Port-wine stain
Peer reviewed by Dr Krishna Vakharia, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 17 May 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Port-wine stain article more useful, or one of our other health articles.
In this article:
Continue reading below
What is port-wine stain?
Synonyms: PWS, naevus flammeus
This is the most common type of capillary malformation and is a congenital malformation of the superficial blood vessels of the dermis.
It is a deep pink or red patch present at birth and grows in size as the child grows. 0.3-5% of newborns are affected.1 There is an equal sex distribution.
The lesion may darken to purple as the child grows and persists throughout life. It can occur anywhere but most often occurs unilaterally on the face or neck. The lesion is flat; the overlying skin is normal. Later in life more papular lesions can occur within the patch. There are frequently emotional and social problems for the affected person because of the stigma of such a visible disfigurement.
Rarely, acquired forms can occur at any age after birth. The cause has not been elucidated but trauma, chronic ultraviolet (UV) exposure, hormonal influences, infections, solid brain tumour and various internal vascular disorders have been suggested as possible associations.2
Pathogenesis
The condition results from abnormal ectasia (dilation) of papillary dermal capillaries and post-capillary venules. Evidence suggests that a deficiency in perivascular nervous tissue results in reduction in vascular tone, leading to dilation. There appear to be two sub-types which differ in morphology. Type 1 (superficial, tortuous, dilated end-capillary loops in the superficial papillary dermis) appears to be more sensitive to laser therapy than type 2 (ectatic vessels in the superficial horizontal vascular plexus). There is evidence that vascular endothelial growth factor and its receptor may be involved in the pathogenesis.3
Distribution
Back to contentsThe head and neck are the most commonly affected sites (65%), although any part of the body can be affected. They are usually unilateral but occasionally bilateral.4
Continue reading below
What does port-wine stain look like? (Appearance)1
Back to contentsPort wine stain - adult
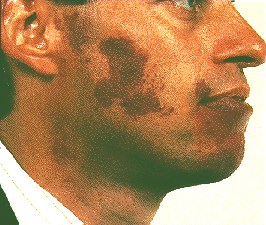
This lesion on the face is rather darker in an older person.
Port-wine stain - infant
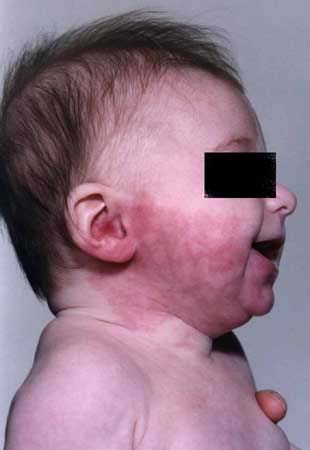
This is not so dark as the other lesions but may develop with time. It is in the distribution of the mandibular segment of the trigeminal nerve.
Natural history
The lesion remains present for life and has no tendency toward involution.
In early life, they are flat and usually clearly demarcated. The colour does not correlate with depth or diameter of capillaries. Blanching on pressure is variable. They are usually unilateral with a clear demarcation at the midline.
The lesions may change from pink in infancy to red in early adulthood to deep purple during middle age.
Nodular vascular lesions may develop, usually in adulthood.
Pyogenic granulomas with bleeding may develop, even in childhood.
Later in life, the vasculature dilates and the lesions may evolve into a raised, thickened plaque with a cobblestone contour. This may occur in up to 65% of facial lesions during adulthood.
Lobulated capillary haemangiomas (pyogenic granulomas) may form, especially with intra-oral lesions.
Differential diagnosis5
Back to contentsThe diagnosis of a port-wine stain is usually clear but there may be concern that it is not an isolated lesion but part of a syndrome (see 'Associated diseases', below). Other conditions to consider include:
Infantile haemangioma
Infantile haemangioma is a benign vascular neoplasm. Occasionally they may cause pressure effects on adjacent vital structures, ulcerate, bleed or cause high-output cardiac failure.
