Verrucae
Plantar warts and myrmecia verrucae
Peer reviewed by Dr Toni Hazell, MRCGPLast updated by Dr Rosalyn Adleman, MRCGPLast updated 6 Aug 2025
Meets Patient’s editorial guidelines
- DownloadDownload
- Share
- Language
- Discussion
- Audio Version
- Add to preferred sources on Google
Medical Professionals
Professional Reference articles are designed for health professionals to use. They are written by UK doctors and based on research evidence, UK and European Guidelines. You may find the Warts and verrucas article more useful, or one of our other health articles.
In this article:
Synonym: myrmecia
Continue reading below
What are verrucae?
Verrucae are hyperkeratotic lesions found particularly over the pressure areas of the feet (heel and ball). They are also known as verrucae plantaris, or plantar warts. They are usually self-limiting but may be treated if symptomatic.
Plantar wart
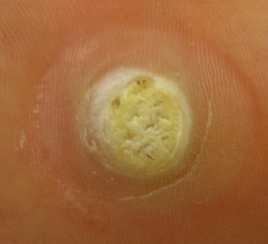
Verrucae causes (aetiology)1
Back to contentsVerrucae are caused by the human papillomavirus (HPV), particularly types 1, 2, 4, 27 and 57.2 They affect epithelial cells causing small rough papules. Replication of the virus within the epithelial cells causes a proliferative reaction and formation of plaque or papule. Incubation is very variable, ranging from one month to over a year.
HPV infection is acquired from direct contact with an affected individual or from the environment (for example, from contaminated floors in places such as communal showers and changing areas or swimming pools). Damaged or wet skin predisposes to infection. It appears the virus can survive outside the body for a significant length of time, probably months or even years.
They should not be used as a reason to stop children swimming, as learning to swim is important in the National Curriculum and helps to prevent death from drowning.3
Continue reading below
How common are verrucae? (Epidemiology)1 4
Back to contentsWarts are very common and thought to affect 7-12% of the population. No large studies are available; however, small studies suggest up to 30% of children and young adults may have warts. There are no high-quality epidemiological studies on prevalence of verrucae specifically.
Verrucae are more common in young people regularly using swimming pools and communal washing/changing areas.
Verrucae symptoms (presentation)
Back to contentsHistory
They may cause pain, particularly with walking.
Occasionally leg or back pain may result from altered posture or gait disturbance.
They are more common in those who are immunosuppressed:
Long-term immunosuppressant usage.
Untreated HIV.
Transplant patients.
Lymphomas and leukaemias.
Examination
Firm, hyperkeratotic lesions.
May have minor pinpoint petechiae centrally within the lesions. These may appear as small black dots.
Usually found over pressure areas.
Flat because of pressure.
May fuse with surrounding warts (mosaic warts - below).
Debrided verruca
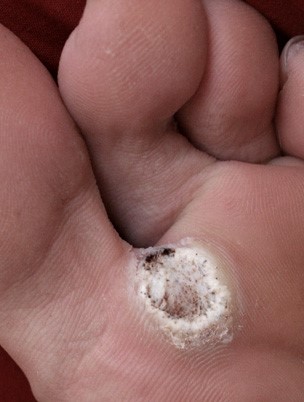
© Goatboy~commonswiki, via Wikimedia Commons
Diagnosis
Diagnosis is made by examination and observation of typical features.
Continue reading below
Differential diagnosis5
Back to contentsCorns: these are inflamed and painful. Paring corns reveals pearly sections of keratin.
Calluses: these are thick and painless patches of hard skin.
Black heel: patches of hard skin with ruptured capillaries.
Verrucous squamous cell carcinoma: this should be considered if long-standing. They invade the dermis but are slow-growing and rarely metastasise.
Lichen nitidus.
Keratoderma.
Diagnosing verrucae (investigations)
Back to contentsNone is usually required or appropriate. Distinguishing them from corns may require paring of the keratin. Blood tests to check for causes of immunodeficiency may be required in unusually widespread or resistant cases.
Management of verrucae1 4 6
Back to contentsTreatment is not necessarily required if the verruca is not painful. However, a wart on the sole of the foot is more likely to cause discomfort than warts in other areas such as the hands.
Topical salicylic acid has the best evidence base and is inexpensive.7 It is therefore normally first-line treatment. There is no evidence for one preparation being more effective than another. The wart should be pared down prior to application. Daily treatment for at least 12 weeks is required.
