Weight loss surgery
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 20 Mar 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Weight loss surgery can work well to help some people to lose weight. However, it may not be suitable or the right decision for everyone. It is not something to be undertaken without very careful consideration. You need to be fully prepared for weight loss surgery and you need to be highly motivated. When considering surgery you must have a full understanding of what it involves, including the risks and benefits. You should also be aware that you need to make long-term changes to your lifestyle and eating habits after your surgery. If you have surgery abroad or in the private sector in the UK then you should budget for two years specialist follow-up in the private sector.
In this article:
Video picks for Other surgery and procedures
Continue reading below
What is weight loss surgery?
Weight loss surgery is any type of surgery that is carried out specifically to help you lose weight. Weight loss surgery is also called bariatric surgery.
What causes weight gain?
Your weight depends on the balance between your energy intake (the calories in food and drink) and how much energy your body uses (burns) up. It also depends on the type of foods and drinks you consume and how these affect your body's natural tendency to maintain the same weight.
See the separate leaflet called Weight Loss (Weight Reduction).
How does weight loss surgery work?
Back to contentsThe way weight loss surgery works can be:
Surgery which may prevent you from being able to eat so much - for example, by reducing the size of your stomach. This means that you will feel full more quickly and therefore eat less.
Surgery which may change the way your body handles the food that you eat - this surgery can make the food that you eat bypass part of your gut (intestine) so that fewer calories are taken up (absorbed) by your body from food.
Some types of surgery which use a combination of both of these ways.
Some of the different types of weight loss surgery are explained in more detail below.
Weight loss surgery can work well to help some people lose weight. However, it may not be suitable or the right decision for everyone who wants to lose weight. Weight loss surgery should only be undertaken after very careful consideration by a multi-disciplinary team involving different professionals - for example, surgeons, dieticians and psychologists.
You need to be fully prepared for weight loss surgery and you need to be highly motivated. It is important that when considering surgery you have a full understanding of what it involves, including the risks and benefits. Surgery alone does not cure a weight problem. You also have to make long-term changes to your lifestyle and eating habits. Some of these are explained further below.
Note: the separate leaflet called Obesity and Weight Loss provides more general information about being overweight or obese. It describes how to determine if you are overweight or obese, and how to assess your body mass index (BMI).
This leaflet just discusses weight loss surgery.
Continue reading below
When is weight loss surgery considered?
Back to contentsIn the UK, the National Institute for Health and Care Excellence (NICE) has produced some guidance to help doctors decide if someone may be suitable for weight loss surgery on the NHS.
To be considered for weight loss surgery, you need:
To have a BMI of 40 or more, or have a BMI between 35-40 plus a health problem that could be improved if you lost weight. For example, high blood pressure, type 2 diabetes, severe problems with your mobility, or sleep apnoea (difficulties with breathing whilst asleep).
To have been seen and treated by a specialised obesity team, or will receive treatment by such a team.
Already to have tried all other weight loss methods with no success. These include changes to your diet, an increase in your physical activity levels and treatment with medicines.
To have no health problems that may make the operation dangerous for you.
To be able to commit to the long-term medical follow-up that is needed after weight loss surgery, such as healthy lifestyle changes.
Also, NICE says that if you have a BMI of 50 or more, weight loss surgery may be considered as a first option. That is, before you have tried any changes to your diet, increased your physical activity levels or tried treatment with medicines for obesity.
The conditions are different if you have been diagnosed with type 2 diabetes in the previous ten years. If this is the case, you can be considered for weight loss surgery if your BMI is 30-34.9. If your BMI is 35 or more, you should be considered a priority for weight loss surgery, and have a more urgent assessment.
Finally, if you are of Asian origin, you may be considered for weight loss surgery at a lower BMI. This is because the risks of being overweight kick in at a lower BMI in people of Asian origin.
