
Will we ever have a male contraceptive pill?
Peer reviewed by Dr Sarah Jarvis MBE, FRCGPLast updated by Abi MillarLast updated 12 Mar 2019
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Could we soon have a male version of the pill? For many people, unsatisfied with current modes of contraception, the prospect probably sounds too good to be true.
In this article:
Video picks for Contraception
But now the question is being posed in earnest, with the announcement of a trial into a new male contraceptive gel. The gel, called NES/T, will be tested on couples in Edinburgh and Manchester and will work by halting men's sperm production. If the trial is successful, NES/T could become the first hormonal contraceptive for men.
"It's a combination of testosterone and a new form of progesterone called Nesterone," says Dr John Reynolds-Wright, who is leading the study. "It works by making the brain tell the testicles to stop producing sperm, but because there's testosterone inside the gel, you don't lose any of the masculine characteristics that testosterone gives you."
The men in the study will apply the gel daily to their upper arms and shoulders, and attend the clinic regularly to monitor their sperm count. Although it will take several months for their sperm count to drop to zero, the team hopes it will subsequently be as effective as the pill (around a 99% success rate) without reducing men's libido.
"This is something that will initially be used by couples who are in a long-term relationship because there's the element of trust that the female partner needs to have in the male partner," says Reynolds-Wright. "But there'll be lots of men who'll want to know they've got control over their own reproductive health even if they aren't in a long-term relationship."
Continue reading below
The market for a male pill
At the moment, men have just three contraceptive choices - condoms, withdrawal or a vasectomy ('the snip'). When you compare this to the number of choices available for women, it's easy to see why many would welcome an alternative.
Since the 1960s, women have been forced to bear the brunt of contraception (with all its inconveniences and side effects) while men who wish to control their fertility have been left with limited options. There would be benefits for women too. While many women take the pill (or other forms of hormonal contraception) without any problems, others struggle with side effects ranging from weight gain to depression. If their male partners could take the 'pill' instead, it would relieve them of the obligation.
Perhaps surprisingly, the majority of women in long-term relationships would trust their partners to use a male pill. In one study, women in Scotland, China and South Africa were asked their views on the subject. Only 13% of the women thought male hormonal contraception was a bad idea, and just 2% said they wouldn't trust their partners to use it.
When men in the same locations were asked their views, between 44% and 83% said they'd use a male contraceptive pill.
As Reynolds-Wright puts it: "Having different options and modalities available will hopefully get more men to engage with reproductive health and contraception."
Failed attempts and false starts
Back to contentsUnfortunately, it would be unwise to get too excited just yet. This is far from the first attempt to develop a male contraceptive - and in fact, the field has been littered with false starts.
Professor John Guillebaud, an expert in reproductive health at University College London, points out that 'heroic failures of male contraception' could comprise an article in itself.
"We've been told year after year, there'll be a male pill in 10 years, but they've been saying 10 years for the last 60," he says. "There are lots of potential methods, but none of them has really taken off, and, as far as I'm aware, all have had great difficulty getting funding."
He cites a few examples from what is a very long list. In the 1970s, the Chinese government tested out a male pill called gossypol, derived from the cotton plant. They stopped when many of the subjects developed hypokalaemia (low potassium in the blood).
In Indonesia, the gendarussa shrub has long been known to suppress male fertility, and a pill has been synthesised from its active ingredient. While this pill has proven successful in early trials, it has seen limited interest in the west.
A precursor to the NES/T gel, a contraceptive injection, was 96% effective in trials, but never saw the light of day thanks to concerns about side effects. (Reynolds-Wright says the gel contains a lower dose of testosterone, which should give rise to fewer side effects.)
Then there is the pill studied by Dr Nnaemeka Amobi, with whom Dr Guillebaud collaborated. Dubbed the 'clean sheets pill' because it gives men a dry orgasm, it too stalled at an early stage of research.
