Lyme disease
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 24 May 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Lyme disease is an infection caused by being bitten by an infected tick. The first and most common symptom is a rash that spreads out from the site of the tick bite. Left untreated, the germs (bacteria) can spread to other areas of the body. In some cases this can cause serious symptoms - often months after the initial tick bite. A course of antibiotic medication will usually clear the infection.
In this article:
Video picks for Other infections
Continue reading below
What is Lyme disease?
Lyme disease is an illness caused by being bitten by a tick that is infected with a germ (bacterium) called borrelia. There are various types of this bacterium but Borrelia burgdorferi causes Lyme disease.
There are different types of Borrelia burgdorferi occurring in different parts of the world. The different types cause different patterns of illness. For example, the typical case of Lyme disease in America may be different to the typical case in the UK.
Lyme disease symptoms
Back to contentsThe symptoms and effects of Lyme disease can be divided into three stages:
Stage one symptoms - early reaction to the local skin infection
A rash and flu-like symptoms are early symptoms of Lyme disease. These can develop at any time between 3 and 30 days after being bitten by an infected tick.
Erythema migrans 'bullseye" rash of Lyme disease
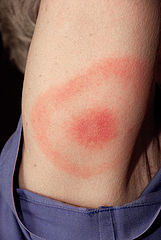
© CDC/James Gathany, Public domain, via Wikimedia Commons
Rash
The classical symptom of Lyme disease is a typical rash called erythema migrans. In the UK, most people with Lyme disease have or have had this rash. In the USA, 70% of people with confirmed Lyme disease have the typical erythema migrans rash.
The rash is usually a single circular red mark that spreads outwards slowly over several days. The circle becomes bigger and bigger with the centre of the circle being where the tick bite occurred. As it spreads outwards, a paler area of skin emerges on the inner part of the circle.
Therefore, the rash is often called a 'bullseye' rash. Some types of the germ (bacterium) do not cause a rash, or the rash is different. For example, in the USA, the rash is less likely to have the 'bullseye' appearance.
The rash usually spreads over at least 5 cm but may be much bigger.
The rash is not usually painful or particularly itchy. It might not be noticed if it is on the back. Without treatment, erythema migrans typically fades within 3-4 weeks.
Note: many insect bites cause a small red blotchy 'allergic' rash to appear soon after the skin is bitten. These soon go away. The rash of erythema migrans is different in that it usually develops several days after the bite, lasts for longer and has a typical spreading circular appearance.
Flu-like symptoms
These occur in about a third of cases. Symptoms include
Tiredness.
General aches and pains.
Red watery eyes.
Chills.
Neck stiffness.
These symptoms are often mild and go within a few days, even without treatment. In some cases, the infection does not progress any further, even without treatment, as the immune system may clear the infection. However, in some cases that are not treated, the disease progresses to stage two.
Stage two symptoms- early disseminated disease
This may develop in untreated people between 3 and 12 weeks after the bite. Disseminated means spread around the body away from the site of the original infection. Symptoms are variable but can include one or more of the following:
Joint problems
Problems can occur in one or more joints. They most commonly affect the knee joint. The severity of joint problems can range from episodes of mild joint pains, to severe joint inflammation (arthritis) causing a lot of pain.
Episodes of joint inflammation last, on average, three months. Joint problems caused by Lyme disease are more common where the infection has been caught in the USA and less common if it has been caught in Europe.
Nerve and brain problems
Some affected people develop inflammation to nerves, particularly the nerves around the face. This may cause the nerve to stop working and result in weakness of the face muscles. This may cause one side of the face to droop. Inflammation of the tissues around the brain (meningitis) and inflammation of the brain (encephalitis) may occur.
Heart problems
Some affected people develop inflammation of the heart (myocarditis) and other heart problems. This may cause symptoms such as dizziness, breathlessness, chest pain and a feeling that your heart is beating in a fast, irregular way (palpitations).
Rash
Several areas of the skin (not where the tick bite occurred) may develop a rash similar to erythema migrans (described above). These 'secondary' rashes tend to be smaller than the original stage one rash. These tend to fade within 3-4 weeks. Occasionally, blue-red nodules called lymphocytomas may develop on the skin, particularly on ear lobes and nipples.
Rarely, other organs such as the eyes, kidneys and liver are affected.
