Impetigo
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 17 Sept 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Impetigo article more useful, or one of our other health articles.
In this article:
Continue reading below
What is impetigo?
Impetigo is a very common superficial infection of the skin. It can be divided into non-bullous and bullous forms. The non-bullous types represent the majority of cases. The infecting organism for the more common non-bullous type is usually Staphylococcus aureus or Streptococcus pyogenes.
Over a period of 50 years there has been a considerable move from streptococci to staphylococci as the principal causative organisms. Meticillin-resistant S. aureus (MRSA) is another increasingly common causative organism for non-bullous impetigo.
Usually the predisposing factor is a breach of the skin but bullous impetigo may affect intact skin and is almost invariably caused by S. aureus. It is also occasionally classified as primary or secondary, where primary impetigo occurs in intact skin, and secondary impetigo in skin already damaged by another condition.
How common is impetigo?
Back to contentsImpetigo is a common condition. It most often affects children although it can occur at any age. In England and Wales, the highest weekly incidence of impetigo in children aged 0-4 and 5-14 has been estimated at 84 per 100,000 and 54 per 100,000 respectively.1 Global estimates suggest around 162 million children have impetigo at any one time, with the prevalence being highest in tropical areas and underprivileged communities.2 The streptococcal form is more common in warmer and more humid climates. There is some evidence for seasonal variation, with staphylococcal infections being more common in warmer months.3
Risk factors
