Parvovirus infection
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 25 Apr 2022
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Slapped cheek syndrome article more useful, or one of our other health articles.
In this article:
Synonyms: erythema infectiosum, slapped cheek disease, slapped cheek syndrome, fifth disease, parvovirus B19
Continue reading below
What is a parvovirus infection?
Parvovirus B19 (B19V) is a common infection, usually presenting as erythema infectiosum in children. There is a wide range of potential consequences of parvovirus B19 infection. These extend from minor febrile illness to erythema infectiosum (fifth disease, slapped cheek syndrome), a generalised rash illness clinically indistinguishable from rubella, aplastic crises in patients with increased red cell turnover, arthropathy and persistent infection in the immunocompromised. It may also cause fetal loss or fetal hydrops and so detection in pregnancy is important for monitoring and possible treatment.
Parvoviruses are among the smallest DNA-containing viruses known to infect mammals (hence the name parvus, which is Latin for small). The only parvovirus known to be pathogenic in humans is parvovirus B19, discovered in 1974 whilst testing for serum hepatitis B antigens. It was so called because it occurred in serum sample 19, panel B. It is a single-strand DNA virus with no lipid coat, which makes it very resistant to the normal means of killing viruses, such as disinfectants and freezing.
Epidemiology
Back to contentsParvovirus is an extremely common infection. It most commonly occurs in children aged between 3-15 years. The most common clinical encounter with parvovirus B19 is as the causative agent of erythema infectiosum (fifth disease). This infection is not a notifiable disease.
It is estimated that around 50% of young men and women have antibodies against B19V, determined via serology tests.1
Infectivity and transmission
Transmission is usually via respiratory secretions but it can also be passed on via blood transfusion, bone marrow transplant, other blood products (but not intramuscular immunoglobulins) and from mother to baby via the placenta.
The incubation period for clinical erythema infectiosum is 4-20 days before the rash develops. The illness is infective from 10 days pre-rash until the onset of the rash. Once the rash appears, it is no longer infectious.
Infectivity is medium. It is less infectious than many other viral infections.2
One attack confers lifelong immunity.
Note:
Patients with aplastic crisis (see 'Complications', below) are highly infectious.
Immunocompromised patients may remain infectious.
Continue reading below
Parvovirus infection symptoms
Back to contentsIt may be asymptomatic (about 25% of infections) or it may present only with nonspecific coryzal symptoms (common).
Erythema infectiosum: this is also called 'fifth disease' because it is the fifth of the classic exanthems.
Parvovirus infection: the trunk rash will have developed a few days after the facial rash
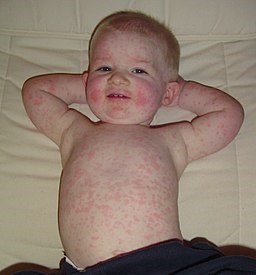
© Andrew Kerr, Public domain, via Wikimedia Commons
Prodromal symptoms usually start around a week following exposure to parvovirus B19. They are usually mild and may include headache, rhinitis, sore throat, low-grade fever and malaise. Less commonly, nausea, diarrhoea, abdominal pain or arthralgia may develop.
Following the prodromal phase, patients are usually symptom-free for around 7-10 days and then the classic 'slapped cheek' rash usually appears as erythema on the cheeks, sparing the nose, perioral and periorbital regions. This disappears after 2-4 days.
About 1-4 days after the facial rash appears, an erythematous macular/morbilliform rash develops on the extremities, mainly on the extensor surfaces. It is usually not itchy in young children but may be itchy in older children and adults. This gradually fades over the subsequent 3-21 days but may recur in reaction to various stimuli, such as exercise, heat and sunlight.
Arthropathy
May present as symmetrical arthropathy, affecting the hands, wrists, knees and ankles.
The symptoms usually resolve within a few days but in some cases persist for two months or longer.
An acute arthropathy is more common in adults than in children and it is more common in women.
The joint pain usually worsens throughout the day.
Complications
Back to contentsIntrauterine infection
See 'Parvovirus B19 in pregnancy', below.
Haematological conditions
Transient aplastic crisis: parvovirus B19 has an affinity for red cell precursors, so a transient aplastic crisis can be provoked by parvovirus infection in any patient with reduced red cell production or increased red cell loss - eg, sickle cell anaemia, thalassaemia, hereditary spherocytosis and iron-deficiency anaemia.
Patients with a transient aplastic crisis may be highly infectious, which may be relevant to other patients in hospital wards.
