Chickenpox
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 29 Dec 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Chickenpox in adults and teenagers article more useful, or one of our other health articles.
In this article:
Synonyms: varicella, varicella zoster
Continue reading below
What is chickenpox?
Chickenpox is a highly infectious disease caused by the varicella-zoster virus. It is a DNA virus of the Herpesviridae family.
The varicella-zoster virus (HHV-3) can cause two forms of disease:1
Primary infection (varicella, or chickenpox).
Reactivation disorder (herpes zoster).
Chickenpox is usually a mild and self-limiting disease, but it can be severely complicated by pneumonitis or disseminated disease in some individuals, particularly neonates and those who are immunocompromised, including those on short courses of oral steroids.2 3 More information on those who are considered to have significant immunosuppression is included in the Green Book chapter on chickenpox.4
Chickenpox is a notifiable disease in Scotland and Northern Ireland but not in England.
How common is chickenpox? (Epidemiology)2 5
Back to contentsChickenpox is predominantly a childhood illness. The incidence is highest before 10 years of age. However chickenpox can occur at any age.6
More than 90% of people older than 15 years of age in England and Wales are immune (seropositive for varicella-zoster immunoglobulin G).
Although contact with chickenpox in pregnancy is common, only an estimated 3 in 1000 pregnancies are complicated by primary varicella-zoster infection.
Women from tropical and subtropical areas are at increased risk of developing chickenpox because they are more likely to be seronegative for varicella-zoster immunoglobulin G.
Peak incidence of varicella occurs from March to May, although there has been a reduction in seasonal variation in recent years.
Infectivity is from a few days before the onset of the lesions until the crusts fall off.
It is not possible to catch shingles from chickenpox, as the former represents a resurgence of a dormant virus. It is possible to catch chickenpox from active lesions of shingles.
Continue reading below
Chickenpox symptoms5
Back to contentsInfection with chickenpox and subsequent immunity can occur without clinical disease.
The incubation period between exposure and the first skin lesions is around 10 to 14 days but can be as long as 21 days.7
The first feature is often pyrexia - temperature of around 38-39°C is usual for up to four days. Prolonged or recurrent fever is suggestive of secondary infection.
Headache, malaise and abdominal pain may be reported.
Rash:
Small, erythematous macules appear on the scalp, face, trunk, and proximal limbs, which progress over 12–14 hours to papules, clear vesicles (which are intensely itchy), and pustules.
Redness around the lesion may suggest bacterial superinfection, probably introduced by scratching.
Vesicles can also occur on the palms and soles. Mucous membranes can also be affected, with painful and shallow oral or genital ulcers.
Vesicles appear in crops and so the stages of development of the rash can differ on different areas of the body. Crops of vesicles appear over the course of 3-5 days.
Crusting occurs usually within 5 days of the onset of the rash, and crusts fall off after 1–2 weeks.
When the crusts fall off they may leave marks that may be present for a few weeks but there is normally no long-term scarring. However, in adolescents and adults there is a greater risk of scarring.
Adults may experience a more widespread rash and more prolonged fever than children.
Immunosuppressed people with chickenpox may present with atypical rash and more extensive lesions (which may be haemorrhagic).
What does chickenpox look like?
Back to contentsNote the pustules and excoriation due to scratching.
Severe chickenpox in a child
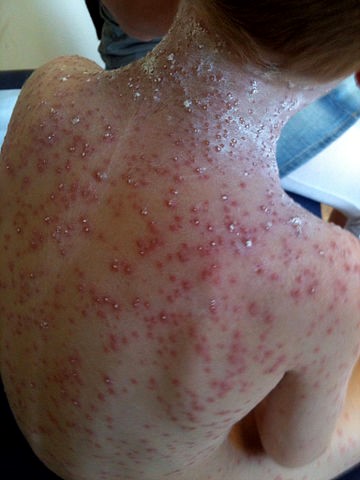
© Gzzz, CC BY-SA 4.0, via Wikimedia Commons
Chickenpox in a child
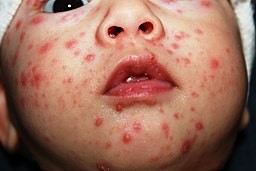
© Øyvind Holmstad, CC BY-SA 4.0, via Wikimedia Commons
Continue reading below
Differential diagnosis
Back to contentsThe clusters of vesicles usually make the diagnosis clear but differential diagnosis includes:5
Generalised herpes zoster or simplex.