Stage three - late Lyme disease
This may develop months to years after infection. It usually develops after a period of not having any symptoms. A whole range of symptoms has been described in joints, skin, nerves, brain and heart:
The commonest symptom is ongoing episodes of joint inflammation (arthritis).
There may be an inflammation of part of the brain (encephalitis).
There may be weakness in nerves - for example, loss of sensation in the fingers or toes.
There may be skin changes, particularly a rash called Acrodermatitis Chronica Atrophicans.
The cause of certain long-standing symptoms of Lyme disease Chronic (persistent) Lyme disease (sometimes called "post Lyme disease") refers to symptoms which do not settle down despite treatment. These symptoms can include tiredness and joint pains similar to those in fibromyalgia or chronic fatigue syndrome. They can also include mood changes, reduction in concentration and memory impairment. This is a controversial subject and experts disagree whether certain symptoms are actually caused by Lyme disease or are due to other problems because there is no good evidence that these chronic symptoms are caused by Lyme disease.
Continue reading below
Lyme disease diagnosis
Back to contentsIn most cases, Lyme disease is diagnosed in stage one of the disease by the typical erythema migrans rash. People with this rash should always be treated for Lyme disease with antibiotics without waiting for the results of tests.
Where Lyme disease is suspected, but where there is no rash, they should have a blood test called an ELISA test. This should ideally be done within 4 weeks of developing the symptoms. If this first test is negative, the test should be repeated in another 4-6 weeks unless Lyme disease is no longer suspected. The blood test is looking for "antibodies" (evidence of the body's response to an infection) which is why it can take a few weeks for the test to become positive.
Treatment is only recommended in people without the rash and with negative tests where the clinical suspicion is high.
In the UK, it is recommended that the tests should only be only carried out in specialised NHS laboratories. Public Health England (PHE) advises that positive tests carried out in other places should be repeated in an NHS laboratory. People who have had the infection and been treated early are unlikely to develop positive blood tests later on. People with stage 2 or 3 of the disease usually have a positive blood test for Lyme disease.
Lyme disease treatment
Back to contentsA course of antibiotic medication will usually clear the infection. The type of antibiotic, and the length of the course, can vary depending on individual circumstances. A doctor will advise. Most people are diagnosed in stage one when treatment will clear the symptoms and prevent the development into stages two or three.
In most cases the antibiotic used is either doxycycline or amoxicillin. The course of treatment is usually two or three weeks. The antibiotic is taken as a tablet, or liquid, by mouth. In cases where there is nerve, heart or brain involvement, it may be necessary to be admitted to hospital for intravenous (IV) antibiotics.
Post-Lyme syndrome treatment
Treatment for persistent (chronic) Lyme disease or post-Lyme syndrome is controversial. Whilst it is well recognised that untreated Lyme disease can develop into stages 2 and 3 of the disease, these stages have clear episodes and are not generally "chronic" (ie persistent symptoms). Many experts do not believe Lyme disease is the cause of persistent long-standing symptoms.
There is no convincing evidence that longer or frequent courses of antibiotics improve the symptoms. Unnecessary antibiotics may cause side-effects, or bacteria may become resistant to them, meaning infections are more difficult to treat in the future.
Continue reading below
Lyme disease prevention
Back to contentsThe following will reduce the risk of developing Lyme disease:
If possible, avoid wooded areas where infected ticks live - particularly in the summer months. When out in the countryside, keep to paths and away from long grass or overgrown vegetation, as ticks crawl up long grass in their search for a feed.
If living in or visiting a tick-prone area, wear appropriate clothing when outdoors, ie long-sleeved shirts and long trousers tucked into socks. Light-coloured fabrics are useful, as it is easier to see ticks against a light background.
Inspect your entire body each day to check for ticks and remove any that are on the skin. Make sure that children's head and neck areas, including scalps, are properly checked.
Consider using an insect repellent spray, cream, etc, on the skin to help avoid tick bites (such as one that contains N,N-diethyl-m-toluamide (DEET)).
Shower or bath after returning from a tick-infested area.
Check that ticks are not brought home on clothes.
Check that pets do not bring ticks into the home on their fur.
Risk factors
Back to contentsMany people affected are forestry workers and other outdoor workers but visitors and holidaymakers to countryside areas where ticks are found are at risk.
Over half of infections acquired in the UK are known to have been caught in the southern counties of England. Areas where it is most common tend to be centres of outdoor activity - in particular, the New Forest, Thetford Forest, the South Downs, Exmoor, the Lake District, the North York moors and the Scottish Highlands.