Editor’s note
Dr Krishna Vakharia, 28th July 2023
NICE have updated their guidance to advise consideration of:
A referral for people of South Asian, Chinese, other Asian, Middle Eastern, Black African or African-Caribbean family background using a lower BMI threshold - 37.5 or 32.5 and 37.5 with a health condition named above.
An expedited referral for people of South Asian, Chinese, other Asian, Middle Eastern, Black African or African-Caribbean family background using a lower BMI threshold - BMI 27.5 to 32.5 - who have recent-onset (diagnosed within the past 10 years) type 2 diabetes.
Weight loss surgery availability
Back to contentsThe availability of weight loss surgery may vary in different areas. You need to be referred to a specialised obesity management team. This team works with you in a number of ways to help you with weight loss, and then assesses you for surgery where appropriate.
Private weight loss surgery may also be available but this does cost money. Also, even if you are paying privately for your surgery, it is likely that your surgeon will only operate if you fit certain strict criteria similar to those outlined above. If you have surgery on the NHS, your consultant and their team will provide specialist follow-up for two years. It is crucial that if you have private surgery, in the UK or abroad, you budget for this follow-up in the private sector as it cannot be fully replicated by your GP.
Continue reading below
Can children have weight loss surgery?
Back to contentsMost of the time, surgery for obesity is not recommended in children. It may sometimes be considered in exceptional cases in children who have been through puberty and who are seriously obese. Children and young people being considered for surgery need very thorough assessments by a specialist team. You may choose to discuss this further with your child's doctor. The rest of this leaflet is about weight loss surgery in adults.
See the separate leaflet called Childhood Obesity for more details.
Benefits of weight loss surgery
Back to contentsIn general, weight loss surgery has been shown to be very effective at helping to achieve long-term weight loss. When compared with diet, or with treatment with tablets to help weight loss, weight loss surgery has been shown to produce greater degrees of weight loss in obese people. In fact, for people who are very obese, weight loss surgery may be the most effective treatment.
Losing a lot of weight after weight loss surgery may also have a dramatic effect on improving your health. The effects being:
Type 2 diabetes may be completely reversed in many people who have had weight loss surgery, or, in others, the control of their diabetes may be greatly improved meaning that they need to take less medication.
In seriously obese people, having weight loss surgery means they are likely to live longer.
There is less risk of stroke, heart attacks, some types of cancer and liver disease not connected with alcohol.
People who have had surgery for weight loss are less likely to develop high blood pressure in the future than those having conventional treatment for their weight loss and some may be able to stop the tablets that they were previously taking for high blood pressure.
Some of the different types of weight loss surgery (discussed below) may enable more weight loss in the long term than others. However, these operations may be more complex and may carry more in the way of risks than some of the more straightforward ones.
Risks of weight loss surgery
Back to contentsNo surgery is without risk and so having weight loss surgery does carry risks. These are:
Developing a blood clot on the lung (pulmonary embolism).
Developing a blood clot in a vein (deep vein thrombosis).
Infection in the lung (at the time of surgery).
Infected skin wound (after surgery).
Gastric band slipping out of place.
Excess skin.
Death during surgery.
The risks vary according to your age, your sex and your BMI and they will be fully explained to you before surgery. Also, in some people, the operation may not always be successful in helping them lose weight.
Having a general anaesthetic, which is necessary for all types of bariatric surgery, also carries risks. The risks from an anaesthetic are greater if you are obese.
How to reduce risks after weight loss surgery
Medication can be given to help with some of the risks. Getting up and about quickly after the operation can also help reduce the risk.
If you lose a lot of weight rapidly following weight loss surgery, you can be more likely to develop stones in your gallbladder (gallstones).
There are also other risks or complications that vary depending on the type of surgery that you have. These are discussed further below.
