Ankylosing spondylitis
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 20 Jan 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Ankylosing spondylitis is a chronic inflammatory arthritis. It mainly affects the lower back but can affect the rest of the spine. Other joints and other parts of the body are sometimes affected.
There is no cure but treatments help with managing symptoms.
At a glance
Ankylosing spondylitis (AS) is a long-term inflammatory condition mainly affecting the spine and pelvis.
It causes inflammation where ligaments join the spine, which can lead to bones fusing together over time.
Common symptoms include back pain and stiffness, especially in the mornings, which usually ease with movement.
Other joints and areas like the eyes or tendons can also be affected.
AS often develops between ages 20 and 30 and is more common in men.
Treatment aims to ease pain, maintain spinal flexibility through exercise and physiotherapy, and slow disease progression.
Medications like anti-inflammatory painkillers and biological therapies are used to manage symptoms and reduce inflammation.
In this article:
Video picks for Back pain
Continue reading below
What is ankylosing spondylitis?
Ankylosing spondylitis (AS) is a persistent (chronic) inflammatory arthritic disease. The word ankylosing means joining together or fusing. The word spondylitis means inflammation of the spine.
It mainly affects the spine and the joints that connect the bottom of the spine with the pelvis (sacroiliac joints). Other joints in other parts of the body may be affected. The type of inflammation in AS causes the affected joints to join together, therefore reducing mobility.
Ankylosing spondylitis is an auto-immune disease. It is not known exactly why ankylosing spondylitis occurs but there is a genetic predisposition. 6 out of 100 people who have a particular gene variant called HLA-B27 have ankylosing spondylitis whereas it is thought that it affects fewer than 1 in 100 people who do not have this protein.
Ankylosing spondylitis is a type of axial spondyloarthritis. See the separate leaflet called Axial spondyloarthritis for more information.
The lower back is typically the main site of inflammation
In ankylosing spondylitis (AS), the ligaments of the lower spine become inflamed at the points where they attach to the spinal bones (vertebrae). This gradually encourages the bone-making cells to grow bone within the ligaments. In time, these bony growths may become larger and form bony bridges between vertebrae that are next to each other. Eventually this can fuse some of the vertebrae together so that they effectively form one larger bone.
The sacroiliac joints and their nearby ligaments are also commonly affected. This inflammation too can ultimately end in fusion between the sacrum and pelvis.
Other areas of the body may be affected
The disease is not always confined to the spine and sacroiliac joints. In some cases, inflammation occurs in other joints and in other parts of the body outside of the spine (detailed below).
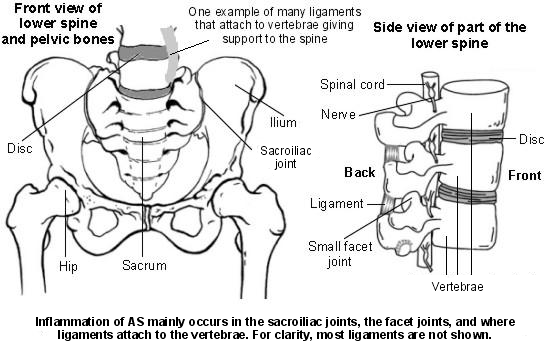
Understanding the lower back
The spine is made up of 33 bones called vertebrae stacked on top of each other. Each of the top 24 vertebrae is the shape of a squat cylinder and between each vertebra is a disc. The discs are made of rubber-like substance which allows the spine to be fairly flexible. Strong ligaments attach the vertebrae to each other and make the spine strong. Near the bottom of the spine, five vertebrae are fused together. They form a triangular-shaped bone called the sacrum. There are two large joints on either side of the bottom of the spine that join it on to the pelvis. They are called the sacroiliac joints because they join the sacrum (sacro-) to the main bone of the pelvis which is called the ilium (-iliac).
Lower spine side view - AS
Who gets ankylosing spondylitis?
Back to contentsAnkylosing spondylitis most commonly develops between 20 and 30 years of age. 80 out of 100 people will develop symptoms before the age of 30 and only 5 in a 100 will first develop symptoms over the age of 45. It is twice as common in men as it is in women. There may be a family history with two or more members of a family being affected.
Continue reading below
What causes ankylosing spondylitis?
