Psoriatic nail disease
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Colin Tidy, MRCGPLast updated 23 Aug 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Nail psoriasis article more useful, or one of our other health articles.
In this article:
Psoriatic nail disease is more common in patients who have psoriatic arthritis such that it is a strong predictor for the development of psoriatic arthritis.1 Nail psoriasis occasionally occurs in the absence of any skin psoriasis. Psoriatic nail disease can be difficult to treat and severe nail changes can severely affect quality of life.
Characteristic nail changes include pitting (small irregularly spaced depressions measuring less than 1 mm in diameter), discolouration (circular areas resembling an oil drop), subungual hyperkeratosis, crumbling of the nail plate and onycholysis (separation of the nail plate from the nail bed).2
See also separate Chronic Plaque Psoriasis and Psoriatic Arthritis articles.
Continue reading below
Psoriatic nail disease epidemiology
An estimated 40-50% of patients with psoriasis have psoriatic nail disease. and 80% of patients with psoriatic arthritis have psoriatic nail disease.3 4
Psoriatic nail disease mainly occurs in patients who also have psoriasis affecting the skin. Fewer than 5% of patients have psoriasis of the nails without any skin involvement.5
Psoriatic nail disease symptoms (presentation)
Back to contentsSigns of nail psoriasis vary according to the part of the nail affected and the nature of the deformity:5
Oil drop or salmon patch: translucent yellow-red discoloration in the nail bed (the skin beneath the nail plate); resembles a drop of oil under the nail plate (the hard part of the nail).
Pitting: loss of parakeratotic cells from the surface of the nail plate.
Beau's lines: transverse lines in the nails due to intermittent inflammation causing growth arrest lines.
Leukonychia: areas of white nail plate due to foci of parakeratosis within the body of the nail plate.
Subungual hyperkeratosis: excessive proliferation of the nail bed and hyponychium (the junction between the free edge of the nail and the skin of the fingertip). This may lead to onycholysis.
Onycholysis: the nail plate separates from its underlying attachment to the nail bed. The nail plate whitens and may detach. Secondary infection may occur.
Nail plate crumbling: the nail plate weakens due to disease of underlying structures.
Psoriatic nail
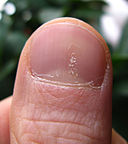
© Seenms, CC BY-SA 3.0, via Wikimedia Commons
Assessment of severity
The Nail Psoriasis Severity Index should be used to assess nail disease in specialist settings if there is a major functional or cosmetic impact or before and after treatment is initiated specifically for nail disease:6
Each nail is split into four quadrants and each is scored 0 or 1 for each of the following: pitting, leukonychia, red spots, nail plate crumbling, onycholysis, splinter haemorrhage, oil drop and nail bed hyperkeratosis.
The total score for each quadrant can therefore be up to 8 and the overall score for each nail is out of 32.
Continue reading below
Investigations7
Back to contentsNail biopsy is not usually performed due to its complexity and patient reluctance but it may be inevitable in cases where only one nail is affected.
Less invasive techniques being explored include:8
Ultrasound.
Optical coherence tomography (works on the principle that infrared light reflected from a nail is measured and the intensity is imaged as a function of position).
Confocal laser scanning microscopy (optimises resolution and contrast of a micrograph to produce 3D images).
Differential diagnosis
Back to contentsThe differential diagnosis of nail psoriasis includes:
Alopecia areata: may be associated with nail pitting and other nail abnormalities.
Lichen planus: longitudinal lines and linear depressions of the nail plate, severe dystrophy and complete destruction of the nail bed may occur.
See also separate Nail Disorders and Abnormalities article.
Continue reading below
Psoriatic nail disease treatment and management
Back to contentsMany treatment options are available but there is no agreed definitive or curative treatment. The treatments focus on improvement of the functional and psychosocial aspects of psoriatic nail disease.
General advice includes:9
Keep nails short to avoid exacerbating onycholysis and reduce the accumulation of material under the nail.
Avoid manicure of the cuticle, which may provoke infection of the nail bed.
Avoid prosthetic nails.
Mild nail disease not causing discomfort or distress does not need any treatment other than nail varnish to disguise pitting. Abrasive acetone-based nail varnish removers should be avoided.
A patient with painful toenail disease should be referred to a podiatrist.10
Any patient with nail psoriasis that has a major functional or cosmetic impact should be referred for dermatology specialist advice.6
The treatment options for nail psoriasis include:
Topical treatments (see below).
Onychomycosis (if present): this requires antifungal therapy for improvement.
Intralesional corticosteroids: intralesional triamcinolone acetonide injected into proximal nail folds is helpful but painful in nail matrix psoriasis.5
Psoralen plus ultraviolet light A (PUVA): improves subungual hyperkeratosis, onycholysis, discolouration and nail crumbling, but not pitting.8
Avulsion therapy.
Systemic therapy for severe cases.
A review by the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis (GRAPPA) found:11
Insufficient evidence to make any recommendation for the use of topical corticosteroids, topical calcipotriol, topical tazarotene, topical cyclosporine, dimethyl fumarates/fumaric acid esters, phototherapy, and alitretinoin.
