Lower back pain
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Rachel Hudson, MRCGPLast updated 9 Oct 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
In this series:Back and spine painSlipped discSpinal stenosisCauda equina syndromeThoracic back painBack pain in children
About 8 in 10 people have one or more bouts of lower back pain. In most cases, it is not due to a serious disease or serious back problem, and the exact cause of the pain is not clear. This is called nonspecific lower back pain. The usual advice is to keep active and do normal activities as much as possible.
Painkillers can help until the pain eases. In most cases, the pain disappears within six weeks but may come back (recur) from time to time. Persistent (chronic) pain develops in some cases and further treatment may then be needed.
In this article:
Video picks for Back pain
Continue reading below
Understanding the lower back
The lower back is also called the lumbosacral area of the back. It is the part of the back between the bottom of the ribs and the top of the legs.
Most of the lower back is made up from muscles that attach to, and surround, the spine. The spine is made up of many bones called vertebrae. The vertebrae are roughly cylindrical and between each vertebra is a disc. The discs between the vertebrae are a combination of a strong fibrous outer layer and a softer, gel-like centre. The discs act as shock absorbers and allow the spine to be flexible.
Close-up view
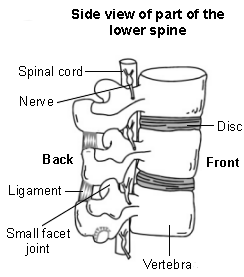
Strong ligaments also attach to nearby (adjacent) vertebrae to give extra support and strength to the spine. The various muscles that are attached to the spine enable the spine to bend and move in various ways.
The spinal cord, which contains the nerve pathways to and from the brain, is protected by the spine. Nerves from the spinal cord come out from between the vertebrae to take and receive messages to various parts of the body.
Lower back pain causes
Back to contentsCommon causes of lower back pain include:
Nonspecific lower back pain.
Nerve root pain (sciatica).
Cauda equina syndrome.
Arthritis.
Nonspecific lower back pain
This is the most common cause of back pain. The majority of cases of sudden-onset (acute) lower back pain are classed as nonspecific. This is the type of back pain that most people will have at some point in their lives.
Nonspecific lower back pain means that the pain is not due to any specific or underlying disease that can be found. It is thought that in some cases the cause may be:
An over-stretch (sprain or strain) of a ligament or muscle.
A minor problem with a disc between two spinal bones (vertebrae).
A minor problem with a small facet joint between two vertebrae.
There may be other minor problems in the structures and tissues of the lower back that result in pain. However, these causes of the pain are impossible to prove by tests. Therefore, it is usually impossible for a clinician to say exactly where the pain is coming from or exactly what is causing the pain - it is usually attributed to the muscles.
To some people, not knowing the exact cause of the pain is unsettling. However, it can be reassuring to know that the diagnosis is nonspecific back pain which means there is no serious problem or disease of the back or spine.
Nerve root pain (sciatica)
This occurs in less than one case in 20 of acute lower back pain. Nerve root pain means that a nerve coming out from the spinal cord (the root of the nerve) is irritated or pressed on. (Many people call this a trapped nerve.)
Pain is felt along the course of the nerve. Therefore, pain is typically felt down a leg, sometimes as far as to the calf or foot. The pain in the leg or foot is often worse than the pain in the back. The irritation or pressure on the nerve may also cause pins and needles, numbness, tingling, or weakness in part of a buttock, leg or foot.
About nine in ten cases of nerve root back pain are due to a herniated/prolapsed disc - often called a slipped disc. (A disc does not actually slip. What happens is that part of the inner softer part of the disc bulges out (prolapses or herniates) through a weakness in the outer harder part of the disc). The prolapsed part of the disc can press on a nerve nearby.
See the separate leaflet called Slipped disc for details. Other less common conditions can cause pressure on a nerve to cause nerve root pain.
What is sciatica?
Cauda equina syndrome
Cauda equina syndrome is a particularly serious type of nerve root problem. This is a rare disorder where the nerves at the very bottom of the spinal cord are pressed on. This syndrome can cause lower back pain plus problems with bowel and bladder function (usually inability to pass urine), numbness in the saddle area (around the genitals and back passage (anus)) and weakness in one or both legs.
