Schistosomiasis
Peer reviewed by Dr Philippa Vincent, MRCGPLast updated by Dr Surangi Mendis, MRCGPLast updated 28 Sept 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
Schistosomiasis is a tropical disease caused by an infection with parasitic worms. In the past it was more commonly known as Bilharzia. Many people do not develop symptoms of acute schistosomiasis, or their symptoms may be mild and go unrecognised. Diagnosis is usually made by testing the urine or poo (faeces) or through a blood test. Treatment is with a medicine called praziquantel. Many people recover completely following treatment.
In this article:
Continue reading below
What are the symptoms of schistosomiasis?
Schistosomiasis can be 'acute' or 'chronic'. Within days of becoming infected, some people can develop a rash or itchy skin. This is known as 'swimmer's itch'.
Acute schistosomiasis
This is also known as Katayama fever. Acute means 'sudden onset' or 'short duration'. Symptoms first develop some weeks after you have been in contact with the infested water. Symptoms can include:
Fever.
Headache.
Tiredness.
Joint and muscle pains.
Cough.
Bloody diarrhoea.
Tummy (abdominal) pain.
Note: many people who are infected do not develop symptoms of acute schistosomiasis, or their symptoms may be mild and go unrecognised. Some may dismiss their symptoms, believing them to have been caused by a simple viral infection. However, they can go on to develop chronic schistosomiasis.
Chronic schistosomiasis
This is more common than acute schistosomiasis. Chronic means 'persistent'. If you have chronic schistosomiasis, you can develop symptoms many months or years after you were first infected. It can cause long-term ill health.
The symptoms depend on the species of schistosoma that you have and where this species produces most of its eggs. Schistosoma mansoni and Schistosoma japonicum tend to lay eggs in the blood vessels around the bowel. Schistosoma haematobium tends to produce eggs in the blood vessels around the bladder. The symptoms are caused by the body's immune system reacting against the eggs that the worms produce, not by the worms themselves. This reaction can cause inflammation and scarring of the tissues and organs of the body.
If eggs are mainly produced in the blood vessels around the bowel, symptoms can include bloody diarrhoea and tummy (abdominal) pain which tends to be cramping. If they are produced in the blood vessels around the bladder, symptoms can include blood in the urine and pain on urinating.
Eggs that have not been excreted by the body can also travel to other parts of the body and cause symptoms. For example, the liver, lungs, heart, brain or nervous system may be affected. Symptoms depend on the affected area but can include:
Breathlessness.
Cough.
Palpitations.
Chest pain.
Liver failure.
Seizures.
Confusion.
Paralysis (if the spinal cord is involved).
Children who are repeatedly infected with schistosomiasis can develop anaemia, malnutrition and learning difficulties.
How do you get schistosomiasis?
Schistosomiasis is a tropical disease caused by a parasitic infection with worms from the Schistosomatidae family. A parasite is an animal that lives on or in another animal and feeds from it.
Schistosoma parasite
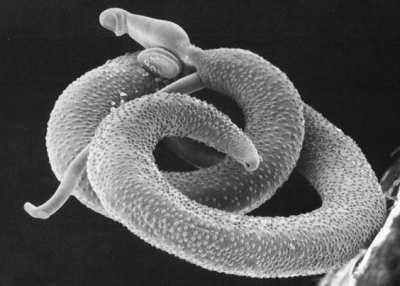
By Waisberg at English Wikipedia [Public domain], via Wikimedia Commons
There are three main worm species that cause schistosomiasis in humans:
Schistosoma haematobium.
Schistosoma mansoni.
Schistosoma japonicum.
Eggs from the mature worms are passed out of the body (excreted) in the poo (faeces) or urine of an infected person. These eggs can get into fresh water if it is contaminated with human sewage. Once in the water, the eggs can infect snails living in the water and they then start to develop into larvae inside the snails. These freshwater snails are known as 'intermediate hosts' because they are needed for the worms to complete their life cycle.
The mature larvae are then released from the snails into the water. The larvae can swim around and can enter the skin of someone who bathes, wades or swims in the water. Once they have got through the skin, larvae then travel to the blood vessels where they mature into adult worms. The worms settle in the blood vessels around the intestine or the bladder (depending on the species). Here, the male and female worms mate and eggs are produced. These eggs can pass from the blood vessels through the wall of the bladder or the bowel so that they can be excreted in the urine or faeces. The life cycle of the worm is then able to start again. The worms can live inside the body of a human for three to five years, producing eggs.
Note: not all eggs are excreted. Some stay in the body and are involved in the development of symptoms (see below).
Continue reading below
How common is schistosomiasis?
The World Health Organization (WHO) reports that over 250 million people are infected with schistosomiasis worldwide, 137 million of which are school-aged children.
How is schistosomiasis spread?
Those who live in or travel to an area where schistosomiasis occurs are at risk of schistosomiasis, although contact with fresh water that contains the snails that act as the intermediate host is also required. This contact can be through, for example:
Swimming.
Boating.
Rafting.
Water skiing.
Bathing.
Working on irrigation equipment.
Drinking from streams or irrigation ditches.
Children and teenagers are most often affected. In some areas of the world nearly all those aged 10-19 may be, or have been, infected. Re-infection is also common.
Continue reading below
How is schistosomiasis diagnosed?
There are a number of tests that can be used to help confirm the diagnosis, or that can be used to assess which parts of the body are affected by the infection. These include:
Urine and poo (faeces) samples
Schistosomiasis is usually diagnosed by testing urine and faeces samples. The test looks for schistosomal eggs in the urine or faeces, using a microscope.
Blood tests
An antibody or antigen blood test can show if someone has, or has had, schistosomiasis. It can take some time for these tests to become positive (4-8 weeks). Other blood tests can check for anaemia and to see if the liver or kidneys are affected.
