Diabetes insipidus
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Doug McKechnie, MRCGPLast updated 23 Aug 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Diabetes insipidus is a rare condition where the body is unable to control the balance of water. People with diabetes insipidus become very thirsty and pee a lot.
At a glance
Diabetes insipidus is a condition where the body cannot control its water balance, causing excessive urination and thirst.
It is different from type 1 and type 2 diabetes (diabetes mellitus).
Symptoms include passing large amounts of urine (polyuria) and feeling very thirsty (polydipsia).
Dehydration and salt imbalances in the blood are possible complications.
See a doctor if you or your child have symptoms like extreme thirst or passing a lot of urine.
Seek urgent medical help for severe dehydration symptoms like confusion or dizziness.
In this article:
Video picks for Other hormone problems
Continue reading below
What is diabetes insipidus ?
Diabetes insipidus is a different condition to type 1 diabetes and type 2 diabetes (diabetes mellitus, usually just called 'diabetes'). They were given similar names because they can have similar symptoms, but they are very different illnesses.
Diabetes insipidus occurs when the body can't control the balance of water. In diabetes insipidus, the kidneys lose control of how much water passes out in urine (pee). People with diabetes insipidus therefore pass large amounts of dilute urine, meaning they have to pee a lot. The medical word for passing large volumes of urine is polyuria.
This means that people with diabetes insipidus lose a lot of fluid in their urine. They become very thirsty as a result, and drink large amounts of water. The medical word for drinking lots of water is polydipsia.
People with diabetes insipidus can become dehydrated easily. The levels of salts in their blood - particularly sodium - can become too high.
There are four types of diabetes insipidus (described below):
Cranial diabetes insipidus, which is caused by a problem in the brain.
Nephrogenic diabetes insipidus, which is caused by a problem in the kidney.
Gestational diabetes insipidus, which occurs in pregnancy.
Dipsogenic diabetes insipidus, which is caused by a different problem in the brain that makes people drink too much water.
Cranial diabetes insipidus
Back to contentsCranial diabetes insipidus occurs due to a problem in the brain.
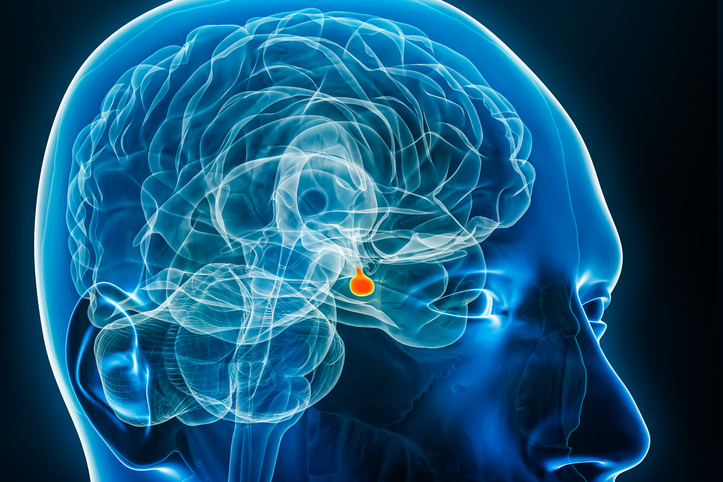
The brain normally produces a hormone called antidiuretic hormone (ADH), also known as vasopressin. ADH is made in a part of the brain called the hypothalamus, and transported to another part of the brain, the pituitary gland, from which it is released into the blood. ADH causes the kidneys to retain water in the body, and produce concentrated urine.
Cranial diabetes insipidus occurs when there is damage to the hypothalamus or pituitary gland, causing less ADH to be released. Lower levels of ADH mean the kidneys lose more water, producing large amounts of dilute urine.
Causes of cranial diabetes insipidus include:
Head injury.
Cancerous (malignant) or non-cancerous (benign) tumours of the brain or pituitary gland.
Damage from surgery to the brain near the pituitary gland and hypothalamus.
Idiopathic diabetes insipidus, when no clear cause is found.