Proteus' syndrome6
This is a disorder in which irregular asymmetric overgrowth of multiple body tissues occur. Severe cases involve large areas of the body (the 'Elephant Man' is the most famous patient to have had this condition) but more localised forms can resemble capillary malformations.
Rubinstein-Taybi syndrome7
Rubenstein-Taybi syndrome is characterised by broad thumbs and big toes, short stature, general learning disability and capillary naevus of the forehead or nape in over 50% of patients.
Morphoea8
Localised morphoea may mimic an acquired port-wine stain.
Miscellaneous
Other conditions which may need to be considered depending on the clinical presentation include non-accidental injury, forceps injury, insect-bite reaction, telangiectatic haemangioma and unilateral nevoid telangiectasias.5
Continue reading below
Associated diseases
Back to contentsGlaucoma5
There is an association between port-wine stains involving the eyelids and glaucoma. Glaucoma may occur in about 10% of facial port-wine stains but the figure rises to between a quarter and a half when both the ophthalmic and maxillary divisions are involved.
Spinal abnormalities9
Neural tube defects and tethered spinal cord may be associated conditions. Lumbar skin changes such as acrochordons (skin tags), an abnormal tuft of hair (fawn's tail) and lipomas have been observed.
Sturge-Weber syndrome
Port-wine stain, in association with ocular intracranial angiomas, causes blindness, focal epilepsy, hemiplegia or general learning disability - Sturge-Weber syndrome.10 The lesion is clearly unilateral and in the trigeminal area, usually in the ophthalmic division. There are ipsilateral capillary malformations on the leptomeninges and cerebral cortex. The condition may be bilateral.
Cobb's syndrome
This includes cutaneomeningospinal angiomatosis. A lesion in the skin overlying the spine is associated with vascular malformations in the underlying spinal meninges. There may be pressure on the spinal cord or nerves, bone erosion and subarachnoid haemorrhage.
Klippel-Trénaunay syndrome
This is also known as angio-osteo-hypertrophy syndrome.11 Klippel-Trénaunay syndrome is an association of a port-wine stain, varicose veins and hypertrophy of a limb. The lower limbs are involved in 95% of patients and it is unilateral in 85%. Most babies are asymptomatic at birth but have problems later in childhood. Complications include:
Varicose veins with venous thrombosis and pulmonary embolism.
Bleeding from varices, the rectum, or the bladder.
Skin ulceration.
Increased sweating overlying the lesion.
Leg circumference or length discrepancy with resultant scoliosis.
Oedema and recurrent infections.
Parkes Weber's syndrome
Parkes Weber's syndrome consists of arteriovenous (AV) malformation in addition to those of the Klippel-Trénaunay syndrome. AV fistulae are usually diffuse and ablation is difficult. Most children present in childhood with an enlarged, warm extremity. The prognosis is worse than with Klippel-Trénaunay syndrome.
Wyburn-Mason's syndrome12
This is also called unilateral retinocephalic syndrome and also Bonnet-Dechaume-Blanc syndrome. There are facial port-wine stains with unilateral AV malformation of the retina and the intracranial optic nerves. Lesions may occur anywhere on the face and there may be facial hypertrophy or occasional involvement of the optic chiasm, the hypothalamus, the midbrain and the basal ganglia, with associated general learning disability or neurological features.
Investigations
Back to contentsIf Sturge-Weber syndrome is suspected, MRI scan of the brain is required. In very early life, results may give false reassurance.13
Photoacoustic imaging can be used to give information relating to the depth of the lesion and its vasculature.14 Cerebral angiography is also occasionally used.
Optical coherence tomography (a technique which acquires optical signals and can identify very small structures just under the surface of the skin) has been adopted for the diagnosis of port-wine stains.15
A number of other newly developed optical and scanning devices are becoming available.16
There is no consensus as to whether patients with isolated capillary malformations require imaging to exclude cerebrovascular abnormalities.
Regular ophthalmic checks to exclude glaucoma should be carried out in the first three years of life.