Types of weight loss surgery
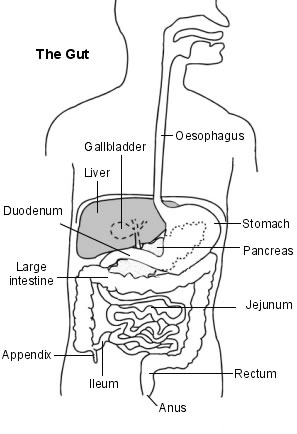
Back to contentsThere are various different types of weight loss surgeries , each with their own advantages and disadvantages. The type of surgery that may be best for you can depend on your weight, any health issues that you may have and the experience of your surgeon. The diagram below is of the normal gut structure (anatomy). This may help when some of the operations are described.
Digestive system
Gastric band surgery
This is a common type of weight loss surgery that is carried out. During gastric band surgery, a special band is placed around the upper part of your stomach, essentially dividing your stomach into two.
When you eat, food passes from your gullet (oesophagus) into the part of your stomach above the band. Because this upper section is smaller than the size that your whole stomach was previously, you will need to eat less than before to feel full. After eating, the food then gradually passes through to the section of your stomach below the band and is digested as normal.
Gastric bands are designed so that their position can be adjusted after the surgery and so the amount of food that you are able to eat can be changed. The band is connected to a special port under your skin to allow this adjustment. Adjustments may be needed in the first few months after your surgery so that the setting that is best for you can be found.
These adjustments can usually be made quickly in an outpatient clinic and you do not need another general anaesthetic or operation. Another advantage of gastric band surgery is that is can usually be carried out using 'keyhole' surgery (laparoscopic surgery). This means a quicker recovery time afterwards. This surgery is also reversible. The band can be removed at a later date if required. However, there would then be a risk that you might put the weight back on.
Gastric band surgery is generally one of the safest types of surgery for weight loss. However, the surgery does still carry some risks and complications. Sometimes a gastric band can slip out of place or it may wear through (erode) the wall of your stomach and become ineffective. A gastric band may also wear out and need replacing at a later date.
However, these problems do not happen in everyone. If they do occur, another operation may be needed to replace the band. Also, for some people, it make take up to two years to get used to their gastric band and modify their eating habits so that they lose weight effectively.
Gastric bypass surgery
Commonly, an operation called a Roux-en-Y gastric bypass is done. During the surgery, your stomach is divided into two, creating a small upper stomach pouch. A part of your upper bowel (small intestine) is then connected to this stomach pouch. This means that when you eat, food bypasses the main part of your stomach and the upper part of your small intestine.
In this upper part of your small intestine, your food would normally start to be digested and taken up (absorbed) by your body. So, with this part of your intestine being bypassed, fewer calories are taken up from the food that you eat. Also, because the new stomach pouch that is created is smaller than the size of your whole stomach, the amount of food that you are able to eat is reduced, thereby restricting calories that you take in.
This operation is again mostly done using keyhole surgery and a general anaesthetic is needed. One of the main risks of gastric bypass surgery is that a leak may develop at the point where your small intestine is connected to your stomach. However, this is rare. If it does occur, further surgery will be needed to repair the leak.
Also, because a part of your intestine is bypassed during the surgery, you may develop a lack (deficiency) of some vitamins and minerals as a result of the surgery. For this reason, blood tests will usually be suggested to look for deficiencies and you will be given supplements if needed.
Gastric bypass surgery may lead to greater weight loss in some people than gastric band surgery but it is more difficult surgery that takes longer to carry out. Studies have found however that it is particularly beneficial to people with type 2 diabetes.
Sleeve gastrectomy
During a sleeve gastrectomy, most of one side of your stomach is removed so that you are left with a smaller 'sleeve' of stomach, which is essentially a narrow tube. This remains connected to your gullet (oesophagus) above and the first part of your intestine below.
So, again, the size of your stomach is made smaller (but in this case it is irreversible), meaning that you can only eat a much smaller meal. You will also feel fuller for a longer period of time after you have eaten. Again, this type of surgery can usually be done using a keyhole procedure.