This accounts for about one-third of people with diabetes insipidus.
It's thought that this may be due to an auto-immune problem.
Brain infections including encephalitis and meningitis.
Brain damage from lack of oxygen, which can happen if someone's heart stops (cardiac arrest).
Rare inherited conditions, such as familial cranial diabetes insipidus and Wolfram syndrome.
Continue reading below
Nephrogenic diabetes insipidus
Back to contentsNephrogenic diabetes insipidus happens when ADH is still being produced, but the kidneys aren't responding to it. So, the kidneys produce large amounts of diluted urine, and lose lots of water from the body.
Causes of nephrogenic diabetes insipidus include:
Rare inherited (genetic) conditions.
Medications, particularly lithium, a medication used to treat bipolar disorder. Roughly 1 in 5 people taking long-term lithium develop some level of nephrogenic diabetes insipidus.
Persistently high levels of calcium in your blood. This seems to stop the kidneys from being able to produce concentrated urine.
Persistently low levels of potassium in the blood. This has the same effect.
Other medical conditions, such as sickle cell disease or polycystic kidney disease.
Gestational diabetes insipidus
Back to contentsThis occurs in pregnant women, but is rare. When it does happen, it usually starts in the third trimester of pregnancy and goes away within a few weeks after giving birth.
It's caused by excessive breakdown of ADH by an enzyme produced by the placenta.
This is more likely to happen in women who are pregnant with more than one baby, as they have more placental tissue, which produces more of the enzyme. The liver also helps to control enzyme activity, so pregnant women with liver problems may be more likely to develop it.
It often goes undiagnosed, because most women find that they pee more often during pregnancy, and the symptoms may just be thought to be normal.
Continue reading below
Dipsogenic diabetes insipidus
Back to contentsDipsogenic diabetes insipidus happens when people drink excessive amounts of fluids.
This can happen because the part of their brain that controls the sensation of thirst is not working properly, meaning that they feel very thirsty (and drink fluids) even when they shouldn't.
This can be caused by:
Damage to the hypothalamus (part of the brain) by a head injury, surgery, infections, or tumours.
Mental health conditions, such as schizophrenia.
How common is diabetes insipidus?
Back to contentsDiabetes insipidus is quite rare. It affects about 1 in 25,000 people. It can happen at any age, but tends to be seen more often in adults. Inherited causes of diabetes insipidus are usually diagnosed in childhood.
Diabetes insipidus symptoms
Back to contentsThe main symptoms of diabetes insipidus are:
Passing large amounts of urine (polyuria).
People with diabetes insipidus may pass between 3 and 20 litres of urine per day.
This can cause people to pass urine frequently (up to every half an hour), including waking up at night frequently to pass urine.
Feeling very thirsty and drinking a lot of fluids (polyuria).
These symptoms can significantly affect people's daily lives. Lack of sleep can make them tired, irritable, and affect their concentration during the daytime.
Sometimes people get symptoms of dehydration, such as:
Headaches.
A dry mouth, lips, and tongue.
Dry skin.
Lightheadedness.
Muscle cramps.
Feeling weak.
Confusion.
In severe cases, unconsciousness and fainting.
Symptoms in children
Older children with diabetes insipidus also get excessive thirst and the need to pass urine frequently. In younger children, particularly children who are too young to communicate that they feel thirsty, symptoms can include:
Poor growth and weight loss.
Irritability and excessive crying.
Fevers.
Constipation.
Older children may have:
Problems with bedwetting at night - although diabetes insipidus is a rare cause of bedwetting, and most children with bedwetting do not have it.
Incontinence of urine during the daytime.
Poor growth
Loss of appetite.
Tiredness and fatigue.
Complications of diabetes insipidus
Back to contentsThe two main complications of diabetes insipidus are:
Dehydration.
Electrolyte (salt) imbalance in the blood, such as dangerously high sodium levels.
Diabetes insipidus can be life-threatening if it is not diagnosed and treated early enough.
How is diabetes insipidus diagnosed?