Other conditions linked to parvovirus include thrombocytopenia, idiopathic thrombocytopenic purpura and neutropenia.
Infection in immunodeficient patients
Parvovirus B19 can cause immunocytopenia in immunocompromised patients.
These patients may be unable to eradicate the infection, due to inadequate levels of IgM. They may remain infectious, yet test negative to IgM serology. Detection of the infection by alternative assays is necessary and is important for infection control.
Meningoencephalitis can occur with acute parvovirus infection.
Other complications
Rarely, parvovirus B19 has been linked to hepatitis, myocarditis, meningitis, encephalitis and peripheral neuropathy.
B19 infection has also been associated with development of a variety of different autoimmune diseases.3
Continue reading below
Differential diagnosis
Back to contentsErythema infectiosum
Rubella (look for suboccipital lymphadenopathy).
Measles (look for Koplik's spots on buccal mucosa).
Scarlet fever (look for strawberry tongue).
Roseola infantum.
Drug eruptions.
Other infections can present with rash, including meningitis and septicaemia.
Older children or adults with arthropathy and rash
Acute rheumatic fever.
Allergic hypersensitivity reaction.
Classic viral exanthems.
Epstein-Barr virus.
Hepatitis (parvovirus may cause transient elevations in liver enzymes).
Rheumatological disorders.
Investigations4 5
Back to contentsInvestigations are not necessary in patients with uncomplicated erythema infectiosum. However, if the clinical scenario requires confirmation of diagnosis (eg, pregnancy, immunocompromised patients, aplastic crisis, arthropathy), the following may be helpful:
B19-specific IgM - a positive screen indicates current or recent infection. NB: immunocompromised patients may be unable to make sufficient IgM and may test negative; they will need other tests.
B19-specific IgG indicates immunity - it usually appears two weeks after infection and persists for life. IgG may also detect seroconversion in immunocompromised patients.
Polymerase chain reaction (PCR) - for the specific detection of parvovirus B19.
Parvovirus infection management
Back to contentsFor healthy and non-pregnant patients, only symptomatic treatment and explanation are needed.
To prevent transmission:
Advise patients to avoid contact with those at risk of complications: pregnant women, immunocompromised patients and those with haematological conditions. If contact does occur, these people should be advised to see their doctor.
Within households and in institutions, transmission is difficult to prevent but hand washing is recommended.
For erythema infectiosum, the diagnostic features appear after the period of infectivity has passed, so exclusion from school has no effect on transmission - children can go to school or nursery with a parvovirus rash.5
Prognosis
Back to contentsThe most common consequence of B19 infection in the compromised person is pure red cell aplasia, resulting in chronic or recurrent anaemia with reticulocytopenia.4 The majority of compromised people have pre-existing antibody to B19 and are not at risk.
Erythema infectiosum: this is a self-limiting condition in immunocompetent patients.
Pregnancy: see 'Parvovirus B19 in pregnancy', below.
Arthropathy: there are no long-term sequelae.
Transient aplastic crisis: this is usually transient, lasting no more than two weeks in otherwise healthy individuals; it responds rapidly to treatment if required.
Immunocompromised patients: the treatment of pure red cell aplasia with immunoglobulin is frequently ameliorative and often curative.
Parvovirus B19 in pregnancy5 6
Back to contentsEpidemiology, transmission and risks7
Pregnant women who develop erythema infectiosum have a 30% chance of passing it on to their unborn baby and a 5-10% chance of fetal loss. Fetal loss usually occurs in the second trimester; it is rare in the first trimester.5
Although the maternal symptoms of the virus are usually short-lived, additional fetal complications that can occur include hydrops fetalis, hepatitis, severe anaemia, inflammation of the heart muscle and cardiac failure.
Maternal infection in the first trimester is associated with a risk of fetal death of 19%. A gestational age of 13-20 weeks is associated with a 15% chance of fetal death and this falls to 6% after 20 weeks.
Identification of parvovirus B19 infection in a pregnant woman is important, as parvovirus infection in the first half of pregnancy may cause intrauterine death and fetal hydrops.
Permanent congenital abnormality and/or congenital anaemia have also been identified as rare consequences of intrauterine infection.
Maternal asymptomatic parvovirus B19 infection is at least as likely to infect and damage the fetus as symptomatic infection.
Diagnosis is important, as intrauterine transfusion of the fetus improves the outcome.