A sleeve gastrectomy is relatively easier and quicker for surgeons than some other types of weight loss surgery. However, it may be slightly less effective than some other operations in terms of the amount of weight loss that someone can have afterwards. For this reason, it is sometimes done as a first operation in people who are very obese and who may have health issues making longer, more complex surgery more risky.
Then a second operation may be suggested at a later date. For example, to convert a sleeve gastrectomy to a gastric bypass. However, some people may not need a second operation, as they may lose enough weight with just a sleeve gastrectomy.
Biliopancreatic diversion
During this operation, most of your stomach is removed, leaving just a small stomach pouch behind. This pouch is then connected to the last part of your small intestine so that the majority of your small intestine is bypassed. At the same time, your bile duct and your pancreatic duct (which normally drain bile and pancreatic enzymes into the upper part of your small intestine to help with the digestion of food) are rerouted into the lower part of your small intestine.
Diagram showing detail around the pancreas
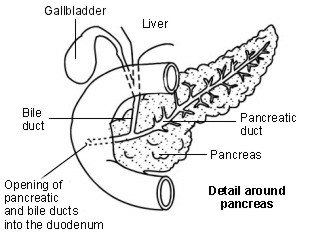
The diagram above shows the normal structures before the rerouting.
Most of the fat and carbohydrate that you eat is normally absorbed by your body in the upper part of your small intestine. So, after this surgery where this part of your intestine is bypassed, most of the fat and carbohydrate that you eat in your diet passes through your body and is not absorbed.
One of the disadvantages of this type of surgery is that is can cause wind (flatulence) and loose, foul-smelling stools (faeces). A biliopancreatic diversion involves quite complex surgery and surgeons need to be experienced in the procedure. Therefore, this type of surgery is not available in all hospitals.
Duodenal switch
This operation is similar to biliopancreatic diversion. The surgeon starts by carrying out a sleeve gastrectomy (see above). Then the upper part of your small intestine (called the duodenum) is cut and the lower half of your small intestine is connected to the remaining part of your duodenum.
Your bile duct and pancreatic duct are then rerouted into the lower part of your small intestine as with a biliopancreatic diversion. During this type of surgery, your body is less able to digest the fat that you eat and to absorb calories from fat. This leads to weight loss but your diet does not have to change too dramatically.
A duodenal switch operation can be very successful in terms of the amount of weight loss that you can have afterwards. However, this is complex surgery and it needs to be carried out by an experienced surgeon. Therefore, this type of surgery is not available in all hospitals. The surgery takes longer and has an increased risk of some complications.
It will usually mean that you need to stay in hospital for a longer period compared with some of the other types of surgery. As you are asleep under a general anaesthetic for longer, there is an increased risk of developing a blood clot in your leg or on your lungs. There is also a risk of leakage where the intestine is joined up, as with a gastric bypass operation.
Side-effects can include offensive-smelling, loose stools and lots of flatulence if you do not stick to a low-fat diet. Also, this type of surgery can lead to some vitamin and mineral deficiencies and supplements of these may be needed. A duodenal switch operation can also interfere with the amount of protein that your body is able to absorb from food.
Protein is important and is needed by our body to help form the structure of our muscles, tissues and organs. Protein is also needed to make various enzymes and hormones. Sometimes, a lack of protein absorbed by the body after a duodenal switch operation can lead to a condition called protein calorie malnutrition which can make you very unwell. For this reason, people who have had a duodenal switch operation are advised to eat a larger amount of protein in their diet.
Other procedures to help weight loss
Back to contentsThere are some other procedures that are being carried out to help with weight loss which are not strictly surgical operations. Not all of these are available on the NHS. They may sometimes be discussed with you by your surgeon if they have received special funding for these procedures on the NHS as part of research project.