"The funding bodies thought there were two big obstacles - that women wouldn't trust a man to take it and that men wouldn't be prepared to take the risk," says Guillebaud. "On top of that, there was the feeling that men wouldn't like to have their ejaculation without delivering any semen. However, in trials of one of the prototype compounds men said they enjoyed sex just as much, and there was another - unproven - advantage in that it should protect against STI transmission from the man to the woman."
Continue reading below
Sexism and side effects
Back to contentsWhen asking what has thwarted progress to date, it's easy to pin the blame on sexism pure and simple. After all, the female pill has well-known side effects - are women being asked to put up with something that would be deemed unacceptable for men?
"Contraception has traditionally been aimed at women because they're the ones who bear the burden of pregnancy," says Reynolds-Wright. "That's how it has been framed - there may be some side effects but the trade-off is that you don't get pregnant. For men considering using hormonal contraception, contraception is being compared not to pregnancy, but to no contraception. It's a different way of thinking about side effects."
This argument may or may not sound convincing - to some, it may sound downright enraging - but coupled with misconceptions around market demand, it has presented a significant obstacle to progress.
Reynolds-Wright says that this caution around side effects should be extended to female contraceptives.
"There should be more of a concern about what side-effect profiles there are for the female contraceptives available," he says. "However, it's important to remember that most women and most men who use these kinds of contraceptives experience only minimal side effects and many of them experience none. And with the injectable, even the men reporting side effects were keen to us it as a form of contraception."
Technological challenges
Back to contentsLess contentious are the technical challenges - since men produce around 1,000 sperm a second (compared to one egg a month for women), it's very difficult to produce a contraceptive that stops all of them.
"There are concerns about sperms which might be damaged as opposed to killed, which might then get through and cause fetal abnormalities," says Guillebaud. "Then there's the issue that you've got to wait 70 days or so until you've got no sperm at all, even if it works as well as that, because that's how long it takes to make the sperm on the production line. In the real world, men and women want the contraception pretty quickly - they don't want to wait three months."
While he says the Edinburgh researchers are doing "very good work in a very difficult area", he is not convinced that they will succeed where so many before them have failed.
"It could come on the market quite quickly if it does give fewer side effects than the others being trialled, but I don't see it being a mass market product," he says. "So maybe we'll have a male pill in 10 years, but I can't see it being anything less than that myself - it's always been 10 years."
With the trial recruitment in full swing, only time will tell. The study is currently enrolling men aged 18-50, who are in a stable relationship with a woman aged 18-34. They can become part of the trial by calling 0161 276 3296 (Manchester) or 0131 242 2669 (Edinburgh).
"We would like to hear from anyone in the Edinburgh or Manchester area who'd be keen to have some more information about getting involved," says Reynolds-Wright.
Patient picks for Contraception
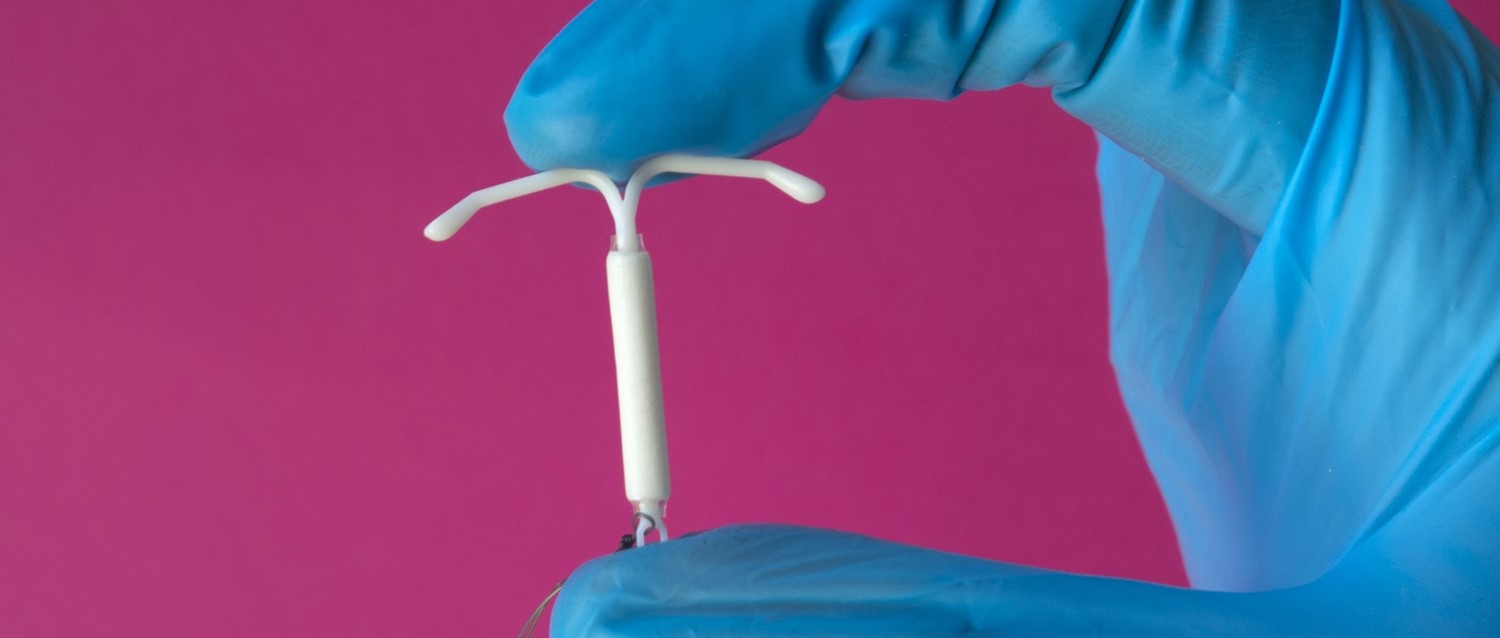
Sexual health
When will I become fertile again after coming off contraception?
If you want to have a baby, you’ve probably got a lot of questions - including how long it can take for you to become fertile again if you’ve been on the contraceptive pill or the coil. And while everyone is different, here’s what we know about fertility after coming off different kinds of contraception.
by Lydia Smith

Sexual health
Should you change your contraception to the coil or implant?
Fewer women in England are using the pill compared to ten years ago. More and more are turning to long-acting reversible contraceptives (LARCs), including the copper or the hormonal coil, the implant or the injectable contraceptive. We explore why this might be and look at the pros and cons of these longer-term options for birth control.
by Lydia Smith
Continue reading below
About the author

Abi Millar
Freelance Journalist
BA (Hons), MA
Abi is a freelance journalist with a special interest in health and medicine writing.
About the reviewerView full bio

Dr Sarah Jarvis MBE, FRCGP
Clinical Consultant
MA (Cantab), BM, BCh (Oxon), DRCOG, FRCGP, MBE
After training in medicine at Cambridge and Oxford, Dr Sarah Jarvis MBE became a GP.
Article history
The information on this page is peer reviewed by qualified clinicians.
12 Mar 2019 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.