Drug allergy
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Hayley Willacy, FRCGP Last updated 20 Nov 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:AllergiesAnaphylaxisAngio-oedemaHouse dust mite and pet allergySkin prick allergy testAntihistamines
Medicines can cause allergic reactions. In this leaflet these reactions are called 'drug allergies'. In this instance the drugs referred to are medicines people take for their health. For example, antibiotics or anti-inflammatory painkillers rather than drugs of addiction.
Allergic reactions can happen with prescribed medicines as well as those you have bought from a pharmacy. Drug allergies may be mild, moderate or severe. Some can come on in a matter of minutes. Others may take days or even weeks to develop. Some reactions are so severe they can be life-threatening. Mild reactions can sometimes be treated simply by stopping the medicine. Severe reactions usually require hospital admission.

Unsure about mixing medicines?
Check for possible interactions between medicines, supplements and foods before taking them together.
In this article:
Video picks for Other allergies
Continue reading below
What is a drug allergy?
An allergy is a response of the body's immune system to something called an allergen. In the case of drug allergy the allergen is a medication.
Most reactions that do not involve the immune system are side-effects rather than true drug allergies. The most common drug allergies are caused by anti-inflammatory painkillers - also called non-steroidal anti-inflammatory drugs (NSAIDs) - and by antibiotic medication.
About 1 in 10 people with asthma become wheezy when they take NSAIDs.
How common are drug allergies?
Back to contentsTests on people who report drug allergies show that only a few have a true allergy. One study confirmed true allergy in only 1 in 10 people who thought they had an allergy to penicillin type medication.
Often they had a rash in childhood at the same time as taking penicillin and just assumed that the medicine was the cause.
Drug allergies do, however, seem to be on the increase. About 15% of people in the UK admitted to hospital have their stay extended because of an allergic drug reaction.
Continue reading below
What are the symptoms of a drug allergy?
Back to contentsMild reactions
In a mild reaction you may develop itchy eyes or a runny nose. All sorts of skin rashes are possible. These include:
Acneform lesions - acne spots on the upper part of the body.
Acute generalised exanthematous pustulosis (AGEP) - the skin becomes red and is covered with small boils. You may develop a high temperature (fever).
Bullous pemphigoid - the skin is covered with blisters filled with clear fluid.
Erythema nodosum - red rounded lumps (nodules), which are tender, form just below the skin's surface. They commonly occur on the shins.
Erythroderma - this causes general redness of the skin.
Fixed drug eruption - this is a rash which comes up on the same area of the skin (hence 'fixed') whenever the same drug is given. The rash can take various forms but commonly looks like measles or larger red blotches on the skin. It frequently occurs on the hands, feet or genitals.
Drug Reaction
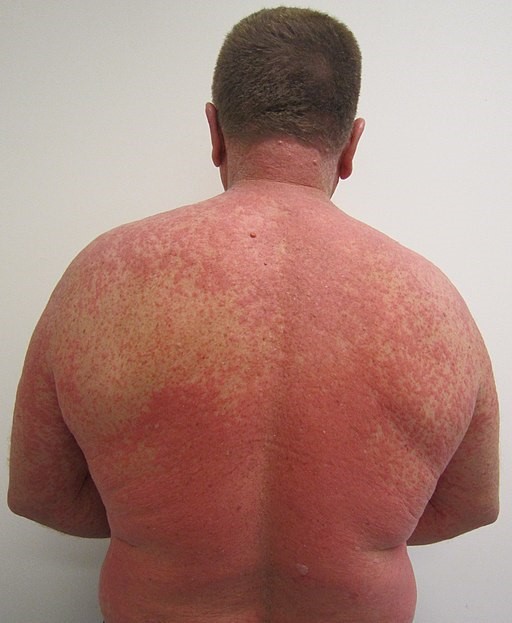
© James Heilman, MD, CC BY-SA 4.0, via Wikimedia Commons
Hypersensitivity syndromes - this is also known as 'drug reaction with eosinophilia and systemic signs' (DRESS). The skin rash is accompanied by other features such as fever, swollen glands and a rise in the number of white cells in the blood, called eosinophils. The rash is made of small, itchy red bumps (papules) commonly seen on the face, arms, legs and trunk.
Lichenoid reactions - this is so called because it looks like a condition called lichen planus. The rash is made of small, red-purple bumps. The bumps are usually shiny and flat-topped (planus means flat). They vary in size from a pinhead to about 1 cm across. The number of flat-topped bumps that develop varies. The rash can appear anywhere on the body but is most likely to occur on the inner wrists, lower legs and lower back.
Lupus drug reactions - this may cause small purple spots like bruises (purpura) on the skin, with or without erythema nodosum.
Photosensitivity - some medicines make the skin more sensitive to sunburn.
Urticaria - this takes the form of itchy raised weals (also known as 'hives') on the skin. formed by tiny amounts of fluid that leak from blood vessels just under the skin's surface.
Vasculitis - this means inflammation of the blood vessels. It can take various forms but nearly always affects the skin of the legs. Bruises of various sizes, ulcers and patches of redness are common findings.
Severe reactions
Most allergies are mild and clear up once the medicine is stopped. However, severe reactions can occasionally occur.
Anaphylaxis is an extreme form of allergic reaction. It can cause:
Swelling of the lips and tongue.
Trouble breathing.
Collapse.
Loss of consciousness.
For further information, see separate leaflets called Anaphylaxis and Dealing with an Allergic Reaction.
