Haemochromatosis
Peer reviewed by Dr Colin Tidy, MRCGPLast updated by Dr Philippa Vincent, MRCGPLast updated 10 Aug 2023
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Haemochromatosis is an inherited (genetic) disorder which causes the body to absorb too much iron from the diet. This excess iron causes damage to organs in which it builds up. The main treatment is the regular removal of blood which helps to remove the excess iron from the body. If treatment is started early, before complications occur, then the outlook for people with haemochromatosis is very good.
At a glance
Haemochromatosis is an inherited condition causing the body to absorb too much iron from food.
This excess iron is stored in organs, such as the liver, pancreas, and heart, causing damage.
Symptoms often start between 30-50 years, including tiredness, joint pain, and abdominal pain.
Diagnosis involves blood tests for iron levels and a gene test.
Treatment involves regularly removing blood (venesection) to reduce iron levels.
Early diagnosis and treatment can prevent serious complications and lead to a normal life expectancy.
Avoiding iron supplements, fortified cereals, and large doses of Vitamin C can help.
In this article:
Video picks for Blood problems
Continue reading below
What is haemochromatosis?
What is haemochromatosis?
People with haemochromatosis have inherited a faulty gene, which directs the body to absorb too much iron from what they eat and drink. Excessive quantities of iron are then stored in various organs. This excess iron may be stored in the liver, pancreas, heart, testicles, ovaries, skin and joints. It causes damage to these tissues, which leads to a variety of symptoms.
Haemochromatosis symptoms
Back to contentsSymptoms of haemochromatosis usually start between the ages of 30 and 50 years. The first symptoms are usually vague and may include feeling weak and tired, and having joint pains or abdominal pains.
As haemochromatosis progresses, more specific symptoms develop due to organ damage but these are significantly less common nowadays due to earlier diagnosis. However there are still many cases each year in people who have not yet been diagnosed.
These problems may include:
Joint pain and swelling, especially the knuckle and the first joint of the first two fingers.
Bronzing of the skin (looking like a permanent tan).
Loss of sex drive.
Loss of body hair.
Period changes in women. Women may have either no menstrual periods or very light menstrual periods. Early menopause may also occur in women with haemochromatosis.
Poor memory.
Feeling irritable.
Developing diabetes.
An increase in the size of the liver.
Most of these symptoms are found in other disorders and so diagnosis can be difficult. Arthritis found only in the knuckle and the first joint of the first two fingers is very suggestive of haemochromatosis.
The need for treatment to remove excess iron does not depend on the presence of symptoms. Because of the risk of developing a serious complication such as cirrhosis, treatment to remove iron buildup from the body is very important even if there are no symptoms.
Continue reading below
Causes of haemochromatosis
Back to contentsHaemochromatosis is a genetic condition. It is passed on through families through codes inside cells called genes. Genes come in pairs. In haemochromatosis, one of the gene pairs does not work properly. A few different genes may be involved but 9 out of 10 people with haemochromatosis have an abnormal 'HFE' gene, which is on chromosome 6.
Haemochromatosis is an autosomal recessive disorder. This means that haemochromatosis will only occur if both copies of the gene are abnormal (one copy from the mother and one from the father). If only one copy is defective, a person will be healthy but will be a 'carrier'. This means he or she will be able to pass on the abnormal gene to a son or daughter.
There is now a gene test which can help to diagnose most people who have haemochromatosis.
When two people who carry the abnormal gene have a child, there is a:
1 in 4 chance that the child will have haemochromatosis (by inheriting the abnormal gene from both parents).
2 in 4 chance that the child will not have haemochromatosis but will be a carrier (by inheriting the abnormal gene from one parent but the normal gene form the other parent).
1 in 4 chance that the child will not have haemochromatosis and will not be a carrier (by inheriting the normal gene from both parents).
These proportions are averages for the whole population and in any one family with both parents being carriers, it would be possible for all children to be affected, all to be carriers, or for all not to be affected or be carriers.
How recessive inheritance works when both parents are carriers (n = normal gene; H = gene for haemochromatosis):
Haemochromatosis inheritance
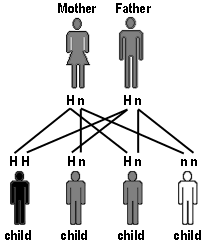
©The Haemochromatosis Society
How common is haemochromatosis?
Back to contentsHaemochromatosis occurs in people from all parts of the world but is most common in people from Northern Europe. Surveys have shown that around 1 in 150 of people of UK origin have haemochromatosis though it is much more common in Northern Ireland with closer to 1 in 100 people affected. Approximately 1 in 10 people carries one copy of the abnormal gene in Northern Europe and is therefore a carrier of haemochromatosis; this is 1 in 5 people in Northern Ireland. Haemochromatosis is now recognised as being one of the most common genetic disorders.
Continue reading below
How is haemochromatosis diagnosed?
