Hives
Urticaria
Peer reviewed by Dr Hayley Willacy, FRCGP Last updated by Dr Philippa Vincent, MRCGPLast updated 20 Jun 2024
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Hives (also called urticaria) are itchy red or white bumps on the skin that look like a nettle rash. Hives are common and are often caused by an allergic reaction, stress, infections, or certain medications. Most hives get better on their own within a few days. This leaflet discusses the causes, types, and treatment for hives.
In this article:
Video picks for Skin rashes
Key points
Hives, also known as urticaria, are raised, red, itchy bumps that can appear anywhere on the body. They are usually an allergic response to something in your environment or something you ate.
Common triggers include allergies, infections, medicines, stress, or physical factors like heat, cold, and pressure. They often come and go within hours, sometimes lasting a bit longer depending on the trigger.
Hives are usually harmless but can be uncomfortable - persistent or severe cases may need medical advice.
Treatments include avoiding the trigger (where possible), and using antihistamines.
Continue reading below
What are hives?
Hives (or urticaria) is an itchy rash caused by tiny amounts of fluid that leak from blood vessels just under the skin surface.
A trigger causes cells in the skin to release chemicals such as histamine. The chemicals cause fluid to leak from tiny blood vessels under the skin surface. The fluid pools to form wheals or welts. The chemicals also cause the blood vessels to open wide (dilate) which causes the flare around the wheals. In about half of the cases, the trigger is not clear and cannot be identified.
What are hives?
Hives symptoms
Back to contentsAn itchy rash is the main symptom of hives (urticaria). The rash can appear anywhere on the body. Small, raised areas called wheals develop on the skin. The wheals look like mild blisters and are itchy. Each wheal is white or red and is usually surrounded by a small red area of skin which is called a flare.
Hives (Urticaria)
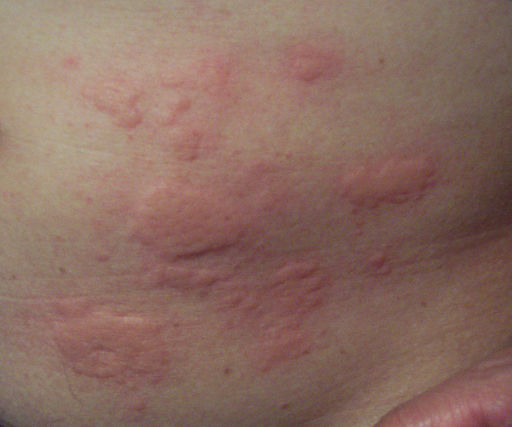
© Enochlau, CC BY-SA 3.0, via Wikimedia Commons
The wheals are commonly 1-2 cm across but can vary in size. There may be just a few but sometimes many develop over various parts of the body. Sometimes wheals that are next to each other join together to form larger ones. The wheals can be any shape but are often round.
As a wheal fades, the surrounding flare remains for a while. This makes the affected area of skin look blotchy and red. The blotches then fade gradually and the skin returns to normal. Each wheal usually lasts less than 24 hours. However, as some fade away, others may appear. It can then seem as if the rash is moving around the body. The rash may clear completely only to return a few hours or days later.
Most people with acute hives do not feel ill; however, the appearance of the rash and the itch can be troublesome.
In some cases a condition called angio-oedema develops at the same time as hives. In this condition some fluid also leaks into deeper tissues under the skin, which causes the tissues to swell. See the separate leaflet called Angio-oedema for more details:
The swelling of angio-oedema can occur anywhere in the body but most commonly affects the eyelids, lips and genitals.
Sometimes the tongue and throat are affected and become swollen. The swelling sometimes becomes bad enough to cause difficulty breathing.
Symptoms of angio-oedema tend to last longer than urticarial wheals. It may take up to three days for the swollen areas to subside and go.
A variation called vasculitic hives occurs in a small number of cases. In this condition the wheals last more than 24 hours, they are often painful, may become dark red and may leave a red mark on the skin when the weal goes. Technically, this type of rash is not urticaria.
Continue reading below
What causes hives?
Back to contentsHives can be triggered by a number of different physical causes. The reason why a rash appears in affected people is not clear. The physical stimulus causes a release of histamine and other chemicals, which causes the rash.
Some known triggers include:
A physical stimulus. Where this is the case the condition is called inducible urticaria. In this type of hives, a rash appears when the skin is physically stimulated (for example, by heat, cold or pressure on the skin).
Allergies - for example:
Food allergies such as allergies to nuts, strawberries, citrus fruit, egg, food additives, spices, chocolate, or shellfish. Sometimes an allergy can develop to a food even if it has been eaten without any problem many times before.
