Vasectomy
Male sterilisation
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 19 May 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:SterilisationFemale sterilisation
Vasectomy is a a form of birth control where a man undergoes a small operation to cut the end of the vas deferens tube. This is the tube that takes sperm from the testicles (testes) to the penis. Sperm are made in the testes. Once the vas deferens is cut, sperm can no longer get into the semen that comes out (is ejaculated) during sexual intercourse.
Vasectomy is very reliable - but not quite 100%. Even after a successful operation about 1 in 2,500 men who have had a vasectomy will become fertile again at some point in the future. This is because, rarely, the two ends of the cut vas deferens re-unite over time.
In this article:
Video picks for Other surgery and procedures
What is a vasectomy?
Continue reading below
What does a vasectomy do?
A vasectomy prevents sperm from being ejaculated during sex. Semen continues to be ejaculated as normal but no longer contains sperm. This means that pregnancy cannot occur as sperm cannot reach the woman's womb (uterus).
Types of vasectomy
Conventional vasectomy (scalpel vasectomy).
Non-scalpel vasectomy.
How does a vasectomy work?
Back to contentsCross-section of male reproductive organs, showing vasectomy procedure
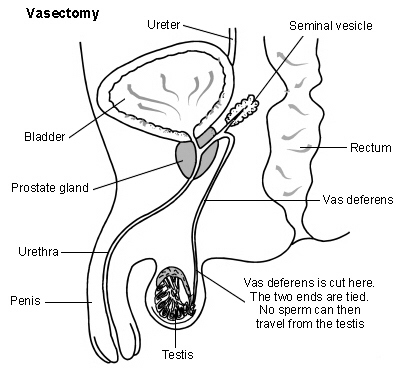
Vasectomy is usually done under a local anaesthetic. The person having the vasectomy is awake but has an injection into the skin to make the area numb so that they do not feel pain. Local anaesthetic is injected into a small area of skin on either side of the scrotum above the testicles (testes).
A tiny cut or puncture hole is made in the numbed skin on each side of the scrotum. The vas deferens can be seen quite easily under the cut skin. It can be cut with a surgical knife (scalpel) or using diathermy. Diathermy is electrical current that cuts and seals the ends of the tubes. It stops the bleeding at the same time. Sometimes a small piece of the vas deferens is removed.
The hole is so small that often no stitches are needed. If stitches are required, either dissolvable stitches or a special surgical tape are used. The operation takes about 15 minutes.
There is usually some discomfort and bruising for a few days afterwards which normally goes away quickly. The discomfort can be helped by wearing tight-fitting underpants day and night for a week or so after the operation. It is also best not to do heavy lifting or strenuous exercise for four weeks or so after the operation.
Continue reading below
Vasectomy risks
Back to contentsMost men have no problems after a vasectomy. Problems are uncommon but include the following:
As with any operation or cut to the skin, there is a small risk of a wound infection.
The bruising around the operation site is sometimes quite noticeable. However, it will go in a week or so.
Rarely, sperm may leak into the scrotum and form a swelling which may need treatment.
A small number of men have a dull ache in the scrotum for a few weeks or months after the operation. This usually settles within three months.
A very small number of men develop a post-vasectomy pain which does not settle over time. This can be mild or severe. It may be in the scrotum, the penis, the testicles (testes) or the lower tummy. The most recent studies show that this only occurs in 0.2% of men.
How do I know it has been successful?
Back to contentsSome sperm survive in the upstream part of the vas deferens for several weeks after vasectomy. These can get into the semen for a while after the operation. About twelve weeks after the operation a semen test will be requested which will be looked at under the microscope to check for sperm.
If there are no sperm in this sample, the vasectomy has been successful. If there are sperm present, another test will be performed a month later. Until it has been confirmed that there are no sperm in the sample another method of contraception must be used to prevent pregnancy.
Continue reading below
What are the advantages of vasectomy?
Back to contentsIt is permanent, therefore reducing the risk of unplanned pregnancies. It is easier to do and more effective than female sterilisation.
What are the disadvantages of vasectomy?
Back to contentsIt may take a few months before the semen is free from sperm. As it is permanent, some people regret having a vasectomy, especially if their circumstances change. Vasectomy does not protect from sexually transmitted infections.
Does a vasectomy affect sex drive?
Back to contentsNo. The sex hormones made by the testicles (testes) - for example, testosterone - continue to be passed into the bloodstream as before so are not affected by a vasectomy. Also, vasectomy does not reduce the amount of semen ejaculated during sex. Sperm only contribute a tiny amount to semen. Semen is made in the seminal vesicles and prostate higher upstream.
