Acute prostatitis
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Toni Hazell, MRCGPLast updated 22 May 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
When the prostate gland becomes infected with a germ (a bacterial infection), the condition is known as acute prostatitis. 'itis' means inflammation, so prostatitis is inflammation of the prostate - not all forms of prostatitis are bacterial, but this leaflet will mainly cover bacterial prostatitis. Symptoms include pain, mainly at the base of the penis and around the anus. A bladder infection commonly occurs at the same time. Treatment includes a four-week course of antibiotic medication.
In this article:
Video picks for Prostate problems
Continue reading below
Acute prostatitis symptoms
Back to contentsIn acute prostatitis, symptoms develop quickly - typically over a few days or so. It usually occurs at the same time as a urine infection. Therefore, you may also have a bladder infection (cystitis). Germs (bacteria) are found in your urine if a urine sample is taken. Symptoms include:
Pain from your prostate, which may be severe. You feel this mainly at the base of your penis, around your anus, just above your pubic bone and/or in your lower back. Pain may spread to your penis and testicles (testes). Passing stools (faeces) can be painful.
Symptoms of a urine infection. For example: pain when you pass urine, passing urine frequently, an urgent desire to pass urine, and sometimes having blood in your urine. Some people can develop problems so that they are unable to pass urine and the urine builds up in the bladder (this is called urinary retention). See the separate leaflet called Urinary Retention.
High temperature (fever). General aches and pains. You generally feel ill.
A small amount of thick fluid (discharge) may come out of your penis from your urethra.
Your prostate feels tender if a doctor examines it with a gloved finger in your back passage (rectum) - this is known as a digital rectal examination, a type of physical examination.
Continue reading below
What is the prostate gland?
Back to contentsCross-section diagram of the prostate and nearby organs
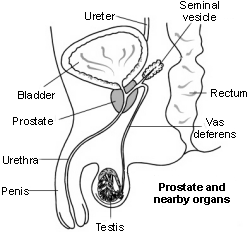
Only men have a prostate gland (just referred to as the 'prostate' from now on here). It lies just beneath the bladder. It is normally about the size of a chestnut. The urethra is the tube that urine travels along from the bladder to the outside and it runs through the middle of the prostate and then through the penis. The prostate helps to make semen but most semen is made by another gland nearby (the seminal vesicle).
Causes of acute prostatitis
Back to contentsInfection by germs (bacteria) that normally live in your bowel
Some bacteria that live harmlessly in the bowel commonly get on to the skin near to the anus when we pass stools (faeces). In some people they may then multiply. Some of these bacteria may then travel up the urethra and cause infection anywhere in the urinary tract - that is, the kidneys, bladder, prostate, or urethra. This is called a 'urinary tract infection'.
A prostate infection may also occur with or without other parts of the urinary tract being infected. Some conditions that cause pooling or blockage of urine increase the risk of a urinary tract infection. For example, having an enlarged prostate gland or kidney stones. This is because bacteria often thrive and multiply quickly in pooled urine.
Less common causes
Damage to the prostate makes it more prone to infection - for example, after prostate surgery.
A thin, flexible, hollow tube (a catheter) passed into the bladder through the urethra may sometimes let bacteria travel to the prostate. This can also happen after a telescopic instrument is passed through the urethra into the bladder (as happens during investigation of the prostate gland and the bladder).
Sometimes the prostate is infected by bacteria in the bloodstream that have travelled from other infections in the body.
Acute prostatitis is not considered a sexually transmitted infection, so a sexual partner is not at risk.
Continue reading below
How common is acute prostatitis?
Back to contentsSymptoms of prostatitis affect around 8% of men at some point in their life, but only about 10% of these have a proven bacterial cause, though it is possible that more are bacterial but we never find out exactly which bacteria it is.
Diagnosing acute prostatitis
Back to contentsDiagnostic tests to assess for infection will likely include:
A urine test may detect germs (bacteria) if you have acute prostatitis and should definitely be positive if you have a urinary tract infection. Your doctor will usually be able to do a quick test on your urine in the surgery (a dipstick urine test). This can show if infection is likely to be present. They may then send your urine sample to the laboratory to be tested further and to confirm infection.