They may also be an option if you are seeing a surgeon privately. If these are an option, you should discuss the procedures in full with your surgeon, including their risks and benefits. Such procedures include:
An intragastric balloon
A special telescope (called an endoscope) is passed through your mouth, down your oesophagus and into your stomach. This allows a special silicone balloon to be inserted into your stomach. The balloon is filled with liquid so that is fills an area of your stomach. With the balloon in place, it can make you feel full more easily and so reduces the amount of food that you are able to eat. However, this is only a short-term option, as the balloon needs to be removed after a maximum of six months.
A balloon can also be inserted without the use of an endoscope, using new technology whereby the patient swallows the balloon and then has an X-ray to check that it is in the right place. The balloon lasts for four months and is then passed naturally in the stools. This is currently recommended by NICE for people who need to lose weight in the short term, but only as part of a clinical trial for those looking for longer-term weight loss.
Intragastric stimulation
Two electrodes are planted into the wall of your stomach, using keyhole surgery. These are joined to a special stimulator that sits under the surface of your skin. The stimulator sends out electrical impulses to the electrodes in your stomach. It is thought that this then sends messages to your brain, telling your brain that you are full and therefore reducing the amount of food that you eat.
Primary obesity surgery endolumenal (POSE)
This new type of weight loss surgery is carried out using an endoscope. An endoscope is a flexible tube with a camera attached that also has a number of channels through which surgical instruments can be passed.
During the surgery, the endoscope is fed through your mouth and into your stomach and the surgeon operates through the channels to make your stomach smaller so that you will feel full more quickly. Because there are no cuts (incisions) into your tummy (abdomen) to reach your stomach, you are likely to recover much more quickly and will not need to stay in hospital for as long.
The procedure is also less painful than conventional weight loss surgery. Apart from balloon insertion, endoscopic surgery is not available on the NHS but is provided by some private clinics.
Which procedure would be best for me?
Back to contentsThe balance between benefits and risks varies from person to person and this is something you should discuss with your surgeon. However, some guidance can be obtained from research looking at the outcome of various procedures.
Recent studies have found that surgery is an effective means of losing weight.whatever the procedure used. Roux-en-Y gastrectomy and sleeve gastrectomy both had better outcomes than adjustable gastric banding. For people with very high BMI, duodenal switch resulted in greater weight loss than Roux-en-Y gastrectomy.
What happens before the surgery?
Back to contentsBefore the surgery, you will be seen by a team including a number of different healthcare professionals. For example, a surgeon, an anaesthetist, specialist nurses, dieticians, a psychiatrist, a hormone specialist (endocrinologist), etc.
It is important that you have full discussions with the team so that you can decide which is the best type of surgery for you, and what the surgery will entail. You will also discuss the risks and benefits of the surgery in your situation, and changes that you will have to make to your diet and lifestyle afterwards.
You may like to ask the surgeon about their experience. How many operations of this type have they done? What is their success rate: how much weight do people generally lose and how long do they keep the weight off for? What complications have people undergoing this type of surgery had? What support and follow-up will you have afterwards?
You may also need to have some investigations to make sure that it is safe for you to have the surgery. For example, these may include tests of your heart and lungs.
You may find it helpful to join a support group and meet up with other people who are waiting for, or who have been through, weight loss surgery. This will give you the opportunity to discuss with other people their experiences surrounding weight loss surgery.
Recovering after weight loss surgery
Back to contentsAfter weight loss surgery, you will need close follow-up. NICE advises that you should be followed up by the specialist team for two years. You will then have annual checks done by your GP.
Diet and exercise
It is essential that you follow eating and exercise guidelines that you are given. After the surgery, in order to lose weight, you will need to change your eating habits. You will need to reduce the amount of food that you eat compared with what you used to eat before the surgery.
You will be given strict guidelines about what to eat in the first few weeks after surgery. Initially, this may be liquids such as unsweetened fruit juices, tea, coffee, smooth soups and build-up drinks. Then, gradually, you will be able to build up to softer foods such as scrambled eggs, pasta, yoghurts, etc and then more textured food. It is important that you eat a healthy balanced diet.