Other viral skin infections.
Stevens-Johnson syndrome (usually the clinical picture is obvious).
Shingles, or herpes zoster, is like chickenpox but confined to just one dermatome. There may also be malaise. The lesions of chickenpox are at different stages and appear in clusters, tending to be central in distribution. The lesions of smallpox are all at the same stage and tend to be more peripheral. Smallpox has been eradicated and there is no known animal vector but the virus is kept in about a dozen laboratories throughout the world. In theory it could be developed for biological warfare or terrorism.
Investigations
Back to contentsUsually the diagnosis is obvious on clinical grounds, especially during an epidemic.
Confirmation can be obtained by taking a scraping of a lesion and using immunohistochemical staining or polymerase chain reaction tests.
Complications require further investigation - eg, respiratory symptoms require CXR and neurological features demand lumbar puncture.
Chickenpox treatment5
Back to contentsGeneral advice
Adequate fluid intake to avoid dehydration.
Dress appropriately to avoid overheating or shivering. Wear smooth, cotton fabrics.
Keep nails short to minimise damage from scratching and secondary bacterial infection from scratching.
The most infectious period is from 24 hours before the rash appears, but infectivity continues until all the lesions are dry and have crusted over (usually about 5 days after the onset of the rash). During this time, a person with chickenpox should avoid contact with:
People who are immunocompromised.
Pregnant women.
Infants aged 4 weeks or less.
Children with chickenpox should be kept away from school or nursery until all the vesicles have crusted over.
Advise to seek urgent medical advice if their condition deteriorates or they develop complications, including young children with chickenpox with:
Bacterial superinfection: sudden high grade pyrexia (often after initial improvement), erythema and tenderness surrounding the original chickenpox lesions.
Dehydration: encourage and monitor fluid intake and seek medical attention if signs of dehydration develop (eg, reduced urine output, lethargy, cool peripheries, reduced skin turgor).
Treatment of symptoms
Paracetamol if pain or fever are causing distress (avoid nonsteroidal anti-inflammatory drugs). Oral paracetamol is not licensed for use in children under 2 months of age.
Topical calamine lotion to alleviate itch.
Chlorphenamine for treating itch associated with chickenpox for people 1 year of age or older. Chlorphenamine is not recommended during pregnancy or breastfeeding.
Otherwise healthy child or adult with chickenpox
If serious complications (eg, pneumonia, encephalitis, dehydration, or severe secondary bacterial infection of the skin) are suspected, admit to hospital.
Consider oral aciclovir 800 mg 5 times a day for 7 days for an immunocompetent, non-pregnant adult or adolescent (aged 14 years or older) with chickenpox who presents within 24 hours of rash onset, particularly for people with severe chickenpox or those at increased risk of complications, such as smokers. Aciclovir is not recommended for otherwise healthy children with uncomplicated chickenpox.
If high temperature (particularly after initial improvement) with redness and pain surrounding the chickenpox lesions, consider bacterial superinfection and manage accordingly.
Pregnant woman with chickenpox
If caught in the first 20 weeks of pregnancy there is a 1-2% risk of congenital varicella syndrome. This causes a range of problems including intrauterine growth restriction, microcephaly, cortical atrophy, limb hypoplasia, microphthalmia, cataracts, chorioretinitis and cutaneous scarring.8
Infection with chickenpox in the later stages of pregnancy can cause premature delivery or neonatal chickenpox infection. This is particularly serious if the mother becomes infected seven days before birth.
Admit to hospital if a pregnant woman has suspected chickenpox and any of:
Respiratory symptoms.