Management of port-wine stain
Back to contentsRefer as young as possible to a dermatology department with laser facilities. Early referral is recommended in view of the cosmetic impact and to rule out associated conditions such as Klippel-Trenaunay syndrome, Sturge-Weber syndrome and glaucoma.4
The tunable pulsed dye laser (PDL) emits light at 585 nm which is preferentially absorbed by haemoglobin.1
The length of the pulse of light (450 microseconds) is just long enough to heat small vessels but not the surrounding tissue. This results in destruction of the blood vessels without any scarring. The results are best in babies or infants.
Treatment is painful and, in small children, requires a general anaesthetic but small infants have smaller areas to be treated (before they have grown). Local anaesthetic is helpful.17
The treatment is tedious, time-consuming and expensive and may not be universally available without charge on the NHS.
Few patients achieve total clearance and some do not respond at all.
Several treatments may be required, spaced at 2-3 monthly intervals; postoperatively, patients are usually advised to avoid the sun, avoid injury and use an emollient.
One study recommended a 'double-pass' technique for patients with capillary malformations resistant to previous laser therapy.18
Another study reported that laser speckle imaging (a method of assessing the degree of scatter of laser beams after they have come into contact with tissue) after laser treatment showed areas of incomplete photocoagulation in some patients. The authors recommended immediate re-coagulation in these cases.19
Surgical excision with or without cosmetic reconstruction may be required for lesions resistant to laser therapy.20
Current research is looking at the added efficacy of PDL with topical imiquimod., exogenous heat or intravenous porphyrin derivatives.21
PDL laser is sometimes used in conjunction with a potassium titanyl phosphate (KTP) laser.1
Combined selective photothermolysis and imiquod is being explored as an effective option.21
Cosmetic camouflage can be useful in hiding the area. It may be prescribed on an FP10. Tattooing of the area with skin-coloured pigment is occasionally carried out.
Complications of port-wine stain
Back to contentsHyperpigmentation is usual in treated areas but this is transient. Permanent hypopigmentation may occur in treated areas. Pyogenic granuloma in treated areas has been described.22
It has been said that failure to treat can result in considerable psychological morbidity but this has been challenged and one study suggested that further research is required.23
Eczematous dermatitis similar to stasis dermatitis can occasionally develop. It is usually responsive to topical steroids or calcineurin inhibitors but often recurs once treatment is stopped.24
Prognosis25
Back to contentsThe lesion is permanent during life and in some may become a major cosmetic disability. Laser treatment can produce good results but complete clearance is rare. Research to develop treatments that will completely eradicate the lesion is ongoing.
Further reading and references
- Intralesional photocoagulation of subcutaneous congenital vascular disorders; NICE Interventional Procedures Guidance, 2004
- Chen D, Hu XJ, Lin XX, et al; Nodules arising within port-wine stains: a clinicopathologic study of 31 cases. Am J Dermatopathol. 2011 Apr;33(2):144-51.
- Laquer VT, Hevezi PA, Albrecht H, et al; Microarray analysis of port wine stains before and after pulsed dye laser treatment. Lasers Surg Med. 2013 Feb;45(2):67-75. doi: 10.1002/lsm.22087.
- Capillary vascular malformation; DermNet.
- Izikson L, Nelson JS, Anderson RR; Treatment of hypertrophic and resistant port wine stains with a 755 nm laser: a case series of 20 patients. Lasers Surg Med. 2009 Aug;41(6):427-32. doi: 10.1002/lsm.20793.
- Kulac M, Karaca S, Acar M, et al; Acquired port-wine stain related to acoustic neuroma. Clin Exp Dermatol. 2006 Jan;31(1):30-2.
- Vural E, Ramakrishnan J, Cetin N, et al; The expression of vascular endothelial growth factor and its receptors in port-wine stains. Otolaryngol Head Neck Surg. 2008 Oct;139(4):560-4. doi: 10.1016/j.otohns.2008.07.015.
- Port-wine stain; Primary Care Dermatology Society, 2022.
- Jackson S et al; Differential Diagnosis for the Dermatologist, 2012
- Hoeger PH, Martinez A, Maerker J, et al; Vascular anomalies in Proteus syndrome. Clin Exp Dermatol. 2004 May;29(3):222-30.