Allergies to insect bites and stings.
Allergies to medicines such as penicillin, aspirin, anti-inflammatory painkillers, etc.
A viral infection such as the common cold or flu can trigger an urticarial rash in some people as a reaction to the virus. A mild viral infection which causes few other symptoms is probably a common trigger of an urticarial rash that develops without an apparent cause.
Skin contact with some substances causes a local area of contact hives in some people. For example, chemicals, latex, cosmetics, plants including pine trees, ointments, nettle stings, etc.
Types of hives
Back to contentsHives can be classed as follows:
Acute - if it develops suddenly and lasts less than six weeks. Most cases last 24-48 hours. In some cases the rash only lasts a few hours. About 1 in 6 people will have at least one bout of hives in their lives. It can affect anyone at any age. Some people have recurring bouts of acute hives.
Chronic - if it persists longer than six weeks. This is uncommon.
Physical causes can result in repeated episodes of acute hives, or a persisting long-term condition.
The main types of inducible urticaria include the following:
Dermographism
Urticaria dermatographia

© R1carver, CC BY-SA 3.0, via Wikimedia Commons
Dermographism (also known as dermatographism and dermatographia) means skin writing. People with this condition develop the rash on areas of skin that have been firmly stroked. (Because of this, it is possible to 'write' on someone's skin by applying firm pressure with a finger or other object. The rash follows the line of the writing on the skin.)
The affected area of skin is usually very itchy but in some mild cases it does not itch much. Although any part of the skin can be affected, the palms, soles of the feet, genital skin and scalp are less commonly affected.
Dermographism is more prone to occur when hot. For example, it may develop more easily after a hot shower. The rash tends to last less than an hour. In many cases the pressure needed to be applied to cause the rash is quite firm. However, some people develop dermographism with just light pressure.
Up to 1 in 20 people will develop dermographism at some stage of life. It most commonly first develops in early adult life. In most cases, the condition tends to improve gradually over a few years and it goes or becomes less severe. However, in some cases the condition remains troublesome for many years.
Cholinergic urticaria or cholinergic hives
Cholinergic hives are quite common. The condition is caused by sweating and is sometimes called heat bumps. The hives rash is quite distinct as the wheals are very small (2-3 mm) with a red flare around each one.
The rash appears within a few minutes of sweating and tends to be worst on the chest, back and arms. The rash lasts from 30 minutes to an hour or more before fading away. Some people become slightly wheezy and short of breath for the duration of the rash.
The sweating that triggers the rash may be due to exercise, heat, high temperature (fever), emotion or eating spicy food. It can be problematic when exercising. In severe cases, hundreds of tiny wheals develop when running or doing other types of exercise. Sometimes the tiny wheals join together to form larger ones.
Cholinergic hives most commonly first develop in early adult life. In many cases the condition tends to improve after a few years and it goes or becomes less severe. However, in some cases the condition remains troublesome for many years.
Cold hives or cold urticaria
Cold hives are quite an uncommon condition. An urticarial rash develops after being exposed to cold, including rain, cold winds and cold water. It may be the cold that triggers the rash, or the re-warming of the skin after coming in from the cold.
The rash affects the chilled parts of the skin. If a large area of skin has been chilled, the rash can be very extensive. For example, swimming in cold water may cause a widespread and severe rash over most of the body that can cause dizziness or fainting. (For this reason, people who are known to develop cold hives should never go swimming alone.)
Delayed pressure hives
Delayed pressure hives are uncommon. The condition can develop alone but it commonly affects people who also have chronic hives. In this type of hives the rash develops 4-6 hours after the affected area of skin has had deep prolonged pressure applied, for example, after wearing a tight seatbelt or wearing a tight watch strap. The rash can be painful and tends to last several hours or longer.
Solar hives or solar urticaria
This is a rare condition in which an urticarial rash develops on skin exposed to sunlight.
Water contact (aquagenic) hives
In this rare condition, an urticarial rash develops on skin exposed to water of any temperature.
Vibratory hives
In this rare condition, the rash comes up after using vibrating tools.
Continue reading below
Diagnosing hives
Back to contentsAre any tests needed?
Usually no tests are needed. The rash is very typical and is easily recognised as hives by doctors. In a few cases it is clear what caused the rash from the events leading up to it, for example if recently stung by a nettle or starting new medication.
A symptom diary
A symptom diary may be helpful in working out if there is a specific cause. A diary might also show if the rash relates to stress, exercise or sunlight. It may help rule out certain causes.
Skin-prick allergy tests
In some cases, if it appears to be related to an allergy, tests such as skin-prick allergy tests may be helpful. Tiny quantities of substances which might cause an allergy are placed on the skin in a special order. If the skin reacts, there may be an allergy to that substance.