Neurological symptoms.
Haemorrhagic rash or bleeding.
Severe disease (for example, dense rash with or without numerous mucosal lesions).
Significant immunosuppression (including recent use of systemic corticosteroids).
Consider/discuss the need for admission with a specialist if other risk factors for severe illness and complications are present such as:
Pregnancy approaching term.
Previous obstetric complications or risk factors.
Smoking.
Chronic lung disease.
Social risk factors.
Close monitoring in the community is not possible.
For all other pregnant women with chickenpox, seek immediate specialist advice from an obstetrician regarding further management such as antiviral treatment and outpatient follow up for the fetus.
Management in the community with specialist input may be considered appropriate. Oral antiviral drugs should only be prescribed in primary care on the advice of a specialist. Close monitoring is needed: review daily, or earlier if her condition deteriorates and have a low threshold for considering admission. Where close monitoring in the community is not possible, admission should be considered.
If there is deterioration, fever persists, or cropping of the rash continues after 6 days, refer for urgent hospital assessment.
If a high temperature develops (particularly after initial improvement) with redness and pain surrounding the chickenpox lesions, consider bacterial superinfection and manage accordingly.
Breastfeeding woman with chickenpox
Admit the woman to hospital if serious complications (eg, pneumonia or encephalitis) are suspected.
For all other breastfeeding women:
Consider aciclovir if presents within 24 hours of rash onset, particularly if she has severe chickenpox or is at increased risk of complications.
Seek urgent specialist advice regarding whether she should continue to breastfeed and whether her baby requires treatment to minimise the risk of complications.
Neonate with chickenpox
Seek immediate specialist advice regarding further management.
Give advice to the parents/carers about contact with other people.
Immunocompromised person with chickenpox
Admit to hospital if serious complications (eg, pneumonia or encephalitis) are suspected.
If complications are not suspected:
Seek immediate specialist advice to confirm the diagnosis of chickenpox and determine whether immediate admission is required to administer intravenous aciclovir.
If a high temperature develops (particularly after initial improvement) with redness and pain surrounding the chickenpox lesions, consider bacterial superinfection and manage accordingly.
Post exposure prophylaxis5
Back to contentsImportant information |
|---|
The UK Health Security Agency provided guidance on 'Post exposure prophylaxis for chickenpox and shingles' in January 2023.9 Chickenpox (varicella) infection in immunosuppressed individuals, pregnant women and neonates can result in severe and even life-threatening varicella disease. Post-exposure prophylaxis (PEP) is recommended to attenuate disease and reduce the risk of complications such as pneumonitis, rather than to prevent infection in these at-risk individuals. Antivirals are now recommended for post-exposure prophylaxis for all at risk groups apart from susceptible neonates exposed within one week of delivery (either in utero or post-delivery). Varicella zoster immunoglobulin (VZIG) is recommended for those for whom oral antivirals are contraindicated. |
For all people with a history of exposure to chickenpox, establish whether:
The diagnosis of chickenpox in the contact is certain.
The exposure was significant enough to put the person at risk of infection.
The person has had chickenpox in the past.
The person is at increased risk of complications of chickenpox (eg, pregnant women, immunocompromised people, and neonates).
The person is in contact with others at high risk of complications (for example, healthcare workers).
Exposure is significant if the person has had contact with:
Chickenpox.
Disseminated zoster.
Immunocompetent people with exposed lesions (for example, ophthalmic zoster).
Immunocompromised people with localised zoster on any part of the body (may have increased viral shedding).
Exposure is significant if the person was in contact with:
Chickenpox from 24 hours before onset of rash to crusting of lesions.
Disseminated zoster from 48 hours before onset of rash to crusting of lesions.
Localised zoster from day of onset of rash until crusting of lesions.
Exposure is significant if it is through:
Maternal/neonatal contact.
Continuous home contact.
Contact in the same room (for example, house or classroom) for 15 minutes or more, or contact on large open wards (particularly paediatric wards).