Two severe reactions which can develop are called Stevens-Johnson syndrome and toxic epidermal necrolysis. Whilst there are some differences in the features of these two conditions, toxic epidermal necrolysis can be considered a more widespread form of Stevens-Johnson syndrome.
The first symptoms may include:
Fever.
Sore throat.
Joint pains.
Itching.
Sickness.
Diarrhoea.
Soreness of the eyes, the inside of the mouth, the throat, the nostrils and the genitals.
Difficulty eating and drinking.
Burning sensation when you pass urine.
Rash.
A rash develops, usually on the face or trunk, which spreads to large areas of the body. It starts with flat red spots, which turn into raised bumps.
If you have Stevens-Johnson syndrome you might notice some spots develop small blisters in the centre to give the typical appearance of 'target lesions'. Blisters can run together to form large fluid-filled areas known as bullae.
In toxic dermatolysis, blistering can become very severe and lead to large areas of skin peeling off.
What causes a drug allergy?
Back to contentsAn allergy is the response produced by the body's immune system to an allergen. The body recognises that something that does not come from itself and attacks it (even though it is usually harmless). It is actually a defence mechanism but the response may be more of a problem than the substance that caused it. An allergen can be caused by many things, such as pollen (which causes hay fever). In this case. the allergen is drugs - medication. This can be prescribed medicines, or those bought over the counter.
The mechanism of action is either through a Type 1 IgE-mediated (a type of immunoglobulin) hypersensitivity, or through a Type 4 T-cell (a type of white blood cell) mediated reaction.
Continue reading below
What drugs are commonly linked to allergies?
Back to contentsAspirin or non-steroidal anti-inflammatory medicines.
Penicillin type antibiotics.
Anaesthetics.
Vaccines.
Substances injected when having some types of x-ray procedures.
It is important to distinguish a side-effect to a medication from a true allergy. Sometimes the symptoms may be similar.
How is drug allergy diagnosed?
Back to contentsIt is usually easy to make the link between the offending medicine and the resulting reaction. If the symptoms clear up when the medicine is stopped this is often enough to confirm a drug allergy.
However, if the reaction is severe, you may need blood and urine tests to check that your liver, kidneys and other bodily functions are working properly. A chest X-ray may be required if your lungs are involved.
If it is not certain that your symptoms are due to a particular medicine, you may need to be given a small amount of the drug, either by mouth, injection or as a skin patch. Then your reactions are monitored under medical supervision.
How is drug allergy treated?
Back to contentsIn most cases, stopping the medicine is enough. Sometimes, complications may require treatment such as steroid or antihistamine tablets.
If you have a drug allergy it is important to carry a card, a medical emergency identification bracelet or equivalent, or a letter from your doctor giving details of the allergy.
Does drug allergy get better?
Back to contentsMost people with drug allergy recover very quickly once the medication is stopped, although the rash can take 10-14 days to fade. People with severe reactions may take a long time to get better, especially if they are elderly or have other medical conditions.
Toxic epidermal necrolysis can be life-threatening in up to half the cases. The less severe Stevens-Johnson syndrome can still be life-threatening for about a tenth of people developing the condition.
Patient picks for Other allergies

Allergies, blood and immune system
Contact dermatitis
Contact dermatitis is a rash caused by your skin reacting to a substance it has come into contact with. You may need patch testing to identify the causative substance. A steroid cream or ointment will usually clear the rash. However, the long-term treatment is to avoid contact with the thing that's causing it.
by Dr Hayley Willacy, FRCGP

Allergies, blood and immune system
House dust mite and pet allergy
House dust mite and pet allergies occur because of a reaction to tiny airborne particles within the home. Symptoms can include a runny or blocked nose, itchy, red or watering eyes and wheezing. If you have asthma, your asthma symptoms can also be made worse by these allergies. Regular use of long term medication can improve symptoms but avoidance of the cause can also be important, especially with pet allergies.
by Dr Colin Tidy, MRCGP

Unsure about mixing medicines?
Check for possible interactions between medicines, supplements and foods before taking them together.
Further reading and references
- Drug allergy: diagnosis and management of drug allergy in adults children and young people; NICE Clinical guideline (September 2014; updated November 2018).
- Allergy UK
- BSACI Guidelines/Standards of Care; British Society for Allergy & Clinical Immunology
- Patterson RA, Stankewicz HA; Penicillin Allergy.
Continue reading below
About the author

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 18 Nov 2028
20 Nov 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.