Becker's naevus
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 22 Sept 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find one of our health articles more useful.
In this article:
Synonyms: Becker melanosis, pigmented hairy naevus of Becker
Continue reading below
What is Becker's naevus?
Becker's naevus is a form of epidermal naevus (birthmark). It usually appears around puberty as a hyperpigmented patch, most often found on the upper trunk or shoulders.1 2 3
See also the article on Epidermal Naevus and its Syndromes.
Becker's naevus on shoulder
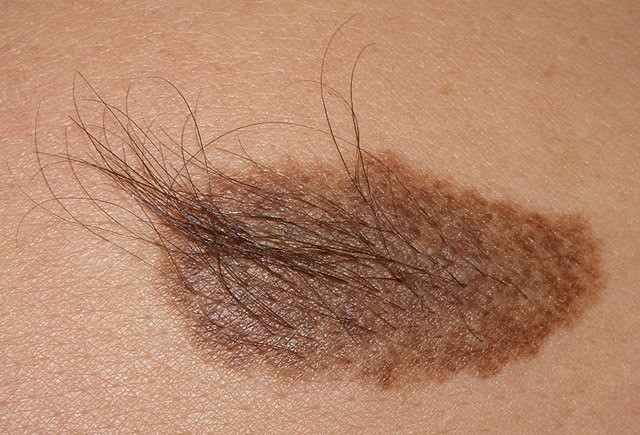
© Jmarchn, CC BY-SA 3.0, via Wikimedia Commons
Aetiology1
Back to contentsThere is overgrowth of the epidermis (upper layers of the skin), pigment cells (melanocytes) and hair follicles. It may be due to a gene defect (as yet unidentified), perhaps triggered by circulating androgens, which would explain its onset during adolescence.
Continue reading below
How common is Becker's naevus? (Epidemiology)1
Back to contentsMore common in males (ratio of 5:1). The estimated prevalence among males is 1 in 200.
Can occur in all skin types.
Usually presents in the second or third decade of life.
Becker's naevus symptoms (presentation)1 2
Back to contentsA large brown area, sometimes covering half the upper back or chest. Most lesions become hairy (hypertrichosis).
After puberty it often becomes darker and expands, usually over a period of 1-2 years.
Occasionally acne may develop in the naevus.
Some fading (reduced pigmentation) may occur in adulthood.
One case of bilateral, symmetrical pigmentation is reported - this is unusual.3
Continue reading below
Diagnosis
Back to contentsThe age of onset, site and the fixed nature of the lesion are usually enough to make the diagnosis. Biopsy may occasionally be needed.
Differential diagnosis1
Back to contentsMcCune-Albright syndrome (with café-au-lait patches on the skin).
Pityriasis versicolor is usually symmetrical and slightly scaly.
Histology3 4
Back to contentsEpidermis: acanthosis and hyperpigmentation of the basal layer, with elongation and fusion of adjacent rete ridges and variable hyperkeratosis.
Dermis: hyperplasia of the dermal smooth muscle and melanophages.
Becker's naevus treatment and management1
Back to contentsNo treatment is necessary except for cosmetic reasons; usually reassurance and a diagnosis are enough.
For cosmetic treatment of the lesion:
Electrolysis or laser treatment may help with hair removal.
Laser treatment can sometimes reduce the pigmentation, but may be ineffective or may worsen the lesion.
Fractional resurfacing has also been used to lighten the lesions.3
For acne in the lesion, use standard acne treatments.
If there is doubt about the diagnosis (eg possible melanoma), urgent referral is appropriate.
Prognosis
Back to contentsThe naevus remains indefinitely. There are no reports of Becker naevi undergoing malignant changes.5
Becker naevus syndrome5 6
Back to contentsBecker's naevus syndrome is a type of epidermal naevus syndrome. It is characterised by the presence of a Becker's naevus with ipsilateral breast hypoplasia or hypoplastic defects of the muscle, skin, or skeleton.
The naevus usually consists of a circumscribed, unilateral, irregularly shaped hyperpigmented macule, commonly occurring around the anterior upper trunk, with/without hypertrichosis and/or acneiform lesions.
Other features may include:
Supernumerary nipple.
Loss of subcutaneous fat
Loss of axillary hair
Musculoskeletal abnormalities and asymmetry.
Further reading and references
- Baalann KP, Krishnan M; Becker's nevus. Pan Afr Med J. 2022 Feb 17;41:142. doi: 10.11604/pamj.2022.41.142.33417. eCollection 2022.
- Kaliyadan F, Ashique KT; Becker Melanosis. StatPearls, Sept 2022.
- Becker Naevus; DermNet. July 2022.
- Becker's Naevus, DermIS (Dermatology Information System)
- Grim KD, Wasko CA; Symmetrical bilateral Becker melanosis: A rare presentation. Dermatol Online J. 2009 Dec 15;15(12):1.
- Cosendey FE, Martinez NS, Bernhard GA, et al; Becker nevus syndrome. An Bras Dermatol. 2010 Jun;85(3):379-84.
- Epidermal naevus syndromes; DermNet.
- Chikani UN, Ohuche IN, Bisi-Onyemaechi AI; Becker's nevus syndrome: a case report. J Med Case Rep. 2021 Aug 9;15(1):395. doi: 10.1186/s13256-021-02996-y.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 20 Sept 2028
22 Sept 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free