Sex may even be more enjoyable, as the worry or inconvenience of other forms of contraception is removed.
What happens to the sperm?
Back to contentsSperm are still made as before in the testicles (testes). The sperm cannot get past the blocked vas deferens and are absorbed by the body.
Is a vasectomy reversible?
Back to contentsIt is very important only to consider a vasectomy when you are certain that you (and any partner) do not want children or further children.. It is important to consider all sorts of situations, including a tragedy in the family or a break-up of the relationship. A vasectomy should only be considered where there is certainty that you would not want more children even in those situations.
It is wise not to make the decision at times of crisis or change, such as after a new baby or termination of pregnancy. It is best not to make the decision if there are any major problems in the relationship with your partner.
Remember there are reversible forms of long-term contraception which are very effective. Consider these as a couple before making your decision. These are all for women. See the separate leaflet called Long-acting Reversible Contraceptives (LARCs).
Ideally, both partners are happy with the decision before a vasectomy. However, it is not legally necessary to obtain your partner's permission.
Vasectomies are considered permanent and reversal is never offered on the NHS. Private providers will offer vasectomy reversal and the success rates of this are quoted as:
75% will achieve pregnancy if the reversal is done within 3 years of the vasectomy.
50-55% if it has been 3 - 8 years since the vasectomy.
40-45% if it has been 9-14 years since the vasectomy.
30% if it has been 15-19 years since the vasectomy.
Less than 10% if it has been more than 20 years since the vasectomy.
Some common questions about vasectomy
Back to contentsIs vasectomy done on the NHS? Yes - most men have a vasectomy done on the NHS. However, waiting lists may vary throughout the country. Some men prefer to have it done at a private clinic or hospital.
Does the operation hurt? No more than any other minor operation that uses local anaesthetic. The injection of local anaesthetic may sting a bit for a few seconds. It is put in just a small area of skin. After this, the operation is usually painless. After the operation, when the local anaesthetic wears off, the top part of the scrotum is normally mildly sore for a few days.
What if I change my mind? Vasectomy is considered permanent. There is an operation to re-unite the two cut ends of the vas deferens. It is a difficult operation and not always successful. It is also never available on the NHS, so needs to be paid for privately.
How soon after the operation can I have sex? It is recommended to abstain from sex for between 2 to 7 days after the vasectomy. However, other methods of contraception will need to be used until the semen specimen has been confirmed as clear of sperm. Some sperm will survive upstream from the cut vas deferens for a few weeks.
I have heard that there is an increase in the risk of prostate cancer after vasectomy. Is this true? In 2017, a rigorous review of 53 studies and 15 million patients suggested no increased risk of prostate cancer following a vasectomy. In 2021, a similar review of 17 million patients suggested a small but significant increased risk of diagnosis of prostate cancer in men who had had a vasectomy but no increased risk of death from prostate cancer. The increased risk was found to be from 16 in 1000 to 19 in 1000. It is not clear why this possible increased risk exists - it is thought that it is possible that men who choose to have a vasectomy are more aware of their health and are more likely to request tests or screening for prostate cancer.
Patient picks for Other surgery and procedures

Surgery and procedures
Surgical drains
A surgical drain is a small plastic tube that is sometimes used after an operation. It is put inside you during the surgery by the doctor and will stick out of your body until it is removed, usually a few days later. It connects to a small plastic bag that collects any fluid or air that has drained away from where you had the operation. Not all operations require a drain to be in: your surgeon will advise you if one is necessary.
by Dr Rachel Hudson, MRCGP

Surgery and procedures
Kidney transplant
Although there are now many successful drugs and treatments to treat kidney disease, when kidney failure occurs, a kidney transplant is the best treatment, associated with the best long-term outcomes. A healthy kidney may be transplanted from a living donor or may be taken from a donor as soon as possible after they have died.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Dohle GR, Diemer T, Kopa Z, et al; European Association of Urology guidelines on vasectomy. Eur Urol. 2012 Jan;61(1):159-63. doi: 10.1016/j.eururo.2011.10.001. Epub 2011 Oct 19.
- Male and female sterilisation; Faculty of Sexual and Reproductive Healthcare (September 2014)
- Patel AP, Smith RP; Vasectomy reversal: a clinical update. Asian J Androl. 2016 May-Jun;18(3):365-71. doi: 10.4103/1008-682X.175091.
- UK Study on Vasectomy Safety; European Association of Urologists
- Vasectomy Reversal; Raj Persad
- Can there be consensus on whether vasectomy is a prostate cancer risk factor?; Minhaj Siddiqui
- Tim Jewell; Vasectomy and Prostate Cancer
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
19 May 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.