Face-to-face contact (for example, having a conversation).
If exposure to chickenpox is not significant, or if they have a history of chickenpox, or if they are known to be immune to chickenpox, reassure.
If the person is not immune, advise them that they may develop chickenpox.
For healthcare workers (and those who work in hospitals and general practice who have contact with patients) with a significant exposure to the varicella-zoster virus, advise that:
If they have a definite history of chickenpox or shingles and have had a significant exposure to the varicella-zoster virus, they can continue working as they are considered to be protected, however, if they develop a rash or fever, or feel unwell they should seek advice from occupational health before patient contact.
If they are not vaccinated and do not have a definite history of chickenpox or shingles, they should avoid contact with high-risk patients for 8–21 days from exposure and contact their occupational health department.
Pregnant woman exposed to chickenpox
Chickenpox infection during pregnancy is rare but may cause a congenital infection with malformation in fewer than 1% of cases.10
Establish the woman's risk of chickenpox, on the basis of her history of chickenpox, the certainty of chickenpox in the contact, and the level of exposure.
If definite history of chickenpox or shingles or two doses of a varicella containing vaccine, and is not immunocompromised, reassure her that she is not at risk of chickenpox because immunity can be assumed.
If no history of chickenpox or shingles (or is uncertain) and significant contact, establish the stage of gestation and seek urgent specialist advice.
Testing for varicella-zoster immunoglobulin G (IgG) antibodies in primary care may be appropriate if results can be available within 24–48 hours of first exposure. If a result within this time is not possible, testing in secondary care is needed.
If the test shows varicella-zoster immunoglobulin G antibodies (evidence of immunity from past infection or immunisation), the woman is immune.
If antibody status is negative, urgently discuss with a specialist the need for prophylaxis.
Advise all women to promptly seek advice if they develop a rash and/or symptoms and have had contact with chickenpox (regardless of whether they have received anti-virals, VZIG or have a history of chickenpox, shingles, or varicella vaccine).
Neonate exposed to chickenpox:
Establish the risk of chickenpox, on the basis of the certainty of chickenpox in the contact, and the level of exposure.
If the neonate's mother is the contact, determine when, in relation to delivery, she developed chickenpox. If someone else is the contact, determine the age of the neonate at the time of contact.
Seek urgent specialist advice regarding the need for testing and further management, and whether the mother should continue to breastfeed if she has chickenpox.
Immunocompromised person exposed to chickenpox:
Assess the certainty of chickenpox in the contact, the level of exposure, and whether the person fulfils the criteria for immunocompromise.
Seek same-day specialist advice regarding testing and management.
Complications of chickenpox
Back to contentsSecondary infection of lesions can occur, probably from scratching. A Polish study of children admitted to hospital found that 21% had secondary skin infection.11
Secondary bacterial infections, especially group A streptococcal infection, can produce necrotising fasciitis and toxic shock syndrome.
Viral pneumonia can be life-threatening - most often in older children and adults, appearing three or four days after the onset of the rash. Chest pain, wheezing and tachypnoea are all signs.12
Encephalitis is a serious illness that may require admission to an ICU. Symptoms include confusion, irritability, drowsiness and vomiting. Weakness or inability to walk, severe headache and neck stiffness are also possible features. An English study of 204 patients admitted to hospital with encephalitis found that in 5% the causative agent was chickenpox.13 The mortality rate is 5-10%.
Other CNS complications - eg, benign cerebellar ataxia, myelitis, vasculitis causing strokes (may occur several months after the chickenpox).7
Other infections - eg, osteomyelitis, sepsis, otitis media.
Chickenpox prevention5
Back to contentsThe most infectious period is from 24 hours before the rash appears, but infectivity continues until all the lesions are dry and have crusted over (usually about 5 days after the onset of the rash). During this time, a person with chickenpox should avoid contact with:
People who are immunocompromised.
Pregnant women.
Infants aged 4 weeks or less.
Children with chickenpox should be kept away from school or nursery until all the vesicles have crusted over.