Back to contentsThe exact cause is not known. However, there is a strong genetic tendency. There is a strong association with a gene variant called HLA-B27. About 9 out of every 10 people with ankylosing spondylitis have this gene variant compared with fewer than 1 out of every 10 in the general population. However, having HLA-B27 does not automatically lead to AS. 94 out of 100 people with HLA-B27 will not develop AS. Also, some people develop AS who do not have this gene variant. It is thought that something may trigger AS to develop in people who have an inherited tendency to develop AS, and that HLA-B27 provides a strong tendency. As yet, the trigger is unknown and other genes and factors may also be involved in causing AS.
Ankylosing spondylitis symptoms
Back to contentsThe most common symptoms of AS are back pain and stiffness.
Back pain. Back pain is the main symptom. Pain usually starts in the lower back and typically becomes gradually worse over several months. There may also be pain over the buttocks and down the back of the thighs. The buttock pain may be felt sometimes on one side and sometimes on the other side. Coughing or straining may make pain worse. Rest does not make it better. In fact, pain may be worse at night and better on getting up in the morning. Exercise and movement usually ease the pain. (This is the opposite to most bouts of common nonspecific lower back pain which may alert a doctor to the diagnosis of AS.) The pain tends to ease as the day goes on. The middle section of the spine (thoracic vertebrae) may also become affected. If this occurs, the joints between the ribs and the spine may also become painful.
Stiffness in the lower spine. The stiffness can be quite severe first thing each morning. It usually improves with activity and exercise, and tends to ease as the morning goes on.
Other joint symptoms apart from the spine. Other joints are affected at some stage in about 4 out of every 10 people with AS. The most common are the hips, knees, ankles and shoulders. Affected joints can become painful, stiff and swollen.
Inflammation of tendons and ligaments. Tendons and ligaments in various parts of the body (in addition to those attached to the vertebrae of the lower spine) may become inflamed and painful where they attach to bones. Common examples are the Achilles tendon (Achilles tendinopathy) where the calf muscles attach to the heel, and where chest muscles attach to the ribs (costochondritis).
Inflammation of part of the eye (uveitis). Uveitis is an inflammation of the eye. It affects about 1 in every 3 people with AS from time to time. People with AS who develop a painful or red eye should seek medical advice. Uveitis will usually be diagnosed by an eye specialist in an emergency department and treatment with eye drops should be started as soon as possible after eye symptoms begin. Treatment of uveitis is usually successful. However, if not treated quickly there can be permanent loss of vision in the eye (partial or complete).
General symptoms. Some people with AS feel generally unwell with symptoms of tiredness or depression. Unintended weight loss or anaemia sometimes occurs.
Associated conditions
Some other conditions develop more commonly than would be expected in people who have AS. People with AS have a greater than average chance of developing:
Cardiovascular disease (see later).
Note: Most people with ankylosing spondylitis do not get these conditions but they are more common in people with AS than in the general population.
Continue reading below
Ankylosing spondylitis diagnosis
Back to contentsThis condition is diagnosed based on:
Symptoms.
X-ray or magnetic resonance imaging (MRI) images
Blood tests can be helpful, but mainly to rule out other conditions. Blood tests can be performed to look for HLA-B27 which may help with the diagnosis.
As the disease progresses, typical changes develop on X-ray pictures of the sacroiliac joints and spine. The X-ray pictures show the bones (vertebrae) gradually fusing together. However, these changes may take several years to become bad enough to be seen on X-ray pictures.
X-ray changes used to be the only way to confidently confirm AS. Now an MRI scan of the sacroiliac joints can confirm the diagnosis at an earlier stage. An MRI scan can give a much more detailed view of a joint than a traditional X-ray picture and can detect inflammation in the sacroiliac joints.
How does ankylosing spondylitis progress?
Symptoms can vary in severity and usually wax and wane. Flare-ups of inflammation which cause periods of worse pain and stiffness tend to occur from time to time. If joints outside of the spine are affected, they tend to flare up at the same time as back symptoms. The number of flare-ups that occur, how severe they are, and how long they last, can vary greatly from person to person.
In time, the movement and flexibility of the spine may reduce. This happens as the inflammation and bony growths cause gradual joining together (fusion, or ankylosis) of some of your bones. The number of vertebrae involved and how much fusion happens vary from person to person. A bent-over, stooping posture may develop if it is very severe.
