Leptospirosis and Weil's disease
Peer reviewed by Dr Doug McKechnie, MRCGPLast updated by Dr Caroline Wiggins, MRCGP Last updated 27 Apr 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Leptospirosis is caused by infection with Leptospira germs (bacteria). The infection passes from animals (commonly rats, cattle, pigs and dogs) to humans. In most cases, leptospirosis causes a mild illness. But, in some people, a more severe illness occurs. This more severe form is commonly referred to as Weil's disease. The main treatment for leptospirosis is antibiotics and most people make a full recovery.
In this article:
Video picks for Other infections
Continue reading below
What is leptospirosis?
Leptospirosis is caused by infection with the germs (bacteria) Leptospira. It is a type of zoonosis infection (an infection that can be passed from animals to humans).
In the majority of cases, leptospirosis causes a mild illness but, in some people, a more severe form of leptospirosis occurs. This more severe form is commonly referred to as Weil's disease.
Leptospirosis symptoms in humans
Back to contentsAs mentioned above, there are two forms of leptospirosis:
A mild form causing a flu-like illness.
A more severe form (Weil's disease).
Around 9 out of 10 people just develop the mild form of the illness.
Symptoms of leptospirosis can start 3 to 30 days after exposure to the germs (bacteria) though most commonly people notice symptoms starting after 7 to 12 days.Some people with mild leptospirosis may develop no symptoms at all.
In both the mild and the severe forms of leptospirosis, flu-like symptoms develop first. They tend to last for between 5 and 7 days and can include:
High temperature (fever) and chills.
Feeling sick (nausea), loss of appetite, being sick (vomiting) and diarrhoea.
Redness of the eyes that looks like conjunctivitis or subconjunctival haemorrhage.
Cough.
Joint and muscle pains (particularly in the calves and lower back).
Feeling tired.
Conjunctivitis appearance
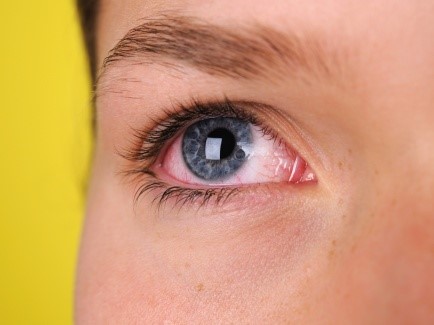
Leptospirosis can mimic the red eye appearance of conjunctivitis
The majority of people then recover as their immune system clears the infection. However, in some people, about a week after the flu-like symptoms have passed, a second stage of the illness then develops (Weil's disease). Symptoms of this second stage can include:
Tummy (abdominal) pain.
Skin rash.
Muscle pains.
Passing very little urine, or a lot more urine than usual.
Shortness of breath.
Swollen hands or feet.
Coughing up blood (haemoptysis).
Some people develop symptoms similar to meningitis.
During this second stage, bacteria begin to infect the organs of the body, such as the kidneys, the liver, the brain, the eyes, the heart and the lungs. Different organs may be infected in different people. However, commonly the kidneys and the liver are affected and kidney or liver failure can occur.
Continue reading below
How common is leptospirosis?
Back to contentsAnimals in countries all over the world carry Leptospira germs (bacteria) but the infection is more common in tropical climates. In the UK, leptospirosis is not very common. Public Health England reports that there are around 50 to 80 cases in England and Wales each year. That is about one case per million people per year.
Leptospirosis has also been reported after episodes of flooding.
How is leptospirosis spread?
Back to contentsBoth wild and domestic animals can become infected with Leptospira, including rats, mice, cattle, pigs and dogs. The germs (bacteria) can live within the animal's kidneys and can be passed out in their urine into water or soil, where they can survive for several months. Often, infected animals show no outward signs of illness.
Leptospirosis can be passed on to humans through direct contact with the bodily fluids or tissues of an infected animal (such as urine) or through contact with contaminated water or soil.
The bacteria can enter the body through a small cut or abrasion in the skin, through mucous membranes such as the skin that lines the mouth, the nose and the front of the eye. The bacteria may also be inhaled and enter the body via the lungs. Once inside the body, Leptospira have the ability to pass via the bloodstream and the lymph system to the internal organs.
