all sun exposure, whether recreational or work-related.
It is particularly important to avoid sun in tropical areas.
It is best to seek shade, particularly when the sun is high between 11 am and 3 pm.
For patients unable to avoid sun exposure, apply a sunscreen (sun protection factor (SPF) 30 or more) and wear protective clothing daily (for example, hats, long sleeves).
Bald heads are a common site for AK and should be protected with a hat.
AKs are a biological marker of sun damage and hence patients with AKs are at a greater risk of skin cancer than those with no AKs. Patients with AKs also need to be educated on self-monitoring and the need to seek a medical opinion if they detect new lesions or changes in old lesions on their skin.
Further reading and references
- Photodynamic therapy for non-melanoma skin tumours (including premalignant and primary non-metastatic skin lesions); NICE Interventional procedure guidance, February 2006
- Dirschka T, Gupta G, Micali G, et al; Real-world approach to actinic keratosis management: practical treatment algorithm for office-based dermatology. J Dermatolog Treat. 2017 Aug;28(5):431-442. doi: 10.1080/09546634.2016.1254328. Epub 2016 Nov 13.
- Dodds A, Chia A, Shumack S; Actinic keratosis: rationale and management. Dermatol Ther (Heidelb). 2014 Jun;4(1):11-31. doi: 10.1007/s13555-014-0049-y. Epub 2014 Mar 14.
- Werner RN, Stockfleth E, Connolly SM, et al; Evidence- and consensus-based (S3) Guidelines for the Treatment of Actinic Keratosis - International League of Dermatological Societies in cooperation with the European Dermatology Forum - Short version. J Eur Acad Dermatol Venereol. 2015 Nov;29(11):2069-79. doi: 10.1111/jdv.13180. Epub 2015 Sep 14.
- Solar keratosis; Primary Care Dermatology Society (PCDS)
- Gupta AK, Paquet M, Villanueva E, et al; Interventions for actinic keratoses. Cochrane Database Syst Rev. 2012 Dec 12;12:CD004415. doi: 10.1002/14651858.CD004415.pub2.
- British Association of Dermatologists guidelines for the care of patients with actinic keratosis 2017; British Association of Dermatologists (2017)
- Actinic keratosis; DermNet NZ
- Casari A, Chester J, Pellacani G; Actinic Keratosis and Non-Invasive Diagnostic Techniques: An Update. Biomedicines. 2018 Jan 8;6(1). pii: biomedicines6010008. doi: 10.3390/biomedicines6010008.
- Management of actinic keratosis in primary care; The Primary Care Dermatology Society (PCDS), updated April 2014
- Del Rosso JQ, Kircik L, Goldenberg G, et al; Comprehensive management of actinic keratoses: practical integration of available therapies with a review of a newer treatment approach. J Clin Aesthet Dermatol. 2014 Sep;7(9 Suppl S2-S12):S2-S12.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 11 Jul 2027
12 Jul 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free