- Kumar S, Suthar R, Panigrahi I, et al; Rubinstein-Taybi syndrome: Clinical profile of 11 patients and review of literature. Indian J Hum Genet. 2012 May;18(2):161-6. doi: 10.4103/0971-6866.100751.
- Nijhawan RI, Bard S, Blyumin M, et al; Early localized morphea mimicking an acquired port-wine stain. J Am Acad Dermatol. 2011 Apr;64(4):779-82. Epub 2010 Sep 17.
- Sardana K, Gupta R, Garg VK, et al; A prospective study of cutaneous manifestations of spinal dysraphism from India. Pediatr Dermatol. 2009 Nov-Dec;26(6):688-95. doi: 10.1111/j.1525-1470.2009.01014.x.
- Sturge-Weber Syndrome, SWS; Online Mendelian Inheritance in Man (OMIM)
- Klippel-Trenaunay-Weber Syndrome; Online Mendelian Inheritance in Man (OMIM)
- D'Souza D; Wyburn-Mason syndrome, Radiopaedia.org, 2014
- Adams ME, Aylett SE, Squier W, et al; A spectrum of unusual neuroimaging findings in patients with suspected Sturge-Weber syndrome. AJNR Am J Neuroradiol. 2009 Feb;30(2):276-81. doi: 10.3174/ajnr.A1350. Epub 2008 Dec 2.
- Kolkman RG, Mulder MJ, Glade CP, et al; Photoacoustic imaging of port-wine stains. Lasers Surg Med. 2008 Mar;40(3):178-82.
- Zhao S, Gu Y, Xue P, et al; Imaging port wine stains by fiber optical coherence tomography. J Biomed Opt. 2010 May-Jun;15(3):036020.
- Sharif SA, Taydas E, Mazhar A, et al; Noninvasive clinical assessment of port-wine stain birthmarks using current and future optical imaging technology: a review. Br J Dermatol. 2012 Dec;167(6):1215-23. doi: 10.1111/j.1365-2133.2012.11139.x. Epub 2012 Oct 5.
- Mahendran R, Sheehan-Dare RA; Survey of the practices of laser users in the UK in the treatment of port wine stains. J Dermatolog Treat. 2004 Apr;15(2):112-7.
- Rajaratnam R, Laughlin SA, Dudley D; Pulsed dye laser double-pass treatment of patients with resistant capillary malformations. Lasers Med Sci. 2011 Apr 8.
- Huang YC, Tran N, Shumaker PR, et al; Blood flow dynamics after laser therapy of port wine stain birthmarks. Lasers Surg Med. 2009 Oct;41(8):563-71.
- Hu X, Jiang C, Lin X, et al; Reconstruction of the Cheek after Large Port-Wine Stain Lesion Resection. Aesthetic Plast Surg. 2011 Mar 18.
- Tremaine AM, Armstrong J, Huang YC, et al; Enhanced port-wine stain lightening achieved with combined treatment of selective photothermolysis and imiquimod. J Am Acad Dermatol. 2012 Apr;66(4):634-41. doi: 10.1016/j.jaad.2011.11.958. Epub 2012 Jan 14.
- Sheehan DJ, Lesher JL Jr; Pyogenic granuloma arising within a port-wine stain. Cutis. 2004 Mar;73(3):175-80.
- Hansen K, Kreiter CD, Rosenbaum M, et al; Long-term psychological impact and perceived efficacy of pulsed-dye laser therapy Dermatol Surg. 2003 Jan;29(1):49-55.
- Fonder MA, Mamelak AJ, Kazin RA, et al; Port-wine-stain-associated dermatitis: implications for cutaneous vascular laser therapy. Pediatr Dermatol. 2007 Jul-Aug;24(4):376-9.
- Klein A, Baumler W, Landthaler M, et al; Laser and IPL treatment of port-wine stains: therapy options, limitations, and practical aspects. Lasers Med Sci. 2011 Mar 10.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 15 May 2028
17 May 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free