This syndrome needs urgent treatment to prevent the nerves to the bladder and bowel from becoming permanently damaged. Medical advice should be sought immediately if cauda equina syndrome is suspected - this should usually be in an emergency department as urgent scans would be required.
Less common causes of lower back pain
Osteoarthritis is the most common form of arthritis and usually occurs in older people.
Ankylosing spondylitis is another form of arthritis that can occur in young adults and which causes pain and stiffness in the lower back.
Rheumatoid arthritis may affect the spine but other joints are usually affected too.
Various uncommon bone disorders.
Narrowing of part of the lumbar spine, causing a condition called "spinal stenosis" where the nerve is trapped in the narrower section.
Tumours.
Infection.
Pressure from structures near to the spine (fewer than one in 100 cases of lower back pain).
The rest of this leaflet is mainly about nonspecific lower back pain - the common type of lower back pain.
Continue reading below
Symptoms of lower back pain
Back to contentsPain immediately after lifting something heavy.
Pain after an awkward twisting movement.
Pain that spreads from the lower back area to one or both buttocks or thighs.
Pain that is usually eased by lying down flat.
Pain when on moving the back, coughing, or sneezing.
Sometimes it can develop for no apparent reason. Some people just wake up one day with lower back pain.
Most people with a bout of nonspecific lower back pain improve quickly, usually within a week or two. However, once the pain has eased or gone it is common to have further bouts (recurrences) of pain from time to time in the future.
Also, it is common to have minor pains on and off for quite some time after an initial bad bout of pain. In a small number of cases the pain persists for several months or longer. This is called chronic back pain (discussed in more detail later).
See the separate article called When to worry about back pain.
Diagnosing lower back pain
Back to contentsMost people who develop lower back pain that comes on suddenly (acutely) have nonspecific lower back pain. If there are no other associated symptoms and the pain is not too bad, many people are confident to just 'get on with it' and treat it themselves, and indeed most get better quickly. However, if the pain is not settling or if there are other concerning features, medical advice should be sought.
A clinician will usually want to ask questions about the symptoms and to perform an examination.
As a general guide, if any of the following occur then there may be a more serious underlying cause. But note: the vast majority of people with lower back pain do not have any of the following symptoms or features. They are included here for completeness and as an aid to what to look out for.
Pain that develops gradually and slowly gets worse and worse over days or weeks.
Constant back pain that is not eased by lying down or resting.
Pain that travels to the chest, or is higher in the back behind the chest.
Weakness of any muscles in a leg or foot.
Lack of feeling (numbness) in any part of the bottom or leg.
Having taken steroid tablets without bone protection for more than a few months.
Symptoms that may indicate an inflammatory (arthritic) cause such as ankylosing spondylitis. The main ones are:
Pain which is worse in the second half of the night or after waking.
Stiffness, in addition to pain, of the back muscles in the morning after getting up from bed that lasts for more than 30 minutes.
The pain is eased (and not made worse) by activity.
Symptoms that may indicate cauda equina syndrome. The main ones are, in addition to back pain:
Numbness around the back passage (anus) - the saddle area.
Bladder symptoms such as loss of bladder sensation; loss of bladder control, incontinence, loss of sensation when passing urine.
Incontinence of stools (faeces).
Symptoms that may indicate a fracture in the spine:
Back pain following major trauma such as a road accident or fall from a height.
Back pain following minor trauma in people with 'thinning' of the bones (osteoporosis).
Symptoms that may indicate infection or spread of cancer affecting the spine.
Onset of pain in a person aged over 50 years, or under 20 years.
Pain that remains when lying down; night-time pain disturbing sleep.
Symptoms or problems in addition to pain such as:
Having or having had a cancer of any part of the body.
General symptoms, such as high temperature (fever), unexplained weight loss, etc.
Injecting street drugs.
Having a poor immune system, for example, being on chemotherapy.
Continue reading below
Are tests needed for lower back pain?
Back to contentsUsually not. A clinician will usually be able to diagnose nonspecific lower back pain from the description of the pain and by an examination. Therefore, in most cases, no tests are needed.