Back to contentsBlood tests
The first tests are to see how much iron is stored in the body. This can be done by having a blood test for iron (ferritin) and transferrin saturations. Transferrin is a protein that transports iron in the blood. Transferrin is mostly made in the liver, and it regulates iron absorption.
Transferrin saturation is the percentage of this protein which is already attached to iron. The levels of both iron in the blood and the transferrin saturation are usually high in haemochromatosis.
Initial tests will also check for any other possible causes of the symptoms. Blood tests will also be done for any possible complications of haemochromatosis such as problems with the liver or diabetes.
Gene test
The test to confirm the diagnosis of haemochromatosis is the gene test for the HFE gene, which is abnormal in 9 out of 10 people with haemochromatosis. (See the section at the end of this leaflet to read more about this gene.)
Scans
A scan of the liver may help to detect how much iron is in the liver. Taking a liver sample (biopsy) used to be needed but is much less often done nowadays because a scan and a gene test can be done instead. However, a liver biopsy may be needed if the iron level in the body is very high or there seem to be other problems with the liver.
Other tests may be needed to check for complications of haemochromatosis, such as an ultrasound scan of the heart (echocardiogram).
Who should be tested?
Back to contentsAnyone with symptoms indicating possible haemochromatosis should be tested for the level of iron in the body. The gene test should be offered if high iron levels are detected.
Brothers, sisters and children of anyone who has haemochromatosis should be tested for the abnormal gene. The test should only be done after talking to a health professional about the possible benefits and problems of having the test.
The clear benefit of being tested is to have treatment early before any complications occur. Possible problems include the psychological impact of a positive test. In 2018, insurance companies in the UK agreed not to require positive genetic tests to be revealed when offering life insurance. See the separate leaflet called Genetic Testing for more details.
Haemochromatosis treatment
Back to contentsTreatment of haemochromatosis is simple and effective. It consists of regular removal of blood which is also known as venesection therapy or phlebotomy. This may need to be done frequently (every week) at first, depending on the level of iron overload in the body.
The levels of iron in the body are monitored closely during treatment. Iron levels are reduced very slowly, often over quite a long period of time. Once levels are normal, regular blood tests monitor the iron levels. Further blood may then need to be removed every so often.
Regular blood removal will not cure some of the complications of haemochromatosis such as diabetes or liver 'scarring' (cirrhosis). Therefore, early diagnosis and treatment are very important.
Liver transplant may occasionally be needed if the liver is very badly affected.
Haemochromatosis cannot be cured because the faulty gene cannot be removed. However, with early diagnosis and the right treatment, symptoms and complications can be avoided.
A haematologist will usually monitor the blood levels and advise on treatment. If there are very high levels of iron, or any evidence of liver damage, a liver specialist (a hepatologist) will also be involved in the management.
Foods to avoid if you have haemochromatosis
Back to contentsThe increased levels of iron in the body cannot be treated by diet alone. Removing blood has a much bigger effect on reducing the levels of iron in the body. However, there are some recommendations of foods to avoid which can help to control iron levels. These are to:
Avoid vitamin supplements or tonics containing iron. This includes multi-vitamins and minerals. A balanced diet should provide all the vitamins and minerals needed.
Avoid breakfast cereals which are heavily fortified with iron.
Large doses of vitamin C should also be avoided because it increases the amount of iron absorbed from food eaten. Vitamin C also increases the amount of iron stored in the body.
Reduce intake of offal (eg, liver and kidney) and red meat.
Tea, coffee and all milk products taken with a meal reduce the amount of iron absorbed from food.
Eating a healthy balanced diet is still important. A very restricted or unusual diet will not significantly affect iron levels, and could cause other symptoms.
Further information on diet is available from the Haemochromatosis Society - see the 'Further reading and references' section at the end of this leaflet.
Alcohol and haemochromatosis
Back to contentsAlcohol can increase the rate at which iron is absorbed, particularly when drinking alcohol with a meal. Excessive amounts of alcohol can also damage the liver itself, adding to the risk of liver problems.
When drinking alcohol, it is important to keep it to sensible levels - an absolute maximum of 14 units per week. This should be spread out over the week rather than in 'binges'. It is sensible to try to avoid drinking alcohol with meals.
Alcohol should be avoided completely if there is liver damage from haemochromatosis or if there is any other liver disease.
Complications of haemochromatosis
Back to contentsThe excess iron stored in body organs can cause damage. The possible complications of haemochromatosis include:
Diabetes due to damage to the pancreas.
Heart disease -for example it can lead to the heart muscles becoming weak (dilated cardiomyopathy) or stiff (restrictive cardiomyopathy), heart failure and abnormal heart rhythms.
Liver 'scarring' (cirrhosis). People with haemochromatosis who develop cirrhosis are also at increased risk of liver cancer and should be checked regularly with ultrasound scans or magnetic resonance imaging (MRI) scans.
Joint damage.
What is the outlook (prognosis)?
Back to contentsIf haemochromatosis is diagnosed and treated early before any complications develop the outlook is very good with no reduction in life expectancy. In most people, haemochromatosis is not a fatal condition and life expectancy is normal.