Ankylosing spondylitis treatment
Back to contentsThe aims of treatment are:
To ease pain and stiffness.
To keep the spine as mobile and flexible as possible.
To slow down the progress of the disease.
Physiotherapy and exercise
It is vital to have as good a posture as possible and a regular exercise routine. This helps to keep a full range of spinal movement and may help to prevent the condition worsening. Regular specific exercises are thought to limit the extent of any spinal deformity that may develop. The exercises may also ease back pain. A physiotherapist will usually be able to advise on the exact exercises to do. Doing exercises in a group may be particularly beneficial. Exercises should become a routine part of daily life.
Medication
Anti-inflammatory painkillers
These medicines are also called non-steroidal anti-inflammatory drugs (NSAIDs). An important reason to take these medicines is to ease pain so that regular exercise can be done without too much discomfort.
It is thought that anti-inflammatory medicines may not only ease symptoms of AS but may also slow down the progression of AS. Therefore, the advice is to take them regularly, not just as and when the pain flares up. There are several different anti-inflammatory medicines - for example, ibuprofen and naproxen are commonly used - but there are others as well. If one does not suit, another may be fine.
However NSAIDs can have side-effects and not everyone can take them. Side effects may include:
Stomach pain and bleeding from the stomach are the most serious. The risk of this is higher over the age of 65 years, or in people who have had a duodenal or stomach ulcer. Usually another medication will be prescribed to protect the stomach from these possible problems. Note: stop taking the tablets and see a doctor urgently if you develop any of the following whilst taking anti-inflammatory medicines:
Severe abdominal pains.
Passing blood or black stools (faeces).
Vomiting blood.
They can worsen or cause chronic kidney disease.
Some people with asthma find that NSAIDs can make their asthma worse - this is uncommon but these people should not continue with NSAIDs.
The leaflet which comes with the tablets gives a full list of possible side-effects. It is not known whether different NSAIDs are better than others in improving AS.
Ordinary painkillers
Painkillers such as paracetamol may be sufficient for someone who cannot take an anti-inflammatory painkiller if their symptoms are mild between flare-ups. It is also possible to take paracetamol in addition to an anti-inflammatory medicine for top-up pain relief.
Biological medicines
Medications that suppress the immune system have become available in recent years. They lessen the damaging effect of AS on the joints. They tend to be divided into two groups: biological therapies and immunomodulators. Immunomodulators are useful in rheumatoid arthritis but research has not shown them to be beneficial in ankylosing spondylitis. However biological medicines (also called biologics), have made a significant impact on the treatment of ankylosing spondylitis.
Biological medicines are substances made by living organisms such as cloned white blood cells. They are designed to target specific molecules of the immune system involved in inflammation. In ankylosing spondylitis, a chemical called cytokine tumour necrosis factor alpha (TNF-alpha) is involved in causing inflammation. Certain medicines in a group called TNF-alpha inhibitors block the action of this chemical. As a result they reduce inflammation and prevent damage to the joints. TNF-alpha inhibitors are also sometimes called anti-TNF-alpha drugs.
TNF-alpha inhibitors are now recommended to people with AS who have not responded well enough to NSAIDs or who can't take them. There are several TNF-alpha inhibitors available:
Adalimumab.
Certolizumab pegol.
Golimumab.
Infliximab.
They are given as an injection under the skin (except for infliximab which has to be given in a drip). The frequency of the injections varies from twice a week to once every eight weeks.
There are risks associated with taking these medicines and they require special monitoring, as some people develop serious side-effects. For example, taking these medicines may increase the risks of developing a serious infection (including tuberculosis, sepsis and pneumonia). Initially they were thought to increase the risks of developing some types of cancer, including lymphoma and leukaemia, but more recent studies suggest that this risk may be significantly lower than initially thought. There does seem to be an increased risk of developing non-melanoma skin cancer.
TNF inhibitors have also been rarely associated with developing multiple sclerosis or drug-induced lupus and they also can make heart failure worse (though they do not cause heart failure).
It is not known if any of the TNF-alpha inhibitors are more effective or safer than the others.
In the UK the National Institute for Health and Care Excellence (NICE) recommends that treatment with a TNF-alpha inhibitor should only be started and supervised by a specialist who is experienced in diagnosing and treating ankylosing spondylitis. They are recommended for people with severe ankylosing spondylitis who have not responded to NSAID treatment or who are unable to take NSAIDs.