Current UK guidelines are clear that routine tests such as X-rays and scans should not be done if the diagnosis is made of nonspecific lower back pain.
Tests such as X-rays, MRI scans or blood tests may be advised in certain situations. This is mainly if there are symptoms, or signs during an examination, to suggest that there may be a serious underlying cause for the back pain.
Treatment for lower back pain
Back to contentsThe following advice and treatment are commonly given for a sudden-onset (acute) bout of nonspecific lower back pain.
Keeping active
It is best to continue with normal activities as much as possible. This may not be possible at first if the pain is very bad. However, it is important to move around as soon as possible, and get back into normal activities.
As a rule, it is best to avoid activities that cause a lot of pain. However, some discomfort when trying to keep active is usual. Avoiding exercise and activities tends to mean the back pain takes longer to resolve and leads to weakening of muscles which makes future bouts of back pain more likely.
Exercises and stretches for lower back pain are very helpful and effective. Physiotherapist-designed exercises for lower back pain can be done at home and can help faster recovery; keeping them up regularly can strengthen the muscles of the lower back, reducing the chance of back pain returning.
In the past, the advice had been to rest until the pain eases. It is now known that this was incorrect advice. The evidence from research trials is that faster recovery is more likely to be achieved by getting moving again and by getting back to work as soon as possible. Persistent (chronic) back pain is less likely to develop by keeping active during back pain rather than resting.
Medication
If painkillers are needed, it is best to take them regularly. The pain is then more likely to be eased for more of the time, enabling exercise and normal activity.
Over the counter painkillers (paracetamol and ibuprofen tablets or gel) are often very effective and should be tried first, but stronger painkillers can be prescribed if they are not helping.
Anti-inflammatory painkillers. They include ibuprofen and naproxen which may be prescribed , but is also available to buy over the counter, without a prescription. Diclofenac is no longer recommended. Some people may not be able to take anti-inflammatories, for example, some people with kidney failure or heart failure. Anti-inflammatory medicine should only be used at the lowest effective dose and for the shortest possible time.
A stronger painkiller such as codeine is an option for a short time if anti-inflammatories do not suit or do not work well. This may be taken as co-codamol, which is codeine with paracetamol. Constipation is a common side-effect from codeine. This may make back pain worse if straining to go to the toilet. To prevent constipation, it is important to have lots to drink and to eat foods with plenty of fibre. Codeine can be addictive if taken for more than a few days so should be taken for the shortest time possible.
Muscle relaxants such as diazepam used to be prescribed occasionally for muscle spasms associated with lower back pain, however these are no longer recommended.
See the separate article called How to relieve sciatica pain.
Other treatments
Heat such as a hot bath may help to ease pain.
It is best to sleep in the most naturally comfortable position on whatever is the most comfortable surface. Advice given in the past used to be to sleep on a firm mattress. However, there is no evidence to say that a firm mattress is better than any other type of mattress for people with lower back pain. Some people find that a small firm pillow between the knees when sleeping on the side helps to ease symptoms at night.
It is important to aim to get back to work as soon as possible. There is no need to wait for complete freedom from pain before returning to work. Returning to work often helps to relieve pain by getting back to a normal pattern of activity and providing a distraction from the pain.
Treatment may vary and the situation should be reviewed by a clinician if the pain becomes worse, or if the pain persists beyond 4-6 weeks, or if symptoms change. Other pain-relieving techniques may be tried if the pain becomes chronic.
Preventing lower back pain
Back to contentsEvidence suggests that the best way to prevent bouts of lower back pain is simply to keep active and to exercise regularly. This means general physical activity such as walking, running, swimming, etc.
There is no firm evidence to say that any particular back strengthening exercises are more useful to prevent back pain than simply keeping fit and active. It is also sensible to be back-aware, for example, not lifting objects when in an awkward twisting posture.
Maintaining a healthy weight is also important to reduce stress on the muscles of the lower back.
How common is lower back pain?
Back to contentsMost people (about six in ten people) will have a bout of nonspecific lower back pain at some point.