Investigation and management in pregnancy
General principles
All pregnant women who have a non-vesicular rash, or contact with someone who has a non-vesicular rash, should be investigated for parvovirus and rubella infection - irrespective of past history, previous serology or gestation:
Contact is defined as being in the same room for >15 minutes or face-to-face contact; however, for parvovirus, this is probably over-cautious, the main risk of infection being from household contacts or prolonged occupational contact.
The IgM result confirms or excludes infection in the four weeks prior to the sample. This also means that parvovirus infection cannot be excluded if investigation starts >4 weeks after onset of the rash.
When/what to test
Test for parvovirus B19 (and rubella) IgM and IgG as soon as possible after contact with, or symptoms of, a rash illness. Include details of dates of illness/contact, details of rash, gestation, etc:
Positive IgG with negative IgM will confirm immunity and the patient can be reassured.
If IgM is detected but IgG is not detected, a further sample should be taken immediately. If the repeat sample is positive for IgM further testing, confirmation by alternative assay is required - eg, detection of high titre B19 virus DNA or IgG seroconversion using an antenatal booking blood (discuss with microbiologist).
If neither IgG nor IgM is detected, a further sample should be tested one month later:
If both are negative, the woman can be reassured that she has no evidence of parvovirus infection but is susceptible.
Management of confirmed parvovirus infection in pregnancy
The management of confirmed parvovirus in pregnancy is now more active than in the past. This is because it has been demonstrated that intrauterine transfusion of the fetus can improve the outcome.
If parvovirus is suspected in pregnancy, advice should be sought from virology, microbiology or infectious diseases - which of these specialties is consulted may depend on local pathways. Suspicion may be due to symptoms or to exposure - a significant contact is defined as being in the same room for 15 minutes or more, or any face-to-face contact with a person with parvovirus, within the preceding three weeks.5
If the diagnosis is confirmed, as detailed in the above section on testing, the National Institute for Health and Care Excellence (NICE) advises referral to a specialist in fetal medicine, to be seen within four weeks. However, Royal College of Obstetricians and Gynaecologists (RCOG) guidance only advises such referral if there is hydrops fetalis seen on ultrasound and so it may be appropriate to seek an urgent review from the woman's obstetrician, and let them make the decision about onward referral to a fetal medicine unit.5
Parvovirus infection prevention
Back to contentsThere is currently no licensed vaccine for parvovirus B19.
Screening of donated blood components before transfusion for patients with sickle cell disease and other congenital anaemias, immunocompromised hosts and women during pregnancy.
All pregnant healthcare workers should have a risk assessment carried out by their employer - depending on the workplace, this may include avoiding scenarios in which they may be exposed to parvovirus.8
Children with parvovirus infectiosum do not need to stay off school or nursery, as once they have the rash they are no longer infectious.
Patients infected with parvovirus B19 are considered non-infectious one day after the rash begins.
Further reading and references
- Fifth disease; DermNet NZ
- Giakoumelou S, Wheelhouse N, Cuschieri K, et al; The role of infection in miscarriage. Hum Reprod Update. 2016 Jan-Feb;22(1):116-33. doi: 10.1093/humupd/dmv041. Epub 2015 Sep 19.
- de Villemeur AB, Gratacap-Cavallier B, Casey R, et al; Occupational risk for cytomegalovirus, but not for parvovirus B19 in child-care personnel in France. J Infect. 2011 Dec;63(6):457-67. doi: 10.1016/j.jinf.2011.06.012. Epub 2011 Aug 16.
- Kerr JR; The role of parvovirus B19 in the pathogenesis of autoimmunity and autoimmune disease. J Clin Pathol. 2016 Apr;69(4):279-91. doi: 10.1136/jclinpath-2015-203455. Epub 2015 Dec 7.
- Landry ML; Parvovirus B19. Microbiol Spectr. 2016 Jun;4(3). doi: 10.1128/microbiolspec.DMIH2-0008-2015.
- Parvovirus B19 infection; NICE CKS, February 2022 (UK access only)
- Viral rash in pregnancy; UK Health Security Agency.
- Lamont RF, Sobel JD, Vaisbuch E, et al; Parvovirus B19 infection in human pregnancy. BJOG. 2011 Jan;118(2):175-86. doi: 10.1111/j.1471-0528.2010.02749.x. Epub 2010 Oct 13.
- Protecting new and expectant mothers at work; Health and Safety Executive
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 24 Apr 2027
25 Apr 2022 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free