Cryotherapy with liquid nitrogen every two weeks until the wart has gone (up to four months) may be effective. For plantar warts, there is evidence that this is more effective if the lesion is pared down first. Clinicians vary in how long they freeze the wart for; usually liquid nitrogen is applied until a ring of frozen tissue is visible around the wart, typically 5 to 30 seconds. There is no evidence that a spray or cotton bud application is more effective. Over-the-counter preparations do not reach such low temperatures and are probably not as effective. Reported cure rates vary hugely. Cryotherapy may be painful, may cause blistering and should be avoided in young children.
Cryotherapy may be used in combination with topical salicylic acid. The latter is applied in between episodes of cryotherapy, once the blistering has settled down.
Other treatments with some evidence base recommended as options by the British Association of Dermatologists (BAD) guidelines include:
Dithranol.
5-fluorouracil (5-FU).
Formaldehyde.
Glutaraldehyde.
Laser.8
Microwave therapy
Photodynamic therapy.
Podophyllotoxin.
Topical immunotherapy.
These treatments would be carried out in secondary care.
Secondary care referral may be necessary in the following situations:5
Facial wart.
Diagnosis is uncertain.
Person is immunocompromised.
Areas of skin that are extensively affected - e.g. mosaic warts of the hands and feet.
Persistent warts that are unresponsive to both topical salicylic acid and cryotherapy.
Complications of verrucae
Back to contentsSecondary to condition or treatment:
Pain.
Infection.
Spread.
Scars and keloid formation.
Psychological.
Malignant change: extremely rare, especially with normal immunity. Whilst it rarely occurs, be aware of the possibility in patients who are immunocompromised (for example, transplant patients).
Prognosis5
Back to contentsCutaneous warts do not usually cause symptoms and in most cases resolve spontaneously within months (at the most, within two years). However, in adults resolution may take 5-10 years..
One study showed in school children, half resolved within one year and two thirds within two years.9 Those with immunosuppression may be resistant to treatment.
Prevention of verrucae5
Back to contentsSuggestions for reducing spread include:
Cover the verruca with a waterproof plaster when swimming. Swimming socks have no value other than in attracting attention and increasing stigma and should not be encouraged.10
Wear flip-flops in communal areas and showers.
Avoid sharing shoes, socks or towels.
Limit auto-inoculation by avoiding trauma (scratching and biting), keeping feet dry and changing socks or tights daily.
Further reading and references
- Al Aboud AM, Nigam PK; Wart. StatPearls, 2021.
- British Association of Dermatologists Guidelines for the management of cutaneous warts; British Journal of Dermatology (2014)
- Witchey DJ, Witchey NB, Roth-Kauffman MM, et al; Plantar Warts: Epidemiology, Pathophysiology, and Clinical Management. J Am Osteopath Assoc. 2018 Feb 1;118(2):92-105. doi: 10.7556/jaoa.2018.024.
- Brenner RA, Taneja GS, Haynie DL, et al; Association between swimming lessons and drowning in childhood: a case-control Arch Pediatr Adolesc Med. 2009 Mar;163(3):203-10.
- Kwok CS, Gibbs S, Bennett C, et al; Topical treatments for cutaneous warts. Cochrane Database Syst Rev. 2012 Sep 12;9:CD001781. doi: 10.1002/14651858.CD001781.pub3.
- Warts and verrucae; NICE CKS, October 2024 (UK access only)
- Loo SK, Tang WY; Warts (non-genital). BMJ Clin Evid. 2014 Jun 12;2014. pii: 1710.
- Becker BA, Childress MA; Common Foot Problems: Over-the-Counter Treatments and Home Care. Am Fam Physician. 2018 Sep 1;98(5):298-303.
- Nguyen J, Korta DZ, Chapman LW, et al; Laser Treatment of Nongenital Verrucae: A Systematic Review. JAMA Dermatol. 2016 Sep 1;152(9):1025-34. doi: 10.1001/jamadermatol.2016.0826.
- Bruggink SC, Eekhof JA, Egberts PF, et al; Natural course of cutaneous warts among primary schoolchildren: a prospective cohort study. Ann Fam Med. 2013 Sep-Oct;11(5):437-41. doi: 10.1370/afm.1508.
- Understanding Verrucas; British Swimming
Continue reading below
About the author

Dr Rosalyn Adleman, MRCGP
MRCGP
Dr Rosalyn Adleman, is an NHS GP working in north London.
About the reviewerView full bio

Dr Toni Hazell, MRCGP
MBBS, BSc, MRCGP, DFSRH, Dip GU med, DRCOG, DCH (London, UK, 2000)
Dr. Toni Hazell qualified from St. Mary’s Hospital Medical School and did her VTS at Northwick Park Hospital.
Article history
The information on this page is written and peer reviewed by qualified clinicians.
Next review due: 5 Aug 2028
6 Aug 2025 | Latest version

Ask, share, connect.
Browse discussions, ask questions, and share experiences across hundreds of health topics.

Feeling unwell?
Assess your symptoms online for free