Viral skin infections
Peer reviewed by Dr Sarah Jarvis MBE, FRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 25 May 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Viral rashes article more useful, or one of our other health articles.
In this article:
Continue reading below
What is a viral infection?
There are many viral skin infections. They range from the common to the rare, from the mild to the severe and from those causing just skin infection to those with associated systemic disease.
The following is a brief account of a selection of the important viral skin infections. Many of the diseases mentioned here are covered in greater detail elsewhere and the reader is referred to appropriate links.
Nonspecific viral rash
Back to contentsThis is a widespread erythematous rash sometimes seen in viral skin infections. It is accompanied by the common symptoms of a viral infection, such as fever, headache and malaise. The rash usually develops rapidly. The appearance varies but commonly takes the form of an erythematous blotchy eruption.
Continue reading below
Local viral infections
Back to contentsHerpes simplex
See the separate Herpes Viruses article.
Herpes zoster
See the separate Shingles article.
Molluscum contagiosum
See the separate Molluscum Contagiosum article.
Warts
See the separate Viral Warts (excluding Verrucae) article.
Orf1 2
Orf is a viral skin infection contracted from sheep and goats. It is caused by a parapoxvirus, which infects mainly young lambs and goats who contract the infection from one another (or possibly from persistence of the virus in the pastures).
Human lesions are caused by direct inoculation of infected material. This viral skin infection may occur in farmers, butchers, vets, children who bottle-feed lambs and possibly even children who play in pastures where sheep have grazed. The incubation period is five or six days.
Lesions are usually solitary but multiple lesions do occur. The lesions are small, firm, red or reddish-blue. They form a lump that enlarges to form a flat-topped, blood-tinged pustule or blister. The fully developed lesion is usually 2 cm or 3 cm in diameter but may be as large as 5 cm. Although there appears to be pus under the white skin, incising this will reveal firm, red tissue underneath. The lesion is sometimes irritable during the early stages and is often tender.
Orf virus on thumb
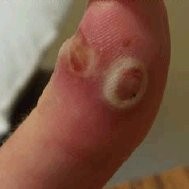
© Joelmills, Public domain, via Wikimedia Commons
Lesions usually occur on the fingers, hands or forearms but may be on the face. Red lymph lines may occur on the medial side of the elbow up to the axilla. There may also be a mild fever. Allergy to the virus may produce erythema nodosum 10-14 days later.
Usually only supportive conservative treatment is required for immunocompetent patients. The lesion may be covered to prevent spread, although human-to-human transmission is rare. It resolves spontaneously in 3-6 weeks.
In immunocompromised people, giant orf lesions can develop with continued progression in size instead of spontaneous regression. This type of lesion can take extended time or may fail to resolve naturally. Surgery may be needed to remove the lesion.
A vaccine has been developed to control the infection in sheep.
Viral infections that produce rashes
Back to contentsThere are a number of viral skin infections that may cause a rash - most of them typically in childhood. Examples include:
Chickenpox (varicella virus).
Monkeypox.3 In 2022, an outbreak of infections with this rare viral infection - usually seen in travellers from West or Central Africa - was identified in many countries across the world, including England. For the first time, human-human transmission among people with no history of travel to Africa or exposure to infected animals was identified. Spread largely by close skin-skin contact, the majority of cases confirmed in the early stages of this outbreak were in urban areas and among young men who self-identified as gay or bisexual. The infection has an incubation period of 5-21 (usually 7-14) days and early symptoms include fever, myalgia, lethargy, headache and lymphadenopathy. This is followed about three days later by a rash (which becomes vesicular and may become pustular), which usually starts on the face and spreads to other parts of the body, including the genital region.
Slapped cheek disease (also called fifth disease or erythema infectiosum) due to parvovirus.
Roseola (erythema subitum, due to herpesvirus 6).
Pityriasis rosea (the cause is unknown but it may be caused by herpesvirus types 6 and 7).
Echovirus and adenovirus infections often produce a rash.
Glandular fever (infectious mononucleosis) may cause a rash but, if amoxicillin or ampicillin (both are antibiotics) is given, there is almost invariably a rash.
HIV infection is often associated with a rash.
Continue reading below
Other viral infections with skin involvement
Back to contentsHand, foot and mouth disease
See the separate Hand, Foot and Mouth Disease article.
Crosti-Gianotti syndrome4
This is a response of the skin to viral skin infection in which there is a papular rash which lasts for several weeks.
Other names include papulovesicular acrodermatitis of childhood, papular acrodermatitis of childhood and acrodermatitis papulosa infantum.