After 12 weeks, treatment should continue only if your AS has shown an adequate improvement. Improvement is often measured by a test called the Bath Ankylosing Spondylitis Disease Activity Index (BASDAI). This asks various questions:
How tired are you?
How much pain do you have in your back?
How stiff are you in the morning?
How long does your stiffness last?
Do you have any areas of tenderness?
How bad is any joint pain or swelling (other than your back or neck)?
If the improvement is not maintained or if the medicine stops working then treatment should be stopped. Other medicines, such as secukinumab, ixekizumab, upadacitinib or tofacitinib may be tried if TNF-alpha inhibitors can't be used or have not been effective.
Other medication
Occasionally, other medicines are used:
A steroid injected directly into a badly inflamed joint is sometimes used to ease symptoms. Steroids taken as tablets or liquids are not used in ankylosing spondylitis.
Medicines called bisphosphonates are used to treat osteoporosis that is associated with AS.
Other treatments
Other treatments sometimes used include the following:
Transcutaneous electrical nerve stimulation (TENS) machines are sometimes used to ease pain. (These give tiny electrical currents into the affected area.)
Heat - for example, a hot shower - may help to ease pain, particularly each morning.
Some people find regular massage is soothing.
Surgery may be needed:
A hip replacement, as the hip sometimes becomes badly damaged by AS.
Surgery for severe spinal deformity.
Ankylosing spondylitis and cardiovascular disease
Back to contentsPeople with ankylosing spondylitis have an increased risk of developing cardiovascular disease as they get older. Cardiovascular disease is disease of the heart and blood vessels, caused by a fatty substance called atheroma. This may eventually lead to conditions such as angina, heart attack or stroke. It is not clear why the risk is increased in people with AS. It may be that the persistent (chronic) inflammation of the condition is partially responsible. There is some evidence that TNF-alpha inhibitors might reduce the risk of developing cardiovascular disease but further research is needed to confirm this.
The risk of cardiovascular disease can be reduced by the following actions:
Do not smoke or stop smoking.
Eat a healthy diet such as the Mediterranean diet.
Ensure that any high blood pressure, diabetes, or a high cholesterol level, are well controlled.
See the separate leaflet called Cardiovascular disease (Atheroma) for more details.
What is the outlook?
Back to contentsThere is no cure for AS and the outlook (prognosis) is variable.
Severe physical disability is unusual and most people can maintain a reasonable level of physical function and lead a relatively normal life.
The pattern of symptoms within the first 10 years of disease often suggests the likely long-term degree of disability. In one study, about 7 out of 10 patients with mild spinal restriction after 10 years did not progress to severe spinal involvement. However, among patients who developed long-term severe spinal involvement, 8 out of 10 had severe spinal restriction within 10 years.
People who develop ankylosing spondylitis at a younger age, tend to have worse progression than those who develop it later.
Eye inflammation (uveitis) may lead to severe sight impairment if not treated promptly.
People with established AS have an increased risk of fracturing the spine if they are involved in an accident such as a car crash or if they fall. This is because the spine becomes easier to fracture as it becomes more stiff and rigid. It is also due to osteoporosis which is more common in people with AS.
Patient picks for Back pain

Bones, joints and muscles
Slipped disc
A slipped disc is an old-fashioned term and does not truly describe what happens in this condition. It is more common to refer to it as a "disc prolapse", "disc herniation" or "disc bulge". There is further discussion below about these terms. However this leaflet will continue to use the term "slipped disc" due to its common usage. A slipped disc often causes sudden severe lower back pain. The disc often puts pressure on a nerve root which causes pain down one leg. Usually the symptoms gradually ease over several weeks. It is best to try and continue with normal activities as much as possible, using painkillers to help. Physical treatments such as spinal manipulation may also help. Surgery may be an option if the symptoms persist.
by Dr Philippa Vincent, MRCGP

Bones, joints and muscles
Lower back pain
About 8 in 10 people have one or more bouts of lower back pain. In most cases, it is not due to a serious disease or serious back problem, and the exact cause of the pain is not clear. This is called nonspecific lower back pain. The usual advice is to keep active and do normal activities as much as possible. Painkillers can help until the pain eases. In most cases, the pain disappears within six weeks but may come back (recur) from time to time. Persistent (chronic) pain develops in some cases and further treatment may then be needed.
by Dr Rachel Hudson, MRCGP
Frequently asked questions
Does AS affect everyone in the same way or does it vary?