Taking supplements
Because you will not absorb certain vitamins and minerals in the same way after your operation, you will need to take some supplements as advised by the specialist team. The levels of these will be monitored for the rest of your life. This includes blood tests for your levels of iron, calcium, copper, zinc, vitamin D and vitamin B12.
Other medications
Some other medications won't be absorbed in the same way after you have surgery, and so may need to be changed. This is particularly an issue for contraceptive pills, so if you are a woman who needs contraception, you may be advised to change to a non-oral method such as the implant or coil.
Mental health
Some people find that the changes that they need to make to their diet and lifestyle after surgery for weight loss are difficult to come to terms with. You can receive help and guidance about what to eat from the team of specialists that will be looking after you. Depending on the operation that you had, you may also be advised to take some vitamin and mineral supplements.
Remember, the surgery won't work all by itself to help you lose weight. You need to work with it. You need to be aware that you will need lifelong medical follow-up after weight loss surgery. You may find being part of a support group helpful.
Excess skin
For some people, having bariatric surgery and losing weight quickly will leave them with excess skin in areas of the body such as the abdomen, thighs and upper arms. Removal of this skin would require another operation which is often not funded on the NHS. Criteria for provision of this surgery on the NHS vary from area to area.
Dr Hazell has worked on several eLearning modules on obesity for the Royal College of General Practitioners (RCGP), many of which were funded by pharmaceutical companies which make drugs for obesity. The RCGP at all times retained full editorial control over the content of these modules. Dr Hazell has no shares or direct financial interests in any such companies.
Patient picks for Other surgery and procedures

Surgery and procedures
Arthroscopy and arthroscopic surgery
Arthroscopy is a surgical procedure which uses a thin telescope with a light source (an arthroscope) to look inside joints. As well as being able to look inside, the surgeon can use an arthroscope to perform keyhole surgery. Arthroscopy is most often used to investigate or treat knee problems. Arthroscopy can also be used for other joints, including the shoulder, hip, elbow, wrist and ankle joints, and even for hand or foot problems. Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor or local hospital.
by Dr Rachel Hudson, MRCGP

Surgery and procedures
Video-assisted thoracoscopic surgery
Video-assisted thoracoscopic surgery (VATS) is a surgical procedure that allows doctors to see inside the chest and lungs. It is a form of 'keyhole' surgery which can be used to do a number of different surgical procedures. Note: the information below is a general guide only. The arrangements, and the way tests are performed, may vary between different hospitals. Always follow the instructions given by your doctor or local hospital.
by Dr Laurence Knott
Further reading and references
- Sjostrom L; Review of the key results from the Swedish Obese Subjects (SOS) trial - a prospective controlled intervention study of bariatric surgery. J Intern Med. 2013 Mar;273(3):219-34. doi: 10.1111/joim.12012. Epub 2013 Feb 8.
- Colquitt JL, Pickett K, Loveman E, et al; Surgery for weight loss in adults. Cochrane Database Syst Rev. 2014 Aug 8;8:CD003641. doi: 10.1002/14651858.CD003641.pub4.
- Spaniolas K, Pories WJ; Surgery for type 2 diabetes: the case for Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2016 Jul;12(6):1220-4. doi: 10.1016/j.soard.2016.02.036. Epub 2016 Mar 2.
- Li SH, Wang YJ, Zhang ST; Development of Bariatric and Metabolic Endoscopy. Chin Med J (Engl). 2018 Jan 5;131(1):88-94. doi: 10.4103/0366-6999.221283.
- Choi HS, Chun HJ; Recent Trends in Endoscopic Bariatric Therapies. Clin Endosc. 2017 Jan;50(1):11-16. doi: 10.5946/ce.2017.007. Epub 2017 Jan 30.
- Swallowable gastric balloon capsule for weight loss; NICE Interventional procedures guidance, November 2020
- Obesity: identification, assessment and management; NICE Clinical guideline, November 2014 - last updated July 2023
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 7 Feb 2028
20 Mar 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.