Chest X-ray
A chest X-ray can sometimes show if the lungs are affected.
Scans
An ultrasound scan of the liver or the heart may be useful to show if schistosomiasis has affected these organs.
Sometimes CT scanning or MRI scanning is used, especially if the brain or spinal cord is affected.
Colonoscopy or cystoscopy: sometimes schistosomiasis is diagnosed after taking samples during one of the following procedures:
Schistosomiasis treatment
A medication called praziquantel is the most common treatment for schistosomiasis. It is a tablet taken by mouth. It is considered to be safe and is effective in most cases. The treatment is usually just a single dose, or two doses taken on the same day. Steroid medication is also sometimes given in acute schistosomiasis. Any complications (see below) will also need to be treated.
What are the complications of schistosomiasis?
In some people, if schistosomiasis is untreated, or if infection goes unrecognised, complications can sometimes occur. These can include:
Chronic liver damage and an enlarged spleen.
Colon (large intestine) inflammation.
Kidney and bladder obstruction.
Repeated blood infections can occur - germs (bacteria) can easily enter the bloodstream through an inflamed colon.
Heart failure.
Bladder cancer - your risk of bladder cancer is slightly increased if schistosomiasis affects your bladder.
Where is schistosomiasis found?
There are certain areas of the world where schistosomiasis occurs. If you travel to, or live in, the following areas you are at risk if you come into contact with contaminated fresh water:
Africa: all fresh water in southern and sub-Saharan Africa, including the great lakes and rivers as well as smaller bodies of water. Transmission also occurs in the Nile River valley in Egypt.
South America: including Brazil, Suriname, Venezuela.
Caribbean: Antigua, Dominican Republic, Guadalupe, Martinique, Montserrat, Saint Lucia (risk is low).
The Middle East: Iran, Iraq, Saudi Arabia, Yemen.
Southern China.
Southeast Asia: Philippines, the Lao People's Democratic Republic, Cambodia, central Indonesia, Mekong Delta.
However, trends in the movement of people and populations (from rural to urban areas and also migration to other countries) is introducing schistosomiasis to new areas.
Additionally, due to a rise in eco-tourism and travel to remote locations, increasing numbers of tourists are becoming infected with schistosomiasis.
Note: chlorinated swimming pools and seawater are generally thought to be safe.
What is the outlook for schistosomiasis?
Almost all people who receive treatment for schistosomiasis will improve. There can be complete recovery in those who have not been infected for long, or those without complications.
Even if someone has developed complications such as liver damage, these can sometimes improve after treatment. However, for some people, complications cannot be reversed and they can develop chronic ill health; occasionally, death can occur. If someone is also infected with malaria, HIV, or hepatitis, the prognosis tends to be worse.
Can schistosomiasis be prevented?
People who travel to areas affected by schistosomiasis should avoid exposure to fresh water that is likely to be contaminated. This means:
Avoiding swimming or wading in fresh water.
Drinking water that is safe. This means either drinking bottled water (ensuring that the bottle is sealed before opening), filtering water or boiling it for at least one minute.
Bathing in safe water. Bath water should be heated for five minutes at 150°F (about 66°C). Water held in a storage tank for at least 48 hours should be safe for showering.
Various measures are being taken to help to reduce schistosomiasis infection in affected countries. These include:
Improved sanitation to decrease sewage contamination of fresh water.
Measures to help reduce occupational and recreational contact with contaminated water.
Treatment of water to help reduce the numbers of the snail 'intermediate hosts'.
Treatment of people in affected areas with medicines to 'kill off' the infection. The WHO uses a strategy involving medicines to help control schistosomiasis in a number of countries. However, in 2021, WHO reported that the COVID-19 pandemic, and work undertaken to reduce its impact, reduced the availability of resources available to treat and manage some neglected tropical diseases, including schistosomiasis.
Patient picks for Travel related infections

Travel and vaccinations
Chikungunya fever
Chikungunya fever is an illness caused by a virus. The virus infects you when you are bitten by a certain type of mosquito. You cannot catch chikungunya fever in the UK but you may be at risk of catching it when abroad. It usually causes a high temperature (the 'fever') and joint pains. In most people it goes away completely after one or two weeks. In a few people it may be a more serious illness. There is no specific treatment. Before travelling, always check travel health websites to get the latest information on infections in the area to which you are going. Chikungunya can be prevented by taking measures to avoid mosquito bites.
by Dr Hayley Willacy, FRCGP

Travel and vaccinations
Roundworms
Roundworms (also called nematodes) are worms with a long round body. They vary in length from several millimetres to up to two metres. Roundworms are common in warm tropical countries and most infections seen in the UK will have been acquired abroad. Children are more often affected than adults. Treatment is usually very effective but wiping out (eradication of) roundworm infections has proved to be very difficult.
by Dr Toni Hazell, MRCGP
Further reading and references
- Schistosomiasis; World Health Organization
- Schistosomiasis; DPDx, Centers for Disease Control and Prevention.
- Nelwan ML; Schistosomiasis: Life Cycle, Diagnosis, and Control. Curr Ther Res Clin Exp. 2019 Jun 22;91:5-9. doi: 10.1016/j.curtheres.2019.06.001. eCollection 2019.
- Lackey EK, Horrall S; Schistosomiasis.
- Carbonell C, Rodriguez-Alonso B, Lopez-Bernus A, et al; Clinical Spectrum of Schistosomiasis: An Update. J Clin Med. 2021 Nov 25;10(23):5521. doi: 10.3390/jcm10235521.
Continue reading below
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 26 Sept 2028
28 Sept 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free