There was a low strength of evidence to support the use of calcipotriol and corticosteroid preparations, topical tacrolimus, oral cyclosporine, oral methotrexate, intralesional corticosteroids, pulsed dye laser, acitretin, Janus kinase inhibitors, and apremilast.
The highest strength of supporting evidence was for the recommendation of biologic agents including tumour necrosis factor inhibitors, and interleukin 12/23, 17, and 23 inhibitors.
Topical treatments8
Topical treatments: topical corticosteroids, salicylic acid, calcipotriol, or tazarotene used alone or in combination can be considered.
However, nail psoriasis is generally refractory to topical treatment. Phototherapy or systemic therapy is therefore often required.6
Intralesional injections, either with corticosteroids, methotrexate or ciclosporin, have been beneficial.
Systemic non-biological treatments
Systemic non-biological therapy should be offered to patients with significant functional impairment and/or high levels of distress as a result of severe nail disease.6
Methotrexate is recommended as the first choice of systemic agent for people with psoriasis.6
However, one study found moderate benefit with treatment using methotrexate or ciclosporin and there were no significant differences in efficacy between the two treatments. A significant improvement was detected in the methotrexate group for the nail matrix findings and in the ciclosporin group for the nail bed findings.8
Systemic biological treatments
The biological therapies adalimumab, efalizumab, etanercept, infliximab and ustekinumab have shown clinically important nail psoriasis improvements using the Nail Psoriasis Severity Index.8
Avulsion therapy12
Avulsion therapy by chemical or surgical means can be used as an alternative therapy for psoriatic nail disease.
Chemical avulsion therapy includes application of an ointment to the affected nail under occlusion for seven days; the nail is removed without any trauma. Chemical avulsion therapy is painless, involves no blood loss and is less expensive than surgical avulsion.
Surgical avulsion therapy can be performed for psoriatic nail disease when other treatments have failed. The matrix (the part of the nail bed that is beneath the nail and contains nerves, lymph and blood vessels) can be electively ablated to prevent regrowth of the nail. This procedure is performed under local anaesthesia.
Other physical therapies8
Other physical therapies tried have included radiotherapy, Grenz rays, laser therapy and electron beam therapy.
Complications
Back to contentsNail psoriasis is associated with discomfort in many patients and leads to significant functional impairment and psychological stress.13
Prognosis
Back to contentsPsoriatic nail disease is not associated with any increase in mortality but can be refractory to treatment and therefore can have significant long-term effects on quality of life.8
Prevention
Back to contentsFor preventative care, the nails should be kept dry and protected from trauma to avoid Köbner's phenomenon (lesions appearing at the site of injury - often written as Koebner's phenomenon) and possible secondary infection.
Further reading and references
- Psoriasis - nail psoriasis; Primary Care Dermatology Society. Last updated May 2022.
- Sobolewski P, Walecka I, Dopytalska K; Nail involvement in psoriatic arthritis. Reumatologia. 2017;55(3):131-135. doi: 10.5114/reum.2017.68912. Epub 2017 Jul 18.
- Psoriasis, nail changes; DermIS (Dermatology Information System)
- Kaeley GS, Eder L, Aydin SZ, et al; Nail Psoriasis: Diagnosis, Assessment, Treatment Options, and Unmet Clinical Needs. J Rheumatol. 2021 Aug;48(8):1208-1220. doi: 10.3899/jrheum.201471. Epub 2021 Feb 15.
- Bardazzi F, Starace M, Bruni F, et al; Nail Psoriasis: An Updated Review and Expert Opinion on Available Treatments, Including Biologics. Acta Derm Venereol. 2019 May 1;99(6):516-523. doi: 10.2340/00015555-3098.
- Nail psoriasis; DermNet NZ
- Psoriasis: The assessment and management of psoriasis; NICE Clinical Guideline (October 2012 - last updated September 2017)
- Grover C, Chaturvedi UK, Reddy BS; Role of nail biopsy as a diagnostic tool. Indian J Dermatol Venereol Leprol. 2012 May-Jun;78(3):290-8. doi: 10.4103/0378-6323.95443.
- Dogra A, Arora AK; Nail psoriasis: the journey so far. Indian J Dermatol. 2014 Jul;59(4):319-33. doi: 10.4103/0019-5154.135470.
- Psoriasis; NICE CKS, September 2022 (UK access only)
- Tracey C et al; How to Treat Dystrophic Nails, Podiatry Today, 2013
- Laheru D, Antony A, Carneiro S, et al; Management of Nail Disease in Patients With Psoriatic Arthritis: An Updated Literature Review Informing the 2021 GRAPPA Treatment Recommendations. J Rheumatol. 2023 Mar;50(3):433-437. doi: 10.3899/jrheum.220313. Epub 2022 Nov 1.
- Pandhi D, Verma P; Nail avulsion: Indications and methods (surgical nail avulsion), Indian Journal of Dermatology, Venereology and Leprology, 2012.
- Baran R; The burden of nail psoriasis: an introduction. Dermatology. 2010;221 Suppl 1:1-5. Epub 2010 Aug 9.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 21 Aug 2028
23 Aug 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free