Continue reading below
Risk factors
Back to contentsPeople exposed to animals or fresh water are at highest risk of being exposed to the disease. This includes:
Farmers.
Vets.
Abattoir workers.
Rodent control workers.
Sewage workers.
Those who take part in freshwater sports.
Leptospirosis diagnosis
Back to contentsIn the early stages of leptospirosis, it may be quite difficult to tell the symptoms apart from the flu. If you know that you have been in contact with water that was possibly contaminated with animal urine, or if you work with animals, you should tell your doctor and this can help to alert them to the possibility of leptospirosis.
Tests are usually carried out to confirm the diagnosis. You may be asked to provide a urine sample to look for Leptospira in your urine. Blood testing can also confirm the diagnosis by looking for evidence of the germs (bacteria) in your bloodstream. Often, more than one test is required, as it can be difficult to diagnose leptospirosis with laboratory tests.
Other tests may also be done to assess the severity of your illness. For example, blood tests to look for anaemia, to look at the clotting of your blood and to look at how your kidneys and liver are functioning.
Leptospirosis treatment
Back to contentsAntibiotics are the main treatment. Antibiotics are usually prescribed as soon as possible after leptospirosis is diagnosed and in some cases before the diagnosis has been confirmed. In mild leptospirosis, antibiotic tablets may be all that is needed. In more severe cases, antibiotics given into your veins (intravenous antibiotics) are used.
People with mild leptospirosis may be treated at home. Those with the severe form of infection are usually admitted to hospital for treatment and monitoring.
Other supportive treatment may be needed - for example:
Medication, such as paracetamol, to help bring down high temperature (fever) and help reduce muscle pains.
Fluids, which may be given intravenously if you are unable to drink enough and are dehydrated.
How long does leptospirosis last?
Back to contentsAs previously discussed , 9 out of 10 people have a mild form of leptospirosis and the outlook (prognosis) in such cases is very good. Most people recover fully within two to six weeks but some may take up to three months to get better.
In more severe cases (Weil's disease), the outlook depends on which organs of the body are involved and to what extent. People severely affected may die from organ failure or internal bleeding. In one study looking at people who were hospitalised with Weil's disease, 20% of people had ongoing symptoms two years after becoming unwell.
How to prevent leptospirosis
Back to contentsThe best way to prevent leptospirosis is to avoid contact with potentially infected animals and potentially contaminated soil and water. You should avoid swimming or entering water that might be contaminated with animal urine.
Those working with animals that could be infected should wear protective clothing and equipment including thick gloves, eye protection and footwear. They should also pay strict attention to hygiene, including meticulous handwashing after exposure to animals. Rodent control can also help to prevent infection - for example, rubbish disposal and ensuring that rodents cannot get into buildings.
If there is contact with fresh, surface waters (for example, canals, ponds or rivers) then you should:
Cover any cuts, scratches or sores with a waterproof plaster. Thoroughly clean any cuts or abrasions that you may have got during the water activity.
Wear protective clothing such as dry suits, gloves or protective footwear.
Wash or shower as soon as possible after water sports.
Avoid capsize drill or rolling in stagnant or slow-moving water.
Leptospirosis vaccine
Vaccination of some animals is carried out to help to control the infection. No human vaccine against leptospirosis is currently available in the UK.
Patient picks for Other infections

Infections
Pilonidal sinus
A pilonidal sinus is an infected tract under the skin between the buttocks. Treatment commonly involves an operation. After the operation it is advised that the area should be kept the area free of growing hair by regular shaving or other means of hair removal.
by Dr Philippa Vincent, MRCGP

Infections
MRSA
Infection with MRSA bacteria mainly occurs in people who are already ill in hospital. It can be difficult to treat MRSA, as the bacteria are resistant to most types of antibiotic medicines. Many people are carriers of MRSA without even realising it, as MRSA often does not cause symptoms in healthy people.
by Dr Toni Hazell, MRCGP
Further reading and references
- Leptospirosis; Public Health England
- Haake DA, Levett PN; Leptospirosis in humans. Curr Top Microbiol Immunol. 2015;387:65-97. doi: 10.1007/978-3-662-45059-8_5.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 25 Apr 2028
27 Apr 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.