Ankylosing spondylitis can vary significantly from person to person. The severity of symptoms can differ, and flare-ups of pain and stiffness tend to occur periodically. The number of flare-ups, their intensity, and how long they last are unique to each individual. The extent to which spinal bones fuse together can also differ, and a bent-over posture only develops in very severe cases.
What is the likelihood of AS being passed down to my children?
Ankylosing spondylitis has a strong genetic component, particularly with the HLA-B27 gene variant. If you have this gene, there's a higher chance your children might inherit it. However, inheriting the HLA-B27 gene doesn't guarantee they will develop AS; about 94 out of 100 people with this gene never develop the condition. While there may be a family history with more than one member affected, it's not a certainty for every child.
Can regular exercise help manage my AS symptoms?
Yes, maintaining good posture and having a regular exercise routine is vital for managing AS. Exercise helps maintain spinal movement and flexibility and may slow down the worsening of the condition. Specific exercises advised by a physiotherapist are thought to limit spinal deformity and ease back pain. It's recommended to make these exercises a routine part of daily life.
How soon will I know if TNF-alpha inhibitor treatment is working?
After starting treatment with a TNF-alpha inhibitor, its effectiveness is usually assessed after 12 weeks. Treatment is continued only if there has been an adequate improvement in your AS symptoms. This improvement is often measured using a test called the Bath Ankylosing Spondylitis Disease Activity Index (BASDAI), which assesses various symptoms like tiredness, back pain, morning stiffness, and joint pain.
Are there any alternative medicines for AS if I cannot take NSAIDs or if they are not effective?
If you cannot take NSAIDs or if they are not effective, your doctor might consider other medications. Ordinary painkillers like paracetamol can be used for mild symptoms between flare-ups. More significantly, biological medicines such as TNF-alpha inhibitors (adalimumab, certolizumab pegol, etanercept, golimumab, infliximab) are recommended for people with severe AS. If TNF-alpha inhibitors are not suitable or effective, other medicines like secukinumab, ixekizumab, upadacitinib, or tofacitinib may be tried.
Does AS only affect the spine, or can it impact other joints and parts of the body?
While AS mainly affects the spine and the sacroiliac joints, it can also manifest in other areas. About 4 out of 10 people with AS experience symptoms in other joints such as the hips, knees, ankles, and shoulders, which can become painful, stiff, and swollen. Tendons and ligaments can also become inflamed where they attach to bones, for example, the Achilles tendon and chest muscles. Inflammation of part of the eye (uveitis) affects about 1 in 3 people with AS.
What are the common early indicators of ankylosing spondylitis that I should watch out for?
The most common early indicators are back pain and stiffness, usually starting in the lower back and gradually worsening over several months. This pain may extend to the buttocks and down the back of the thighs, and can be worse at night or first thing in the morning. Unlike common back pain, rest doesn't improve it, and exercise or movement usually eases the pain and stiffness. Morning stiffness can be severe but typically improves with activity.
Further reading and references
- TNF-alpha inhibitors for ankylosing spondylitis and non-radiographic axial spondyloarthritis; NICE Technology Appraisal Guidance, February 2016
- BSR and BHPR guideline for the treatment of axial spondyloarthritis (including ankylosing spondylitis) with biologics; British Society for Rheumatology (2016)
- Secukinumab for active ankylosing spondylitis after treatment with non-steroidal anti-inflammatory drugs or TNF-alpha inhibitors; NICE Technology appraisal guidance, September 2016
- Spondyloarthritis in over 16s: diagnosis and management; NICE Guidance (Feb 2017)
- Ixekizumab for treating axial spondyloarthritis; NICE Technology appraisal guidance, July 2021
- Upadacitinib for treating active ankylosing spondylitis; NICE Technology appraisal guidance, September 2022
- Confirmed axial spondyloarthritis (including ankylosing spondylitis); NICE; April 2024
- Wenker KJ, Quint JM; Ankylosing Spondylitis.
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 19 Jan 2028
20 Jan 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.