Causes of the Crosti-Gianotti syndrome include:
Hepatitis B virus
Echoviruses
Respiratory syncytial virus
It affects children aged between 6 and 12 months - females more than males. There may be clusters and a preceding upper respiratory tract infection is not uncommon.
A profuse eruption of dull red spots develops over three or four days. They appear first on the thighs and buttocks, then on the outer aspects of the arms and finally on the face, often in an asymmetrical pattern.
The spots are 5-10 mm in diameter and a deep red colour. Later they often look purple, especially on the legs, due to leakage of blood from the capillaries. They may develop fluid-filled blisters.
Kaposi's sarcoma
See the separate Kaposi's Sarcoma article.
Viral skin infections and sport5
Back to contentsSport increases the risk of transmission of viral skin infection generally. A number of features may predispose to transmission:
There may be direct skin-to-skin contact (as in rugby, wrestling on other contact sports).
Profuse sweating may cause maceration of skin and provide a portal of entry.
Sharing wet areas predisposes to transfer of infection from feet. These include showers and swimming pools. Bare but dry feet, as in judo, other oriental martial arts and gymnastics, are associated with a lower risk of transmission.
Common viral infections that afflict athletes include those caused by herpes simplex virus, human papillomavirus and molluscum contagiosum virus.
Herpes gladiatorum6
The name of this viral skin infection implies association with martial arts. In association with rugby it is called 'scrum pox'. Transmission is primarily by direct skin-to-skin contact and abrasions may facilitate a portal of entry. The majority of lesions occur on the head or face, followed by the trunk and extremities. Recurrent episodes may follow the initial infection.
A prodromal itching or burning sensation is followed by clustered vesicles on an erythematous base which heal with crusts over about one to two weeks. Less often, headache, malaise, sore throat and fever may be reported.
Because of its unusual location, herpes gladiatorum any be confused with impetigo, varicella, staphylococcal furunculosis, or allergic or irritant contact dermatitis. Accurate diagnosis requires viral immunofluorescence and cultures should be obtained by gently breaking an intact vesicle and firmly rubbing the swab tip across the base of the erosion.
Treatment of herpes gladiatorum is with oral aciclovir, ganciclovir or similar agents and is most effective if commenced at the first symptoms of an outbreak. Topical aciclovir is probably less effective. Any secondary infection should also be treated.
The virus can survive for hours to days outside the host if conditions are appropriate. Hence, all contaminated surfaces should be cleaned with antiseptic solution. In the vesicular phase and until the crusts have separated, patients should avoid sports which could involve physical contact.
Prophylactic use of valacyclovir has been shown to be efficacious in lowering the incidence of outbreaks of herpes gladiatorum among adolescents at a 28-day wrestling camp.7
Viral skin infection and immune compromise
Back to contentsViral skin infections tend to be much more aggressive and virulent if the immune system, especially the T-cell system, is inadequate. The classical example is in HIV and skin disease but unusual and gross viral skin infection may occur in any condition in which immunity is impaired.
Further reading and references
- Viral skin infections; DermNet NZ
- Orf: characteristics and diagnosis; Public Health England
- Kassa T; A Review on Human Orf: A Neglected Viral Zoonosis. Res Rep Trop Med. 2021 Jul 8;12:153-172. doi: 10.2147/RRTM.S306446. eCollection 2021.
- Monkeypox; GOV.UK (May 2022)
- Chuh A, Zawar V, Sciallis GF, et al; Pityriasis Rosea, Gianotti-Crosti Syndrome, Asymmetric Periflexural Exanthem, Papular-Purpuric Gloves and Socks Syndrome, Eruptive Pseudoangiomatosis, and Eruptive Hypomelanosis: Do Their Epidemiological Data Substantiate Infectious Etiologies? Infect Dis Rep. 2016 Mar 21;8(1):6418. doi: 10.4081/idr.2016.6418. eCollection 2016 Mar 21.
- Nowicka D, Baglaj-Oleszczuk M, Maj J; Infectious diseases of the skin in contact sports. Adv Clin Exp Med. 2020 Dec;29(12):1491-1495. doi: 10.17219/acem/129022.
- Thompson AJ, Matinpour K, Hardin J, et al; Molluscum gladiatorum. Dermatol Online J. 2014 Jun 15;20(6). pii: 13030/qt0nj121n1.
- Anderson BJ, McGuire DP, Reed M, et al; Prophylactic Valacyclovir to Prevent Outbreaks of Primary Herpes Gladiatorum at a 28-Day Wrestling Camp: A 10-Year Review. Clin J Sport Med. 2016 Jul;26(4):272-8. doi: 10.1097/JSM.0000000000000255.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 24 May 2027
25 May 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free