Risk factors include poor hygiene and skin conditions that lead to a break in the protective layers. Atopic eczema is a common risk factor; others include bites, trauma to the skin, scabies, chickenpox, burns and contact dermatitis.
Continue reading below
Symptoms of impetigo
Back to contentsNon-bullous impetigo
Non-bullous lesions usually start as tiny pustules or vesicles that evolve rapidly into honey-coloured crusted plaques that tend to be under 2 cm in diameter. It is usually on the face (particularly around the mouth and nose) and may also be on the extremities where bites, abrasions, lacerations, scratches, burns or trauma have occurred. It spreads rapidly. Satellite lesions may occur as a consequence of autoinoculation. There may be some itching. There is little or no surrounding erythema or oedema. Regional lymph nodes are often enlarged.
Impetigo on chin
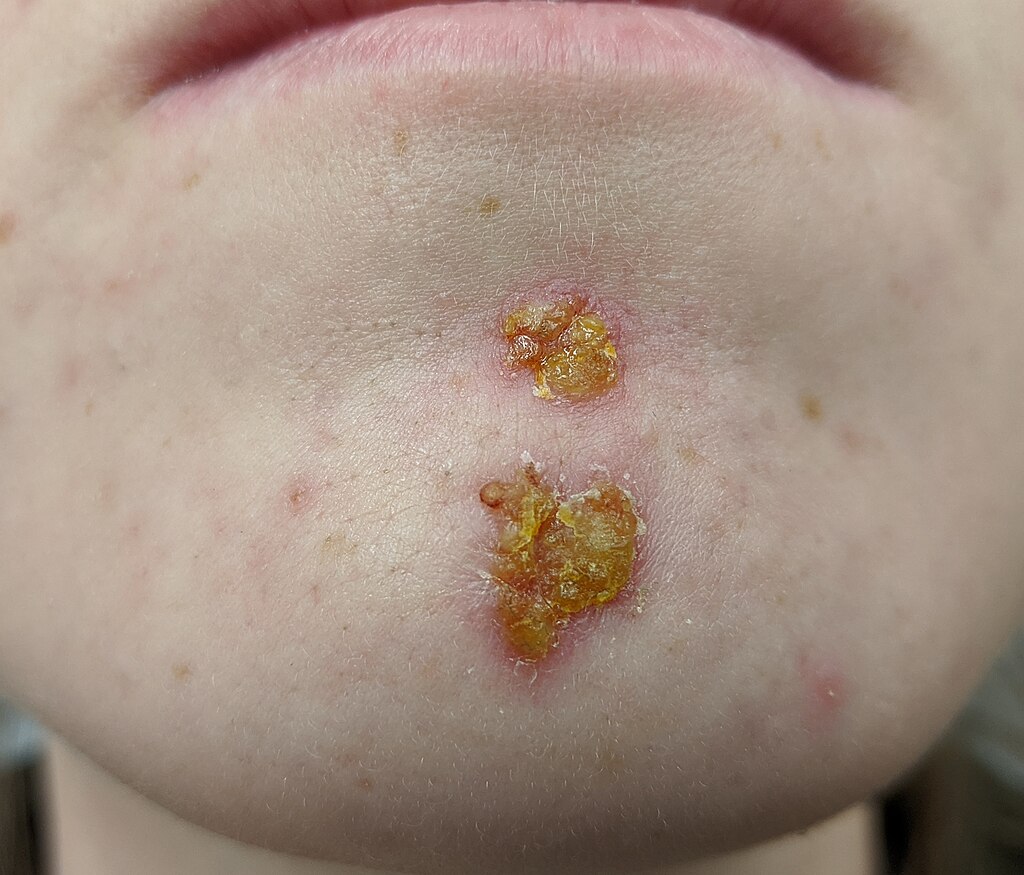
© James Heilman, MD, CC BY-SA 4.0, via Wikimedia Commons
Impetigo elbow
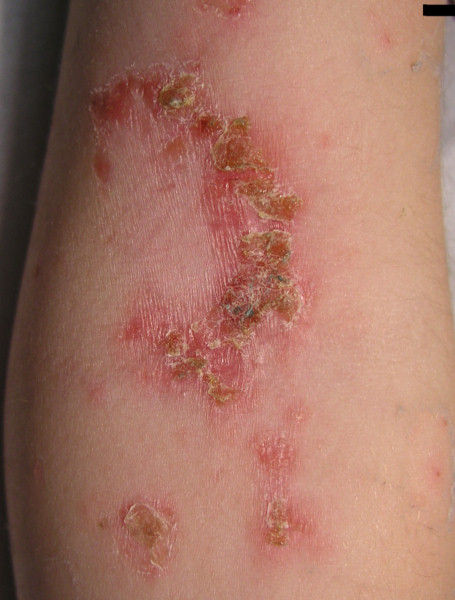
© Evanherk at Dutch Wikipedia, CC BY-SA 3.0, via Wikimedia Commons
Bullous impetigo
Bullous lesions have a thin roof and tend to rupture spontaneously. They are usually on the face, trunk, extremities, buttocks, or perineal regions. They are more likely to occur on top of other disease like atopic eczema.
There is little erythema and usually no regional lymphadenopathy. Bullous lesions are more common in neonates but can occur at any age. This type is more likely to be painful and may be associated with systemic symptoms of malaise.
Bullous impetigo
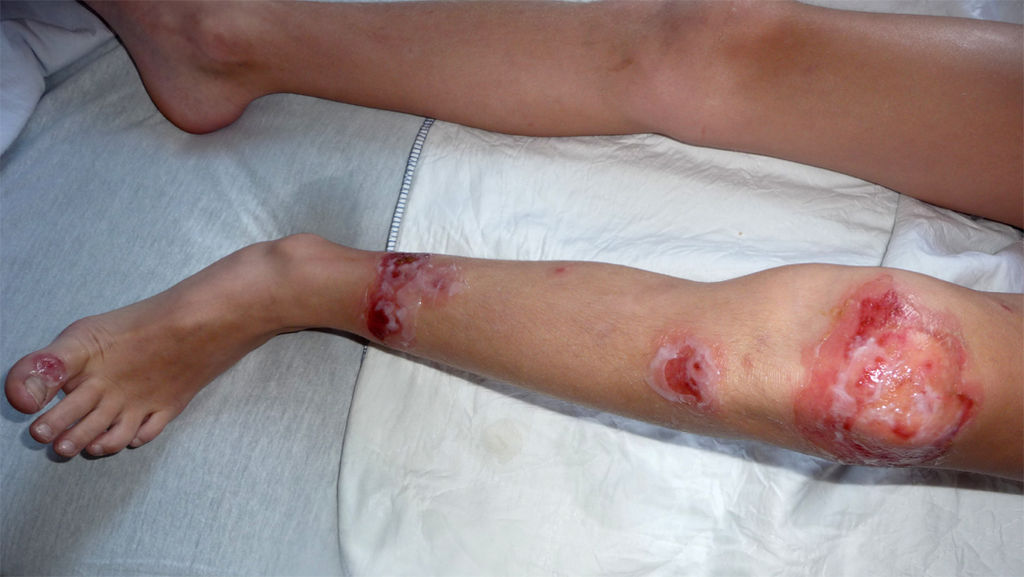
© Milliejen, CC BY-SA 3.0, via Wikimedia Commons
Ecthyma
This begins as a non-bullous impetigo but ulcerates and becomes necrotic. It is deeper and may occur with lymphadenitis.
