Hand, foot and mouth disease
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 29 Apr 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Hand, foot and mouth disease article more useful, or one of our other health articles.
In this article:
Continue reading below
What is hand, foot and mouth disease?
Hand, foot and mouth disease (HFMD) is a viral illness which commonly causes lesions involving the mouth, hands and feet. However, it may also affect other areas such as the buttocks and genitalia. The most common cause of hand, foot and mouth disease is Coxsackievirus A16 (CA16) but it is frequently caused by other coxsackieviruses or enteroviruses, particularly coxsackie A6 and enterovirus A71.1It is normally a mild, self-limiting illness but occasionally has serious complications, and fatalities have occurred in epidemics around the world. Coxsackievirus A10 has been associated with severe disease presentations.1
Epidemiology2
Back to contentsHand, foot and mouth disease occurs worldwide, with a peak incidence in the summer and autumn in temperate climates.
Vietnamese studies suggest a link between increase in temperature and humidity and the number of cases of HFMD.1
It typically affects children younger than 10 years of age, especially children younger than 4 years of age.
Outbreaks occur frequently in nurseries, childcare centres, and schools. Spread within families is also common.
Most adults are immune following previous exposure. However, adult cases may occur, especially with Coxsackievirus A6 infection.
Large-scale surveillance in China showed that 90% of cases occurred in children under the age of 5 with a death rate of 3 in 10,000 cases.1
Continue reading below
Hand, foot and mouth disease causes 12
Back to contentsHand, foot and mouth disease is most often caused by the group A Coxsackieviruses (particularly CA16) or enterovirus 71 (EV71). These closely related viruses are of the Picornaviridae family, Enterovirus genus, which includes echoviruses and polioviruses. It can be caused by other group A and B Coxsackieviruses, particularly Coxsackieviruses A6 and A10.3
Transmission is commonly by the faecal-oral route. Contact with skin lesions and oral secretions (including coughs and sneezes) can also allow transmission. An infected individual can continue to shed the virus in the stools for some weeks.
The incubation period is 3-6 days and infectivity is highest in the first week.1
Hand, foot and mouth disease symptoms 12
Back to contentsThe mucocutaneous lesions appear 1-2 days after a prodromal period of fever, malaise, anorexia and myalgia; and last approximately 7-10 days with spontaneous resolution.
Prodrome: includes a low-grade fever, malaise and loss of appetite. There may be a sore mouth or throat, cough or abdominal pain. EV71 can occasionally cause vomiting.
Diagram illustrating mouth, hand and foot lesions
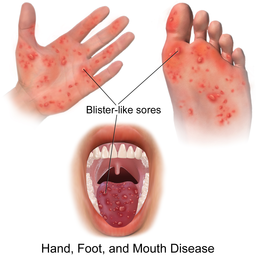
© BruceBlaus, BruceBlaus, CC BY-SA 4.0, via Wikimedia Commons
Mouth lesions: after the prodrome, lesions develop in the mouth. These may be on the buccal mucosa, tongue and hard palate. The uvula, gums, lips and skin around the mouth are sometimes involved. They begin as macular lesions that progress to vesicles which then erode. Mouth lesions are typically yellow ulcers surrounded by red haloes. They may be uncomfortable or painful. Children aged less than 5 years tend to have more severe symptoms than older children.
Skin lesions: most usually then also develop skin lesions. They are mainly on the palms, soles and between the fingers and toes. Lesions start as 2-5 mm erythematous macules but rapidly progress to grey vesicles with an erythematous base. Lesions may also appear on the trunk, thighs, buttocks and/or genitalia, particularly in younger children. Lesions are usually asymptomatic but can be itchy or painful.
Continue reading below
Differential diagnosis2
Back to contentsHerpangina (caused by similar Coxsackieviruses or echoviruses with lesions similar to hand, foot and mouth disease but limited to the posterior oral cavity with no skin lesions).
Viral pharyngitis.
Oral forms of lichen planus.
Investigations2
Back to contentsDiagnosis is usually clinical and investigations are not usually necessary.
The virus can be isolated from throat, vesicle or rectal swabs (placed in viral transport medium) or from faecal culture. Viral shedding in faeces can be intermittent so more than one specimen may be required.
Polymerase chain reaction (PCR) has made enteroviral subtyping possible and is increasingly the test of choice in specialist centres, although rarely used in routine clinical practice.
Hand, foot and mouth disease treatment2
Back to contentsThere is no known treatment, so management is generally supportive:
Parents may need to be reassured that it is unrelated to foot and mouth disease in animals.
Encourage adequate fluid intake. If the mouth is uncomfortable, dehydration may result from poor fluid intake.
Suggest a soft diet (soup, ice cream, mashed potato, etc).
Antipyretic analgesics, such as paracetamol or ibuprofen, are usually all that is required.