Blood tests
In other cases, blood tests for allergy may be useful. In some people, blood tests may help to point to a cause. These may be general blood tests, or blood tests to look for specific proteins produced by the immune system, called autoantibodies. Where these are found, it is likely that it is the body's own immune system over-reacting and causing the rash. Skin-prick tests are usually ordered in an allergy clinic; blood tests are unreliable and, although they can be ordered by GPs, it is usually best for these to be requested from allergy clinics as well.
Exclusion tests
In some people, 'exclusion' or 'challenge' tests may be needed, for example, testing to see if cold or pressure always causes the rash, or excluding certain foods from the diet to see if that stops the rash from coming back.
Biopsy
Occasionally, if urticarial vasculitis is suspected, a sample of the skin may be taken (a skin biopsy) for further analysis.
Hives treatment
Back to contentsOften no treatment is necessary, as the rash commonly goes within 24-48 hours. A cool bath or shower may ease the itch. Calamine lotion or menthol 1% in aqueous cream can help with itching, although if it is left on for too long the itch may come back. These can be bought without a prescription.
Once it is clear what causes the hives, it may be possible to avoid situations that trigger them. For example, dermographism can often be prevented by avoiding firm pressure against the skin as much as possible. In mild cases, no additional treatment may be needed.
Home remedies
Various other factors may make symptoms worse (but are not the main trigger). The following are tips that some people have found helpful; however, there is little proof that they work in everybody:
Try avoiding tight clothes if wheals occur at sites of local pressure, for example, under belts, under tight-fitting shoes, etc.
Try keeping cool, as hives may tend to flare up in warmer conditions. In particular, keep the bedroom cool at night.
For some people alcohol, hot baths, strong sunlight, and emotion make symptoms worse. If you think any of these are making symptoms worse then it may be helpful to try to avoid them.
See a doctor if you think a medicine is making symptoms worse, as a change in medication may be an option. Some medicines that may be triggers include aspirin, anti-inflammatory painkillers, and angiotensin-converting enzyme (ACE) inhibitors.
Antihistamines for urticaria
Many types of hives are helped by taking antihistamine medicines. (However, these medicines may not help some cases of delayed pressure hives.) Antihistamines block the action of histamine which is involved in causing hives.
The most commonly used antihistamines for hives are:
These do not usually cause drowsiness.
A doctor may advise doses which are higher than the usual recommended dose in order to control the rash. If the itch is making it difficult to sleep, sometimes an antihistamine which causes drowsiness can also be taken at night. Examples of antihistamines used in this way include chlorphenamine or hydroxyzine.
All these antihistamines can be bought over the counter, without a prescription. Whilst a doctor will often recommend taking up to four times the licensed dose (and there is good evidence that this is safe and effective), this should be discussed with a doctor or clinical pharmacist first. Antihistamines are not usually advised in pregnancy.
Some people take antihistamines now and then when a rash flares up. If an antihistamine is taken as soon as the rash appears, the rash tends to fade more quickly than it would do normally. If the rash recurs frequently then a regular dose of an antihistamine may be advised to prevent the rash from occurring.
In cholinergic urticaria where the rash develops on exercise, a dose of an antihistamine just before exercising may help to prevent or limit a flare-up of the rash.
Steroid tablets
Occasionally for severe flare-ups of hives, a course of prednisolone tablets taken for a week may be helpful, but the benefits have to be weighed up against the risks. Unlike most types of hives, those caused by a physical stimulus are not helped by steroids.
Other treatments
Someone with severe episodes of hives may be referred to a specialist. Skin specialists (called dermatologists) or allergy specialists (called immunologists) may be able to help. In particular, if angio-oedema or anaphylaxis occurred at the same time, urgent hospital admission would be required. This is to reverse the reaction quickly and also to confirm the diagnosis and, where possible, to identify a cause. For example, if a nut allergy is suspected to have caused a severe episode then this can confirmed by tests.
Occasionally other treatments may be used, such as a tablet called montelukast, which is usually used for asthma. This may be particularly useful in delayed pressure urticaria, where antihistamines often do not help.
Omalizumab is a newer medication which acts against autoantibodies produced by the body's own immune system. It has to be given by injection once a month. This has been shown to be effective for some types of inducible urticaria in some studies. In the UK the National Institute for Health and Care Excellence (NICE) has recommended its use for chronic spontaneous urticaria where other treatments have not worked. It has to be given by a hospital consultant.
Treatment with ultraviolet light (phototherapy) can cause an improvement in symptoms but, unfortunately, this may only last for a few months.