Persistent (chronic) lower back pain
Back to contentsNonspecific lower back pain is classed as chronic if it lasts for longer than six weeks. In some people it lasts for months, or even years. Symptoms may be constant. However, the more usual pattern is one in which symptoms follow an irregular course. That is, reasonably long periods of mild or moderate pain may be interrupted by bouts of more severe pain.
What is the treatment for chronic nonspecific lower back pain
Initial treatment is similar to sudden-onset (acute) attacks, aiming to keep as active as possible. Also, painkillers can help when needed. Other types of medicines including tricyclic antidepressants (amitriptyline) and gabapentinoids (gabapentin and pregabalin) used to be suggested for chronic back pain, but these are no longer recommended.
A national guideline (from the National Institute for Health and Care Excellence (NICE), referenced below) recommends one or more of the following treatments should be considered. Each of these treatments has some evidence from research trials to suggest that they will help to ease symptoms in some people (but not all):
Structured exercise programme. This means a programme of exercise supervised by a professional such as a physiotherapist. This is likely to be in a group setting. Exercises may include aerobic activity, movement instruction, muscle strengthening, posture control and stretching. It typically consists of up to eight supervised sessions over 8-12 weeks with encouragement to keep on doing the exercises at home between sessions.
A course of acupuncture. It is not clear how this may work. (Some doctors feel that this is a controversial recommendation as the evidence for effectiveness is weak.)
Cognitive behavioural therapy (CBT) may also be recommended as a treatment option. There is good evidence from research trials that it can help. CBT aims to help change the way that people think, feel and behave. It is used as a treatment for various health problems, including various types of chronic pain.
If the above treatments have not helped much then a referral to a specialist pain clinic might be advised. Sometimes nerve root injections or facet joint injections are suggested, depending on the findings in the pain clinic.
Lower back pain in pregnancy
Back to contentsLower back ache or pain is common in pregnancy, especially in the second and third trimesters. Not all painkillers (other than paracetamol) are safe to take in pregnancy so check with your pharmacist first. Modified stretches and exercises can be done and you can usually be referred to a physiotherapist more quickly if you are pregnant. You may need to rest more.
Patient picks for Back pain

Bones, joints and muscles
Ankylosing spondylitis
Ankylosing spondylitis is a chronic inflammatory arthritis. It mainly affects the lower back but can affect the rest of the spine. Other joints and other parts of the body are sometimes affected. There is no cure but treatments help with managing symptoms.
by Dr Philippa Vincent, MRCGP

Bones, joints and muscles
Slipped disc
A slipped disc is an old-fashioned term and does not truly describe what happens in this condition. It is more common to refer to it as a "disc prolapse", "disc herniation" or "disc bulge". There is further discussion below about these terms. However this leaflet will continue to use the term "slipped disc" due to its common usage. A slipped disc often causes sudden severe lower back pain. The disc often puts pressure on a nerve root which causes pain down one leg. Usually the symptoms gradually ease over several weeks. It is best to try and continue with normal activities as much as possible, using painkillers to help. Physical treatments such as spinal manipulation may also help. Surgery may be an option if the symptoms persist.
by Dr Philippa Vincent, MRCGP
Further reading and references
- Back pain - low (without radiculopathy); NICE CKS, September 2023 (UK access only)
- Low back pain and sciatica in over 16s: assessment and management; NICE Guidelines (November 2016 - last updated December 2020)
- Sciatica (lumbar radiculopathy); NICE CKS, September 2023 (UK access only)
- Mauck MC, Aylward AF, Barton CE, et al; Evidence-based interventions to treat chronic low back pain: treatment selection for a personalized medicine approach. Pain Rep. 2022 Sep 30;7(5):e1019. doi: 10.1097/PR9.0000000000001019. eCollection 2022 Sep-Oct.
- Back pain in pregnancy NHS website page
Continue reading below
About the author

Dr Rachel Hudson, MRCGP
General Practitioner and Medical Author
MBChB, MRCGP (2008), BSc (Medical Science), DFSRH, DRCOG, DCH
Dr Rachel Hudson, is an NHS GP working in the North West of England.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 8 Oct 2027
9 Oct 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.