If the mouth is very painful, the following topical agents can be considered although there is no evidence of efficacy:
Lidocaine oral gel.
Benzydamine spray or mouth wash. (Spray only for those aged over 5 years, mouthwash for those aged over 12 years.)
Choline salicylate oral gel (not in children under the age of 16 years or in women who are pregnant or breastfeeding due to the risk of Reye's syndrome).
Teething gels may be useful in younger children.
Any cardiovascular or neurological complications need to be treated appropriately in secondary care (see below).
Indications to consider referral
Signs of significant dehydration (particularly in a child). Admission to hospital is rarely required.
Neurological signs or symptoms - for example, myoclonic jerks, persistent or severe headaches, signs of developing encephalitis.
Persistent oral ulcers.
Advice about school and childcare settings
Public Health England does not recommend that children be kept away from school/nursery/childcare for any period of time. There is no need to isolate a child with HFMD and it is not notifiable.4
Advise on general hygiene measures (see 'Prevention', below).
Advice for pregnant women
There are no known adverse consequences for the fetus if a pregnant woman is in contact with HFMD. The pregnant woman should seek medical advice from her obstetrician if she is immunosuppressed.
Seek specialist advice if a woman develops HFMD within three weeks of expected delivery, as there may be a risk of passing the infection to the newborn. In rare cases this can lead to severe infection in the neonate, although usually illness is mild.
Complications2
Complications are rare. They include the following:
Secondary infection of skin that has been scratched.
Painful stomatitis due to oral involvement. This can lead to dehydration.
Neurological involvement and meningitis are more likely if EV71 is the causative organism although it remains very rare in Europe; it is more common (though still rare) in outbreaks in the West Pacific and Asia. 5 6 Neurological involvement can include aseptic meningitis, encephalitis, polio-like syndrome, acute transverse myelitis, Guillain-Barre syndrome, benign intracranial hypertension, and acute cerebellar ataxia. The mortality rate from severe disease has been reported as between 10 and 25%. 2
Cardiorespiratory failure can occur in severe cases.
Prognosis2
Back to contentsThis is generally excellent with a full recovery in the vast majority people.
Symptoms tend to improve within 3-6 days, usually with full resolution of skin and mouth lesions within 7-10 days.
Those cases caused by EV17 have a greater likelihood of developing neurological complications, although this is rare. Aseptic meningitis usually resolves without sequelae but encephalitis is more likely to have adverse outcomes. During epidemics, particularly in the Western Pacific region, there have been a number of fatalities, particularly in the outbreak in China in 2009.
Infection results in immunity to the specific causative virus, but recurrence can occur with a different member of the enterovirus group.
Hand, foot and mouth disease prevention2
Back to contentsGood hygiene measures prevent spread within the family:
Thorough handwashing after using the toilet. There is evidence that handwashing has a significant protective effect.7
Covering of nose and mouth when coughing or sneezing.
Hygienic disposal of used tissues and nappies.
Avoidance of sharing of cups, eating utensils, towels, etc.
The virus can be shed in faeces for some time after recovery, so good hygiene should be maintained.
Further reading and references
- Hand foot and mouth disease; DermNet NZ
- Guerra AM, Orille E, Waseem M; Hand, Foot, and Mouth Disease.
- Hand, foot and mouth disease; NICE CKS, September 2024 (UK access only)
- Kimmis BD, Downing C, Tyring S; Hand-foot-and-mouth disease caused by coxsackievirus A6 on the rise. Cutis. 2018 Nov;102(5):353-356.
- UK Health Security Agency Guidance; Managing specific infectious diseases: A to Z; Hand, Foot and Mouth Disease
- Mao Q, Wang Y, Yao X, et al; Coxsackievirus A16: epidemiology, diagnosis, and vaccine. Hum Vaccin Immunother. 2014;10(2):360-7. doi: 10.4161/hv.27087. Epub 2013 Nov 14.
- Choi CS, Choi YJ, Choi UY, et al; Clinical manifestations of CNS infections caused by enterovirus type 71. Korean J Pediatr. 2011 Jan;54(1):11-6. Epub 2011 Jan 31.
- Ruan F, Yang T, Ma H, et al; Risk Factors for Hand, Foot, and Mouth Disease and Herpangina and the Preventive effect of hand-washing. Pediatrics. 2011 Apr;127(4):e898-904. Epub 2011 Mar 21.
- Zhu P, Ji W, Li D, et al; Current status of hand-foot-and-mouth disease. J Biomed Sci. 2023 Feb 24;30(1):15. doi: 10.1186/s12929-023-00908-4.
- Liang Z, Wang J; EV71 vaccine, an invaluable gift for children. Clin Transl Immunology. 2014 Oct 31;3(10):e28. doi: 10.1038/cti.2014.24. eCollection 2014 Oct.
Continue reading below
About the author

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 28 Apr 2028
29 Apr 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free