Are hives dangerous?
Back to contentsUsually not. The rash is itchy but normally fades within a day or so and causes no harm. Most people with hives (acute urticaria) do not feel too unwell unless they have a cold or flu that is triggering the rash. The cause of the rash is not known in more than half of cases and it is commonly a one-off event.
However, hives may be more serious in the following situations:
Food allergy. If a food allergy is the cause then the rash is likely to return each time you eat the particular food. This is more often a nuisance than serious.
Severe allergies. People who have a severe allergic reaction to peanuts, insect stings, etc, often have an urticarial rash as one of the symptoms. This is in addition to other symptoms such as severe angio-oedema, breathing difficulties, collapse, etc. A severe allergic reaction is called anaphylaxis. Note: most people with acute urticaria feel well and do not have anaphylaxis.
How long do hives last?
Back to contentsInducible urticaria most commonly occurs in healthy young adults. As a rule, hives triggered by physical stimuli tend to improve and become less troublesome with time (often going, or being much less troublesome, after 2-5 years).
Acute hives usually last less than six weeks. Most cases last 24-48 hours and in some cases the rash only lasts a few hours.
Persistent hives tend to come and go. There may be times when the rash appears on most days, and then times when the rash may go away for a while. The severity of the rash and itch varies from person to person. Some things such as heat, cold, menstrual periods, stress, or emotion may make the rash flare up worse than usual.
Symptoms may go away completely after a few months; however, the condition lasts several years in some cases.
In about half of cases, symptoms go within 3-5 years after the condition first starts.
In about 1 in 5 cases the symptoms persist on and off for more than 10 years.
Complications of hives
Back to contentsThere are usually no serious complications, but the itch can be very annoying and difficult to ignore. If skin is scratched excessively then there is a risk of infection.
Frequently asked questions
Back to contentsAre hives contagious?
Hives are not contagious and cannot be passed from person to person. Whilst other causes of a skin rash are contagious, hives aren't.
What's the difference between hives and a rash?
A rash is a broader term for any change in the skin’s colour or texture. Hives are a type of rash that presents as raised, itchy bumps, that often appear suddenly.
Can stress cause hives?
Stress can trigger or worsen hives as it causes the body to release chemicals such as histamine, which leads to a reaction on the skin.
Patient picks for Skin rashes

Skin, nail and hair health
Epidermoid and pilar cysts
Epidermoid and pilar cysts are commonly referred to as 'sebaceous cysts' (pronounced 'seb-ay-shuss'). They are overgrowths of skin cells (called keratin) held together in a little capsule, or sac. They are harmless smooth lumps just under the surface of the skin. They are not cancerous and do not require removal unless they are bothering you by the look or the feel of them. They can occur almost anywhere in the body, but are commonly found on the back or scalp.
by Dr Doug McKechnie, MRCGP

Skin, nail and hair health
Rosacea
Rosacea is a skin condition that affects parts of your face. Symptoms can include facial flushing, facial redness, spots, thickening of your skin, and eye problems such as dry eyes and sore eyelids. Not all symptoms occur in all cases. Rosacea affects about 1 in 20 people in the UK, usually in middle age. Many cases are mild. Spots can usually be cleared with antibiotic treatment. Other treatments may be used for other symptoms. A complication that affects the front of the eye (the cornea) is uncommon but serious. See a doctor urgently if you have rosacea and develop any eye pain or visual problems.
by Dr Rosalyn Adleman, MRCGP
Further reading and references
- Omalizumab for previously treated chronic spontaneous urticaria; NICE Technology Appraisal Guidance, June 2015
- BSACI guideline for the management of chronic urticaria and angioedema; British Society for Allergy and Clinical Immunology (Feb 2015)
- Chronic physical/inducible urticaria; Primary Care Dermatology Society
- Urticaria; NICE CKS, March 2024 (UK access only)
- Chronic urticaria: off-label doses of cetirizine; NICE 2014
- Zuberbier T, Abdul Latiff AH, Abuzakouk M, et al; The international EAACI/GA(2)LEN/EuroGuiDerm/APAAACI guideline for the definition, classification, diagnosis, and management of urticaria. Allergy. 2022 Mar;77(3):734-766. doi: 10.1111/all.15090. Epub 2021 Oct 20.
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Hayley Willacy, FRCGP
General Practitioner, Medical Author
MBChB (1992), DRCOG, DFFP, MRCOG (Part 1) MRCGP (2007), DFSRH (2013), MSc - medical education (2020)
Dr Hayley Willacy was an NHS GP working in northwest England, who retired from clinical practice in 2022 after 30 years.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 19 Jun 2027
20 Jun 2024 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.