If complications do occur then the prognosis may be much worse. This depends on which complication develops and how severe it is.
Patient picks for Blood problems

Allergies, blood and immune system
Thalassaemia
Thalassaemia is an inherited condition affecting the blood. There are different types, which vary from a mild condition to a serious or life-threatening condition. For the more severe forms of thalassaemia, modern treatment gives a good outlook, but lifelong monitoring and treatment are needed. Good treatment is important to prevent complications developing.
by Dr Colin Tidy, MRCGP

Allergies, blood and immune system
Polycythaemia rubra vera
Polycythaemia rubra vera (PRV) is a myeloproliferative disorder, which means the bone marrow makes too many blood cells. It is also sometimes just called polycythaemia (PV). There is an abnormally high number of red blood cells in your blood. You may also have an abnormally high number of platelets and white blood cells.
by Dr Hayley Willacy, FRCGP
Frequently asked questions
Can I prevent haemochromatosis?
No, haemochromatosis is a genetic condition inherited from your parents, meaning it cannot be prevented. However, early diagnosis and treatment can prevent symptoms and complications from developing.
Are all my children guaranteed to inherit haemochromatosis if both my partner and I are carriers?
No, it's not guaranteed that all your children will inherit the condition. If both parents are carriers of the abnormal gene, there is a 1 in 4 chance that a child will have haemochromatosis, a 2 in 4 chance they will be a carrier but not have the condition, and a 1 in 4 chance they will not have haemochromatosis and not be a carrier. These are averages, and specific outcomes can vary within a single family.
What is the role of a haematologist and hepatologist in managing haemochromatosis?
A haematologist typically monitors your blood iron levels and advises on the regular blood removal treatment (venesection therapy/phlebotomy). If your iron levels are very high, or if there is any sign of liver damage, a liver specialist (hepatologist) will also be involved in your care.
If I have haemochromatosis, can I still take my usual multi-vitamin supplement?
You should avoid vitamin supplements or tonics that contain iron, including many multi-vitamins and mineral supplements. It's generally recommended to get your vitamins and minerals from a balanced diet, as larger doses of vitamin C can also increase iron absorption and storage, and should also be avoided.
Will limiting certain foods significantly reduce my iron levels?
Dietary changes alone are not enough to treat the increased iron levels of haemochromatosis. Regular blood removal (phlebotomy) has a much greater impact on reducing iron levels. However, avoiding iron-fortified cereals, large doses of vitamin C, offal, and reducing red meat intake can help manage iron levels. A very strict or unusual diet is not recommended as it won't significantly affect iron levels and could lead to other issues.
What are the common early signs of haemochromatosis that might be missed?
The initial symptoms are often vague and can include feeling weak and tired, as well as experiencing joint pains or abdominal pains. Because these symptoms are common to many other conditions, haemochromatosis can be difficult to diagnose early on without specific tests.
How often will I need to have blood removed for treatment?
Initially, you might need to have blood removed frequently, possibly weekly, depending on how much excess iron you have in your body. Your iron levels will be closely monitored, and once they return to normal, you'll need regular blood tests and further blood removal from time to time to maintain normal levels.
Further reading and references
- Adams PC, Barton JC; How I treat hemochromatosis. Blood. 2010 Jul 22;116(3):317-25. Epub 2010 Mar 22.
- Crownover BK, Covey CJ; Hereditary hemochromatosis. Am Fam Physician. 2013 Feb 1;87(3):183-90.
- Fitzsimons EJ, Cullis JO, Thomas DW, et al; Diagnosis and therapy of genetic haemochromatosis (review and 2017 update). Br J Haematol. 2018 May;181(3):293-303. doi: 10.1111/bjh.15164. Epub 2018 Apr 16.
- EASL clinical practice guidelines for HFE hemochromatosis. J Hepatol. 2010 Jul;53(1):3-22. doi: 10.1016/j.jhep.2010.03.001. Epub 2010 Apr 18.
- Healthy eating and haemochromatosis; The Haemochromatosis Society
- Common conditions associated with hereditary haemochromatosis genetic variants: cohort study in UK Biobank; Pilling
- Haemochromatosis UK
Continue reading below
About the authorView full bio

Dr Philippa Vincent, MRCGP
General Practitioner, Medical Author
MB BS, Bsc, MRCGP (2000), DCH, DFSRH, DRCOG
Dr Philippa Vincent is an NHS GP working in North London.
About the reviewerView full bio

Dr Colin Tidy, MRCGP
General Practitioner, Medical Author
MBBS, MRCGP, MRCP (Paediatrics), DCH
Dr Colin Tidy is an NHS Doctor, based in Oxfordshire.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 8 Aug 2028
10 Aug 2023 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free
Sign up to the Patient newsletter
Your weekly dose of clear, trustworthy health advice - written to help you feel informed, confident and in control.
By subscribing you accept our Privacy Policy. You can unsubscribe at any time. We never sell your data.