Back to contentsDiabetes insipidus is usually suspected on the basis of typical symptoms and because of other things; for example, if someone has had a recent head injury or brain surgery. Further tests are needed to confirm the diagnosis. These can include the following:
Blood and urine tests
For example:
To check the levels of sodium and potassium salts in the blood. These can be high in diabetes insipidus.
To check the level of sugar (glucose) in the blood and urine. This should be normal in diabetes insipidus. It will be high in diabetes mellitus (which can also cause excessive thirst and urination).
To check how concentrated the urine is. In diabetes insipidus, the urine will be very diluted.
A water deprivation test
This is a special test where people avoid drinking any water or other fluids for a certain period of time (usually around 6-8 hours). The volume of urine that they produce is measured, along with regular blood and urine samples to measure how concentrated their blood and urine is.
Normally, people who have not drunk any fluids for a long time produce less urine, and their urine becomes more concentrated. People with dipsogenic diabetes insipidus also show this response; the main problem is that they're drinking too much water, so, when they stop drinking for a long period, they stop urinating as much, and their blood and urine tests return to normal.
People with craniogenic or nephrogenic diabetes insipidus, however, continue to pass large volumes of dilute urine even when they haven't drunk any fluids for several hours.
Antidiuretic hormone test
A further test, after the water deprivation test, can determine whether someone has cranial or nephrogenic diabetes insipidus.
After the period of fluid deprivation, a medicine called desmopressin (which is very similar to ADH) is given.
In cranial diabetes insipidus, the desmopressin replaces the missing ADH, and so the volume of urine will reduce and it will become more concentrated.
In nephrogenic diabetes insipidus, the kidneys don't respond to desmopressin, meaning that the person will continue to pass large volumes of dilute urine.
Other tests
Other tests may sometimes be suggested to look for possible causes of diabetes insipidus. For example, a magnetic resonance imaging (MRI) scan of the brain and pituitary gland.
Diabetes insipidus treatment
Back to contentsCranial diabetes insipidus
The underlying cause of cranial diabetes insipidus may need treating first; for example, if there is a tumour affecting this hypothalamus or pituitary gland.
Otherwise, the following may be suggested:
Careful control of fluid intake. In mild cases, cranial diabetes insipidus may be controlled by drinking enough fluid to quench thirst and to keep salt levels in thirst blood stable. Sometimes, this may be the only treatment required.
Desmopressin. This is a manufactured form of ADH. It can have the same effect as ADH on the kidneys. It comes as tablets, a nasal spray, melts that dissolve in the mouth, and injections. For more information see the separate leaflet called Desmopressin.
Sometimes cranial diabetes insipidus only lasts for a short period (perhaps a few weeks) after a head injury or brain surgery and so treatment may only be needed in the short term. However, other causes may mean that lifelong treatment is required for diabetes insipidus.
Nephrogenic diabetes insipidus
Treatments for nephrogenic diabetes insipidus include:
Treating the underlying cause, if possible.
Medications, such as lithium, are a common cause. It may be possible to stop or change the medication.
However, this needs to be done carefully, as the medication may have other important benefits.
Stopping or changing medication should only be done in agreement with your doctor.
Eating a low-sodium and low-protein diet. This can help to reduce urine volume.
Don't make dietary changes without consulting with your doctor first.
Medications may be required for more severe cases. These include:
Thiazide diuretics. Normally, these cause people to produce more urine, but they can have the opposite effect in nephrogenic diabetes insipidus.
Non-steroidal anti-inflammatory drugs (NSAIDs).
Desmopressin. Although this shouldn't have much effect in nephrogenic diabetes insipidus, where the problem is not due to a lack of ADH, some people do get a partial response to desmopressin, and it is sometimes used if other treatments are not working.
What is the difference between diabetes insipidus and diabetes mellitus?
Back to contentsDiabetes insipidus and diabetes mellitus are very different conditions, but have some symptoms in common. Diabetes mellitus, which includes type 1 and type 2 diabetes, is much more common than diabetes insipidus.
Both diabetes mellitus and diabetes insipidus can cause people to feel very thirsty and pass lots of urine.