Differential diagnosis4
Back to contentsVarious viral skin infections including herpes simplex, herpes zoster and varicella-zoster viruses.
Continue reading below
Diagnosing impetigo
Back to contentsDiagnosis is usually purely clinical but a swab for culture and sensitivity may be useful if:
The impetigo is extensive or severe.
MRSA is suspected.
The impetigo is recurrent or failing to respond to treatment. (Take nasal swabs if there is recurrent impetigo, to exclude nasal staphylococcal colonisation. Use Naseptin® to eradicate it if found.)
Managing impetigo45
Back to contentsGeneral advice
Advise good hygiene measures:
Keep the affected area(s) clean.
Wash hands after touching affected area(s).
Avoid sharing of towels and bathwater.
Avoid scratching the affected area. Keep fingernails short and clean.
Public Health England (PHE) advises that children should stay off school (or adults should stay off work) until lesions are all dry and scabbed over, or the affected person has been on antibiotics for 48 hours.6
Topical antibiotics
A Cochrane review found good evidence for efficacy of topical mupirocin and fusidic acid, and that they were as effective as oral antibiotic treatment. There was no evidence for topical disinfectants being effective therapy.7
Opinion varies as to whether crusts should be soaked off prior to applying topical treatment. The National Institute for Health and Care Excellence (NICE) Clinical Knowledge Summary on impetigo advises that fusidic acid be used first-line in localised infections, three times a day for seven days. Mupirocin should be reserved for cases where MRSA is the causative organism, to avoid resistance.
Systemic antibiotics
Oral antibiotics are only needed when infection is extensive or resistant to topical treatment, or causing systemic symptoms. A seven-day course is recommended. Flucloxacillin is recommended as first-line treatment when oral antibiotics are required.
Clarithromycin or erythromycin are recommended as second-line for those who are allergic to penicillin, with clarithromycin being preferred, as side-effects are less common.
Bullous infection usually requires oral antibiotics.
NICE recommendations8
To reduce the spread of impetigo, advise about good hygiene measures to reduce the spread of impetigo to other areas of the body and to other people.
Localised non-bullous impetigo
Hydrogen peroxide 1% cream for people who are not systemically unwell or at high risk of complications (eg, immunocompromised or co-existing skin conditions).
If hydrogen peroxide 1% cream is unsuitable, offer a short course of a topical antibiotic if not systemically unwell or at high risk of complications.
First-choice topical antibiotic: fusidic acid 2%. Alternative: mupirocin 2%.
Widespread non-bullous impetigo
A short course of a topical or oral antibiotic if not systemically unwell or at high risk of complications.
Offer a short course of an oral antibiotic for:
All people with bullous impetigo.
Those with non-bullous impetigo who are systemically unwell or at high risk of complications.
First-choice oral antibiotic: flucloxacillin. Alternatives: clarithromycin; erythromycin (in pregnancy).
If MRSA is suspected or confirmed: consult a local microbiologist.
Do not offer combination treatment with a topical and oral antibiotic to treat impetigo. Advise to seek medical help if symptoms worsen rapidly or significantly at any time, or have not improved after completing a course of treatment.
Impetigo that is worsening or has not improved after treatment with hydrogen peroxide 1% cream:
A short course of a topical antibiotic if the impetigo remains localised; or
A short course of a topical or oral antibiotic if the impetigo has become widespread.
Impetigo that is worsening or has not improved after completing a course of topical antibiotics:
A short course of an oral antibiotic (see the recommendations on choice of antimicrobial); and
Consider sending a skin swab for microbiological testing.
For people with impetigo that is worsening or has not improved after completing a course of oral antibiotics, consider sending a skin swab for microbiological testing.