Up to a fifth of Lyme disease is caught while abroad, in particular, the USA, France, Germany, Austria, Scandinavia and eastern and central Europe.
Outcome (prognosis)
Back to contentsThere is a very good chance of a complete cure with no further problems when treated with antibiotic medication in stage one of the disease.
If not treated in stage one, it is possible to develop some symptoms of stage two or three. However, these are often mild and transient symptoms such as a skin rash or mild joint pains. Some people develop more severe symptoms, such as meningitis, if they progress to stage two or three.
Treatment with antibiotics during stage two or three is also usually curative. However, a prolonged course of antibiotics may be needed.
It is difficult to treat "post-Lyme syndrome", as it is not known what causes these ongoing symptoms. However, most eventually clear up with time.
Infection with Lyme disease does not produce lifelong immunity so tick bite prevention measures need to be continued to reduce the risk of further infection.
Frequently Asked Questions
Back to contentsHow common is Lyme disease?
Since 1975 when it was first noted, thousands of cases have been reported in the USA. Lyme disease is less common in the UK but there are between 2,000 to 3,000 confirmed cases a year in England and Wales.
How do humans get Lyme disease?
The germ (bacteria) that causes Lyme disease lives on certain animals, usually rodents such as mice, some birds and some other small animals. The bacteria are usually harmless to the animals.
Ticks are small insect-like creatures, about the size of a pinhead, and they feed by sucking blood from animals such as mice. In this way, some ticks become infected with the bacteria that cause Lyme disease.
Ticks cannot jump or fly but they climb on to passing humans from long grass or foliage. If an infected tick bites a human then the bacteria may be passed into the human. The bacteria that cause Lyme disease cannot pass from person to person.
Note: most ticks in the UK are not infected by the bacterium that causes Lyme disease. Therefore, most tick bites will not cause Lyme disease.
After a person has been bitten by a tick, it usually takes 24-48 hours for the bacteria in the tick to pass into that person. Therefore, removing a tick soon after being bitten - within 24 hours - significantly reduces the risk of developing Lyme disease, even from an infected tick. This is why checking for ticks on the skin after spending time outside is so important.
How to remove a tick that is attached to your skin
Ticks attached to the skin can be removed by:
Gently gripping the tick as close to the point of attachment to the skin as possible. Do this preferably using fine-toothed tweezers or forceps, or a tick removal device.
Pulling steadily upwards, away from the skin. Take care not to crush the tick.
Inexpensive tick removal devices may be available at veterinary surgeries and pet supply shops and are useful for people who are frequently exposed to ticks. These should be used in accordance with manufacturers' instructions.
Do NOT do any of the following:
Burn the tick off (for example, using lighted cigarette ends or match heads).
Apply petroleum jelly, alcohol, nail varnish remover, or other substances (as this may stimulate the tick to regurgitate potentially infected material into the skin, which may increase the risk of transmission of infection).
Use your fingers to pull the tick off.
Squeeze or crush the tick.
After removal, DO clean the skin with soap and water, or skin disinfectant, and wash hands.
Patient picks for Other infections

Infections
Rheumatic fever
Rheumatic fever is an illness caused by a particular type of bacterium called beta-haemolytic streptococcus. It is the same bug that can cause a sore throat. It can affect your heart, as well as your joints, skin and nervous system.
by Dr Hayley Willacy, FRCGP

Infections
MRSA
Infection with MRSA bacteria mainly occurs in people who are already ill in hospital. It can be difficult to treat MRSA, as the bacteria are resistant to most types of antibiotic medicines. Many people are carriers of MRSA without even realising it, as MRSA often does not cause symptoms in healthy people.
by Dr Toni Hazell, MRCGP
Further reading and references
- Lyme disease: guidance, data and analysis; Public Health England - now UK Health Security Agency (last updated 2022)
- Lantos PM; Chronic Lyme disease. Infect Dis Clin North Am. 2015 Jun;29(2):325-40. doi: 10.1016/j.idc.2015.02.006.
- Lyme disease; NICE Guidance (April 2018 - last updated October 2018)
- Lyme Disease; NICE Quality standard, 2019
- Lyme disease; NICE CKS, November 2022 (UK access only)
- Removing a Tick; CDC
- Acrodermatitis Chronica Atrophicans; DermNet NZ
- Lyme Disease; Skar
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 12 May 2028
24 May 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.