In diabetes mellitus, this happens when blood glucose (sugar) levels become very high. Some of this excess glucose leaks into the urine. This pulls more water into the urine, meaning that people with very high blood glucose levels produce large amounts of urine, and feel thirsty because of fluid loss.
In diabetes insipidus, this happens because kidneys are unable to produce concentrated urine (see above for a detailed explanation of why this happen). Blood sugar levels are normal.
Diabetes insipidus and diabetes mellitus have similar names for historical reasons.
The ancient Greeks used the term 'diabetes' to describe conditions where people were very thirsty and passing large amounts of urine.
Doctors noticed that people with diabetes often had sweet-tasting urine (doctors don't taste urine samples any more!), and named the condition 'diabetes mellitus' - mellitus meaning 'sweet' in Latin.
Later, it was noticed that some people produced large amounts of dilute urine that didn't taste sweet; scientists realised this was a different condition, which they called 'diabetes insipidus' - insipidus meaning 'tasteless' in Latin.
Other considerations
Back to contentsTreatment for diabetes insipidus is very effective, but people with diabetes insipidus should take care in certain situations.
Always follow the advice of your endocrinologist.
General points to consider include:
Consider wearing an alert bracelet or having a medical alert on your phone, so that medical professionals know you have diabetes insipidus and take medication (if applicable), if you become too unwell to tell them.
Various charities, such as the Pituitary Foundation, make alert cards that explain to emergency clinicians what diabetes insipidus is, what your usual treatment is, and what emergency treatment they should give. See Further Reading, below.
If you use desmopressin nasal spray: switch to desmopressin tablets or melts if you have a heavy cold, blocked nose, or sinusitis, to ensure that you get the full dose.
Dehydration can be very serious, and even life-threatening, for people with diabetes insipidus.
If you develop diarrhoea or vomiting, drink plenty of fluids (small sips are better) to keep hydrated and replace the fluid you're losing. Seek medical attention if you have severe vomiting or diarrhoea, or are unable to keep fluids and medication down.
If you have a fever, or it's a hot day, ensure you maintain your fluid intake and consider drinking more to replace what you're losing through sweat.
If you normally take desmopressin, and have missed it or are unable to take it, drink water until you are no longer thirsty.
Seek urgent medical attention if you are developing symptoms of dehydration, such as severe headaches, drowsiness, confusion, muscle cramps, or reduced consciousness.
Drinking too much can also be dangerous, particularly if you are taking desmopressin. This can lead to water overload, causing your blood sodium levels to drop dangerously low.
If you have taken more than your usual dose of desmopressin, limit your fluid intake until your urine output is back to normal. Allow yourself to become thirsty and pass excess urine before taking the next dose of desmopressin. The same advice applies if you have taken your normal dose of desmopressin, but then drunk a lot of fluids.
Seek urgent medical attention if you have vomiting, headaches, confusion, drowsiness, convulsions or seizures.
When to see a doctor
Back to contentsAlways see a doctor if you, or your child, have symptoms of diabetes insipidus, such as feeling very thirsty, drinking lots of fluids, or passing large amounts of urine.
Patient picks for Other hormone problems

Hormones
Acromegaly
Acromegaly is a rare, progressive condition in which you make too much growth hormone. This causes a range of symptoms that develop gradually, often over several years. The most noticeable symptoms are that your hands and feet become larger and features of your face may become more prominent. The cause is usually a small non-cancerous growth (tumour) in the pituitary gland. Treatment options include surgery to remove the growth and medicines to block the release or effects of growth hormone.
by Dr Mohammad Sharif Razai, MRCGP
Hormones
Pituitary gland disorders
This leaflet gives a brief overview of the pituitary gland and the hormones it makes. The pituitary gland is found at the base of the brain and is 'pea-sized'. The pituitary gland is an overall controller of a number of other glands in the body, overseeing the function of these organs through hormones.
by Dr Hayley Willacy, FRCGP
Frequently asked questions
Can diabetes insipidus be cured, or is it a lifelong condition?