Other tests such as an ultrasound scan or computerised tomography (CT) scan or MRI scan may be advised following acute prostatitis. This is to rule out any problem with your urinary tract that may have contributed to causing the infection. CT and MRI scans are usually arranged by a hospital consultant rather than the GP.
Blood tests may or may not be done, depending on your exact symptoms. Sometimes this may include a prostate specific antigen (PSA) test, which is more usually done when concerned about prostate cancer. If it is raised, this does not necessarily mean that you have cancer - the test may become normal after you have antibiotics.
Acute prostatitis can produce similar symptoms to a sexually transmitted infection. For this reason, if you are at risk of a sexually transmitted infection, your doctor may suggest that you have some swab or urine tests to exclude this. Note: acute prostatitis is not a sexually transmitted infection.
Acute prostatitis treatment
Back to contentsAntibiotics. A four-week course is usually needed, though the recommendation is for an initial two-week course and then a review and consideration of giving another two weeks' worth. Antibiotics are generally started before the confirmatory urine test results are back. The first antibiotic may be changed after the result of the urine test is back. The urine test may find exactly which germ (bacterium) is causing the infection and the best antibiotic to treat it, but this does not always happen - sometimes the result is less specific. Four weeks of antibiotics are thought to be necessary to reduce the chance that you develop persistent (chronic) prostatitis. If you are very unwell, you may need to go into hospital to have the antibiotics given through a vein.
Paracetamol or ibuprofen ease pain and high temperature (fever). They are best taken regularly rather than now and then. Stronger painkillers are sometimes needed.
Laxatives can keep your stools (faeces) soft, if needed. They may help to ease pain if you have hard stools in your back passage (rectum), pressing on your infected prostate.
Complications of acute prostatitis
Back to contentsRarely, apart from chronic bacterial prostatitis, other complications of acute prostatitis can occur. These include:
Sudden-onset (acute) urinary retention. Because it may be so painful to pass urine, urine can build up in your bladder, causing pain in your lower tummy (abdomen) and inability to pass urine at all. To relieve this, a thin, flexible, hollow tube (a catheter) is needed. This is usually inserted through a small cut in your tummy (abdomen) directly into your bladder to drain the urine. The catheter can usually be removed once the antibiotics have started working and the infection of the prostate is clearing.
Prostate abscess. If the antibiotics do not effectively treat the prostate infection, rarely you can develop an abscess of your prostate. Your doctor may suspect this if your symptoms do not improve despite antibiotic treatment. Further tests are needed to confirm a prostate abscess, such as an ultrasound or CT scan of your prostate. If an abscess is present, an operation is needed to drain it.
Outlook (prognosis)
Back to contentsAcute prostatitis usually clears with a course of antibiotics. However, it is important to take the full course to clear the infection completely. There is a risk that an acute infection may become a persistent (chronic) infection if you do not take the full course of antibiotics - this can lead to chronic pelvic pain syndrome. See the separate leaflet called Chronic Prostatitis for further details.
Patient picks for Prostate problems

Men's health
Chronic prostatitis
Prostatitis means that you have inflammation of your prostate gland. There are two main types of prostatitis: short-lived (acute) or persistent (chronic). It can also be caused by an infection (infective) or be non-infective. Less than 1 in 10 cases of prostatitis are due to bacterial infection. For the diagnosis of chronic prostatitis, symptoms need to have been present for at least three months. In acute prostatitis, symptoms usually come on and go away much more quickly. About 9 in 10 men with chronic prostatitis have chronic prostatitis/chronic pelvic pain syndrome (CPPS). About 1 in 10 men with chronic prostatitis have chronic bacterial prostatitis.
by Dr Toni Hazell, MRCGP

Men's health
Prostate problems
Prostate and urethral problems can affect the smooth flow of urine in men. This leaflet will give you a brief explanation of the different prostate and urethral conditions and how the urine system can be affected.
by Dr Rachel Hudson, MRCGP
Further reading and references
- Coker TJ, Dierfeldt DM; Acute Bacterial Prostatitis: Diagnosis and Management. Am Fam Physician. 2016 Jan 15;93(2):114-20.
- Prostatitis - acute; NICE CKS, August 2021 (UK access only)
- Urological infections; European Association of Urology (2022 -updated 2024)
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 14 Apr 2028
22 May 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.