Varicella vaccination4
Varicella vaccines contain live, attenuated virus.
The two-dose vaccination schedule (doses given 4 to 8 weeks apart) provides about 98% protection in children and about 75% protection in adolescents and adults.
Transmission of vaccine virus from immunocompetent vaccinees to susceptible close contacts has occasionally been documented but the risk is very low.
Transmission in the absence of a post-vaccination rash has not been documented.
Pre-exposure vaccination is recommended for:
Non-immune healthcare workers.
Individuals who may be exposed to varicella virus in the course of their work, in virology laboratories and clinical infectious disease units.
Healthy susceptible contacts of immunocompromised patients where continuing close contact is unavoidable.
Prognosis5
Back to contentsFor most children, chickenpox infection is usually a self-limiting, relatively mild disease without complications. Severe disease and complications are more likely to occur in children younger than 1 year of age, adolescents, adults, pregnant women, and immunocompromised people.
Recovery from primary varicella infection usually leads to lifelong immunity. Recurrence of varicella infection in otherwise healthy people is uncommon. Recurrence may be more likely in people who are immunocompromised.
Further reading and references
- Freer G, Pistello M; Varicella-zoster virus infection: natural history, clinical manifestations, immunity and current and future vaccination strategies. New Microbiol. 2018 Apr;41(2):95-105. Epub 2018 Mar 2.
- Chu L, Daganzo S, Aronowitz P; Chickenpox in a Vaccinated Adult. J Gen Intern Med. 2019 Mar;34(3):479-480. doi: 10.1007/s11606-018-4816-9. Epub 2019 Jan 8.
- Cohen J, Breuer J; Chickenpox: treatment. BMJ Clin Evid. 2015 Jun 15;2015. pii: 0912.
- Wu CT, Tsai SC, Lin JJ, et al; Disseminated varicella infection in a child receiving short-term steroids for asthma. Pediatr Dermatol. 2008 Jul-Aug;25(4):484-6. doi: 10.1111/j.1525-1470.2008.00720.x.
- Varicella: the Green Book, Chapter 34; Public Health England (June 2019)
- Chickenpox; NICE CKS, November 2023 (UK access only)
- Navaratnam AMD, Ma N, Farrukh M, et al; Chickenpox: an ageless disease. BMJ Case Rep. 2017 Dec 22;2017. pii: bcr-2017-222027. doi: 10.1136/bcr-2017-222027.
- Heininger U, Seward JF; Varicella. Lancet. 2006 Oct 14;368(9544):1365-76.
- Ghosh S, Chaudhuri S; Pregnancy and varicella infection: a resident's quest. Indian J Dermatol Venereol Leprol. 2013 Mar-Apr;79(2):264-7.
- Guidelines on post exposure prophylaxis (PEP) for varicella and shingles; UK Health Security Agency. (January 2023)
- Gaymard A, Pichon M, Bal A, et al; How to manage chickenpox during pregnancy: case reports. Ann Biol Clin (Paris). 2018 Dec 1;76(6):669-674. doi: 10.1684/abc.2018.1385.
- Gowin E, Wysocki J, Michalak M; Don't forget how severe varicella can be-complications of varicella in children in a defined Polish population. Int J Infect Dis. 2013 Jul;17(7):e485-9. doi: 10.1016/j.ijid.2012.11.024. Epub 2013 Jan 23.
- Masih I, Boyle R, Donnelly A, et al; Varicella pneumonitis in an immunocompetent patient. BMJ Case Rep. 2011 Mar 3;2011. pii: bcr0820103259. doi: 10.1136/bcr.08.2010.3259.
- Granerod J, Ambrose HE, Davies NW, et al; Causes of encephalitis and differences in their clinical presentations in England: a multicentre, population-based prospective study. Lancet Infect Dis. 2010 Dec;10(12):835-44. doi: 10.1016/S1473-3099(10)70222-X. Epub 2010 Oct 15.
Continue reading below
About the authorView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 27 Dec 2028
29 Dec 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free