The duration of diabetes insipidus varies depending on its cause. For example, cranial diabetes insipidus might only be temporary, lasting a few weeks after a head injury or brain surgery, meaning short-term treatment is sufficient. However, other causes of diabetes insipidus, across all types, may require ongoing, lifelong treatment.
What is the role of diet in managing nephrogenic diabetes insipidus?
For nephrogenic diabetes insipidus, eating a diet low in sodium (salt) and protein can help reduce the volume of urine produced. However, it's important not to make any changes to your diet without first consulting with your doctor.
Are there any specific concerns for pregnant women with gestational diabetes insipidus?
Gestational diabetes insipidus is rare and typically starts in the third trimester, resolving within a few weeks after birth. It happens because an enzyme from the placenta breaks down ADH too much. It's more likely in women pregnant with multiple babies due to more placental tissue, or in those with liver problems. It can often go undiagnosed as its symptoms, like increased urination, might be mistaken for normal pregnancy changes.
What should I do if I experience symptoms of dehydration or over-hydration?
Dehydration can be serious. If you have severe vomiting or diarrhoea, can't keep fluids or medication down, or experience symptoms like severe headaches, drowsiness, confusion, muscle cramps, or reduced consciousness, seek urgent medical attention. If you are taking desmopressin and drink too much, which can lead to dangerously low blood sodium, limit fluid intake until urine output returns to normal. Allow yourself to feel thirsty before the next desmopressin dose. Seek urgent medical attention if you have vomiting, headaches, confusion, drowsiness, or seizures.
How does desmopressin work and when is it used?
Desmopressin is a manufactured form of antidiuretic hormone (ADH) that mimics the effects of ADH on the kidneys, helping them retain water and produce concentrated urine. It is typically used to treat cranial diabetes insipidus, where the body doesn't produce enough ADH. While it isn't expected to have much effect in nephrogenic diabetes insipidus (where the kidneys don’t respond to ADH), some individuals may experience a partial response, and it may be used if other treatments are ineffective. It's available as tablets, nasal sprays, melts, and injections.
Why is it important to wear an alert bracelet if I have diabetes insipidus?
Wearing an alert bracelet or having a medical alert on your phone is important. In emergencies, if you become too unwell to communicate, it informs medical professionals that you have diabetes insipidus and if you take medication. Charities such as the Pituitary Foundation also provide alert cards that explain your condition, your usual treatment, and emergency care instructions to clinicians.
If I have a blocked nose, can I still use my desmopressin nasal spray?
No, if you use desmopressin nasal spray and have a heavy cold, a blocked nose, or sinusitis, it's advised to switch to desmopressin tablets or melts. This ensures that you receive the full and correct dose of your medication.
Further reading and references
- The Pituitary Foundation
- Ananthakrishnan S; Diabetes insipidus in pregnancy: etiology, evaluation, and management. Endocr Pract. 2009 May-Jun;15(4):377-82. doi: 10.4158/EP09090.RA.
- Di Iorgi N, Napoli F, Allegri AE, et al; Diabetes insipidus--diagnosis and management. Horm Res Paediatr. 2012;77(2):69-84. doi: 10.1159/000336333. Epub 2012 Mar 16.
- Saifan C, Nasr R, Mehta S, et al; Diabetes insipidus: a challenging diagnosis with new drug therapies. ISRN Nephrol. 2013 Mar 24;2013:797620. doi: 10.5402/2013/797620. eCollection 2013.
- Valenti G, Tamma G; History of Diabetes Insipidus. G Ital Nefrol. 2016 Feb;33 Suppl 66:33.S66.1.
- Sick day rules; The Pituitary Foundation, 2023.
Continue reading below
About the authorView full bio

Dr Doug McKechnie, MRCGP
Medical Writer
MA, MBBS, MSc, DRCOG, MRCP(UK), MRCGP(2021), FHEA
Dr Doug McKechnie is an NHS GP working in London. He works full-time clinically and is also the Deputy Lead for the Clinical and Professional Practice module at University College London Medical School.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 21 Aug 2028
23 Aug 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.