Impetigo that recurs frequently:
Send a skin swab for microbiological testing and review the choice of antibiotic when results are available. Change the antibiotic according to results if symptoms are not improving, using a narrow-spectrum antibiotic if possible.
Consider taking a nasal swab and starting treatment for decolonisation, eg, nasal mupirocin.
Consider testing and decolonising household contacts.
Consider recommending the use of an antibacterial wash daily across the whole body, eg, Dermol.
Refer to hospital or seek specialist advice if:
There is impetigo and any symptoms or signs suggesting a more serious illness or condition (eg, cellulitis).
There is widespread impetigo in people who are immunocompromised.
There is bullous impetigo, particularly in babies (aged 1 year and under).
Impetigo is recurring frequently.
The patient is systemically unwell.
A high risk of complications exists.
Complications of impetigo
Back to contentsIf the causative organism is a group A beta-haemolytic streptococcus then rare complications such as scarlet fever or glomerulonephritis may occur. However, impetigo is most often caused by staphylococci.
Cellulitis, lymphangitis, suppurative lymphadenitis, and staphylococcal scalded skin syndrome may occur occasionally.
Mortality in infants with staphylococcal scalded skin syndrome is low but it can be as high as 63% in adults.9 It represents a serious clinical challenge and will usually require admission to hospital.
Prognosis
Back to contentsThe condition usually resolves without complications but it is highly contagious and may recur due to re-infection from family members with shared towels, etc.
Preventing impetigo
Back to contentsMeasures described include:
Avoidance of contact with infected individuals. Those affected should avoid school/nursery/work as above and cover the lesions where possible. They should use their own towels, flannels, clothing, etc, all of which should be washed separately and regularly.
Keeping wounds clean.
Teaching good personal hygiene. This is important for parents, carers and health professionals. For example: wash hands after contact with lesions or infected patients (with antibacterial soap and water or waterless antibacterial cleansers).
Treating pre-existing underlying skin diseases, such as atopic dermatitis (for example, antihistamines and topical steroids reduce scratching and hence skin damage and spread).
For patients with recurrent impetigo, asymptomatic family members and S. aureus nasal carriers, try measures to reduce colonisation of the nose and spread, such as the use of Naseptin®. Mupirocin may also be used (twice a day for five days applied to each nostril).
For MRSA screening and eradication, refer to local guidelines.
Exclusive updates for healthcare professionals
Stay informed with the latest clinical updates, professional insights, and evidence-based guidance. The Patient Pro newsletter curates essential content for healthcare professionals—delivered straight to your inbox.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
Further reading and references
- Elliot AJ, Cross KW, Smith GE, et al; The association between impetigo, insect bites and air temperature: a retrospective 5-year study (1999-2003) using morbidity data collected from a sentinel general practice network database. Fam Pract. 2006 Oct;23(5):490-6. doi: 10.1093/fampra/cml042. Epub 2006 Jul 27.
- Bowen AC, Mahe A, Hay RJ, et al; The Global Epidemiology of Impetigo: A Systematic Review of the Population Prevalence of Impetigo and Pyoderma. PLoS One. 2015 Aug 28;10(8):e0136789. doi: 10.1371/journal.pone.0136789. eCollection 2015.
- Leekha S, Diekema DJ, Perencevich EN; Seasonality of staphylococcal infections. Clin Microbiol Infect. 2012 Oct;18(10):927-33. doi: 10.1111/j.1469-0691.2012.03955.x.
- Impetigo; NICE CKS, August 2022 (UK access ony)
- Managing common infections: guidance for primary care; Public Health England, August 2020 - last updated June 2021
- Guidance on infection control in schools and other childcare settings; UK Health Security Agency (September 2017 - last updated February 2023)
- Koning S, van der Sande R, Verhagen AP, et al; Interventions for impetigo. Cochrane Database Syst Rev. 2012 Jan 18;1:CD003261. doi: 10.1002/14651858.CD003261.pub3.
- Impetigo: antimicrobial prescribing; NICE Guidance (February 2020)
- Handler MZ, Schwartz RA; Staphylococcal scalded skin syndrome: diagnosis and management in children and adults. J Eur Acad Dermatol Venereol. 2014 May 20. doi: 10.1111/jdv.12541.
Continue reading below
About the authorView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 16 Sept 2027
17 Sept 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free